Melanoma Diagnosis and Treatment
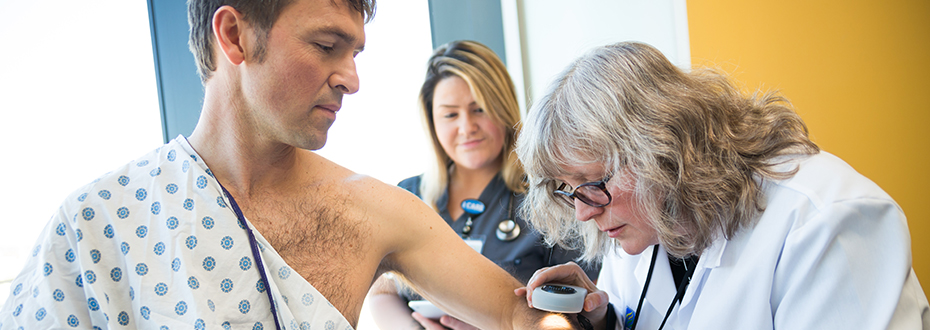
Our team includes some of the nation’s leading experts on diagnosing and treating melanoma. Doctors with many different specialties work together to provide outstanding care.
- Our experts develop an individual treatment plan for you based on your needs and specific cancer.
- Our physician-nurse practitioner team has a combined 45 years of experience in melanoma screening. You benefit from quick diagnosis and treatment.
- Our team meets three times a month, pooling their knowledge to recommend the best treatment.
- You'll have access to groundbreaking research and clinical trials exploring the latest treatments.
- We offer Mohs surgery to treat some melanomas.
- We offer tumor-infiltrating lymphocyte therapy (TIL therapy) for people with late-stage melanoma.
Melanoma screening
We have the expertise and tools to catch suspicious lesions early, when melanoma is most curable. You'll find:
- Full-body exams: These are typically done once a year. Patients at high risk of melanoma have them more often.
- Full-body photography: This tracks changes over time. Our high-resolution DermSpectra system uses nine cameras and a private booth.
- Mole Mapper, a free smartphone app that helps you track moles between visits.
Melanoma diagnosis
If you have a mole or skin area that looks abnormal, your doctor may run tests such as:
- Skin exam: Your doctor will examine your skin for moles, lesions or areas that look abnormal. They may use a device called a dermatoscope, which has a light and magnifier to show skin more clearly. They may take photos to track changes over time.
- Biopsy: If a mole looks suspicious, your doctor may remove a small amount of tissue. A doctor will look at the tissue under a microscope to check for cancer cells. For some minor cases, the entire tumor is removed as part of the biopsy, and only monitoring is needed otherwise.
- Sentinel lymph node biopsy: If a deeper melanoma is found, your doctor will check whether cancer has spread to your lymph nodes. Your doctor will remove the "sentinel" lymph node, the node where cancer is most likely to spread first. That node and possibly others will be checked under a microscope for cancer cells.
- Further lymph node biopsies: If no cancer is found in the sentinel lymph node, it is highly unlikely the melanoma has spread. If cancer cells are found, other lymph nodes may be removed and examined.
Melanoma treatments
Your treatment will depend on the depth of the melanoma and how advanced it is. In mild cases, surgical removal may be all that’s needed.
Melanoma surgery
- In-office excision: Many early-stage melanomas can be removed during an office appointment.
- Wide local excision: For slightly deeper cancers, margins around the cancer are wider to ensure that all the cancer is removed.
- Mohs surgery: This is most often used for other skin cancers. But our technology and expertise make it an option for certain melanomas. The surgeon removes a layer of skin and tissue at and around the tumor and examines it under a microscope. The process is repeated until no cancer cells are seen.
- Lymph node dissection: If a biopsy shows cancer in a sentinel lymph node, your doctor may recommend removing nearby lymph nodes to keep the cancer from spreading.
Targeted therapy
These medications lock onto receptors on melanoma cells. We run advanced tests on your cancer to pinpoint whether targeted therapy can help you. Examples:
- BRAF inhibitors: About half of people with melanoma have tumor mutations in what is called the BRAF gene. These changes cause the gene to make an abnormal protein that helps melanoma cells grow rapidly. Medications (given as pills) called BRAF inhibitors shut down the abnormal protein.
- MEK inhibitors: Something called the MEK gene works with the BRAF gene, so MEK inhibitors (also in pill form) can work in the same way.
Immunotherapy
Immunotherapy harnesses the power of your immune system to destroy cancer. Your natural immune cells hunt down and attack cancer. But sometimes the cancer fights back by sending signals that confuse the immune cells or switch them off. Immunotherapy works by switching them back on so they can destroy the cancer.
We offer several types of immunotherapy for melanoma, including:
- Immune checkpoint inhibitors: Sometimes cancer sends false signals to “checkpoints” on your immune cells, which switches them off. These drugs jam the checkpoints so the immune cells stay on and attack the cancer. They are usually given by IV.
- Tumor-infiltrating lymphocyte therapy (TIL therapy): TIL therapy is a type of immunotherapy that uses lymphocytes, which are a type of blood cell. Doctors take some of your lymphocytes, turn them into cancer fighters, and give them back to you.
Learn more about immunotherapy at the Knight Cancer Institute.
Radiation therapy
Radiation in the form of high-energy rays can kill cancer cells. Radiation may be used after surgery, especially if cancer has invaded lymph nodes. Radiation is also used to treat melanoma that has come back after surgery and to treat organs affected by the spread of melanoma.
Chemotherapy
Chemotherapy may be recommended for people with melanoma that has spread to distant parts of the body. Some chemotherapy drugs can shrink these melanomas, though the cancer often starts growing again within several months.

Additional services
- Look for a clinical trial for melanoma.
- We offer a full range of support services for patients and families.
- Our rehabilitation clinic offers services for cancer patients.
- We offer Oregon’s only support program for cancer patients diagnosed from ages 15 to 39.
Learn more
- Melanoma Treatment, National Cancer Institute
- Treating Melanoma Skin Cancer, American Cancer Society
- Melanoma Treatments, Skin Cancer Foundation
- Melanoma: Diagnosis and Treatment, American Academy of Dermatology
- Treatment Options, AIM at Melanoma Foundation
- Side Effect Management, AIM at Melanoma Foundation
Location
Knight Cancer Institute, South Waterfront
Center for Health & Healing, Building 2, ninth floor
3485 S. Bond Ave.
Portland, OR 97239
Free parking for patients and visitors
Refer a patient
- Refer your patient to OHSU.
- Call 503-494-4567 to seek provider-to-provider advice.
Cancer clinical trials
Clinical trials allow patients to try a new test or treatment.
Read more
Learn more about OHSU Knight Cancer Institute treatments: