Hydrocephalus
OHSU Doernbecher provides state-of-the-art care for hydrocephalus.
- Our pediatric neurosurgeons are national leaders in treating this complex disorder.
- We are among the few children’s hospitals to offer a minimally invasive technique that avoids shunts in some infants. It dramatically reduces complications and follow-up surgeries.
- We have rapid, radiation-free imaging for continuing care.
Understanding hydrocephalus
Hydrocephalus, sometimes called “water on the brain,” is the most common condition treated by pediatric neurosurgeons. Most patients are younger than 6 months old when diagnosed.
Hydrocephalus

Hydrocephalus occurs when too much cerebrospinal fluid, or CSF, builds up. This clear liquid flows in and around the brain and spinal cord to cushion them against injury. CSF also delivers nutrients, removes waste and helps maintain the brain’s proper equilibrium.
If CSF is blocked by disease or injury, it can build up and put pressure on brain tissue, possibly causing damage. In infants, whose skull bones aren’t fused, hydrocephalus can cause the head to expand.
Main types and causes in children
-
Congenital
This type is present at birth and can be the result of genetic abnormalities or problems in fetal development.
-
Acquired
This type can develop at any age as a result of injury or disease.
-
Communicating
In this type, CSF is not absorbed properly after it leaves a network of four brain cavities, called ventricles, where it's produced. It's called "communicating" because CSF can still flow among the ventricles. Causes include bleeding in the brain, and infection.
-
Noncommunicating
In this type, also called obstructive hydrocephalus, CSF is blocked in one or more of the passages between ventricles. Causes include narrowing of a key passage; bleeding in the brain of a premature infant; or a blockage such as a cyst or tumor.
Symptoms
Symptoms vary depending on age and type. They include:
- Headaches
- Vomiting
- Drowsiness
- In infants, an uncommonly large head or a sudden increase in head size
- Poor feeding
- A decline in thinking abilities, affecting school or work
- Irritability
- Blurred or double vision
- Slow heart rate
- Problems with balance and coordination
- Seizures
- “Sunset” eyes, with the eyes forced downward so the lower lid covers part of the iris, making it look like a setting sun
Leading-edge treatment
Doernbecher Children’s Hospital offers ETV/CPC, the most advanced surgery for treating hydrocephalus in some infants. This procedure eliminates the need for a shunt.
How it works
The surgeon guides a flexible neuroendoscope, a tiny telescope with attached surgical equipment and computer-aided navigation, through a small incision in the skull.
The surgeon creates a small opening in the floor of a ventricle, a CSF-filled cavity in the brain. This procedure, called endoscopic third ventriculostomy, or ETV, allows CSF to flow through more of the brain and be absorbed.
A second procedure, performed at the same time, treats tissue inside the ventricle. It’s called choroid plexus cauterization, or CPC. It may reduce the brain’s ability to produce CSF. ETV and CPC also may work together to restore the brain’s equilibrium.
Why this matters
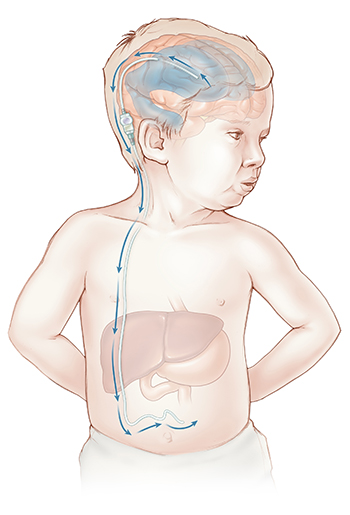
A shunt — a surgically placed valve and tubing that drains CSF from the brain to the belly — can be lifesaving treatment. It also carries lifelong risks, including:
- Shunt malfunctions that require follow-up surgeries
- Infections that can result in learning disabilities and other problems
- Potentially serious shunt failures
In successful ETV/CPC, patients need only one surgery. In addition, ETV failure almost always occurs in the first year, when the risk of serious complications is low.
Comprehensive care
For children who need a shunt, Doernbecher offers top-notch surgical expertise and excellent outcomes.
Pediatric neurosurgeons Nathan Selden, M.D., and Christina Sayama, M.D., have national reputations for excellence in treating hydrocephalus and other conditions. In addition, our team includes specialists and technology for all aspects and phases of care. This includes:
- A “quick-brain” MRI scanner to check for shunt complications. This rapid imaging requires no sedation and, unlike a CT scan, uses no radiation.
- Precise protocols for immediate, effective treatment for children with possible shunt complications.
Related conditions
-
Chiari malformation
The pediatric specialists at Doernbecher Children's Hospital offer advanced care for Chiari malformation, including a less-invasive procedure with equally good results.
-
Spina bifida
Doernbecher provides complete care for spina bifida with both an integrated pediatric spine clinic and Oregon's only program for ongoing care into adulthood.
Learn more
- Hydrocephalus Information Page, National Institute of Neurological Disorders and Stroke
- Hydrocephalus Association, an advocacy group with information and support
- National Hydrocephalus Association, another advocacy group with information for patients and families
Refer a patient
- Refer your patient to OHSU Doernbecher.
- Call 503-346-0644 to seek provider-to-provider advice.
Meet Jake Vinyarskiy

Jake Vinyarskiy (left, with older brother Nicholas) was just weeks old when he was diagnosed with hydrocephalus. His worried mom, Brandy Alexander, spent hours on the internet researching the condition. She learned about a shunt-free procedure, but Jake's doctor couldn't do it. Then the family was referred to OHSU Doernbecher Children's Hospital. Read Jake's story.