Understanding Stem Cell Transplants
Stem cell transplants from bone marrow or blood offer lifesaving treatment. They are also taxing physically and emotionally.
It’s important to know:
- A transplant may enable doctors to destroy blood diseases and improve your body’s ability to produce healthy new blood cells.
- A transplant may use your cells or cells from a donor.
- Transplants with donor cells have the highest chance of success when donor cells closely match those of the patient.
- Transplant patients must devote weeks to treatment, with close monitoring.
- Your care team will carefully consider the risks and benefits of a transplant and discuss them with you.
What are stem cells?
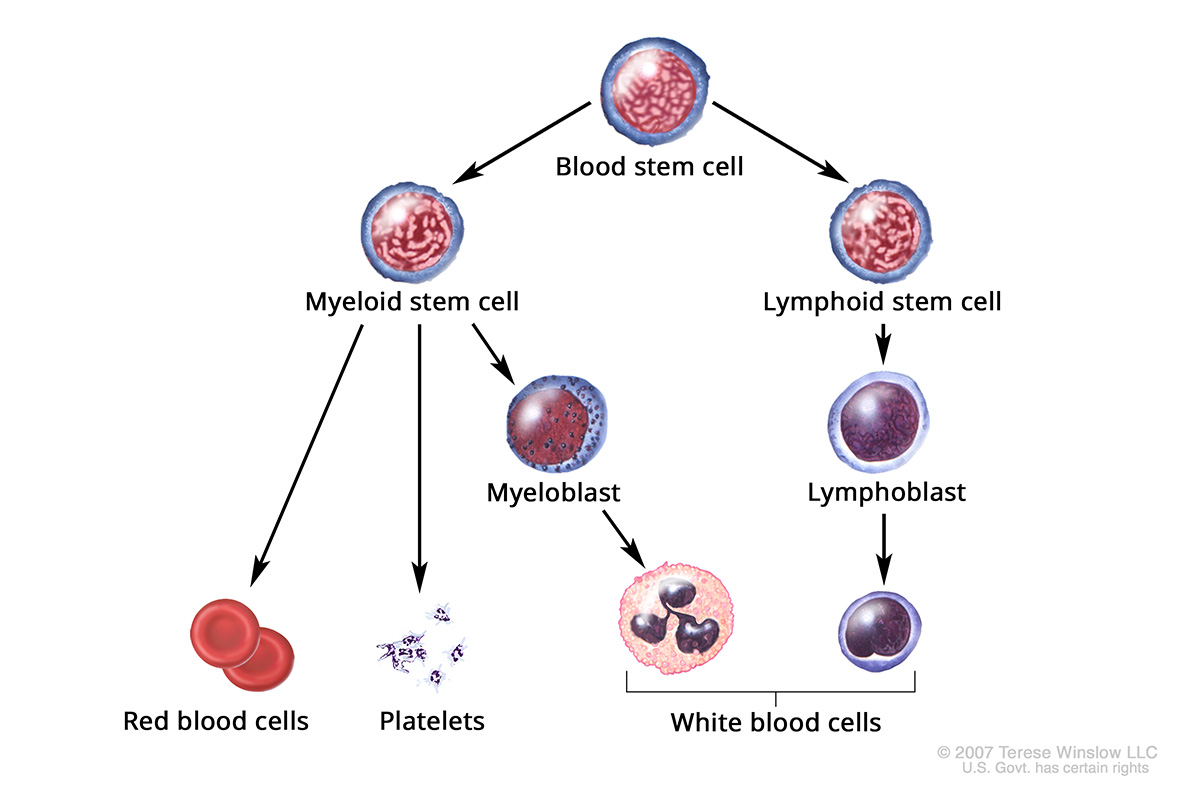
Blood cells are short-lived and must be replaced. Blood-forming stem cells (hematopoietic cells) divide and multiply. Some mature into one of three blood cell types:
- White blood cells that fight infection
- Red blood cells that carry oxygen throughout the body
- Platelets that help the blood clot
Stem cells are found in bone marrow, in the bloodstream and in umbilical cord blood. In the bloodstream, they are called peripheral blood stem cells (PBSCs). Stem cells from any of these sources can be used in transplants.
Blood-Forming Stem Cell
What are stem cell transplants?
With a stem cell transplant, a doctor gives you healthy replacement cells that help you fight infection and disease. Doctors most often use stem cell transplants to treat blood disorders and blood cancers that:
- Cause your bone marrow to make abnormal cells.
- Slow down cell production.
A transplant is like a blood transfusion. There are three types:
- Bone marrow transplant: Doctors collect stem cells from marrow with a hollow needle.
- Peripheral blood stem cell transplant: PBSCs are collected from blood drawn with a small needle.
- Umbilical cord blood: Stem cells are collected from umbilical cord blood.
For patients
Call 503-494-7999 to:
- Request an appointment
- Seek a second opinion
- Ask questions
Help and education:
Location
Knight Cancer Institute, South Waterfront
Center for Health & Healing, Building 2
3485 S. Bond Ave.
Portland, OR 97239
Free parking for patients and visitors
Refer a patient
- Refer your patient to OHSU.
- Call 503-494-4567 to seek provider-to-provider advice.
Kids and teens

Read more
Learn more about OHSU Knight Cancer Institute treatments:
During your stem cell treatment, you undergo a process called conditioning. Chemotherapy, radiation therapy or both are used to destroy cancer cells — and healthy cells that could keep your body from accepting transplanted cells.
New cells are added to your bloodstream with an IV. The cells collect in your bone marrow, where they produce new blood cells. Because conditioning leaves your immune system weak, you will need two to three weeks of monitoring.
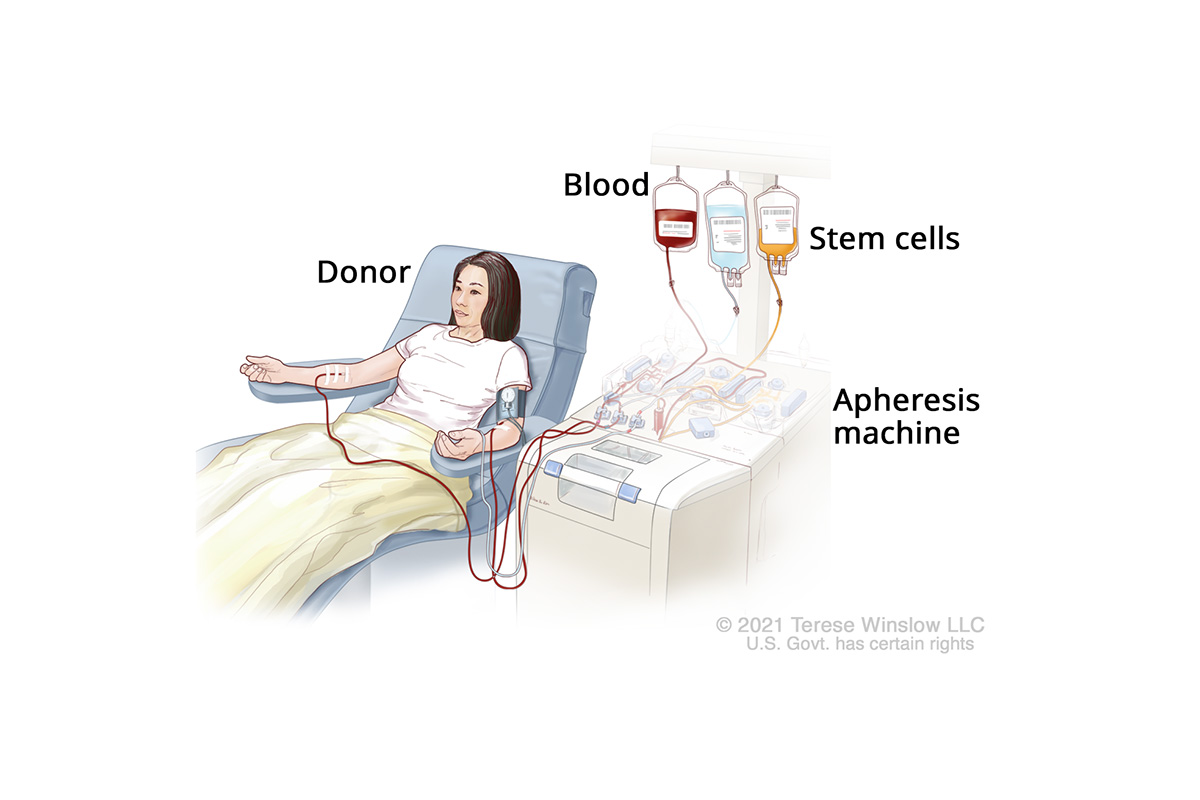
Step 1: Stem cells are removed from the donor.
The donor’s blood is drawn and run through an apheresis machine to extract stem cells.
Stem Cell Donor
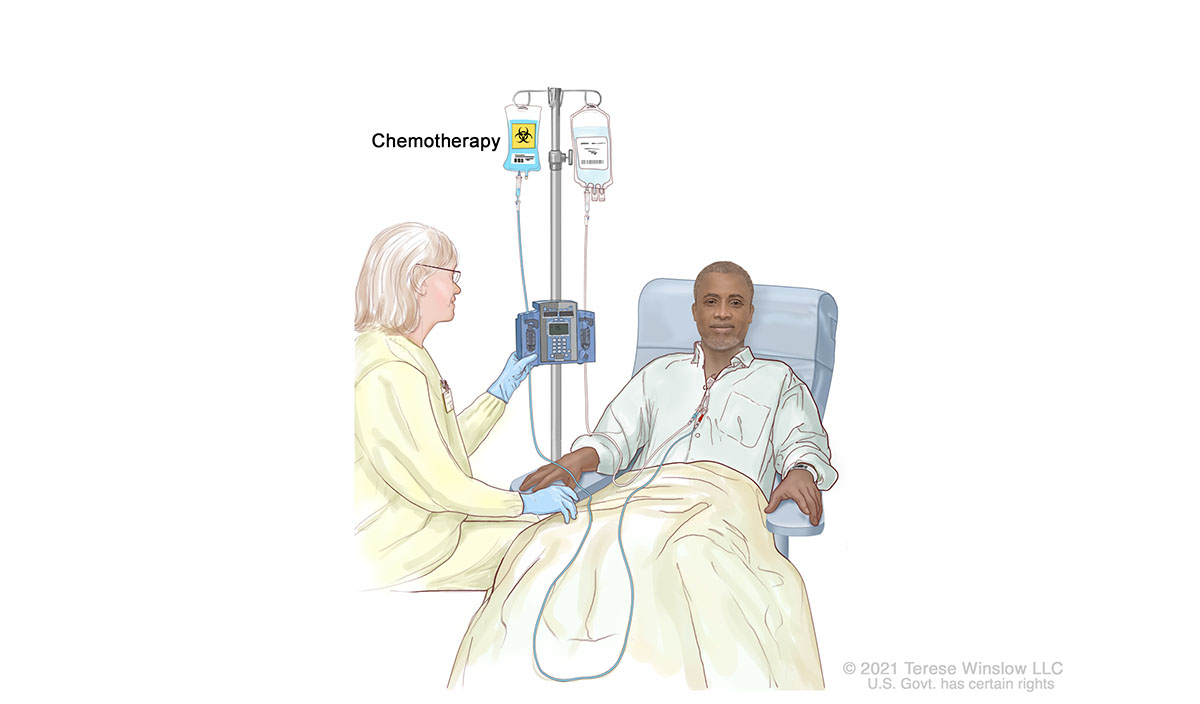
Step 2: Patient receives treatment to destroy blood-forming cells.
The patient has chemotherapy and/or radiation therapy to prepare for the new cells.
Stem Cell Transplant Preparation
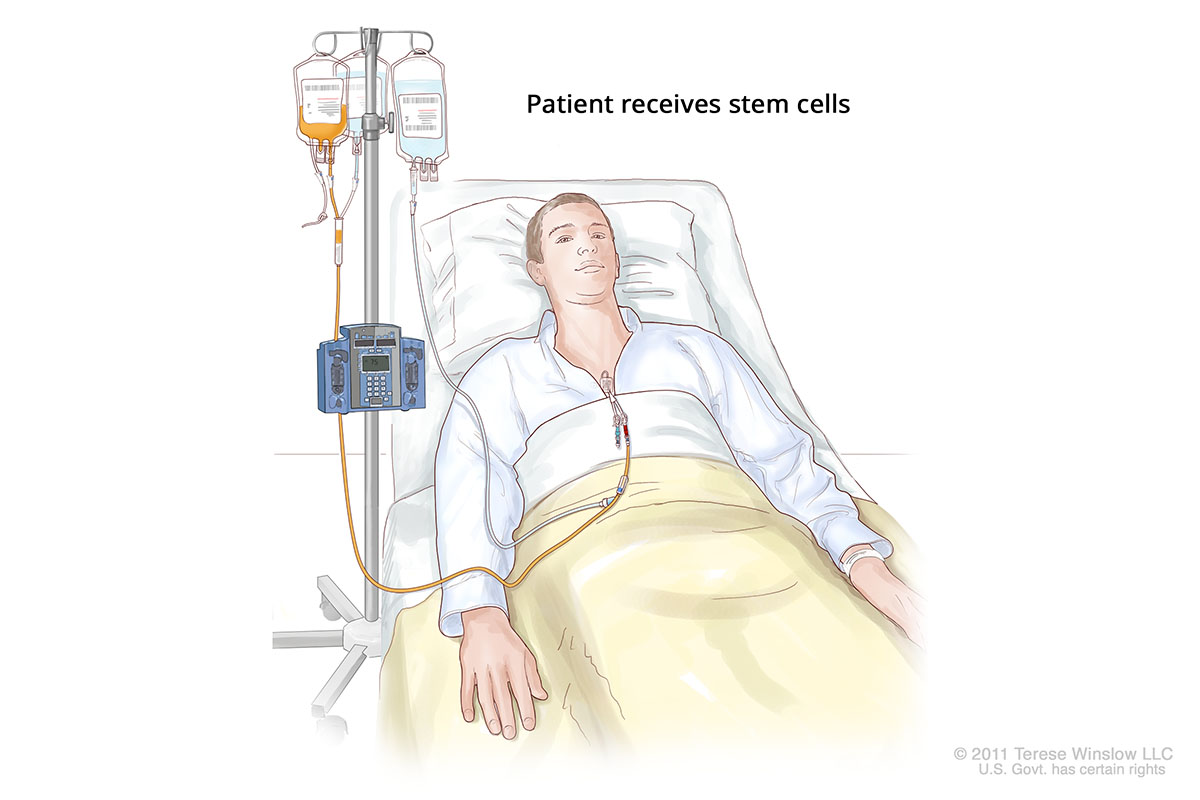
Step 3: Patient receives stem cells.
The patient receives donor cells in an IV. Note, this illustration depicts a patient with a chest port that allows providers to connect an IV without repeated needle sticks.
Stem Cell Recipient
Deciding on a transplant
At the OHSU Knight Cancer Institute, we consider every person with blood cancer for a stem cell transplant. It might be right for you if your cancer didn’t respond to other treatment or if your cancer came back after treatment.
Our providers meet at weekly gatherings called tumor boards to develop the best treatment options for each patient.
We will tailor recommendations to:
- Details of your disease
- Your individual condition, needs and wishes
- Details of the transplant type
Our transplant nurse navigator will be your first contact. This health care professional will provide information and resources, and help you understand the process. The navigator will also be your advocate and guide.
You’ll want to consider:
- Finances
- Health risks
- Time off work
- The need to be near OHSU for weeks
- Physical and emotional difficulties that come with having a transplant
What disorders do transplants treat?
Bone marrow/stem cell transplants may be an option to treat:
Other blood cancers and blood disorders:
- Amyloidosis
- Aplastic anemia
- Myelodysplastic syndromes
- Myeloproliferative neoplasms
- Paroxysmal nocturnal hemoglobinuria
Other conditions:
- Germ cell tumors
- Sarcoma
- Lupus
Types of stem cell transplant procedures
There are two main types of stem cell transplants, each with risks and benefits. OHSU is the only place in Oregon that offers allogeneic transplants.
Autologous transplant
What is it? This type uses your own stem cells. This eliminates the risk of your body rejecting donor cells or of donor cells attacking your body. A relapse may be more likely, though, because you won’t have healthy donated cells to attack any diseased cells that remain after conditioning.
How it works: Your care team draws blood and uses a machine to separate out stem cells. The stem cells are frozen. After the conditioning process, the cells are transplanted using an IV drip.
Allogeneic transplant
What is it? We use cells from a donor. Sometimes your own cells are too diseased to collect and reuse. Donor cells are more aggressive in killing any diseased cells left after conditioning. The risk is that they may aggressively target your healthy cells as well, a complication called graft-versus-host disease.
How it works: After the conditioning process, we transplant healthy donor cells using an IV drip. The donor cells help your body rebuild your immune system. A donor can be a relative or someone else whose marrow matches yours.
Allogeneic transplants include:
- Syngeneic transplants that use cells from a twin.
- Haploidentical transplants that use partial or imperfectly matched cells. OHSU is among the few hospitals in the country with the expertise to offer these.
- Cord blood transplants that use cells from umbilical cord blood collected and stored right after delivery.
What should you expect during transplant therapy?
- First contact: Our transplant nurse navigator contacts you to offer information, resources and a general treatment timeline.
- First appointment: We discuss whether you might benefit from a transplant, then begin the process of getting insurance authorization.
- Evaluation: You have testing that helps us better understand if a transplant will work.
- Conditioning: You receive chemotherapy and/or radiation therapy to kill cancer cells and bone marrow cells.
- Transplant: We transplant the cells, and they begin to multiply in your bone marrow.
- Recovery and rehabilitation: Your care team will closely monitor you, usually in the hospital, for two to three weeks as you wait for your new cells to begin producing healthy blood cells.
Stem cell transplant risks
As with any procedure, transplants involve risks. Your care team will discuss these with you in detail.
Infection: Chemotherapy and radiation therapy weaken your immune system. You are at high risk of infection for up to six weeks until your new cells make healthy blood cells. Your care team will keep you in a safe environment with protection against airborne germs. You will receive safety instructions for going home.
Low platelets: Your platelets will be low for three or more weeks. We will take great care to help you avoid injury or bleeding. Some patients may need a blood transfusion to replace platelets.
Pain: Mouth or throat pain is a common side effect of chemotherapy and radiation therapy. It may cause difficulty eating or swallowing for a few weeks.
Graft failure: Transplant (graft) failure occurs when the body rejects the donor cells. This is rare with stem cell transplants but more common when HLA types are poorly matched.
Graft-versus-host disease: This happens when transplanted cells from the donor attack the recipient’s tissue and organs. This common complication can range from mild to life-threatening.
Organ damage: Chemotherapy and radiation can leave lasting damage. We’ll monitor you closely for signs of any problem.
Infertility: The chemotherapy and radiation therapy used before transplants typically result in infertility. OHSU fertility experts can offer options before your treatment begins to preserve your ability to have children.
Physical and emotional effects
Transplants are difficult. They require weeks in or near the hospital, away from work and regular activities. Our cancer social workers and other experts can provide support to you and your family before, during and after treatment.
Learn about the wide array of support services and other resources for patients and families.
Donating bone marrow
OHSU has participated in Be The Match: The National Marrow Donor Program since 1996. This program helps people find a lifesaving marrow or PBSC donor. Donors must meet medical guidelines and should expect to spend 20 to 30 hours over four to six weeks to donate.
Testing for patients and donors
To find the closest match, doctors test the patient’s blood and a potential donor’s blood to find their human leukocyte antigen (HLA) type.
HLA markers
Everyone inherits a set of HLA markers from their parents. These markers, on the surface of almost all of your cells, tell your body which cells belong to you. The more matching markers you and a donor have, the better your chances of a successful transplant.
OHSU has success with haploidentical transplants, in which as few as half the markers match. This makes transplants an option for almost everyone.
Learn more about donating
Find more information about the donation process:
- On our Preparation and Treatment page
- From Be the Match