Amyloidosis
OHSU offers the only treatment and research center in Oregon for amyloidosis. Because amyloidosis can affect many organs, it’s important to seek care from a center like OHSU, where many specialists work together.
You’ll find:
- A team of experts from across specialties. We treat amyloidosis from every angle.
- An amyloid clinic coordinator to arrange your appointments and answer questions.
- Clinical trials to test promising therapies that are not widely available.
- The latest imaging methods for a precise diagnosis.
- Oregon’s largest bone marrow/stem cell transplant center.
- The state’s longest-running heart and kidney transplant programs.

Team-based care
OHSU has specialists for any care you need. Your team may include:
- Hematologist-oncologists (doctors who are experts in blood disorders)
- Cardiologists (heart doctors)
- Nephrologists (kidney doctors)
- Neurologists (brain, spinal cord and nerve doctors)
- Otolaryngologists (ear, nose and throat doctors)
- Radiation oncologists (doctors who use radiation therapy to treat cancer and other disorders)
- An amyloid clinic coordinator
- Genetic counselors
- Social workers
- Pharmacists
- Dietitians
- Physical therapists
- Occupational therapists
Understanding amyloidosis
What is amyloidosis?
Amyloidosis is a group of diseases in which clumps of abnormal proteins build up in organs or tissues.
Proteins are molecules that fold into specific shapes to do important jobs in our bodies. When they misfold, they are called amyloid proteins.
Amyloid proteins build up in organs and tissues because the body can’t break them down like it can with normal proteins. This buildup — in the heart, liver, kidneys, blood vessels, digestive tract and nervous system — causes damage and disrupts function. Severe cases can lead to life-threatening organ failure.
Amyloidosis affects different parts of the body in different people.
Who gets amyloidosis?
Amyloidosis is rare but more common than often recognized. About 4,500 people in the U.S. are diagnosed each year with the most common type, AL amyloidosis.
Risk factors include:
- Age: Most patients are 40 or older at diagnosis.
- Family history: Some types run in families. They include hereditary transthyretin amyloidosis.
- Other conditions: Having multiple myeloma or lymphoma, for example, raises the risk of AL amyloidosis. Some inflammatory diseases raise the risk of AA amyloidosis. Long-term kidney dialysis increases risk of dialysis-related amyloidosis.
Outcomes
Outcomes depend on the type of amyloidosis and the body parts affected. Cases that affect the heart tend to be more serious.
There is no cure for amyloidosis yet. But for some types of the disease, treatment can ease symptoms and slow buildup. With effective treatment, many patients live with amyloidosis for decades.
Amyloidosis symptoms
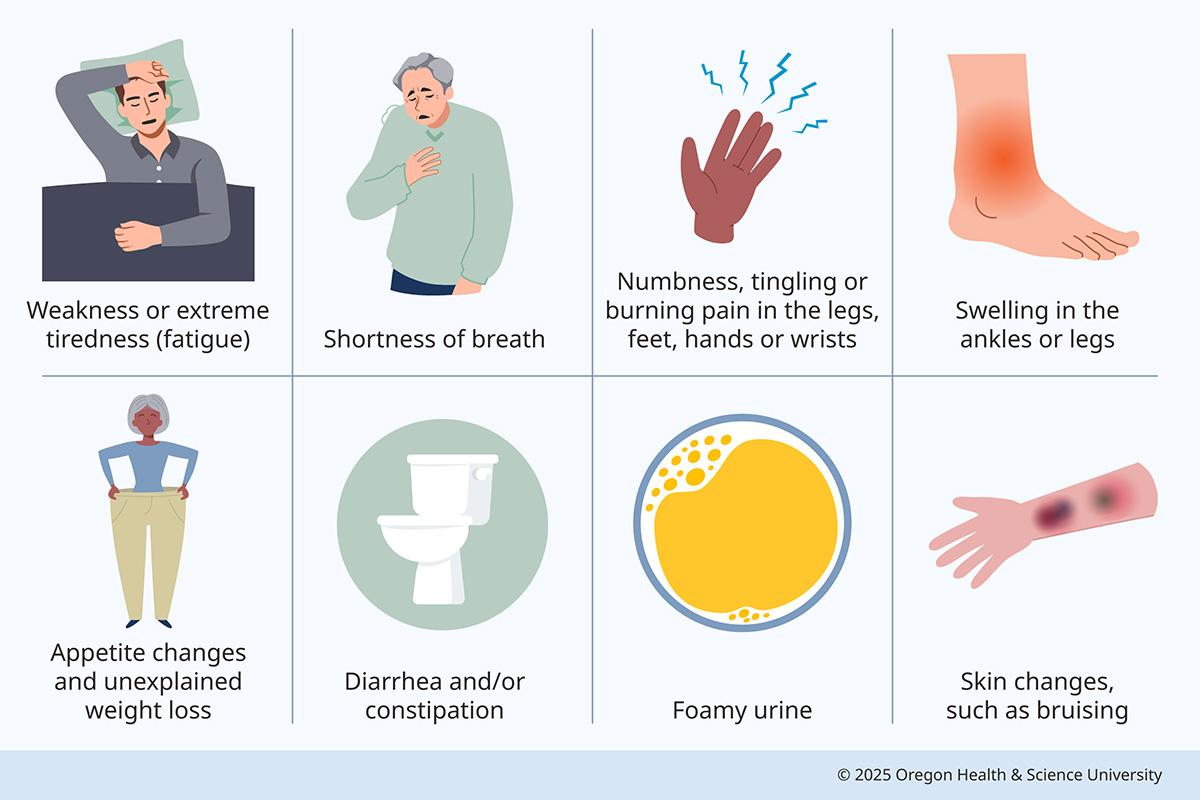
Amyloidosis may not cause noticeable symptoms until it seriously affects organs. Symptoms vary depending on the part of the body affected. They may include:
- Fatigue and weakness
- Shortness of breath
- Appetite changes and weight loss
- Diarrhea and constipation
- Irregular heartbeat
- Foamy urine
- Swelling in the ankles or legs
- Joint pain
- Numbness, tingling or burning pain in the legs, feet, hands or wrists
- Skin changes such as bruising
- Enlarged tongue
- Carpal tunnel syndrome
Amyloidosis Signs and Symptoms
Diagnosing amyloidosis
Amyloidosis can be challenging to diagnose. Symptoms can be vague or similar to those of other diseases.
A physical exam and medical history are first steps. Your care team may also recommend:
Biopsy: The doctor takes a small tissue sample to check for amyloid deposits. Tissue for a biopsy may be taken from:
- Belly fat
- Bone marrow
- Nerve tissue
- An affected organ such as the kidney or heart
Blood and urine tests: These tests can help show which organs might be affected.
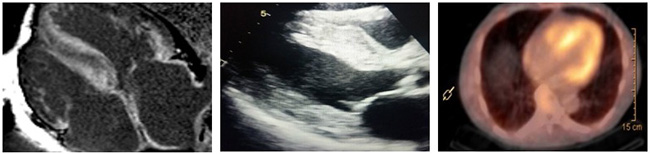
Imaging tests: Scans can help the doctor tell the type and extent of amyloidosis. They include:
- Echocardiogram: This test uses sound waves to show heart motion and blood flow. It can show heart damage specific to types of amyloidosis.
- Magnetic resonance imaging: MRI uses radio waves and magnetic fields to create detailed images of organs and tissues. MRI can be used to check the structure and function of organs.
- Nuclear imaging: A tiny amount of radioactive material is injected into a vein to highlight body parts on a special scan. This test can show early heart damage from amyloidosis, avoiding a heart biopsy. It can also show the form of amyloidosis, helping doctors make treatment recommendations.
Electromyography: This test measures electrical activity in your muscles. It helps doctors identify nerve problems.
Genetic testing: If doctors suspect you have an inherited form of amyloidosis, they may refer you to OHSU genetic experts. These specialists can help you understand your condition and guide you through next steps.
Types of amyloidosis
There are at least 30 types of amyloidosis, including:
AL amyloidosis
AL amyloidosis, the most common type, is also known as amyloid light chain amyloidosis or primary amyloidosis. Parts of antibody protein molecules in bone marrow, called light chains, misfold to form amyloid fibrils (strings or threads). About 15% of patients with multiple myeloma, a blood cancer, also have AL amyloidosis.
AL amyloidosis may affect the:
- Heart
- Kidneys
- Liver
- Nerves
- Digestive system
- Muscles
- Skin
- Joints
Transthyretin amyloidosis
In this type, also known as ATTR amyloidosis, a protein called transthyretin that is made mostly in the liver misfolds into amyloid.
ATTR amyloidosis has two main types:
- Wild-type transthyretin amyloidosis: The transthyretin protein is structurally normal, but amyloid deposits form for unknown reasons. Deposits are found mainly in the heart and tendons. This type can lead to carpal tunnel syndrome and spinal stenosis. It is not hereditary and may be more common than once thought.
