Gastrointestinal Stromal Tumor (GIST)

Gastrointestinal stromal tumors (GISTs) are rare tumors found in the digestive tract.
The GIST team at the OHSU Knight Cancer Institute has years of experience caring for patients with this cancer. We treat more patients with GISTs than any other hospital on the West Coast.
We offer you:
- GIST specialists, led by internationally renowned oncologist Michael Heinrich, M.D.
- One of the largest GIST programs in the United States.
- Access to emerging treatments through clinical trials.
- Team-based care with surgeons, gastroenterologists and other specialists working together.
- Gleevec, a targeted medication developed through pioneering work at OHSU.
- A full range of support services for you and your family.
Understanding gastrointestinal stromal tumors
What are GISTs?
Gastrointestinal stromal tumors start in the wall of the GI tract. They may start in what are called the interstitial cells of Cajal, or ICCs. These cells are sometimes called the pacemakers of the GI tract because they signal muscles to move food and liquid through. More common GI cancers, such as colon cancer, start in different cell types.
GISTs can start anywhere in or near the GI tract. About 60% start in the stomach and about 30% in the small intestine. The rest start in the esophagus, large intestine or, rarely, other parts. Most but not all GISTs are cancer.
Lower Gastrointestinal Anatomy
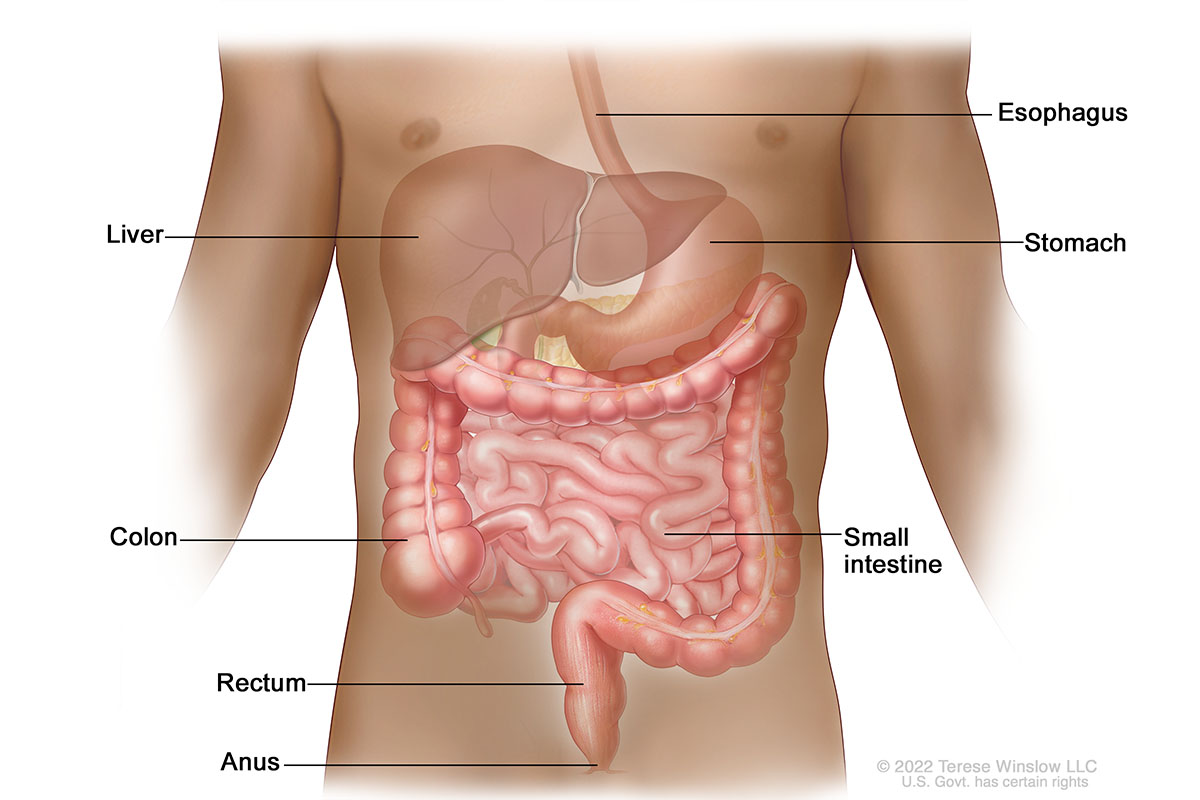
Who gets GISTs?
About 4,000 to 6,000 people are diagnosed with GISTs in the U.S. each year, according to the American Cancer Society. GISTs make up less than 1% of GI cancers.
GIST survival rates
A key concept in understanding survival is five-year relative survival rate. This is the percentage of people alive five years after they were diagnosed, compared with the general population. (It doesn’t count death from other causes.)
The five-year relative survival rate for GIST is 85%, according to the American Cancer Society. The rate is 95% if the GIST is caught before it has spread.
It's important to remember that survival rates are averages and can't predict the outcome for any one patient. It's also important to know that they are based on treatments available more than five years ago. Patients who are diagnosed now may have a better outlook.
GIST risk factors
Doctors don’t fully understand what causes GISTs, but they have identified risk factors that include:
- Age: Most patients are older than 50, though these tumors can occur at any age.
- Gender: Men are at slightly higher risk.
- Race: Black people are more likely to develop GISTs.
- Inherited conditions: Most cases are not inherited. However, a rare inherited condition called primary familial GIST syndrome, caused by a genetic mutation, puts family members at higher risk. OHSU offers expert genetic testing and risk assessment to help you identify and manage risk.
Symptoms of GISTs
Symptoms of gastrointestinal stromal tumors include:
- Blood in stool or vomit
- Belly pain, possibly severe
- Swollen belly or lump in belly
- Fatigue
- Painful swallowing
- Loss of appetite, or feeling full after eating very little
- Weight loss
Locations
Knight Cancer Institute, South Waterfront
Center for Health & Healing, Building 2
3485 S. Bond Ave.
Portland, OR 97239
Free parking for patients and visitors
Refer a patient
- Refer your patient to OHSU.
- Call 503-494-4567 to seek provider-to-provider advice.
Cancer clinical trials
Clinical trials allow patients to try a new test or treatment.
Results show promise

Learn about promising findings of Dr. Michael Heinrich’s work to test a GIST medication in clinical trials.
Read more
Learn more about OHSU Knight Cancer Institute treatments:
Stay informed
News: Read about research breakthroughs, patient care and many other topics on our OHSU News site.
Connect with us
GIST diagnosis
Your care team will ask you about your symptoms and medical history. We will also do a thorough physical exam to check for lumps or signs of tenderness or swelling. We may recommend tests such as:
Imaging tests: These noninvasive tests provide detailed images of your digestive tract. Common tests include:
- CT (computed tomography) scan
- MRI (magnetic resonance imaging) scan
- PET (positron emission tomography) scan
Endoscopic ultrasound: We guide an endoscope (a long, thin tube with a light and camera) down your throat. This enables us to see your esophagus, stomach and the first part of your small intestine. An ultrasound probe at the tip creates images. Our interventional endoscopists (gastroenterologists with special training) do hundreds of these a year. Patients are kept comfortable, usually with deep sedation under an anesthesiologist’s supervision.
Biopsy: We remove a small tissue sample, typically with a thin needle during an endoscopic ultrasound. The ultrasound helps guide the needle, ensuring precision. A type of doctor called a pathologist uses a microscope to check the tissue for cancer cells.
GIST stages
The stage of your GIST plays an important role in treatment decisions. Your care team will determine the stage based on:
- Tumor size
- Whether the cancer has spread to lymph nodes or distant parts of your body
- How fast cancer cells are growing and dividing (a measure called mitotic rate)
Here are the stages for the most common GIST, one that starts in the stomach or, rarely, in a layer of fatty abdominal tissue called the omentum. Read more on the American Cancer Society website.
Tumor Sizes

Stage I: The tumor has not spread to nearby lymph nodes, and mitotic rate is low.
- Stage IA: The tumor is no larger than 5 centimeters.
- Stage IB: The tumor is larger than 5 centimeters but not larger than 10 centimeters.
Stage II: The cancer has not spread to nearby lymph nodes. In addition, the tumor is no larger than 5 centimeters, and the mitotic rate is high. Or the tumor is larger than 10 centimeters, and the mitotic rate is low.
Stage III: The cancer has not spread to nearby lymph nodes, and the mitotic rate is high.
- Stage IIIA: The tumor is larger than 5 centimeters but not larger than 10 centimeters.
- Stage IIIB: The tumor is larger than 10 centimeters.
Stage IV: The cancer has spread to nearby lymph nodes and/or to distant parts of the body.

-
Surgery
-
- Robert L. Eil, M.D.
- Accepting new patients
-
- Sandy H. Fang, M.D., FACS, FASCRS (she/her)
- Accepting new patients
-
- Erin W. Gilbert, M.D., M.C.R., FACS
- Accepting new patients
-
- Daniel O. Herzig, M.D., M.B.A., FACS, FASCRS (he/him)
- Accepting new patients
-
- Kim C. Lu, M.D., FACS, FASCRS (he/him)
- Accepting new patients
-
- Skye C. Mayo, M.D., M.P.H., FACS
- Accepting new patients
-
- Rodney F. Pommier, M.D., FACS, FSSO
- Accepting new patients
-
- Flavio G. Rocha, M.D., FACS, FSSO
- Accepting new patients
-
- Divya Sood, M.D.
- Accepting new patients
-
- V. Liana Tsikitis, M.D., M.B.A., M.C.R., FACS, FASCRS (she/her)
- Accepting new patients
-
- Stephanie G. Wood, M.D., FACS
- Accepting new patients
-
-
Medical oncology
-
- Kelly Jo Hamman, M.S., CGC
- Accepting new patients
-
- Michael C. Heinrich, M.D.
- Accepting new patients
-
- Charles D. Lopez, M.D., Ph.D.
- Accepting new patients
-
-
Medical genetics
-
- Kelly Jo Hamman, M.S., CGC
- Accepting new patients
-
GIST treatment
Your care team will work with you to recommend a treatment plan for your specific needs and wishes.
Targeted therapy
Targeted therapy treats the cancer using medication. You may be a candidate for Gleevec, a daily pill developed through groundbreaking work by Knight Cancer Institute physician and scientist Brian Druker, M.D.
Gleevec works to shrink tumors by blocking proteins GISTs need to grow. In about two out of three patients, the tumors shrink by 50% or more. Your care team may recommend Gleevec before surgery to shrink the tumor or after to help keep cancer from spreading or returning.
Sometimes, tumors become resistant to Gleevec. In this case, you might receive additional medications, such as:
- Sunitinib (Sutent)
- Regorafenib (Stivarga)
- Ripretinib (Qinlock)
- Avapritinib (Avaykit)
The Knight Cancer Institute is leading several clinical trials of promising treatments for GISTs.
Surgery
Our surgeons have exceptional expertise in treating gastrointestinal cancers, including GISTs.
- Small tumor: If the tumor hasn’t spread, the cancer can often be entirely removed. A minimally invasive laparoscopic surgery with small incisions may be an option. Lymph nodes are rarely removed because, unlike in many other cancers, GISTs usually don’t spread to them.
- Large tumor: If the tumor is large or invading other organs, we may need to take out parts of these as well to remove as much of the cancer as possible.
GIST team
Learn more
- Read about our cancer registries, including a GIST Registry, which offer patients the opportunity to contribute to research and to receive updates.
- Look for a clinical trial for GIST patients.
- Gastrointestinal Stromal Tumors Treatment, National Cancer Institute
- Gastrointestinal Stromal Tumor (GIST), American Cancer Society
- Gastrointestinal Stromal Tumors, National Organization for Rare Disorders
- GIST Support International
- The Life Raft Group
- GIST Cancer Research Fund