Understanding Esophageal Cancer
Esophageal cancer is a rare condition of the digestive system. It’s important to know:
- Esophageal cancer is up to four times more common in men.
- Chronic gastroesophageal reflux disease, or GERD, is a risk factor for the most common type of esophageal cancer in the U.S.
- Heavy smoking and drinking are risk factors for the second most common type.
- This cancer is uncommon overall, but the most common type has risen dramatically in recent decades.
- Specialized care makes it possible to catch the disease’s early signs, giving you a better chance for successful treatment.
What is esophageal cancer?
Your esophagus is the muscular tube that connects your throat (larynx) to your stomach. When you swallow food, layers of muscle move it down the esophagus to the stomach.
Esophageal cancer happens when abnormal cells form in the tissue that lines the esophagus. As the cells multiply, cancer invades layers of the esophagus and may spread to other parts of the body.
Anatomy of the Upper Digestive System
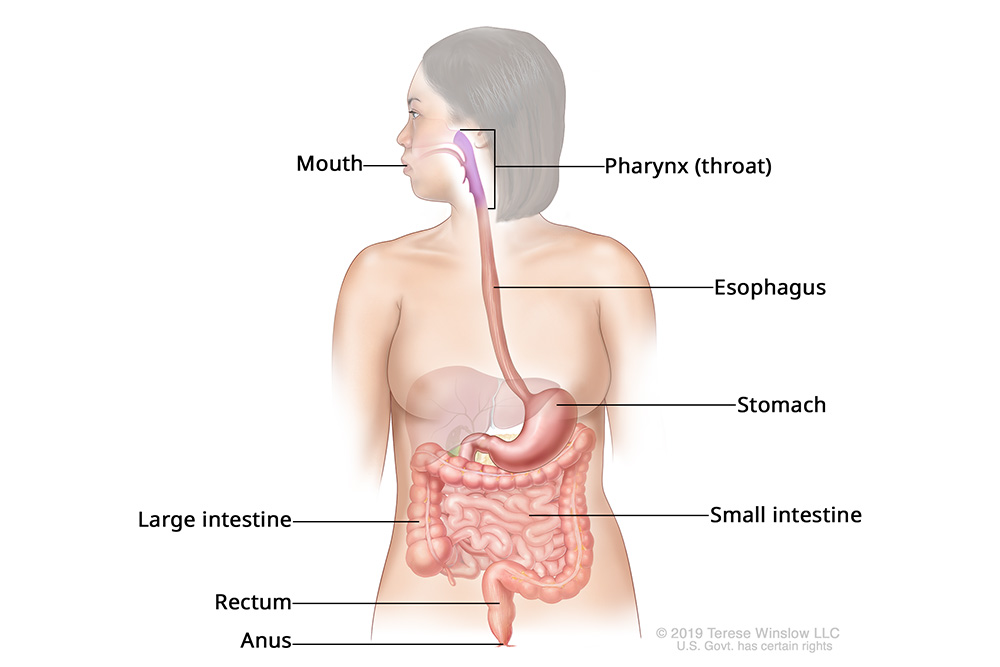
Who gets esophageal cancer?
About 22,000 people in the U.S. are diagnosed with esophageal cancer every year, according to the National Cancer Institute. Roughly 55,000 people in the U.S. are living with the condition.
GERD
In GERD, also known as acid reflux, stomach acid travels up into the lower part of the esophagus. GERD is one of the biggest risk factors for esophageal adenocarcinoma. Still, most people with GERD will not go on to develop cancer.
GERD risk factors: You are more likely to have reflux if you are overweight or have a hiatal hernia. In this condition, part of the stomach bulges up through an opening (the hiatus) in the diaphragm (the muscle between the abdomen and chest). The hernia can weaken muscles in the lower esophagus.
Barrett’s esophagus: Frequent reflux can damage the lining of the esophagus. In some people, cells in this area die and are replaced with cells more like the ones in your stomach. This condition, called Barrett’s esophagus, increases your risk of esophageal cancer.
Other risk factors for esophageal cancer
- Age: Esophageal cancer is more common in people ages 55 to 84.
