Understanding Lymphoma
Lymphoma is a blood cancer that begins in lymphocytes, a type of white blood cell that helps the body fight infection. It’s important to know:
- Doctors divide the disease into non-Hodgkin lymphoma and Hodgkin lymphoma.
- Both types occur in children and adults.
- Lymphoma has nearly 70 subtypes, some aggressive and some slow, some common and some rare.
- Both main types of lymphoma are highly treatable, especially when caught early.
What is lymphoma?
Lymphoma occurs when abnormal lymphocytes multiply and grow. Lymphocytes are the body’s infection-fighting cells. They produce proteins called antibodies that attach themselves to foreign or diseased cells to destroy them.
- Lymphocytes and the lymph system: Lymphocytes are part of the lymph system, a network of vessels (similar to blood vessels), glands and organs that power the immune system. The system circulates a clear fluid called lymph. This fluid carries lymphocytes through the body.
- Lymph nodes: Small glands in the system called lymph nodes filter the lymph to remove unwanted substances. These nodes often trap breakaway cancer cells. Doctors can remove and examine lymph nodes to see if and how far cancer has spread.
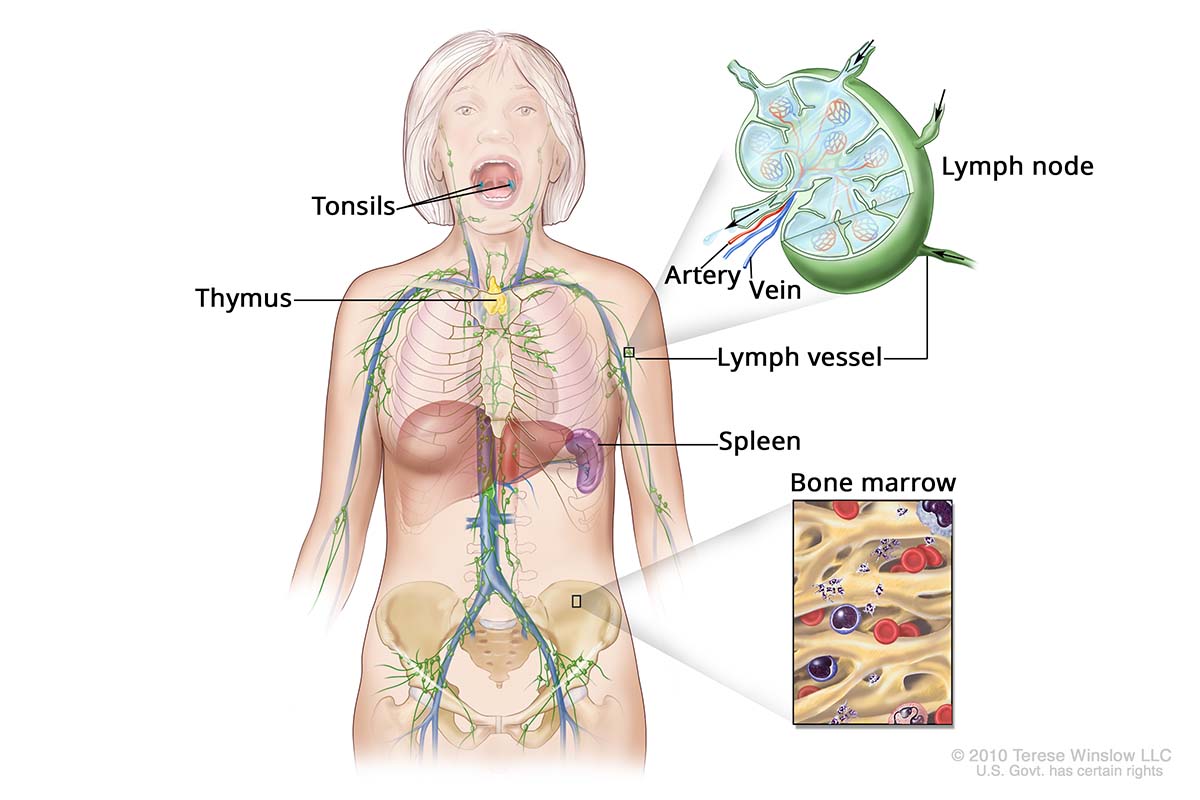
The Lymph System
Lymphocyte types
There are three main types:
- B cells, which typically make antibodies
- T cells, which typically destroy infected or abnormal cells
- Natural killer cells, also called NK cells, which destroy virus-infected cells
They are produced in:
- Bone marrow, tissue in the bone that also makes blood cells
- Lymph nodes, the bean-shaped glands that filter unwanted substances
- Spleen, an organ in the abdomen that is part of the immune system
- Thymus, a gland in the chest linked to the development of T cells
- Tonsils, two lymph nodes in the back of the throat
Lymphoma types
- Non-Hodgkin lymphoma, the most common type, has subtypes that range from slow-growing to aggressive.
- Hodgkin lymphoma is marked by the presence of large cancer cells called Reed-Sternberg cells.
Who gets lymphoma?
Non-Hodgkin lymphoma
About 79,000 new cases of non-Hodgkin lymphoma are diagnosed in the U.S. every year, according to the National Cancer Institute. Roughly 872,000 Americans are living with it.
Risk factors include:
- Age: More than three in four patients are 55 or older at diagnosis.
- Gender and race: White men are at higher risk.
- Health history: Risk increases if you have a weakened immune system from:
- HIV/AIDS
- Some genetic disorders
- Organ transplant
- Some autoimmune diseases
- Some infections
- Environmental exposure: Routine exposure to radiation, benzene and some weed-and insect-killing chemicals may increase risk.
Hodgkin lymphoma
About 8,900 new cases of Hodgkin lymphoma are diagnosed in the U.S. every year, according to the National Cancer Institute. Roughly 240,000 Americans are living with it.
Risk factors include:
- Age: Nearly one in three patients is age 20 to 34 at diagnosis. People younger than 20 account for about 1 in 8 cases, as do people in the 35-44 and 55-64 age groups.
- Gender: Men are at slightly higher risk.
- Family history: Having a parent, sibling or child with lymphoma increases risk.
- Health history: People with HIV (the virus that causes AIDS) or the Epstein-Barr virus (which causes mononucleosis) are at higher risk.
Lymphoma survival rates
A key concept in understanding survival is five-year relative survival rate. This is the percentage of people who are alive five years after they were first diagnosed, compared to the general population. (It doesn’t count death from other causes.)
Today, both types of lymphomas offer a positive outlook, especially when caught early.
Non-Hodgkin lymphoma: The five-year relative survival rate for non-Hodgkin lymphoma is 74%. If the cancer is confined to one site of the lymph system, the rate is 87%.
Hodgkin lymphoma: The five-year relative survival rate for patients with Hodgkin lymphoma is 89%. The rate rises to more than 92% for patients with cancer that is in only one site of the lymph system.
It’s important to know that survival rates are averages and can’t predict the outcome for any one patient.
Lymphoma symptoms
Lymphoma may have no symptoms, or signs may be similar to those of other health conditions. Doctors may find lymphoma through routine blood tests or when treating a separate condition. Symptoms may include:
- Swollen lymph nodes
- Fever, sweating or chills
- Cough or shortness of breath
- Fatigue
- Chest pain or pressure
- Unexplained weight loss or loss of appetite
- Frequent infections
- Bruising or bleeding easily
Lymphoma Signs and Symptoms

Types of non-Hodgkin lymphoma
Non-Hodgkin lymphoma isn’t one disease. It’s a group of more than 60 blood cancers with similar traits. Doctors describe NHL in two ways:
Cell type:
- B-cell lymphoma accounts for 90% of cases.
- T-cell lymphoma accounts for about 10% of cases.
- NK-cell lymphoma makes up less than 1% of cases.
How fast they grow and spread:
- Aggressive lymphomas make up about 60% of cases:
- Burkitt lymphoma is a rare cancer that starts in B cells.
- Central nervous system (CNS) lymphoma starts in the brain or spinal cord.
- Diffuse large B-cell lymphoma is the most common NHL that affects B cells.
- Mantle cell lymphoma (MCL) is a rare B-cell type cancer.
- Peripheral T-cell lymphomas are a group of rare NHLs that start in mature T cells.
- Slow-growing (indolent) lymphomas include:
- Small lymphocytic lymphoma (SLL) and chronic lymphocytic leukemia (CLL) are the same disease, but SLL refers to disease in the lymph nodes. CLL refers to disease in the bloodstream (leukemia) and bone marrow.
- Cutaneous T-cell lymphoma affects the skin. It is caused by mutated T cells.
- Follicular lymphoma is the most common indolent NHL that affects B cells.
- Marginal zone lymphoma (MZL) affects B cells in certain spleen and lymph node tissue.
- Mucosa-associated lymphoid tissue (MALT) lymphoma is a B-cell lymphoma that develops in the mucous membranes that line the body’s organs.
- Lymphoplasmacytic lymphoma (Waldenstrom macroglobulinemia) leads to a buildup of the macroglobulin protein (antibody).
Types of Hodgkin lymphoma
Hodgkin lymphoma occurs when abnormal lymphocytes outnumber normal white blood cells, leaving the immune system less able to fight infection. It can be divided into two categories:
- Classical Hodgkin lymphoma is identified by Reed-Sternberg cells. It accounts for 95% of cases. It has four subtypes:
- Nodular sclerosis, the most common subtype, in which lymph nodes have scar tissue.
- Mixed cellularity, the second-most-common subtype, most often found in people with HIV.
- Lymphocyte-rich lymphoma, with scattered Reed-Sternberg cells.
- Lymphocyte-depleted lymphoma, the rarest form, usually diagnosed at an advanced stage.
- Nodular lymphocyte-predominant Hodgkin lymphoma lacks Reed-Sternberg cells. Instead, a type of B cell sometimes called popcorn cells mark this subtype.
Lymphoma staging
Doctors use staging to measure how fast and how much the cancer is spreading. Staging is based on a physical exam, scans and analysis of tissue samples (biopsy). Doctors also consider fever, weight loss, tumor size, age, gender and other factors.
At OHSU, your care team will use the Lugano classification system, which divides non-Hodgkin and Hodgkin lymphoma into limited stage or advanced stage. The E designation means cancer affects tissue outside the lymph system.
Limited stage
Stage I: Cancer is in one lymph site (a set of lymph nodes, the thymus or the spleen, for example).
Stage IE: Cancer affects one site outside the lymph system but no lymph nodes.
Stage II: Cancer affects two or more lymph node regions, with all the regions above or all below the diaphragm.
Stage IIE: Cancer has grown from a lymph node area into an organ outside the lymph system. Other lymph nodes on the same side of the diaphragm may have cancer.
Stage II bulky: This definition varies by lymphoma type but indicates a larger tumor that may need more aggressive treatment. In some cases, it’s considered to be in the advanced stage. For Hodgkin lymphoma, a bulky tumor is wider than one-third of the chest or at least 10 centimeters across.
Advanced stage
Stage III: Cancer extends to lymph node regions above and below the diaphragm, or above the diaphragm but involving the spleen.
Stage IV: Cancer has widely spread to one or more organs outside the lymph system, without direct invasion. Lymph nodes may or may not be affected. Lymphoma is also Stage IV if it has spread to cerebrospinal fluid (the liquid that bathes the brain and spinal cord) or bone marrow.
Learn more
- Lymphoma, American Cancer Society
- Lymphoma, Blood Cancer United
- Lymphoma, National Cancer Institute
- Hodgkin Lymphoma, American Cancer Society
- Non-Hodgkin Lymphoma, American Cancer Society
- Understanding Lymphoma Lymphoma Research Foundation
Locations
Knight Cancer Institute, South Waterfront
Center for Health & Healing, Building 2
3485 S. Bond Ave.
Portland, OR 97239
Free parking for patients and visitors
Refer a patient
- Refer your patient to OHSU.
- Call 503-494-4567 to seek provider-to-provider advice.
Cancer clinical trials
Clinical trials allow patients to try a new test or treatment.
Kids and teens

Read more
Learn more about OHSU Knight Cancer Institute treatments: