Pediatric Scoliosis
OHSU Doernbecher provides team-based care and the latest techniques for children and teens with scoliosis (curved spine).
Our Multidisciplinary Pediatric Spine, Scoliosis and Deformity Clinic — one of the nation’s few with experts in both orthopaedics and neurosurgery — treats all types of pediatric scoliosis. We monitor and manage this condition with a full array of specialists, recommending surgery only when necessary.
Understanding scoliosis
How scoliosis curves the spine
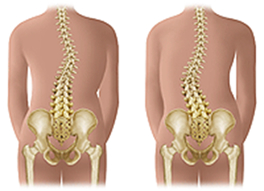
Scoliosis causes the spine to curve sideways, often in a C or S shape. Types and severity vary. Mild cases rarely cause pain and can go unnoticed. In moderate or severe cases, the curve can get worse, making early diagnosis and treatment important.
Who gets scoliosis?
Scoliosis can affect all ages, but it’s most common in adolescents. It affects more girls than boys. It can also run in families, so children with an affected parent or sibling should get regular checkups.
Types and causes
Pediatric scoliosis is categorized in several ways, including the patient’s age, the location in the spine, and cause. Most cases are “idiopathic,” meaning doctors can’t identify the cause. Some are the result of another condition.
-
Patient’s age
Congenital scoliosis: This relatively rare form is present at birth. It occurs when vertebrae — the bones in the spine — develop abnormally.
Infantile scoliosis: This type is diagnosed in children up to age 3. It makes up about 1 percent of idiopathic scoliosis cases in children, according to the Scoliosis Research Society.
Juvenile scoliosis: This type is diagnosed in children ages 4 to 9. It makes up about 10 to 15 percent of children's idiopathic cases, according to the Scoliosis Research Society.
Adolescent idiopathic scoliosis: This type is diagnosed in ages 10 to 18, a time of rapid growth. It's the most common type, making up about 80 percent of idiopathic cases in children. Girls are usually diagnosed from ages 10 to 12, boys from ages 11 to 16.
Early-onset scoliosis: This is any idiopathic scoliosis that develops before age 10.
-
Related conditions
Neuromuscular scoliosis: This type of scoliosis is caused by a condition of the brain, spinal cord or muscular system, such as cerebral palsy, muscular dystrophy or spina bifida.
Syndromic scoliosis: This type occurs as part of a syndrome, such as Down syndrome, Marfan syndrome or neurofibromatosis.
-
Structural or nonstructural
Structural scoliosis: The curvature is irreversible and caused by a disease, condition or unknown factor.
Nonstructural scoliosis: In this type, the spine is structurally normal but curves because of another condition, such as muscle spasms or a difference in leg length. It is usually temporary, going away when the underlying condition is treated.
-
Location and pattern
Thoracic scoliosis: This is a curve in the thoracic (midback) spine, the most common location.
Lumbar scoliosis: This is a curve in the lumbar (lower back) spine.
Thoracolumbar scoliosis: This curve involves vertebrae in the lower thoracic spine and the upper lumbar spine.
Double curve: This type has two curves, like an S.
Dextroscoliosis: This type curves to the right, most often in the thoracic spine.
Levoscoliosis: This type curves to the left, commonly in the lumbar spine.