- Gender: It’s three to four times more common in men.
- Alcohol use: Regularly drinking alcohol, including beer and wine, increases risk.
- Tobacco use: Smoking and any other use of tobacco irritates the lining of the esophagus and may increase risk.
- Diet: Not getting enough fruits, vegetables and certain vitamins can make esophageal cancer more likely.
- Health history: Conditions affecting the esophagus, such as achalasia, increase your risk. In people with achalasia, the muscles at the bottom of the lower esophagus make it difficult for food to pass. People with a history of cancers linked to smoking, such as lung cancer, also may have a higher risk of esophageal cancer.
Esophageal cancer outcomes
The key to successful treatment for esophageal cancer is early detection.
A key concept in understanding survival is five-year relative survival rate. This is the percentage of people who are still alive five years after they were first diagnosed, compared to the general population. (It doesn’t count death from other causes.)
If esophageal cancer is found before it spreads, the five-year relative survival is 48%. If the cancer has already spread at the time of diagnosis, the survival rate is more discouraging, but treatment options are still available to help you live longer and better.
Remember that survival are averages and can’t predict the outcome for any one person. They are also based, by definition, on the treatments that were available five or more years ago, and don't reflect recent improvements.
Signs of hope: At the Knight Cancer Institute, world-class researchers are dedicated to finding new ways to detect cancer early.
Quality of life: While esophageal cancer sometimes cannot be cured, treatment can keep you comfortable and give you time to do things you want to do. You might set goals such as taking a special trip. Maybe you hope to see a child or a grandchild marry or graduate.
At the Knight Cancer Institute, your goals become our goals.
Your team is devoted to extending and improving your life regardless of your long-term outlook.
Esophageal cancer symptoms
You may not notice symptoms in early stages. As the disease gets worse, the tumors grow and make it difficult for the esophagus to do its job. Some symptoms are similar to those of other conditions, such as reflux and achalasia.
Symptoms include:
- Difficulty swallowing
- Choking while eating
- Heartburn or indigestion
- Hoarse voice that does not go away
- Pain in your throat or upper chest
- Vomiting
- Coughing up blood
- Black, tarlike stools
If you have these symptoms, especially if they don’t get better, it’s important to talk with your doctor.
Screening for esophageal cancer
If you face a higher risk for esophageal cancer, such as having Barrett’s esophagus, regular testing helps detect even the slightest change. Our team may do screening tests such as an upper endoscopy.
In this procedure, we look at the lining of your esophagus with an endoscope — a thin, flexible tube with a camera at the tip. Your doctor guides the endoscope through the throat into the esophagus. You will be sedated.
Types of esophageal cancer
- Adenocarcinoma: This is the most common type in the U.S. It starts in the mucus-producing cells that line the surface of the esophagus. Adenocarcinoma often develops in the lower esophagus near the stomach. It may also occur where the esophagus meets the stomach, an area called the gastroesophageal junction. Adenocarcinomas that form there are not technically esophageal cancer but are treated similarly.
- Squamous cell carcinoma: This type often starts higher in the esophagus, near the chest and neck. Most of these cases in the U.S. are linked to a history of smoking and drinking.
Stages of esophageal cancer
Your doctors will assign a stage to your cancer. The stage indicates how far it has advanced. This helps doctors recommend the most effective treatments.
Staging takes into account factors such as:
- What the cancer cells look like under a microscope.
- Whether the cancer has grown through the wall of the esophagus.
- Whether it has spread to lymph nodes (bean-size structures that play a role in the immune system) or beyond.
This is a simple description of staging for adenocarcinoma of the esophagus, the most common type. Find a more detailed outline at the American Cancer Society.
