Uterine Sarcoma

There are two primary kinds of uterine cancers, endometrial cancer and uterine sarcoma. This page discusses uterine sarcoma. Visit our endometrial cancer page.
Uterine sarcoma is a rare cancer that forms in the uterus, a part of the female reproductive system. When this cancer is found early, treatment is more effective.
The National Cancer Institute recognizes the OHSU Knight Cancer Institute as one of the best places in the nation to receive cancer care. You’ll find:
- Expert diagnosis and treatment for cancers of the female reproductive system
- Clinical trials for uterine sarcoma
- Nurses who guide you through your care
- Support services, including help for fertility after cancer
- A Sarcoma Survivorship Registry that helps advance research on treatments
What is uterine sarcoma?
Anatomy of Female Reproductive System
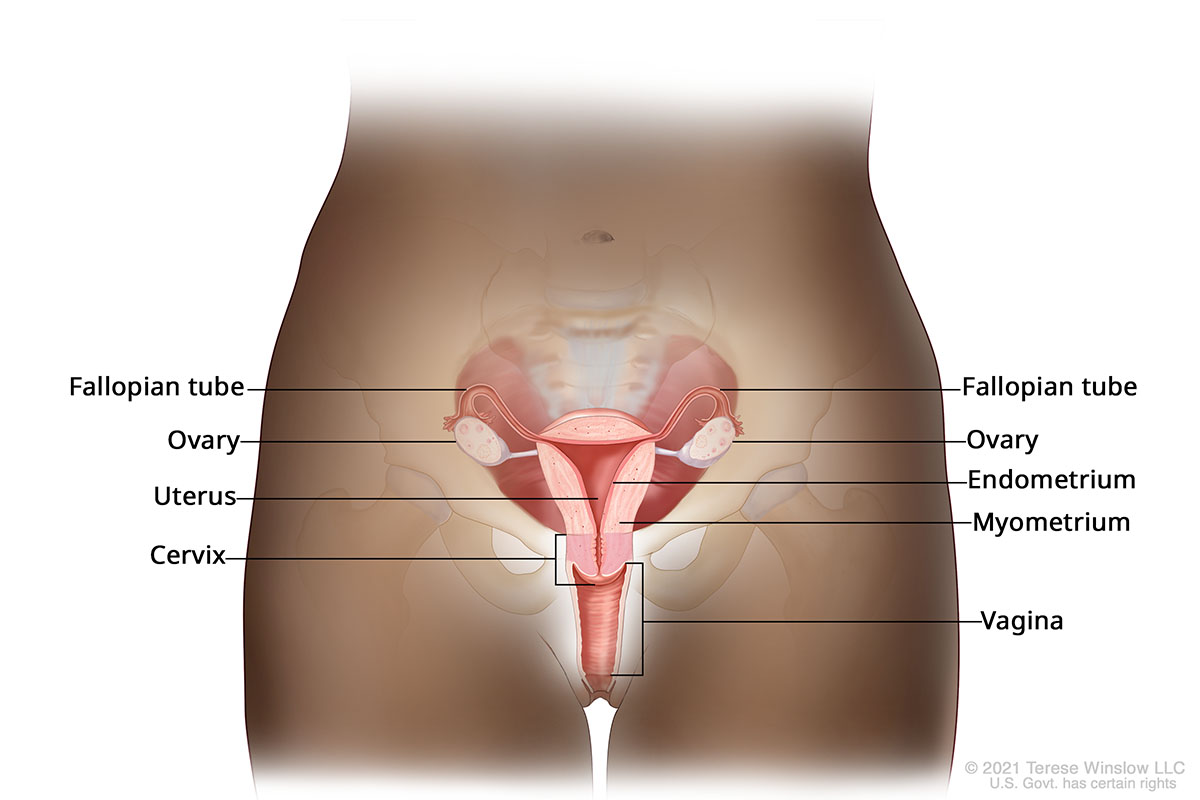
A sarcoma is a cancer that forms in bone, muscle or connective tissue. It starts when cells grow out of control.
Uterine sarcoma can develop in the:
- Myometrium: Muscles of the uterus
- Parametrium: Tissue that surrounds and supports the uterus
Types of uterine sarcoma
Uterine leiomyosarcoma: This is the most common type. It starts in the muscles of the uterus.
Adenosarcoma: This accounts for about 5% of uterine sarcomas. It starts between the muscles and inner lining of the uterus.
Undifferentiated sarcoma: This accounts for about 5% of uterine sarcomas.
Endometrial stromal sarcoma: This accounts for about 2% of uterine sarcomas. It starts in the inner lining of the uterus. It tends to grow slowly, making it easier to treat.
Who gets uterine sarcoma?
About 3,300 cases of uterine sarcoma are diagnosed in the United States every year. Most cases are found in people over 40. The average age at diagnosis is 60.
Risk factors
Anyone with a uterus is at some risk. Risk factors include:
Radiation therapy: Having had radiation to the pelvis.
Eye cancer: Having had an eye cancer called congenital retinoblastoma raises risk.
Kidney cancer: A family history of a kidney cancer called hereditary leiomyomatosis and renal cell cancer (HLRCC) raise risk. We offer genetic counseling and testing to see if you have inherited a gene linked to a higher risk.
Tamoxifen: Taking or having taken this drug for breast cancer increases risk.
Survival rates
Uterine sarcoma is often found in later stages, making it tougher to treat.
The five-year relative survival for uterine sarcoma is 75% for patients whose cancer is found early, according to a study from 2023. This rate is the portion of people who are alive five years after they were diagnosed compared with the general population.
Rates for later stages of uterine sarcoma are less encouraging. It’s important to remember that survival rates are averages. They don’t predict the outcome for any one person.
Uterine sarcoma signs and symptoms
Uterine sarcoma symptoms include:
- Unusual vaginal bleeding or spotting
- Pain, a lump or a feeling of fullness in the belly
- Urine or bowel problems
These symptoms may have other causes. It’s best to tell your doctor if you have these symptoms so you can get the right care.
Uterine sarcoma diagnosis
If your doctor thinks you may have uterine sarcoma, you may have any of these tests:
Ultrasound: This uses sound waves to create an image of your uterus. A small probe is placed in your vagina.
Hysteroscopy: This uses a thin, flexible tube with a camera. It’s placed inside you to show the uterus lining.
Endometrial biopsy: This uses a thin, flexible tube placed through the vagina and cervix. The tube removes a bit of the uterus lining to look at under a microscope.
Dilation and curettage: This is also called a D&C. A bit of tissue is taken from inside the uterus to look at under a microscope. This may be done if a biopsy doesn’t give clear results.
Genetic testing: This uses a blood test to look for changes in your DNA that are linked to uterine sarcoma.
Uterine sarcoma stages
Doctors use stages to describe how much cancer is in the body and how much it has spread.
Uterine sarcoma stages go from stage I through IV (4). Generally, a higher number means the cancer has spread more.
Staging is complex and varies from person to person. It’s best to talk with your doctor about your stage.
Stage I: The cancer is only in the uterus.
Stage II: The cancer has spread outside the uterus but not the pelvis.
Stage III: The cancer has spread outside the uterus to tissues in the abdomen, or it has spread to nearby lymph nodes.
Stage IV: The cancer has spread to the rectum, bladder or to distant parts of the body. It may be in nearby lymph nodes.
Uterine sarcoma treatment
Your care team will work with you on a plan tailored to your diagnosis, health and desire to have children.
Surgery
Surgery is the standard treatment for uterine sarcoma that is found early. We use robotic surgery for less pain, less time in the hospital, and quicker recovery.
Types of surgery include:
Total hysterectomy: This removes the uterus and cervix.
Bilateral salpingo-oophorectomy: This removes the ovaries and fallopian tubes on both sides.
Radical hysterectomy: This removes the uterus, cervix and part of the vagina. It may also remove the ovaries, fallopian tubes or nearby lymph nodes.
Lymph node dissection: This removes lymph nodes to check them for cancer.
Radiation therapy
Radiation therapy uses beams of energy to damage or destroy cancer cells.
Options include:
- External beam radiation: This type uses a machine outside the body to target the cancer.
- Brachytherapy: This type uses a higher dose in a smaller area. A radiation source is placed in a tube that’s put into the vagina for a short time. You may get doses over several visits.
Chemotherapy
Chemotherapy is used to kill or stop the growth of cancer cells. Chemo drugs are usually given in a series of infusions, or IV drips. Chemo may be used with surgery or radiation therapy.
Hormone therapy
Hormones are the body’s chemical messengers. Hormone therapy works on hormones to stop cancer cells from growing. These drugs may be given as a pill, liquid or shot.
Immunotherapy
Immunotherapy uses your immune system to knock out cancer cells. Immunotherapy drugs set up immune cells to find and target cancer cells.
Learn more
- Uterine Sarcoma, National Cancer Institute
- Uterine Sarcoma, American Cancer Society
Uterine sarcoma team
Gynecologic oncologists
-
- Amanda Bruegl, M.D. (she/her)
- Accepting new patients
-
- Amanda J. Compadre, M.D. (she/her/ella)
- Accepting new patients
-
- Ross Harrison, M.D., M.P.H. (he/him)
- Accepting new patients
-
- Breana L. Hill, M.D. (she/her)
- Accepting new patients
-
- Jessica Jou, M.D., M.S., FACOG (she/her)
- Accepting new patients
-
- Elizabeth Munro, M.D.
- Accepting new patients
Radiation oncologists
-
- Cheryl Claunch, M.D., Ph.D. (she/her)
- Accepting new patients
-
- Casey Williamson, M.D., M.A.S. (he/him)
- Accepting new patients
Location
Knight Cancer Institute, South Waterfront
Center for Health & Healing, Building 2
3485 S. Bond Ave.
Portland, OR 97239
Free parking for patients and visitors
Refer a patient
- Refer your patient to OHSU.
- Call 503-494-4567 to seek provider-to-provider advice.
Cancer clinical trials
Clinical trials allow patients to try a new test or treatment.
Read more
Learn more about OHSU Knight Cancer Institute treatments:
Stay informed
News: Read about research breakthroughs, patient care and many other topics on our OHSU News site.