Curve Patterns
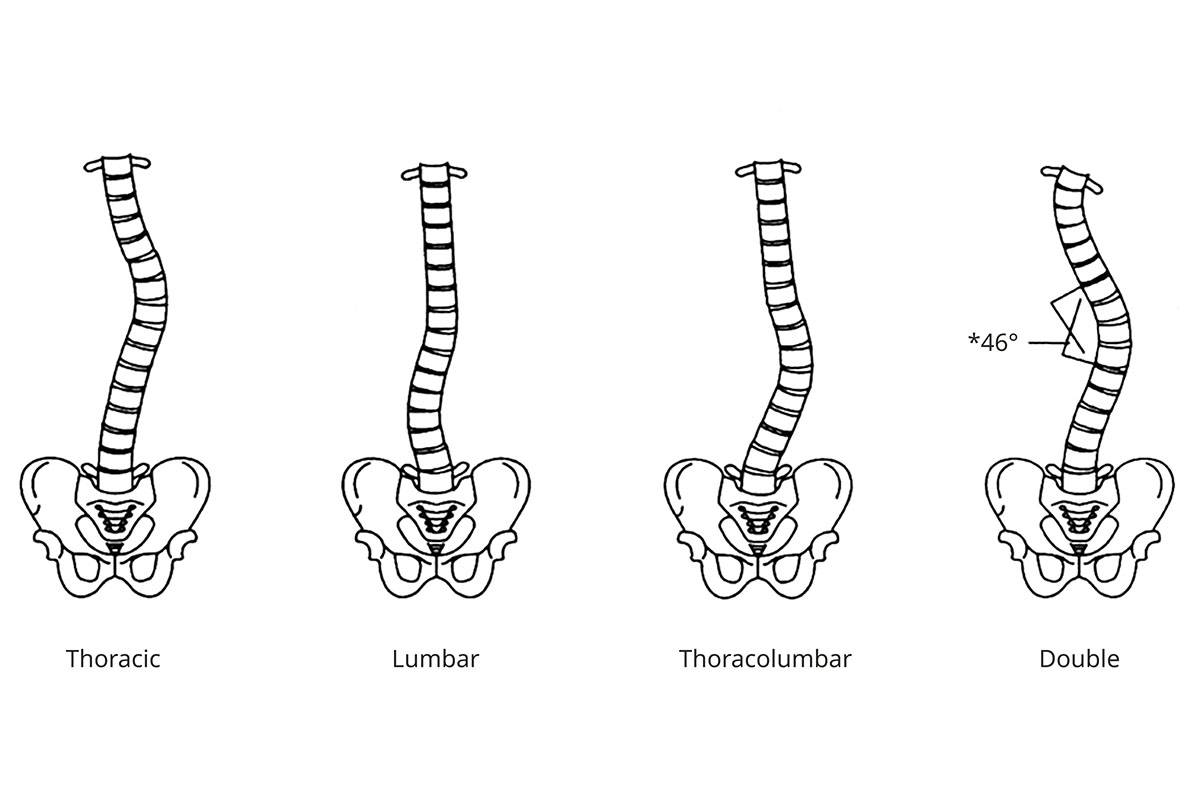
Scoliosis happens when the spine curves, often in a C or S shape. It's most common in teenagers.
Symptoms
Symptoms may first be detected at a school screening or regular checkup. They include:
- Shoulders are at different heights.
- Head is not centered on the body.
- One shoulder blade sticks out.
- Arms hang differently.
- A hip or hips are unusually high.
- The sides of the rib cage are at different heights.
- Waist is uneven.
- Dimples, hairy patches or color abnormalities are on the skin over the curve.
- The body leans to one side.
Diagnosis
- Medical history: The doctor reviews the patient's medical history by looking at records and by asking the patient and parents questions about possibly related symptoms and conditions.
- Exam: The doctor looks at the back, chest, hips, legs, feet and skin. The doctor looks for signs of unevenness, such as whether the head is centered on the body and whether the shoulders, hips and rib cage are even. The child is examined while standing upright and while bending forward.
- Imaging: An X-ray or EOS scan enables the doctor to see whether the spine is curved. The doctor can also identify the site of the curve and measure its angle. Our EOS Imaging System, one of only two in Oregon, creates better images with less radiation.
Treatment
If your child needs treatment, the spine specialists at Doernbecher’s Multidisciplinary Pediatric Spine, Scoliosis and Deformity Clinic will work with your child’s regular doctor on a treatment and management plan.
Specialists at Doernbecher include experts in pediatric neurosurgery, orthopaedics, physical therapy, medical imaging, nutrition, genetics, orthotics and other fields. We also use the latest technology, such as growing-rod systems for early-onset scoliosis that minimize the number of surgeries needed.
- Monitoring: Some curves require no treatment. For curves between 20 and 25 degrees, doctors may examine a child or teen every six to 12 months as the patient grows to make sure the curve doesn't get worse. Our EOS Imaging System, available for children and adults, enables us to take scans with less radiation than other methods.
- Bracing: If a growing child or adolescent has a curve between 25 and 40 degrees, a brace can keep the curve from getting worse, preventing surgery.
- Physical therapy: We offer a therapist certified in the Schroth Method. This noninvasive technique can stabilize your child's curve and lower the chances of needing surgery.
- Surgery: Surgery to correct scoliosis may be recommended for a child with a curve exceeding 40 degrees or an adolescent with a curve of more than 50 degrees. Depending on the case and the child's age, surgery may involve implanting rods to straighten the spine as the child grows, or fusing affected vertebrae.
Learn more
- Scoliosis in Children and Adolescents, National Institute of Arthritis and Musculoskeletal and Skin Diseases
- Scoliosis Research Society, an advocacy group with parent and patient resources
- National Scoliosis Foundation, an advocacy group with support and information such as a glossary and FAQs
Refer a patient
- Refer your patient to OHSU Doernbecher.
- Call 503-346-0644 to seek provider-to-provider advice.