Bladder Cancer

The OHSU Knight Cancer Institute offers you expert care for bladder cancer. You’ll find:
- Complete care from doctors who specialize in cancers of the urinary tract.
- Nonsurgical techniques that treat your cancer while preserving your bladder function.
- Advanced surgical techniques, including minimally invasive options and options to preserve or reconstruct your bladder.
- Specialists who meet every other week to combine their expertise for each patient.
- Nurse coordinators who schedule your appointments and answer your questions.
- A wide range of support services for you and your family.
Understanding bladder cancer
Urinary System Anatomy
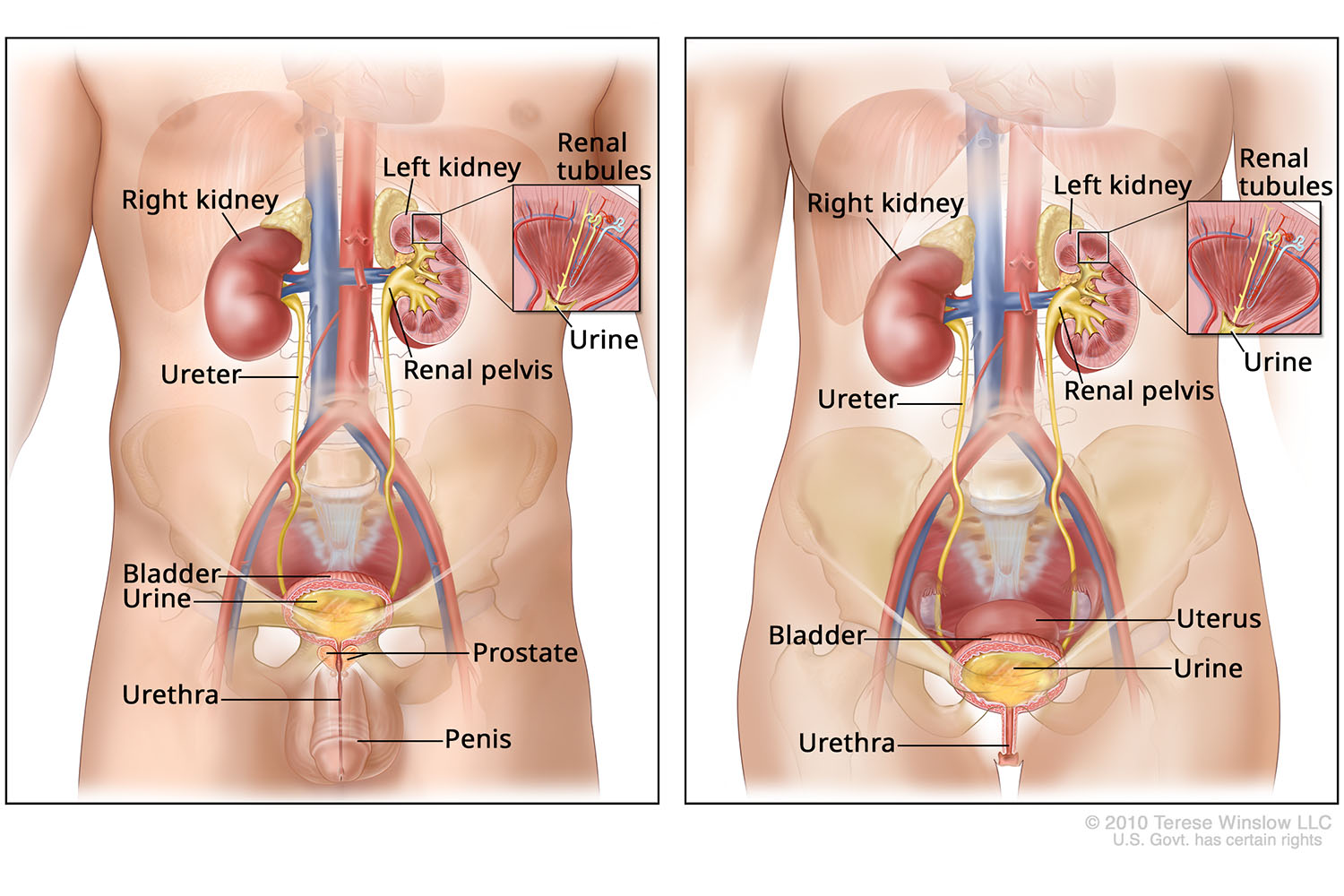
What is bladder cancer?
The bladder is part of the urinary tract, the system that removes urine from the body. This muscular, hollow organ sits in the pelvis. It collects urine from the kidneys through tubes called ureters. Urine exits the bladder through a tube called the urethra. Bladder cancer develops when cells in the bladder’s lining grow out of control.
Who gets bladder cancer?
Bladder cancer is among the most common cancers in the United States. About 84,500 people in the U.S. are diagnosed every year, according to the National Cancer Institute. About 763,000 people in the U.S. are living with it.
Scientists don’t yet know exactly what causes bladder cancer, but they have identified risk factors:
- Smoking: This is the most common risk factor.
- Age: More than 90% of those diagnosed with bladder cancer are 55 or older. People in the 65-74 age group are diagnosed most often.
- Gender: Bladder cancer is about four times more common in men.
- Race: Bladder cancer is about twice as common in white people as in people of color.
- Exposure to certain substances: Toxins such as arsenic in drinking water or prolonged contact with certain industrial chemicals can increase risk.
- Previous cancer treatment: Some types of chemotherapy used for leukemia and lymphoma can raise the risk of bladder cancer. So can radiation therapy in the pelvis.
- History of urologic cancer: You face a higher risk if you’ve had the disease or a similar cancer in the kidneys, ureters or urethra.
- Health history: Birth defects in the bladder can increase your risk, as can chronic bladder or urinary tract infections or inflammation.
- Family history: Bladder cancer appears to run in families. Sometimes this happens because of exposure to the same toxins. You can also inherit a genetic change from a parent for a condition linked to bladder cancer, such as Lynch syndrome or Cowden syndrome. OHSU offers expert genetic testing and counseling to help you identify and manage risk.
Survival rates
A key concept in understanding survival is five-year relative survival rate. This is the percentage of people who are still alive five years after they were first diagnosed, compared to the general population. (It doesn’t count death from other causes.)
The five-year relative survival rate for bladder cancer is 79%, according to the National Cancer Institute. This rises to 98% if the cancer is caught in the earliest stage. It's important to know that these are averages. They can't predict the outcome for any one patient.
Bladder cancer symptoms
These symptoms can also occur with other conditions, such as a urinary tract infection, bladder stones or an overactive bladder. Talk with your doctor if you have any of the following:
- Blood in urine
- Difficulty urinating
- Frequent or urgent need to urinate
- Pain in the belly or lower back
- Pain or burning when urinating
- Unexplained weight loss
- Urine leakage
Diagnosing bladder cancer
People usually come to the OHSU Knight Cancer Institute after tests show blood in their urine. Your care team may recommend tests such as:
Physical exam: Your doctor does a complete physical. It may include a pelvic exam for women and a rectal exam for men or women. Sometimes the doctor can feel a bladder tumor.
Urinalysis: Testing can detect blood or other substances in urine that may indicate bladder cancer.
Urine cytology: A type of doctor called a pathologist looks at urine under a microscope to check for cancer or precancerous cells.
Urine culture: We place a urine sample in a lab dish to see if bacteria grow. This can indicate whether an infection is causing urinary symptoms.
Cystoscopy: Your urologist inserts a cystoscope (a thin tube with a camera and light) through the urethra and into the bladder. This lets us look for abnormal tissue.
Biopsy: A pathologist uses a microscope to check a tissue sample for cancer cells. Your doctor may remove the sample during a cystoscopy or a similar procedure.
CT scan: In computed tomography, special X-ray equipment and a computer create 3D images. We may use a CT scan to rule out kidney stones, which are more common than bladder cancer. If bladder cancer has been found, CT scans can show if cancer has spread to the chest, belly or pelvis.
MRI scan: Magnetic resonance imaging uses radio waves and a large magnet to take detailed pictures inside the body. We are the only center in Oregon with a 3 Tesla MRI to show small areas in great detail. We may take scans to measure bladder tumors or to check for bladder cancer that may have spread.
Ultrasound: Sound waves create images of soft tissue inside the body. We may use ultrasound to measure bladder tumors or check nearby areas for cancer that may have spread.
Chest X-ray: We may recommend this test to see if bladder cancer has spread to the lungs.
Bone scan: If we suspect that bladder cancer has spread to your bones, a special scan can detect it. We inject a tiny amount of radioactive material into the bloodstream, which carries it to the bones. Cancer shows as a white spot on the scan.
Types of bladder cancer
-
Urothelial carcinoma
Urothelial carcinoma, previously called transitional cell carcinoma, forms in the urothelial cells lining the inside of the bladder. It makes up about 90% of U.S. cases.
Your doctor may describe bladder cancer by how far it has grown through the bladder wall, which has four layers.
- Noninvasive cancers are in the inner layer.
- Invasive cancers have grown farther into the lining.
Urothelial carcinoma has two subtypes. Both can grow through the bladder lining and spread:
- Papillary tumors are usually noninvasive. They typically grow from the inner layer of the lining toward the center of the bladder.
- Flat tumors can be more invasive. They grow along the surface of the bladder lining.
Urothelial cancer can also affect:
- The kidneys
- The ureters, the body’s two tubes that carry urine from each kidney to the bladder
- The urethra, the tube that carries urine from the bladder to outside the body
-
Rare types of bladder cancer
Squamous cell carcinoma: This cancer develops in the bladder lining and is almost always invasive. Causes include chronic bladder irritation, such as from an infection or prolonged use of a urinary catheter (a tube to drain urine from the body).
Adenocarcinoma: Adenocarcinoma grows in mucus-secreting glands in the bladder. Most bladder adenocarcinomas are invasive.
Small cell carcinoma: Less than 1% of bladder cancers are small cell carcinomas. These aggressive cancers start in nervelike, hormone-producing cells known as neuroendocrine cells.
Sarcoma: This cancer, rare in the bladder, starts in muscle cells. It has subtypes that include rhabdomyosarcoma, which is more common in children.
Bladder cancer staging
Staging describes the size of a tumor and how far cancer cells have spread. It helps your doctors recommend the best treatment plan. The following stages are for urothelial carcinoma, the most common type of bladder cancer.
Stage II Bladder Cancer
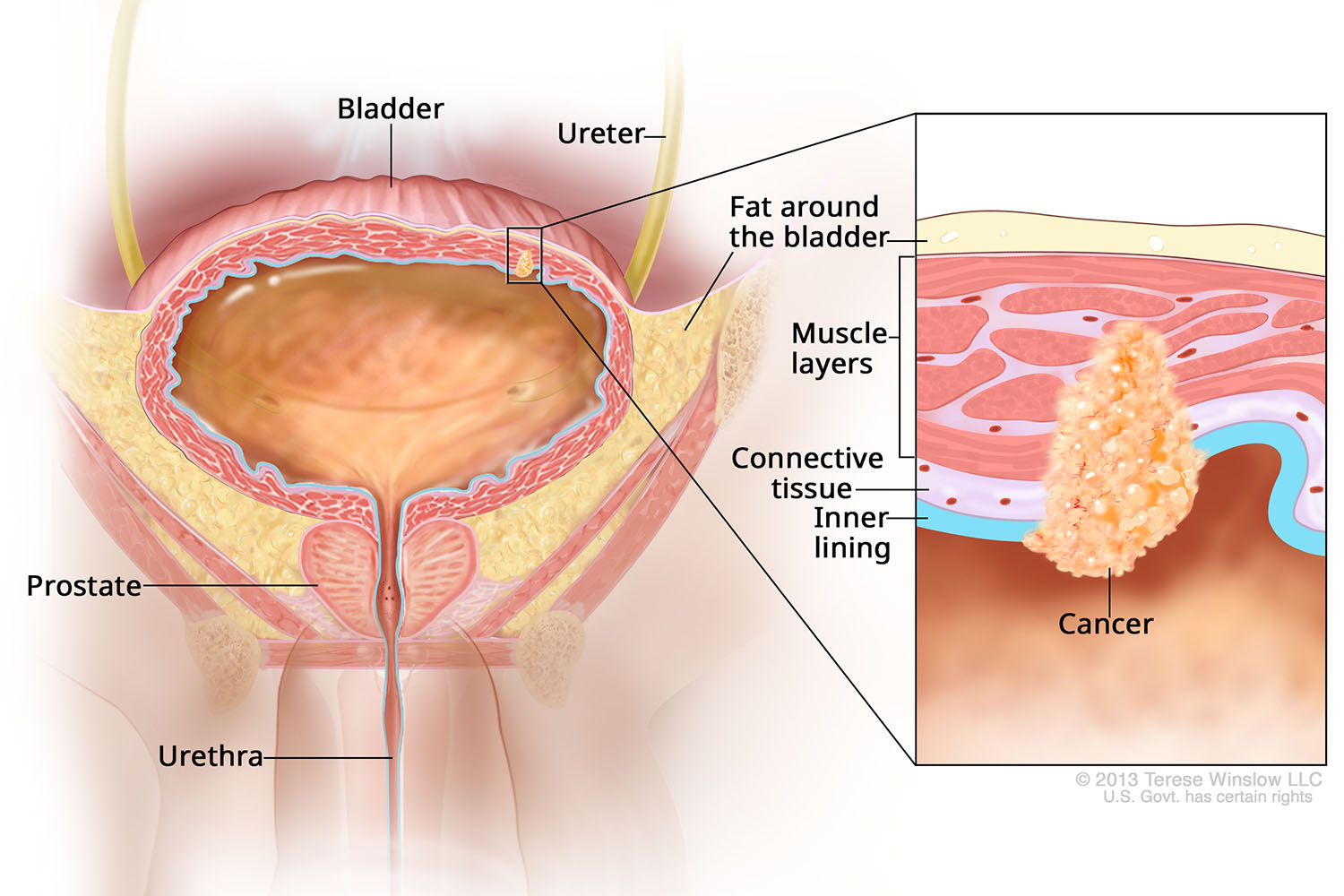
-
Stage 0
Stage 0a: The tumor is a noninvasive papillary carcinoma on the inner surface of the bladder lining.
Stage 0is: The cancer is a noninvasive flat tumor confined to the inner surface of the bladder.
-
Stage I
Cancer has spread to the connective tissue next to the bladder lining. This layer is called the lamina propria.