- Hereditary transthyretin amyloidosis: An inherited genetic mutation gives the transthyretin protein an abnormal structure. This type typically affects the heart and nerves.
Patients with ATTR amyloidosis can have a wide range of symptoms. ATTR amyloidosis may affect the:
- Nerves
- Heart
- Tendons
- Spine
- Digestive tract
AA amyloidosis
AA amyloidosis is also known as amyloid A protein amyloidosis and secondary amyloidosis. AA amyloidosis can develop as a result of an inflammatory disease, such as rheumatoid arthritis, or a chronic infection. It often affects the kidneys and sometimes the heart or liver.
Dialysis-related amyloidosis
This type affects people with poor kidney function who have spent several years on dialysis, a treatment to remove waste and toxins from the blood. Amyloid proteins build up in joints and tendons, causing pain and numbness.
Leukocyte chemotactic factor 2 amyloidosis
This rare type, also known as ALECT2 amyloidosis, mainly affects the kidneys and liver. It is often seen in patients with Latin American ancestry.
Localized amyloidosis
In this type, amyloid proteins collect in a specific area, such as the airway, an eye or the bladder.
Treating amyloidosis
Our specialists work together to consider every option for your care. Treatments vary depending on the type and severity of your amyloidosis. We may recommend:
Chemotherapy
One or more chemotherapy medications may be given by mouth or injected into a muscle, vein or under the skin. The medications circulate in the bloodstream to kill plasma cells that produce abnormal proteins. To improve effectiveness, chemotherapy drugs may be combined with targeted therapies.
Targeted therapies
Targeted therapies fight abnormal cells by taking aim at specific genes or proteins, or by harnessing the immune system. These therapies limit damage to healthy cells.
- Immunomodulatory drugs help the immune system fight abnormal cells.
- Monoclonal antibodies attach to proteins in abnormal cells.
- Proteasome inhibitors allow proteins to build up and destroy abnormal cells.
- RNA silencers and RNA stabilizers block formation of abnormal transthyretin or amyloid fibrils.
Radiation therapy
To destroy amyloid deposits limited to a specific area, such as the airway or bladder, we may use external radiation therapy. A machine outside your body delivers highly targeted beams of energy to attack abnormal cells.
OHSU was the first center in Oregon to use advanced, image-guided radiation therapy that targets abnormal cells while avoiding healthy tissue.
Bone marrow/stem cell transplant
OHSU’s state-of-the-art bone marrow/stem cell transplant center is the largest in Oregon, giving us unmatched expertise in these complex procedures.
First, your doctors destroy diseased plasma cells with chemotherapy or radiation therapy. Next, a specialist transplants healthy new cells to help fight infection and rebuild your immune system.
Organ transplant
If amyloid deposits have badly damaged your kidneys or heart, your doctor may suggest surgery transplant surgery. Learn about:
Clinical trials and research
As the only academic health center in Oregon, OHSU is committed to applying the latest research developments to patient care.
We offer access to leading-edge clinical trials to test promising therapies for amyloidosis that affects the nerves, blood vessels, heart and other organs. We also work with other institutions to study amyloidosis and test new therapies.
Clinical trials: Learn more about trials to test promising new therapies:
- Trials for amyloidosis that affects the heart
- OHSU trials for blood disorders, including AL amyloidosis
- All OHSU clinical trials
Research: Read published studies on amyloidosis from OHSU researchers.
Learn more
- Amyloidosis, MedlinePlus, U.S. National Library of Medicine
- Amyloidosis and Kidney Disease, National Institute of Diabetes and Digestive and Kidney Diseases
- Amyloidodis Foundation
- Amyloid Research Consortium
Our team
-
- Rupali S. Avasare, M.D.
- Accepting new patients
-
- Nizar Chahin, M.D.
- Accepting new patients
-
- Ahmad Masri, M.D., M.S.
- Accepting new patients
-
- Richard T. Maziarz, M.D.
- Accepting new patients
-
- Eva Medvedova, M.D.
- Accepting new patients
-
- Joshua S. Schindler, M.D. (he/him)
- Accepting new patients
-
- Rebecca Silbermann, M.D., M.M.S.
- Accepting new patients
Locations
Parking is free for patients and their visitors.
- See the “Our team” section, and visit the providers’ profile pages to see where they see patients.
- Find an OHSU location.
Refer a patient
- Refer your patient to OHSU.
- Call 503-494-4567 to seek provider-to-provider advice.
Read more
Learn more about these OHSU treatments: