Colon Cancer Signs and Symptoms
Signs of colon cancer don’t always appear right away. Often, signs might seem like another illness. That’s why it’s important to see your doctor if symptoms don’t go away.
Colon cancer, when combined with rectal cancer, is also known as colorectal cancer
Signs and symptoms
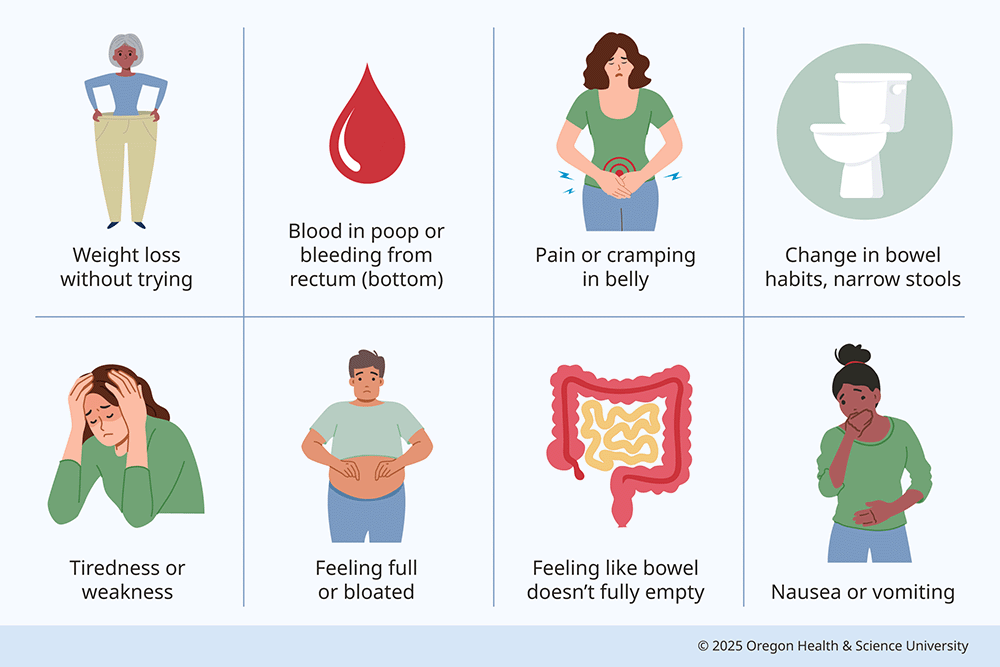
Signs and symptoms can include:
- Changes in bowel habits, such as frequent diarrhea or narrow stools
- Ongoing discomfort in the belly, including cramping, bloating and gas
- Mucus or blood in stools, which might make them look dark brown or black
- Changes in appetite
- Vomiting
- Losing weight without trying
- Weakness or tiredness
A blood test showing a low red blood cell count (anemia) can also be the first sign of colon cancer. Colon cancers can bleed into the belly, according to the American Cancer Society. Over time, that can lead to a low red blood cell count.
Colon Cancer Signs and Symptoms
Colon cancer risk factors
Risk factors for colon cancer include:
- Family history: Having a close relative, such as a parent or sibling, with a history of colon cancer increases risk.
- Gastrointestinal conditions: Having inflammatory bowel disease, including ulcerative colitis and Crohn’s disease, increases risk.
- Diet: Eating foods low in fiber and high in animal fats such as red meat can increase risk.
- Weight: Being overweight or obese can raise risk.
- Tobacco: Using cigarettes, cigars or chewing tobacco can raise risk.
- Inactivity: Lacking regular exercise increases risk.
- Race and ethnicity: Native Americans, Alaska Natives, Jews of Eastern European descent (Ashkenazi) and Black people have higher risk.
Parents sometimes pass down increased risk through inherited genetic changes, or mutations. These are called hereditary cancer syndromes:
- Familial adenomatous polyposis
- Lynch syndrome (also called hereditary nonpolyposis colorectal cancer, or HNPCC)
- MUTYH-associated polyposis
- Peutz-Jeghers syndrome
Inheriting a genetic change does not mean you will get cancer. The Knight offers expert genetic testing and counseling to help you identify and manage risk.
Location
Knight Cancer Institute, South Waterfront
Center for Health & Healing, Building 2
3485 S. Bond Ave.
Portland, OR 97239
Free parking for patients and visitors
Refer a patient
- Refer your patient to OHSU.
- Call 503-494-4567 to seek provider-to-provider advice.
Cancer clinical trials
Clinical trials allow patients to try a new test or treatment.
Read more
Learn more about OHSU Knight Cancer Institute treatments: