Pancreatic Cancer

Pancreatic cancer starts when cells grow out of control in the pancreas, an organ that sits between the stomach and spine. The pancreas helps digest food and control blood sugar.
Pancreatic cancer has few or no early signs, making it harder to find and treat. Still, five-year survival rates have more than doubled since 2004.
At the Knight Cancer Institute, our expertise, large team and unmatched research give you the highest level of care. The National Cancer Institute recognizes the Knight as one of the best cancer centers in the nation.
We offer:
- A focus on “whole person” care for pancreatic cancer, recognized for excellence by the National Pancreas Foundation
- Nurse navigators who guide you through treatment
- Social workers, pain specialists and other experts to support you and your family
- Treatments you can’t find anywhere else in the Pacific Northwest
- Advances from OHSU’s Brenden-Colson Center for Pancreatic Care, which focuses on early detection and treatment
- Lifesaving therapies through our Pancreatic High-Risk Clinic
Quick links
What makes us different
National recognition: We’ve earned the National Cancer Institute’s highest designation for research excellence.
Advanced training: Our doctors completed fellowships — at least a year of post-residency training — at top cancer centers. They include the National Cancer Institute and Stanford, Duke and Johns Hopkins medical centers.
Commitment to research: We are one of the world’s few fully integrated pancreatic treatment and research centers. Our doctors and scientists in the Knight Cancer Institute and the Brenden-Colson Center work together to bring discoveries in the lab to patients as quickly as possible.
Early detection: Finding pancreatic cancer early is a core mission of the Brenden-Colson Center. The center has joined forces with the Knight Cancer Institute’s Cancer Early Detection Advanced Research Center to detect pancreatic cancer when it’s most curable. The center also offers a clinic for patients at high risk of pancreatic cancer.
What is pancreatic cancer?
Pancreatic cancer occurs when abnormal cells in the pancreas grow out of control.
The pancreas is shaped like a long, horizontal pear. It’s about 6 inches long and has three main parts: a head, body and tail.
Pancreas Anatomy
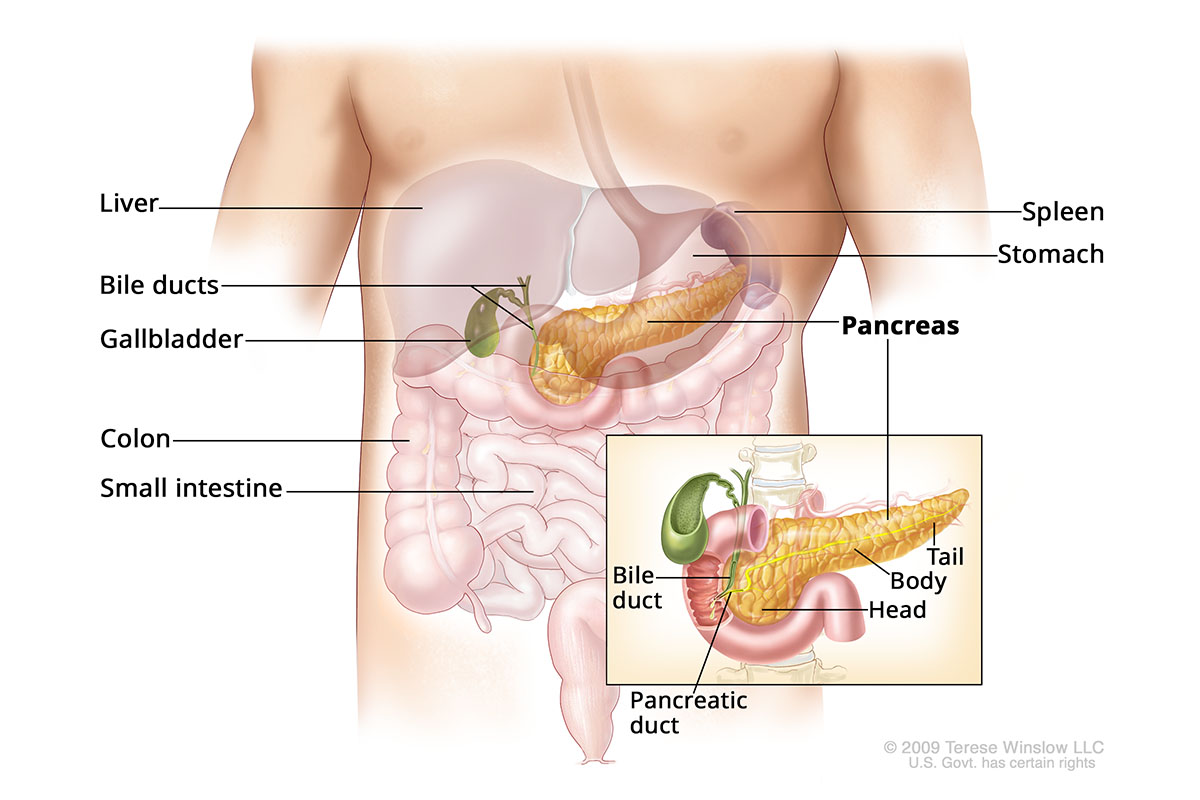
Who gets pancreatic cancer?
Pancreatic cancer accounts for about 3% of new cancer cases in the U.S. each year, according to the National Cancer Institute. That is about 67,440 cases. Pancreatic cancer is slightly more common in men than women. Risk increases with age.
Types of pancreatic cancer
There are two main types:
Exocrine pancreatic cancer: This is the much more common type. It starts in exocrine cells, which make proteins called enzymes to digest food. The most common type of exocrine pancreatic cancer is ductal adenocarcinoma. It starts in the pancreatic duct, which runs along the pancreas and connects with the small intestine.
Neuroendocrine pancreatic cancer: This type forms in endocrine cells, which make hormones. These cancers are also called pancreatic neuroendocrine tumors, or PNETs.
Pancreatic cancer survival rates
Pancreatic cancer is challenging to treat, in part because it’s often found after it has spread. Long-term survival rates are discouraging.
At the same time, five-year survival rates have steadily climbed. They have more than doubled since the mid-2000s, according to the National Cancer Institute. It’s also important to know that cancer survival rates are based on large groups of people. They can’t predict what will happen to you.
There are signs of hope, too. The Knight and other major cancer centers can offer surgery to more patients than ever. Your team at the Knight will be devoted to giving you the longest, highest-quality life possible.
Clinical trials and research
Clinical trials are research studies with human subjects. Trials may test new devices, new drugs, or existing drugs in new combinations. Or they may test new ways to prevent or find cancer.
Our leadership in clinical trials gives you early access to promising treatments. Our national and global research partners also help with the latest advances.
Support services
- Cancer social workers can help you with financial, housing or transportation issues.
- Cancer nutrition services provide registered dietitians to help before, during and after cancer treatment.
- Acupuncture for cancer can help you manage side effects.
- Cancer registries, including for pancreatic cancer, propel research and share information about the latest advances.
Learn more
- Pancreatic Cancer, American Cancer Society
- Pancreatic Cancer – Patient Version, National Cancer Institute
- Facing Pancreatic Cancer, Pancreatic Cancer Action Network
Location
Knight Cancer Institute, South Waterfront
Center for Health & Healing, Building 2
3485 S. Bond Ave.
Portland, OR 97239
Free parking for patients and visitors
Refer a patient
- Refer your patient to OHSU.
- Call 503-494-4567 to seek provider-to-provider advice.
Cancer clinical trials
Clinical trials allow patients to try a new test or treatment.
New blood test for pancreatic cancer has 85% accuracy

The OHSU test can find pancreatic cancer earlier, when it can be treated more effectively.
Read more
Learn more about OHSU Knight Cancer Institute treatments:
- Surgery
- Chemotherapy/medical oncology
- Radiation therapy
- Immunotherapy
- CAR T-cell therapy
- Targeted therapy
Find other pancreas care at OHSU.
Stay informed
News: Read about research breakthroughs, patient care and many other topics on our OHSU News site.