An all-woman breast cancer team? Yes
Celeste Saenz moves from Texas to Oregon after finding the expert care and support she needs at OHSU

Celeste Saenz packed up a moving truck and drove 2,000 miles from San Antonio to Portland. It was worth it to get breast cancer care at the OHSU Knight Cancer Institute.
Never mind the COVID-19 pandemic. Or the freak October snowstorm in New Mexico. Or that she didn’t know anyone in Oregon.
“It was kind of scary sometimes,” she says. “But I felt like I had to do it, and I had to do it now, or who knows how long I’d be waiting.”
She had searched for four months to find two women surgeons who could work together to remove and reconstruct her left breast. That was hard to find in Texas but routine at OHSU, where women far outnumber men on the breast cancer team.
Saenz feels comfortable with women health care providers because she has post-traumatic stress disorder from a sexual assault in the military. Her all-female OHSU care team understood her situation and surrounded her with support from the start.
Nurse navigator Debra Harris guided her through care. Social workers helped address her concerns before she even met her doctors. And, most importantly, her plastic surgeon, Dr. Juliana Hansen, and her cancer surgeon, Dr. Arpana Naik, are experts who often team up in the operating room.
“Once I was able to find OHSU and the services I needed, everything went really smoothly,” Saenz says.
It’s common to find women professionals and a team devoted to your needs in breast cancer care at OHSU.
“It was shocking to me that Celeste had to work so hard to get a team that fit her needs,” Dr. Hansen says. “She had to move from Texas across the country to specifically come here. She’s so brave.”
“We’ve got to fight this thing”

Saenz was on vacation to celebrate her 38th birthday in September 2019 when she got the call: The almond-sized lump in her left breast was cancer. She had an instant of “oh, crap” shock and a few tears before her Air Force training kicked in.
“Then it was like, all right, suck it up,” she says. “We’ve got to fight this thing. The military gives you the mindset to focus on what’s in front of you, get your feelings out of it, get the information you can, and push forward. That’s what I did.”
Saenz grew up in a military family and served 15 years on active duty with the Air Force. She learned Korean to intercept and translate top-secret communications, then served two years in South Korea. She later retrained to be a respiratory therapist at a military medical center in Nevada.
She intended to stay in the military until she retired, but a sexual assault while on active duty brought her service to an abrupt end.
What stayed was the trauma.
Saenz returned to San Antonio, where she grew up, and was working through her post-traumatic stress when cancer changed her priorities.
From long hair to a buzz cut
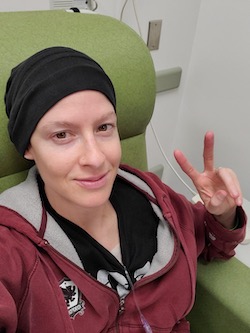
Her doctor felt the tumor in a routine wellness check. Saenz didn’t worry at first, because she had a similar lump in her right breast about a year earlier. That one turned out to be a harmless pouch of fluid.
A mammogram, then an ultrasound and finally a biopsy confirmed this one was cancer. At first, her Texas doctors thought a lumpectomy would be enough to remove the tumor. Then the tumor tripled in size and grew a satellite nodule in just six weeks. Saenz needed chemotherapy to shrink the tumor and then a mastectomy to remove all the tissue in her left breast.
She buzzed her long, wavy brown hair military-short and wore an “F— Cancer” T-shirt to her chemotherapy treatments.
Halfway through her six chemo cycles, in March 2020, COVID-19 was declared a pandemic.
Many surgical procedures were banned in Texas to free up hospital resources, making it even harder for Saenz to find the type of surgery and team she needed.
She was looking for two women surgeons who could do her mastectomy and start her reconstruction at the same time.
“I always ask for female providers, especially when it came to breast cancer and being exposed all the time,” she says. “It’s a sensitive area and a sensitive topic for me.”
She wanted to find a team with expertise in the latest surgical techniques. She hoped to keep her nipple and an envelope of skin for a more natural look after reconstruction. And she needed to find a hospital that took her VA medical insurance.
The first place that checked all her boxes was OHSU. Three of four plastic surgeons, two primary cancer surgeons, and most of the nurses and other specialists on OHSU’s breast cancer team are women. Dr. Naik is an expert in skin- and nipple-sparing surgery, and Dr. Hansen is highly skilled in creating a natural appearance.
Oregon’s relatively low rates of COVID-19 at the time and OHSU’s safety precautions also put her at ease.
“We coordinate your surgical care and work closely as a team,” Dr. Hansen says. “We wouldn’t dream of doing it any other way.”
The team understood and respected her request for all-women providers and was careful to ensure that men didn’t come into her room unexpectedly. That can be tricky at an academic health center, where trainees play integral roles.
“It’s awkward for me to have to tell a student who’s trying to be a doctor why I’m so uncomfortable every time,” she says. “But they tried to make sure that didn’t happen. I didn’t have that in other places.”
“Everything is looking up”
After two surgeries, Saenz is recovering, cancer-free, cleared for exercise, and happy with the results.
For most of her life, she had long hair down to her belly button. She’s kept it in a buzz cut with clippers for about a year, even after it started to grow back.
“I’m kind of at the point of, let me deal with everything else and not my hair,” she says.
She has mostly kept to herself in her sparsely furnished Beaverton apartment to avoid exposure to COVID-19. Her only visitors were her parents, who helped care for her after her surgeries.
But now that she’s vaccinated and the weather is warming up, she’s looking forward to getting out more to explore the Pacific Northwest — and maybe even growing out her hair again. Her one-year lease ends in October 2021, but she might stay longer. She wants to focus on her mental health, go back to school and figure out a new career path.
“Everything is looking up,” she says. “Once I can get out more, it will be a new beginning. I’m ready to be done with this and get back to the things I need to do to get healthy again.”
— By Suzanne Pardington Effros, a Portland writer who previously worked as a communications specialist at Portland State University and as an education reporter at The Oregonian.
Note: OHSU considers accommodations regarding health care professionals based on specific characteristics, such as gender identity, only on an individual basis and only if certain criteria are met. Even if criteria are met, accommodations can only be provided under certain circumstances when possible and cannot be guaranteed.
Location
OHSU Breast Center, South Waterfront
Center for Health & Healing, Building 2, ninth floor
3485 S. Bond Avenue
Portland, OR 97239
Free parking for patients and visitors
Refer a patient
- Refer your patient to OHSU.
- Call 503-494-4567 to seek provider-to-provider advice
Cancer clinical trials
Clinical trials allow patients to try a new test or treatment.
Read more
Learn more about OHSU Knight Cancer Institute treatments:
More patient stories
Read more inspiring stories from cancer patients who were treated at OHSU.