Stephen Back Brain Regeneration Lab

Regeneration and repair in the developing and aging brain
The Back Lab develops novel strategies to promote regeneration and repair after injury to the developing and adult brain. Our work spans from premature infants to adults with dementia and focuses on the fundamental biological processes that govern white and gray matter development, injury and recovery.
One major focus of the lab is neurological disorders that cause cerebral white matter injury (WMI) and disturbances in myelination. We study cerebral palsy in survivors of premature birth, multiple sclerosis and vascular dementias. All these disorders share mechanisms in which aberrant glial responses and extracellular matrix signaling arrest oligodendrocyte maturation and prevent effective remyelination. By integrating human pathology with advanced experimental models, we develop novel molecular strategies to restore myelin and improve motor and cognitive function.
We also study how hypoxia disrupts gray matter maturation in disorders like maternal sleep apnea or apnea of prematurity. We are finding that gray matter is markedly more resistant to injury than white matter but is very sensitive to low oxygen exposures. Hypoxia alone can trigger profound disturbances in neuronal maturation and synaptic development that persist into adulthood. Our goal is to define novel causes of chronic neurobehavioral disabilities in survivors of premature birth as they become adults. Our findings guide new preventive and therapeutic approaches in maternal and neonatal care.
On this page you can:
Accomplishments
The Back Lab has made foundational discoveries that redefine how white and gray matter vulnerability and repair are understood from prematurity to aging. We have long-standing funding from the NIH (NINDS and NHLBI) including recent support from NIA for our dementia studies. Our accomplishments include:
- Defining the role of maturation dependent vulnerability of the oligodendrocyte lineage to oxidative stress and hypoxia-ischemia
- Discovering that white matter injury in the developing and aging brain sustains myelination failure due to maturation arrest of oligodendrocyte progenitors.
- Identifying that white matter lesions generate specific sizes of hyaluronic acid and disrupt the maturation of oligodendrocyte progenitors
- Identifying that mild to moderate low oxygen exposure to the preterm gray matter can permanently disrupt the maturation of key neuronal populations in diverse gray matter regions
- Defining a novel role for microglial ferroptosis in white matter lesions in Alzheimer’s disease and vascular dementia
News
- Study implicates enzyme in neurodegenerative conditions
- JNeurosci Spotlight: Useful Genetic Mouse Lines
- Dr. Philip Adeniyi joins African Brain Journal editorial board
- OHSU scientists discover new cause of Alzheimer’s, vascular dementia
- OHSU physician-scientist pioneers research to better understand maternal sleep apnea
Research Projects
At the Back Lab, our approach is multidisciplinary and technology-forward. We integrate cellular and molecular biology, electrophysiology, physiology, pharmacology, neuropathology, quantitative morphometry and stereology, advanced microscopy and high-field MRI. We use human tissues and unique animal models to link basic science with human disease.
As part of the OHSU neuroscience community, one of the most highly NIH-funded programs in the United States, we benefit from a deeply collaborative and translational research environment. By combining rigorous human pathology with innovative experimental platforms, we aim to redefine how white and gray matter injury is understood and treated across the lifespan.
Cerebral gray matter dysmaturation in preterm brain injury
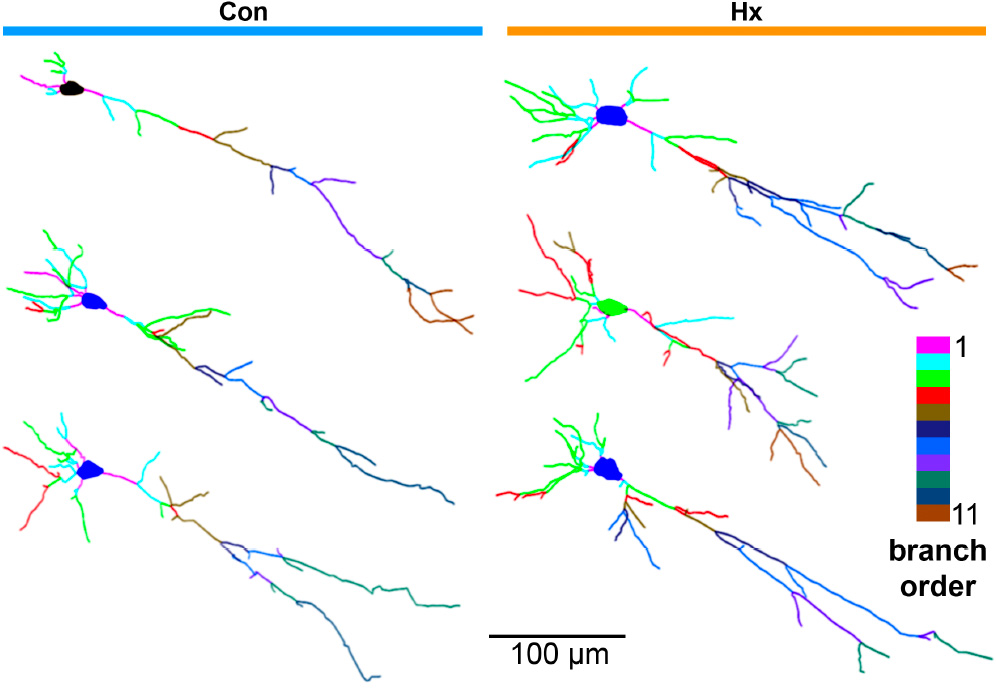
Learn more in Riddle et al., Journal of Neuroscience, 2026.
We are defining how hypoxia disrupts molecular pathways and increases the risk for neurodevelopmental disorders like autism and mental illness. For former preterm infants, this could lead to improved neurobehavioral outcomes. Read about our 2019 study that showed lack of oxygen doesn't kill infant brain cells.
Preterm infants with white matter injury (WMI) often show diffuse reductions in cortical and subcortical gray matter growth. Our work challenged the longstanding assumption that this impairment results from widespread neuronal death. Instead, we demonstrated that transient hypoxia alone, even without significant oxidative damage or neurodegeneration, can chronically disrupt neuronal maturation.
In small and large animal models, neurons in the cerebral cortex, subplate and hippocampus survive hypoxia but develop persistent structural and functional abnormalities. After as little as 30 minutes of moderate hypoxia, immature neurons show abnormal dendritic arborization and impaired synaptic activity. After one month, CA1 hippocampal neurons show long-lasting disturbances in synaptic activity and cellular mechanisms essential for learning and memory. Our findings redefine preterm gray matter injury as a disorder of neuronal dysmaturation rather than degeneration.
This suggests that we can treat preterm brain injury, that is assumed to be untreatable, after the early phase of injury. Therapies that promote dendritic maturation may restore circuit development and improve long-term neurological outcomes.
Supported by NHLBI, we developed a novel preclinical model of repetitive fetal hypoxia in preterm sheep that mimics maternal sleep apnea. Funded by NINDS, we use preterm-equivalent mouse models to define novel molecular pathways that may explain neuronal dysmaturation. This work is also supported by the Sharma family.
These studies are led by Art Riddle, M.D., Ph.D., and James Maylie, Ph.D., working with Zsolt Bagi, M.D., Ph.D., at the Medical College of Georgia.
Molecular mechanisms of myelination failure
Most cerebral white matter injury (WMI) can’t be seen during its acute phase, so early intervention is often not possible. Our lab focuses on therapies that promote regeneration and remyelination in chronic white matter lesions. Therapeutic strategies suggested by our work could help treat preterm WMI, multiple sclerosis and vascular dementias.
We identified the extracellular matrix as a central regulator of myelination failure. In chronic human WMI, hyaluronic acid (HA) and its receptor CD44 are highly enriched. Working with Larry Sherman, Ph.D., we showed that reactive astrocytes generate high–molecular weight forms of HA that blocks maturation of late oligodendrocyte progenitors (preOLs).
We also discovered that white matter lesions process HA into bioactive fragments, including a 210 kDa fragment that selectively blocks remyelination. This fragment signals through a non-canonical TLR4–TRIF pathway and activates the transcription factor FoxO3. This blocks oligodendrocyte maturation even in the presence of pro-myelination signals. These findings suggest novel strategies to promote myelination.
These ongoing NINDS-funded studies are led by Taasin Srivastava, Ph.D. We are studying maturation-dependent responses to hypoxia-ischemia and the roles of TSG-6 in myelination disorders. In related studies, we are working with OHSU’s Larry Sherman, Ph.D., and Justin Dean, Ph.D., at the University of Auckland to test the effects of novel hyaluronidase inhibitors to promote repair of preterm brain injury.
This work is also supported by the Huebner family.
White matter injury in Alzheimer’s disease and vascular dementia
The Back Lab has extensive expertise in collecting and preserving human brain tissue. Working with C. Dirk Keene, M.D., Ph.D., at the University of Washington, we maintain a large collection of brain samples from autopsies of people with Alzheimer’s disease and vascular dementia. We also have brain tissue from autopsies of premature and term infants.
Over decades, we have developed immunohistochemical protocols that detect human molecules in specific cell types in both white and gray matter. These resources let us anchor research findings in human pathology.
Current studies focus on mechanisms of chronic white matter injury. We study changes in the extracellular matrix that cause myelination failure and regulation of cell death mediated by ferroptosis. Our findings could lead to new approaches to treat Alzheimer’s disease and vascular dementia.
Publications
Below are some of the Back Lab’s significant publications. Find the most recent publications by Dr. Stephen Back on PubMed.
TSG-6-mediated extracellular matrix modifications regulate hypoxic-ischemic brain injury
Journal of Neuroscience 2024
Srivastava T, Nguyen H, Haden G, Diba P, Sowa S, LaNguyen N, Reed-Dustin W, Zhu W, Gong X, Harris EN, Baltan S, Back SA.
A TLR-AKT-FoxO3 immune tolerance-like pathway disrupts the repair capacity of oligodendrocyte progenitors
Journal of Clinical Investigation 2018
Srivastava T, Diba P, Dean JM, Banine F, Shaver D, Hagen M, Gong X, Su W, Emery B, Marks DL, Harris EN, Baggenstoss B, Weigel PH, Sherman LS, Back SA.
Prenatal cerebral ischemia disrupts MRI-defined cortical microstructure via disturbances in neuronal arborization
Science Translational Medicine 2013
Dean JM, McClendon E, Hansen K, Azimi-Zonooz A, Chen K, Riddle A, Gong X, Sharifnia E, Hagen M, Ahmad T, Leigland LA, Hohimer AR, Kroenke CD, Back SA.
Arrested preoligodendrocyte maturation contributes to myelination failure in premature infants
Annals of Neurology 2012
Buser JS, Maire J, Riddle A, Nelson K, Gong X, Luo NL, Ren J, Nguyen T, Struve J, Sherman LS, Miller SP, Chau V, Hendson G, Ballabh P, Grafe MR, Back SA.
Histopathological correlates of MRI-defined chronic perinatal white matter injury
Annals of Neurology 2011
Riddle A, Dean JM, Buser JR, Gong X, Maire J, Chen K, Ahmad T, Cai V, Nguyen T, Kroenke CD, Hohimer AR, Back SA.
People
The Back Lab is a close-knit team of scientists and clinicians who work across projects and disciplines. We have been nicknamed the “dogma busters” for challenging assumptions in brain injury research.
We collaborate widely, publish rigorously quantitative work and support our trainees’ career development.
Principal investigator Stephen Back, M.D., Ph.D.
Dr. Stephen Back is a professor of pediatrics, neurology and anesthesiology-critical care medicine. A pioneer in developmental brain injury research, Dr. Back has been funded by the NIH since 1997. He was one of the first people at OHSU to receive a Javits Award from NINDS, in recognition of his studies in preterm brain injury.
-
- Stephen A. Back, M.D., Ph.D.
- Clyde and Elda Munson Professor of Pediatric Research
-
Appointments and titles
- Professor of Pediatrics, School of Medicine
-
Areas of interest
- Research on mechanisms of brain injury due to prematurity
Affiliated faculty
Art Riddle, M.D., Ph,D., is an assistant professor of pediatrics and neurology. He earned his doctoral degrees through the OHSU Neuroscience Graduate Program and completed his residency at Cincinnati Children’s Hospital. Dr. Riddle joined OHSU in 2019 as a postdoctoral scholar in neurophysiology, working with Dr. James Maylie. His research focus is the susceptibility of the preterm brain to hippocampal dysmaturation mediated by intermittent hypoxia.
-
-
Appointments and titles
- Assistant Professor of Pediatrics, Division of Neurology, School of Medicine
-
Areas of interest
- Research on brain injury in premature infants
- Neonatal neurology
- Inpatient neurology
-
Taasin Srivastava, Ph.D., is a research assistant professor in the department of pediatrics. He earned his Ph.D. in neurobiology at the University of Arkansas and worked with OHSU’s Dr. Tom Soderling before he joined the Back Lab. As a postdoctoral scholar in the Back Lab, he identified novel forms of hyaluronan that block oligodendrocyte progenitor maturation in the newborn and adult brain. His research focus is to define signaling mechanisms mediated by the proteoglycan TSG-6 that regulate susceptibility to stroke in preterm neonates and adults.
-
-
Appointments and titles
- Research Assistant Professor of Pediatrics, School of Medicine
-
Areas of interest
- Mechanisms of brain injury due to prematurity
- Extra cellular matrix (ECM) mechanisms that support neuro-protective outcomes
-
Philip Adeniyi, Ph.D., postdoctoral fellow

Dr. Philip Adeniyi completed his undergraduate and graduate training in Nigeria, earning a Ph.D. in anatomy and neurobiology from Olabisi Onabanjo University. In the Back Lab, Dr. Adeniyi transformed how neurodegeneration related to Alzheimer’s disease and vascular dementia is studied in human autopsy brain tissue. He developed a novel protocol that made it possible to interrogate the role of microglial ferroptosis in myelination failure in human white matter lesions. His current research is on the vulnerability of glial populations to ferroptosis in aging human white matter, and in a novel animal model of vascular dementia developed with Dr. Zsolt Bagi at Augusta University. Dr. Adeniyi is highly engaged in the international neuroscience community. He is the founder of Africa Young Scientists and has held leadership roles in the International Society of Neurochemistry.
Deepto Mizan, research assistant

Deepto Mizan’s first foray into neuroscience was during high school, doing electrophysiology studies with Dr. James Maylie at OHSU. Deepto holds a B.S. in neuroscience from UCLA. He joined the Back Lab’s vascular dementia and Alzheimer’s team in 2023 to pursue his interest in mechanisms of learning and memory and gain hands on experience. Deepto has been integral to studies to define the role of ferroptosis in degeneration of white matter glia in human autopsy cases and an animal model of vascular dementia.
Josh Mayeri, research assistant

Josh Mayeri holds a B.S. in animal sciences from Oregon State University, where he worked as a research assistant in the department of animal and rangeland sciences. Before college, he already had 12 years' experience raising goats and sheep. In the Back Lab, Josh studies the impact on fetal brain development of maternal intermittent hypoxia in pregnant sheep. In the coming year, he will divide his time between OHSU and OSU. At OSU, he will work with Dr. Jacob Raber on learning and memory studies in the adult offspring of controls and animals that sustained intermittent hypoxia during pregnancy. Josh aspires to a career as a large animal veterinarian.
Vikrant Sharma, M.S., research assistant

Vikrant Sharma first sought to join the Back Lab as a 12-year-old aspiring neuroscientist. During high school, he joined us as a volunteer. Vikrant holds a dual B.S. in biomedical engineering and electrical engineering from Boston University. He also holds a master’s degree in material science and engineering with a concentration in nanomaterials from BU, where he wrote a thesis on photoacoustic control of iPSC-derived cardiac organoids. As a research assistant since 2025, Vikrant analyzes complex data sets. He works with Dr. Riddle to analyze near-infrared spectroscopy studies in fetal sheep, and with Dr. Srivastava to analyze the extent of myelination of Nodes of Ranvier in mouse optic nerves. Vikrant aspires to a career as a dual M.D./Ph.D. clinician scientist.
Xi Gong, M.D., lab manager

Dr. Xi Gong trained as a plastic surgeon in China and has a master's degree in pathology research. She has been the Back Lab manager and lab mother since 2008. She has optimized immunohistochemical protocols that drive our morphometric and stereology studies, helping the Back Lab be well known for rigorous quantitative studies of brain injury in animal models and human tissues. Dr. Gong has invaluable experience with the optimal handling of delicate human autopsy tissues from both the preterm and aging brain. She has worked closely with postdocs and graduate students to accomplish the seemingly impossible with human tissue. Dr. Gong also ensures that members of the Back Lab are on track to advance their career, no matter their next step.
Contact us
Email Dr. Stephen Back at backs@ohsu.edu.
Donate
Support our work to develop therapies that restore the developing and aging brain.
Advancing Alzheimer’s research
Dr. Stephen Back reveals a form of cell death in the brains of patients with Alzheimer’s disease, thanks to donor funding.