Stage IIA Adenocarcinoma of the Esophagus
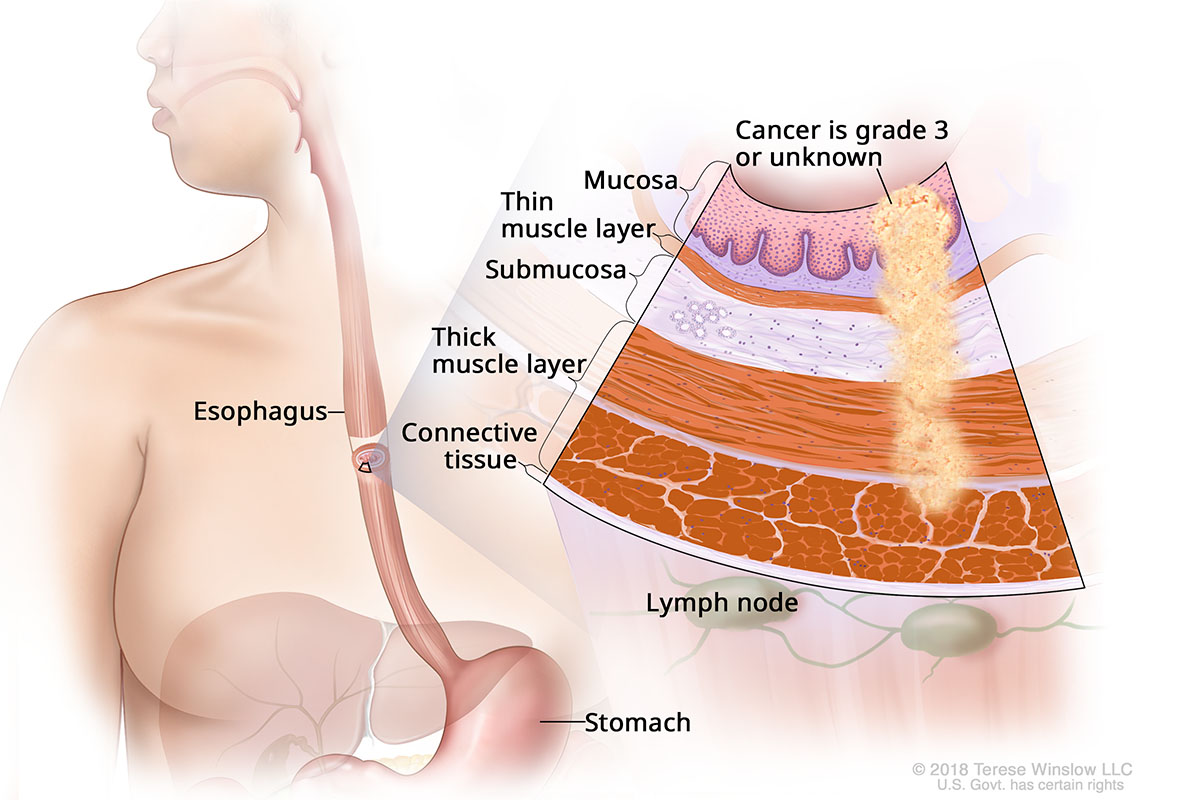
- Stage I: The cancer has grown into layers below the surface of the esophagus but hasn’t spread to any lymph nodes or distant organs.
- Stage II: The cancer invades more deeply into layers of the esophagus and may have spread to one or two nearby lymph nodes.
- Stage III: The cancer has spread as far as the outer layer of the esophagus and to as many as six nearby lymph nodes. Or it has spread to the diaphragm or to tissue covering the lungs or heart, and to as many as two lymph nodes.
- Stage IV: The cancer affects as many as six nearby lymph nodes; and the diaphragm, lung or heart coverings; or vital structures such as the windpipe or spine. Or it has spread to layers of the esophagus and to seven or more lymph nodes. Or it has spread to distant lymph nodes or organs.
Learn more
- ECEF: Esophageal Cancer Education Foundation
- Esophageal Cancer, U.S. National Library of Medicine
- Esophageal Cancer Treatment, National Cancer Institute
- Esophagus Cancer, American Cancer Society
Location
Knight Cancer Institute, South Waterfront
Center for Health & Healing, Building 2
3485 S. Bond Ave.
Portland, OR 97239
Free parking for patients and visitors
Refer a patient
- Refer your patient to OHSU.
- Call 503-494-4567 to seek provider-to-provider advice.
Read more
Learn more about OHSU Knight Cancer Institute treatments: