Bile Duct Cancer

Expert care is vital to diagnosing and treating bile duct cancers. These cancers are often found after they've spread, making treatment challenging.
At the OHSU Knight Cancer Institute, we offer the knowledge, skill and tools to treat this complex cancer. Patients benefit from the deep expertise of our surgeons, oncologists and other specialists. We also offer the latest treatments.
You’ll find:
- A team of specialists who work together to give each patient the best care.
- Advanced tests to help guide treatment.
- Hepatic arterial infusion (HAI) therapy.
- Experts in molecular profiling, which can help in treating some bile duct cancers.
- Palliative care specialists, who can help relieve symptoms and stress at any stage of bile duct cancer.
- Access to clinical trials testing promising new treatments.
Understanding bile duct cancer
What is bile duct cancer?
Bile duct cancer, often called cholangiocarcinoma, begins in a bile duct. The bile ducts are thin tubes that connect the liver and small intestine.
Bile ducts carry a fluid called bile from the liver to:
- The small intestine, where it helps digest fats in food.
- The gallbladder, where it is stored and later released into the small intestine.
Bile ducts are part of the biliary system, the organs and ducts that make and store bile.
Bile duct anatomy
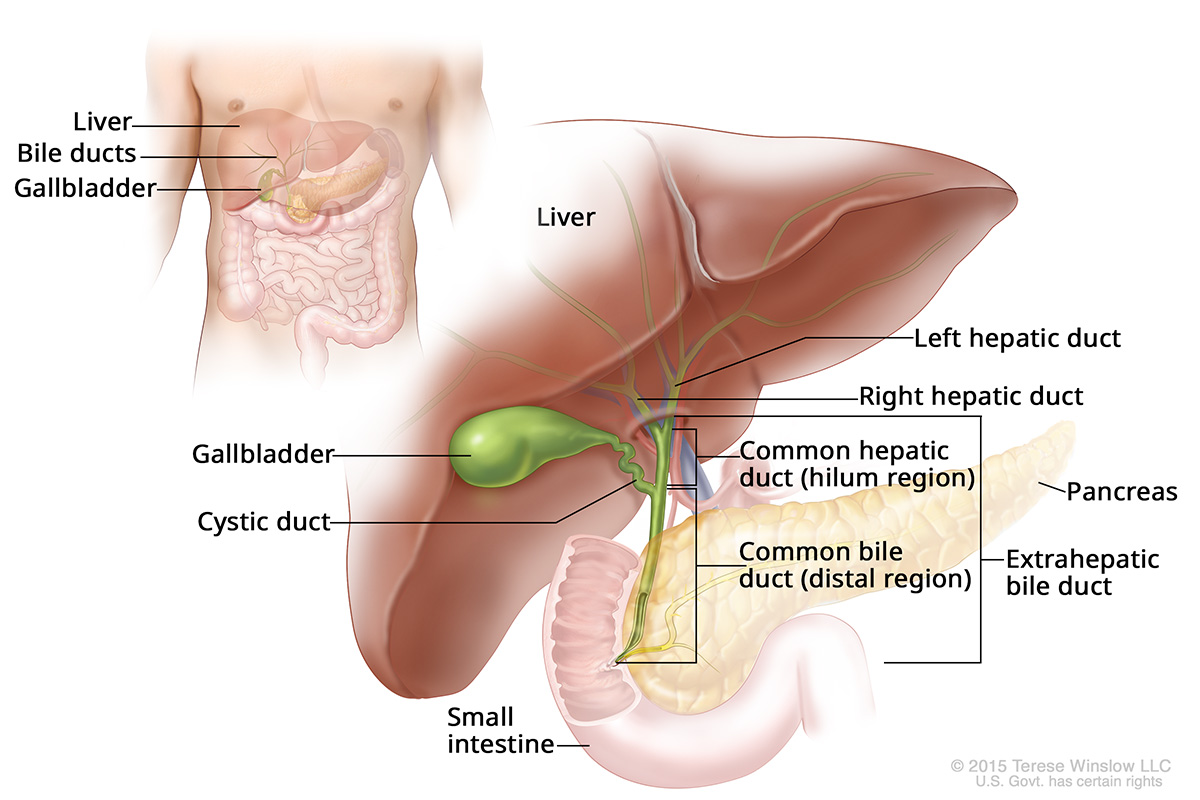
The body’s bile ducts branch down from the liver and gallbladder, joining into one duct before entering the small intestine.
The liver’s right and left hepatic ducts combine into the common hepatic duct as they exit the liver. Lower down, they join the cystic duct from the gallbladder to form the common bile duct.
Extrahepatic Bile Duct Anatomy
Who gets bile duct cancer?
Bile duct cancer is rare, with about 8,000 new cases in the U.S. each year, according to the American Cancer Society.
Risk factors include:
- Diseases in the liver or bile ducts
- Primary sclerosing cholangitis (a disease that can block bile ducts and damage the liver)
- Liver fluke infections (parasitic worms; more common in Asia)
- Viral hepatitis
- Cirrhosis
- Bile duct stones
- Choledochal cysts (a larger-than-normal bile duct from birth)
- Inflammatory bowel disease
- Age; about two-thirds of patients are 65 or older
- Alcohol use
- Diabetes
- Obesity
- Family history
Location
Knight Cancer Institute, South Waterfront
Center for Health & Healing, Building 2
3485 S. Bond Ave.
Portland, OR 97239
Free parking for patients and visitors
Refer a patient
- Refer your patient to OHSU.
- Call 503-494-4567 to seek provider-to-provider advice.
Cancer clinical trials
Clinical trials allow patients to try a new test or treatment.
Rare tumor, remarkable patient

Lynn Zimmer had a tumor in her bile duct. Could surgeons remove it and reconnect her digestive system?
Read more
Learn more about OHSU Knight Cancer Institute treatments:
Types of bile duct cancer
Bile duct cancers are classified based on where they occur:
Extrahepatic bile duct cancer is outside the liver.
- Perihilar, or hilar, bile duct cancer develops near where the left and right hepatic ducts join. This is the most common type, accounting for about 50% to 70% of cases. It is also called a Klatskin tumor.
- Distal bile duct cancer develops farther down, where the common bile duct travels through the pancreas. It accounts for 20% to 30% of cases.
Intrahepatic bile duct cancer occurs in bile ducts in the liver. This is the least common type.
Survival rates for bile duct cancer
Because this cancer is often found after it has spread, long-term outcomes can be discouraging. At the same time, outcomes are averages and can’t predict the outcome for a specific person.
At the Knight Cancer Institute, we offer a full range of therapies, plus clinical trials to try promising new treatments. Your care team will give you the highest quality of life possible for as long as possible.
Symptoms
Most often, bile duct cancer grows for years before signs or symptoms appear. Symptoms often occur after a tumor blocks a bile duct. Symptoms can also be similar to those of a more common ailment, such as gallstones.
Symptoms can include:
- Light-colored or greasy stools
- Dark urine
- Yellowing of the skin and the whites of the eyes (jaundice)
- Itching
- Nausea and vomiting
- Weight loss
- Chills
- Fever
- Pain in the upper right abdomen
Diagnosing bile duct cancer
Tests may include the following.
-
Blood tests
- Your care team can check the level in your blood of bilirubin, a chemical in bile. Buildup can be a sign that a tumor is blocking a bile duct.
- The team may look for substances that show how your liver is working.
- Doctors may look for “markers” or gene mutations that are linked to some bile duct cancers. Knowing if you have mutations can also guide treatment.
-
Imaging tests
- Ultrasound: This test uses sound waves to create detailed images of the inside of your body. Your care team may use a wand outside your body (abdominal ultrasound). Or your team may guide a tool through your mouth and stomach to your small intestine (endoscopic ultrasound). Or the team may place a tool near your bile ducts through a small incision (laparoscopic ultrasound).
- MRI scan: Magnetic resonance imaging uses radio waves and magnets to create images of soft tissues.
- Magnetic resonance cholangiopancreatography: MRCP is a type of MRI that produces detailed images of the area around your liver, gallbladder, bile ducts and pancreas.
- CT scan: Computed tomography uses X-rays to produce detailed images.
- Cholangiography: This test produces pictures that help doctors see if bile ducts are blocked, narrowed or widened. Some types of this test can be done outside your body. In another, a doctor guides a long, flexible tube through your throat and stomach to the first part of your small intestine.
- PET scan: Positron emission tomography uses a small amount of a radioactive substance that’s injected, swallowed or inhaled. This helps cancer cells show up on the scan. The scan can also show how organs or tissues are working.
-
Laparoscopy
Your doctor guides a thin tube with a light and video camera to your bile ducts through an incision. The doctor can measure the tumor and/or take a tissue sample to look for cancer cells.
-
Cholangioscopy
Your doctor guides a long, flexible tube through your throat and stomach and into your small intestine. The doctor can then guide a tiny camera inside to look for blockages or tumors. The doctor can also take a sample of any tumor.
-
Biopsy
Your doctor takes a small sample of tissue, with a needle or through an incision, so it can be checked for cancer cells.
Bile duct cancer staging
Staging helps your doctors understand the extent of cancer so they can make the best treatment recommendations. Doctors determine a bile duct cancer's stage based on a tumor's size and spread.
Here is a simple description of staging for perihilar cholangiocarcinoma, the most common bile duct cancer. The American Cancer Society website has more details.
- Stage I: The cancer has not spread outside the bile duct.
- Stage II: The cancer has grown into nearby fatty or liver tissue.
- Stage III: The cancer has grown into the liver’s portal vein, hepatic artery or both. Or the cancer has spread to one to three nearby lymph nodes.
- Stage IV: Cancer has spread to four or more lymph nodes, or elsewhere in the body.
Bile duct cancer treatment
Our doctors have expertise in the latest treatments for bile duct cancer. They work in teams, pooling their expertise for each patient.
Treatments might include:
Surgery

Surgery is recommended in about 10-20% of cases. Most of the time, bile duct cancer is found too late for surgery to be a good option.
We might do one of two types:
- Potentially curative surgery: Your care team will recommend surgery to remove the tumor if tests show there’s a good chance to get all of it.
- Palliative surgery: Your care team might recommend surgery to relieve symptoms or prevent complications, such as by removing a blockage. This type won’t cure the cancer but can help you feel better.
Radiation therapy
Experts use high-energy radiation beams or particles to kill cancer cells. They might use it to:
- Shrink a tumor before surgery.
- Extend life when surgery isn’t possible but cancer has not widely spread.
- Relieve pain or other symptoms.
Types of radiation therapy:
- EBRT: External beam radiation therapy is the most common type. Machines outside the body precisely direct X-rays to the tumor.
- Radioembolization: OHSU is among a handful of U.S. centers with an advanced treatment called radioembolization. Your care team guides a catheter (thin flexible tube) to blood vessels in or near the liver. They deliver tiny beads with radioactive particles through the catheter. The particles kill cancer cells while mostly sparing healthy tissue.
Thermal ablation
The care team destroys cancer cells with heat, cold, microwave or electrical currents. Often, the team inserts a needle or probe into the tumor. This treatment may be used when the tumor is small but surgery isn’t a good option.
Irreversible electroporation
Irreversible electroporation, or IRE, uses electrical impulses to create pores in a cancer cell that cause the cell to die. It does little damage to nearby tissue.
Photodynamic therapy
In photodynamic therapy, or PDT, doctors inject a light-activated medication that collects in cancer cells. A few days later, the doctor guides a flexible tube through the throat and stomach into your bile ducts.
A light at the end of the tube is turned on, activating the medication and killing the cancer cells. This option may help when surgery isn’t possible.
Chemotherapy
Chemotherapy uses medications to kill cancer cells nearly anywhere in your body. It may be given by mouth or IV.
It’s not effective for many types of bile duct cancer but may be used:
- After surgery, to keep cancer from returning.
- To shrink a tumor before surgery.
- As palliative therapy, to shrink or slow tumors. This can relieve pain or other symptoms.
Hepatic artery infusion (HAI)
We are one of the few cancer centers in the U.S. to offer hepatic arterial infusion (HAI) therapy. Doctors place a pump in your belly to deliver a powerful dose of chemotherapy into your hepatic artery, which supplies blood to most bile duct tumors. This helps shrink the tumor with minimal side effects. The Knight is a national leader in HAI therapy for bile duct cancer.
Targeted therapy
Some bile duct cancers respond to medications that “target” a gene mutation. About half of intrahepatic bile duct cancers have a mutation that can be targeted with medication.
These medications are more likely to leave healthy cells alone. Learn more about targeted therapy at the Knight Cancer Institute, a global pioneer in the field.
Immunotherapy
Immunotherapies use a range of ways to arm the body’s own immune system against cancer. Some help the body recognize and kill cancer cells, for example. The Knight Cancer Institute is a national leader in these next-generation therapies.
Liver transplant
A small portion of patients with intrahepatic or perihilar bile duct cancer are candidates for a liver transplant. It might help cure the cancer.
Palliative therapy
OHSU palliative therapy experts can help patients and their families ease symptoms and stress at any stage of serious illness.
Your care team also might offer treatments that won’t cure the cancer but that can relieve symptoms and/or extend life. These might include surgery, chemotherapy or radiation therapy. Medications can also lessen pain, nausea and itching.
Clinical trials
The Knight Cancer Institute is a national center for clinical trials to test new ways to prevent, detect and treat cancer.
You may be eligible for a clinical trial of a promising treatment that isn’t widely available. Bile duct clinical trials include:
- A trial studying the use of HAI and chemotherapy to treat intrahepatic bile duct cancer.
- A trial, with other leading cancer centers, to study a three-medication chemotherapy regimen to treat bile duct cancer before surgery.
Gallbladder cancer
Gallbladder cancer is a cancer of the biliary system. It is rare, with about 12,000 new cases in the U.S. each year, according to the American Cancer Society.
Gallbladder cancer has many of the same symptoms as bile duct cancer. They often appear only after the cancer has spread.
They can include:
- Jaundice
- Itchy skin
- Dark urine
- Light-colored or greasy stools
- Belly pain and nausea
Treatments for gallbladder cancers are similar to those for bile duct cancers. Surgery may be recommended if it’s found early enough. Other treatments include:
- Radiation therapy
- Chemotherapy
- Targeted therapy
- Immunotherapy
- Palliative therapy
The Knight Cancer Institute is part of a clinical trial testing whether chemotherapy is more effective before surgery than after.
Bile duct cancer team
-
Surgery
-
- Christopher R. Connelly, M.D., F.A.C.S.
- Accepting new patients
-
- Robert L. Eil, M.D.
- Accepting new patients
-
- C. Kristian Enestvedt, M.D., FACS
- Accepting new patients
-
- Erin W. Gilbert, M.D., M.C.R., FACS
- Accepting new patients
-
- John G. Hunter, M.D., FACS
- Accepting new patients
-
- Erin C. Maynard, M.D., FACS
- Accepting new patients
-
- Skye C. Mayo, M.D., M.P.H., FACS
- Accepting new patients
-
- Rodney F. Pommier, M.D., FACS, FSSO
- Accepting new patients
-
- Flavio G. Rocha, M.D., FACS, FSSO
- Accepting new patients
-
- Oren Shaked, M.D., FACS
- Accepting new patients
-
- Brett C. Sheppard, M.D., FACS
- Accepting new patients
-
- Divya Sood, M.D.
- Accepting new patients
-
- Patrick J. Worth, M.D., M.C.R., FACS, FSSO (he/him)
- Accepting new patients
-
-
Medical oncology
-
- Emerson Y. Chen, M.D.
- Accepting new patients
-
- Jeff Donovan, PA-C
- Accepting new patients
-
- Adel Kardosh, M.D., Ph.D.
- Accepting new patients
-
- Guillaume Pegna, M.D.
- Accepting new patients
-
-
Radiation oncology
-
- Nima Nabavizadeh, M.D.
- Accepting new patients
-
-
Medical genetics
-
- Kelly Jo Hamman, M.S., CGC
- Accepting new patients
-