Lung Cancer

Lung cancer happens when abnormal cells form and grow out of control in one or both lungs. Lung cancer has few signs and symptoms early on in its early stages. Doctors sometimes find it after a chest X-ray for another condition.
Lung cancer can be challenging to treat. Still, survival rates have risen as treatments have improved. Doctors are also making strides in finding lung cancer sooner.
At the OHSU Knight Cancer Institute, our large team and leading-edge research give you the highest level of care. The National Cancer Institute recognizes the Knight as one of the top cancer centers in the nation.
We offer:
- World-class experts in lung cancer care and research
- A team focused on getting more people screened for lung cancer so it’s found as early as possible
- A weekly lung cancer clinic where patients can have tests, meet with specialists and get support services in one visit
- Surgeries with smaller cuts and less recovery time, including a procedure pioneered by two OHSU surgeons
- Genetic analysis of lung tumors to help choose the most effective treatment
Quick links
What makes us different
- Expertise: Our experts include surgeons, pulmonary medicine specialists, and radiation and medical oncologists. They have advanced training and experience to treat the most complex cases.
- Teamwork: Our specialists meet regularly to pool their expertise, one patient at a time. They go over test results, treatment options and clinical trials.
- Innovation: Knight scientists are investigating how to improve immune response to lung cancers. Doctors use a precise robotic system to collect lung tissue for cancer screening. They can also do video-assisted and robotic surgery.
- Research excellence: The Knight’s researchers work to quickly turn lab findings into patient care. We offer more than 400 clinical trials, with early access to new drugs, diagnostic tools and treatments.
- Nurse navigators: Your nurse navigator will guide you through treatment and answer your questions. You won’t have to worry about every detail.
- Support for you and your family: Learn about our full range of services, including social workers who specialize in cancer care.
What is lung cancer?
Lung anatomy
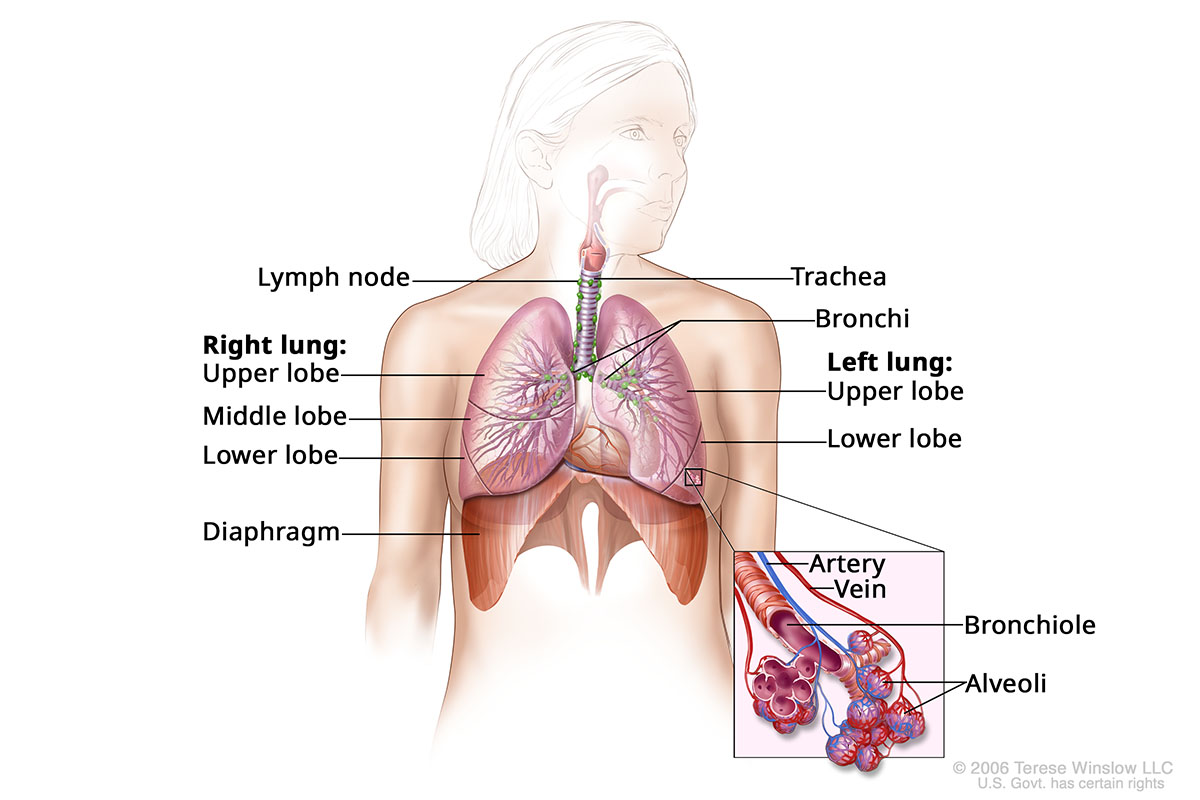
Lung cancer is the uncontrolled growth of abnormal cells in one or both lungs, the organs we use to breathe.
The lungs fill the upper part of the chest. They bring oxygen into the body and remove carbon dioxide and other gases. Lungs contain blood vessels, air tubes (bronchial tubes and bronchi) and air sacs (alveoli).
Who gets lung cancer?
Lung cancer is one of the most common cancers in the U.S. It makes up about 11% of new cancer cases.
Lung cancer is more common in people with a history of smoking and in people exposed to indoor radon. People who have never smoked can also get it.
Lung cancer types
There are two main types:
Non-small cell lung cancer: This type makes up about 85% to 90% of lung cancers. It includes several subtypes, most commonly adenocarcinoma, as well as squamous cell carcinoma and large cell carcinoma.
Small cell lung cancer: This type makes up about 10% to 15% of lung cancers. It is strongly linked to smoking and is most often found in current or former smokers. It tends to grow and spread more quickly than non-small cell lung cancer.
Lung cancer survival rates
Lung cancer is difficult to treat, partly because it is often found after it has spread. Long-term survival rates are discouraging. Still, 5-year survival rates have nearly doubled since 2000, according to the National Cancer Institute.
It’s also important to know that cancer survival rates are based on large groups of people. They can’t predict what will happen to you.
When lung cancer can’t be cured, our team works to give patients the longest, highest-quality life possible. We help patients spend time with loved ones and pursue goals.
Clinical trials and research
Clinical trials are research studies with human subjects. Trials may test new drugs, tests or treatments. We are leaders in giving patients early access to promising treatments.
- The Knight is known worldwide for cancer research, including therapies that target cancer cells while leaving healthy tissue mostly alone.
- The Knight has research partners across the country and around the world, connecting you to the latest advances in prevention, diagnosis and treatment.
Learn more
- Lung Cancer – Patient Version, National Cancer Institute
- Lung Cancer Basics, U.S. Centers for Disease Control and Prevention
- About Lung Cancer, American Cancer Society
- Lung Cancer, American Lung Association
How to stop smoking
- Quit Smoking, OHSU Knight Cancer Institute
- Oregon Tobacco Quit Line, Oregon Health Authority
- How to Quit Smoking, U.S. Centers for Disease Control and Prevention
Location
Knight Cancer Institute, South Waterfront
Center for Health & Healing, Building 2
3485 S. Bond Ave.
Portland, OR 97239
Free parking for patients and visitors
Refer a patient
- Refer your patient to OHSU.
- Call 503-494-4567 to seek provider-to-provider advice.
Cancer clinical trials
Clinical trials allow patients to try a new test or treatment.
Read more
Learn more about OHSU Knight Cancer Institute treatments:
Stay informed
News: Read about research breakthroughs, patient care and many other topics on our OHSU News site.