Types of Clinical Simulation Training
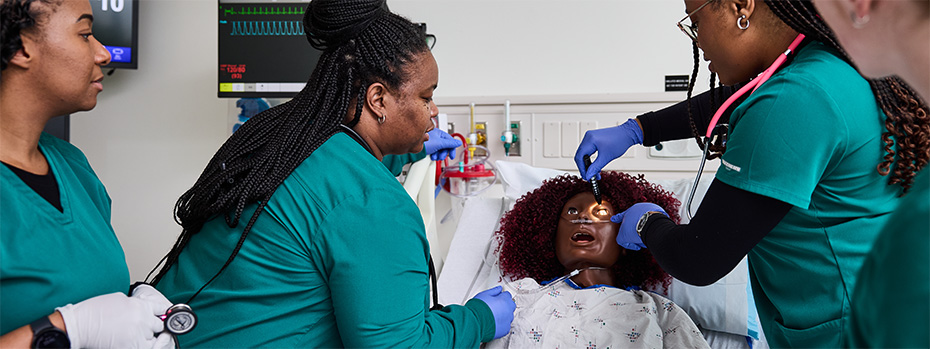
OHSU offers a range of simulation modalities (types of training) across our centers, from manikins to virtual reality, in settings that mimic real clinical care. Simulations range in fidelity (how realistic they are) from low-fidelity exercises that teach basic skills to high-fidelity scenarios that prepare you for complex care.
These simulations are used across OHSU’s medical, nursing, pharmacy and physician assistant programs. Explore simulation training and programs to see how each simulation is used in different health programs.
Manikin-based simulation
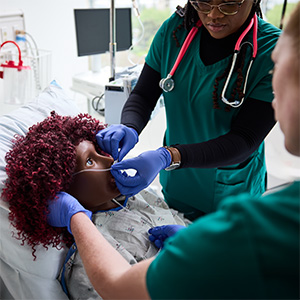
Practice skills and refine procedures without risk to real patients using life-size manikins. The manikins range from newborns to adults and can breathe, blink, cry, bleed, convulse and talk.
Manikins display realistic vital signs and can be programmed to simulate medical emergencies like cardiac arrest, strokes, major trauma and childbirth. They respond realistically to medications and anesthesia.
Key clinical skills:
-
Emergency and critical care skills
- Airway complications
- Breathing complications
- Low oxygen complications (hypoxia)
- Cardiac complications
- Circulation complications
- CPR skill building
- Defibrillation, cardioversion and pacing
-
IV, medication and procedure skills
- Vascular skill development (IV starts and access)
- IV drug administration
- Pharmacology skill development (medication safety and response)
- Urinary catheterization
- Male and female anatomy skills
-
Patient care and assessment skills
- Patient care skill development
- Diagnostic skill building
- Diagnostic sounds and modules (heart, lungs, etc.)
-
Pregnancy, birth and postpartum skills
- Normal and assisted vaginal deliveries
- Shoulder dystocia (delivery complication)
- Labor complications
- Breech and placental deliveries
- C-section deliveries
- Postpartum care
Skills-training simulation

Skills-training simulation uses partial manikins and task trainers (models of specific body parts for practicing procedures and exams) to help you develop clinical skills and practice patient interactions. You'll start with basic skills like drawing blood and progress to advanced procedures like endovascular surgery and trauma care.
This training improves your critical thinking, decision-making, clinical techniques and visual, tactile and coordination skills without risk to real patients.
Key clinical skills:
- Suturing
- Dissection
- Pattern cutting
- Drawing blood
- Endovascular surgery
- Trauma care
Tissue-based simulation

Tissue-based simulation lets you practice surgical and procedural skills using human tissue from donors and animal tissue from industry partners.
As you advance in your curriculum, simulation difficulty increases. You’ll start in dry labs with task trainers (models that let you practice specific procedures). Then you’ll move to wet lab experiences with human or animal tissue.
Key clinical skills:
- Suturing and knot-tying
- Dissection and surgical exposure techniques
- Vascular and soft tissue repair
Virtual reality simulation

Virtual reality simulation lets you practice surgical procedures and techniques including endoscopy, bronchoscopy and laparoscopic surgery. You'll interact with virtual patients and receive audio and haptic feedback (physical sensations like resistance and texture) in low-risk environments that closely mirror real-life situations.
Key clinical skills:
-
Endoscopy and bronchoscopy
You'll practice lower and upper gastrointestinal flexible endoscopy and bronchoscopy on virtual patients with realistic feedback.
-
Laparoscopic techniques
You'll practice laparoscopic surgical techniques including:
- Cutting
- Knot-tying
- Clipping
- Camera navigation
You'll also perform complete procedures like cholecystectomies, hysterectomies and oophorectomies.
-
Surgical skills
You'll practice surgical instrument control using robotic surgery systems. The simulator tracks your progress over time and provides performance feedback.
Standardized patient simulation

Work with trained actors called standardized patients to practice patient communication and interactions. OHSU's program includes over 70 standardized patients who help you build the skills you need for patient care.
You'll practice:
- Patient interviews
- Physical exams
- Diagnosing patients
In complex scenarios, a standardized patient can be paired with a task trainer. This allows you to perform more invasive skills on the trainer instead of on an actual person, providing a more realistic learning experience.
How do I become a standardized patient?
If you’re interested in becoming a standardized patient, search OHSU’s standardized patient job listings.
-
Standardized patient FAQ
What is a standardized patient?
A standardized patient is a trained actor who portrays a specific patient case. Standardized patients are typically healthy people who learn to present a patient's history and physical symptoms. They repeat their story the same way to several students, respond to questions, undergo physical exams and give students constructive feedback.
What happens in a typical standardized patient exercise?
Students rotate from station to station, alone or in groups. A faculty member may observe and grade using a checklist. The student interviews or examines you for 10-15 minutes. You’ll complete evaluation forms, then break character to give the student feedback.
How is this different from acting?
This work focuses on discipline within the case and exam requirements, not dramatic moments or playing to an audience. You may need to appear anxious, irritable or confused if the scenario requires it. The ability to improvise helps. You don't need medical background or vocabulary.
How do I know what to say when the medical student interviews me?
You receive training by reviewing a patient's case or script. The script details the medical problem, past medical history, family situation, social situation and emotional state you will portray. You learn specific body language, movement and responses to physical examination. You may attend formal training sessions with other standardized patients at our center.
Will I undergo a physical exam or remove my clothing?
For cases requiring no physical exam, you wear street clothes. If students perform a physical exam, you may wear a hospital gown. We outline these cases before you agree to participate.
Do I decide if the student passes?
No. Faculty decide whether students pass. Your job includes giving students verbal feedback on their interpersonal skills from a patient's perspective. Some exams require standardized patients to use a checklist to grade students, and we provide training for these.
How often would I work?
The work is temporary, part-time and seasonal. We schedule standardized patient sessions according to student needs and program requirements. Some standardized patients work two or three days a year while others work 10 days in a month. Standardized patients who arrive on time and perform well receive first preference for future work.
Email us at SPprogram@ohsu.edu for more information about the standardized patient program.
Sensitive Exam Teaching Associates (SETAs)
Sensitive Exam Teaching Associates, or SETAs, are trained participants who work with clinical educators to teach proper technique for genital, prostate, chest and pelvic exams. Unlike standardized patients, who portray a wide range of clinical scenarios, SETAs specialize in teaching sensitive physical exam skills using a highly standardized approach.
You may see SETA roles listed alongside standardized patient positions in OHSU job searches. Availability and eligibility vary by role.
Study at OHSU
Explore our health and science degree programs.
Contact us
Have questions? Email us at simulation@ohsu.edu.
Standardized patient jobs
Body donation program
Request simulation services
Faculty and staff can reserve simulation resources to support teaching, research and health care training.