-
Stage II
Cancer has spread to the bladder’s muscle wall and is called muscle-invasive disease.
Stage IIA: The tumor has spread to the inner half of the bladder’s muscle wall.
Stage IIB: The tumor has spread to the outer half of the bladder’s muscle wall.
-
Stage III
Stage IIIA: One of the following:
- The tumor has grown through the muscle layer into fatty tissue that surrounds the bladder or into the prostate, uterus or vagina.
- The tumor ranges from as shallow as the connective tissue next to the bladder’s lining to as deep as the prostate, uterus or vagina. In addition, cancer has spread to one lymph node in the lower part of the pelvis.
Stage IIIB: The tumor ranges from as shallow as the connective tissue next to the bladder’s lining to as deep as the prostate, uterus or vagina. In addition, one of the following:
- Cancer has spread to two or more lymph nodes in the lower part of the pelvis.
- Cancer has spread to lymph nodes along the iliac arteries, which supply blood to pelvic organs.
-
Stage IV
Stage IVA: Cancer has spread to lymph nodes beyond the iliac arteries, which supply blood to pelvic organs.
Stage IVB: Cancer has spread to distant parts of the body, not including lymph nodes.
Bladder cancer treatment
Treatment for bladder cancer depends on the type and stage of the disease, your overall health and other factors. We may recommend testing to look for genetic changes and other features when cancer has spread. This testing can help your care team decide:
- If immunotherapy might help.
- If you are eligible to try a promising therapy in a clinical trial.
Team-based care: At OHSU, your care team may include a range of providers, including expert urologic oncologists and urologists. These specialists are highly trained in the urinary system and cancer care. Your urologic oncologist may be the lead provider in caring for early-stage bladder cancer that has not spread to muscle.
Surgery
Surgery is often the first treatment for bladder cancer. The goal is to completely remove the tumor. At the Knight Cancer Institute, our surgeons are experts at advanced procedures for cancers of the urinary tract and reproductive organs. These procedures may include:
Transurethral resection of bladder tumor: TURBT can remove small, early-stage bladder cancers. The surgeon takes out the tumor and a narrow border of surrounding tissue. TURBT may be the only treatment needed for Stage 0 cancers. It may be combined with chemotherapy, radiation therapy, immunotherapy or additional surgery for Stage I, II and III cancers.
Cystectomy: If cancer has spread into the bladder’s muscle wall, surgery may be needed to remove part or all of the bladder. Our surgeons are highly experienced in minimally invasive robotic surgery for patients with bladder cancer. This option offers precision, less pain and a shorter recovery.
- Partial cystectomy removes the tumor and nearby muscle wall. This option preserves the bladder, though cancer may return in another part of the bladder.
- Radical cystectomy removes the bladder, reducing the risk of future bladder cancer. Sometimes lymph nodes, the prostate gland, ovaries, fallopian tubes, uterus or cervix are also removed.
Reconstructive surgery (urinary diversion): We offer three ways to rebuild the urinary tract, depending on your needs and wishes. All use parts of the intestine to create a new bladder.
Chemotherapy

Chemotherapy is cancer-fighting medication. Your care team may use chemotherapy in combination with radiation therapy or surgery. For bladder cancer, chemotherapy may be:
- Systemic, meaning it’s placed in your bloodstream to kill cancer cells circulating nearly anywhere in your body.
- Delivered directly to areas with tumors.
Chemoradiation: Our team has expertise in combining systemic chemotherapy with radiation therapy. Chemoradiation treats people with muscle-invasive bladder cancer and can help avoid bladder removal. It’s also an option for people who are too frail for surgery.
Intravesical therapy: Your doctor gently inserts a thin, flexible tube through the urethra into the bladder. We then deliver chemotherapy and immunotherapy medications through the tube once a week for six weeks. This therapy can help keep cancer from coming back.
Radiation therapy
Radiation therapy uses beams of energy, such as X-rays, to destroy cancer cells.
External beam radiation therapy is most effective for bladder cancer. It uses a machine to send focused radiation beams directly to the tumor. We use technology called cone beam CT (CBCT) scanning to create detailed images to target the radiation, protecting healthy tissue.
Learn more about how we treat cancer with radiation therapy.
Immunotherapy
Knight Cancer Institute researchers are involved in hundreds of clinical trials to test innovative approaches to cancer, including bladder cancer.
For example, we’re combining immunotherapy with radiation therapy for bladder cancer that has spread to see if the approach relieves symptoms, prevents cancer growth or prolongs life.
Your care team will talk with you about whether a clinical trial is right for you.
Learn more
- American Bladder Cancer Society
- BCAN
- Bladder Cancer, American Cancer Society
- What is Bladder Cancer?, National Cancer Institute
Bladder Cancer team
-
- Christopher Amling, M.D., FACS
- Accepting new patients
-
- Jennifer Botelho, MPAS, PA-C (she/her)
- Accepting new patients
-
- Jeremy Paul Cetnar, M.D., M.S.H.P.R.
- Accepting new patients
-
- Mark Garzotto, M.D.
- Accepting new patients
-
- Sudhir Isharwal, M.D., M.B.A.
- Accepting new patients
-
- Ryan Kopp, M.D.
- Accepting new patients
-
- Lisa Langmesser, MHS, PA-C
- Accepting new patients
-
- Jen-Jane Liu, M.D.
- Accepting new patients
-
- Ronald Ng, M.D. (he/him)
- Accepting new patients
-
- Max Poole, PA-C (he/him)
- Accepting new patients
-
- Christopher W. Ryan, M.D.
- Accepting new patients
-
- Hilary Shreves, M.S.N., A.C.N.P.-B.C.
- Accepting new patients
-
- Marshall Strother, M.D.
- Accepting new patients
-
- Jacqueline Vuky, M.D.
- Accepting new patients
-
- Casey Williamson, M.D., M.A.S. (he/him)
- Accepting new patients
Location
Knight Cancer Institute, South Waterfront
Center for Health & Healing, Building 2
3485 S. Bond Ave.
Portland, OR 97239
Free parking for patients and visitors
Refer a patient
- Refer your patient to OHSU.
- Call 503-494-4567 to seek provider-to-provider advice.
Cancer clinical trials
Clinical trials allow patients to try a new test or treatment.
Read more
Learn more about OHSU Knight Cancer Institute treatments:
Stay informed
News: Read about research breakthroughs, patient care and many other topics on our OHSU News site.