Residency Details
The information below will answer many of your questions about the Orthopaedic Surgery Residency Program. Expand the sections to learn about how to apply to the program and what to expect during the interview process. See the curricula and learn specifics about rotation, the call schedule and more. There is even a list of fellowship programs of past residents.
-
How to apply
OHSU participates in the Association of American Medical Colleges Electronic Residency Application Service. Applications must be submitted electronically through the ERAS system by November 1 to be considered. Please contact your dean's office for your student workstation software and information on the electronic application process.
A complete application is standard and includes the following items:
- ERAS application (CV) with photograph
- Medical school dean's letter
- Three letters of recommendation (Three is the minimum and we will accept up to four letters. We will accept either a traditional letter or the AOA Standardized Letter of Recommendation. Chair or Program Director letters are welcome but not required. We encourage applicants to obtain letters from faculty who know them best and can speak to their abilities and strengths)
- USMLE board scores - We do not have a minimum cutoff score. We normally require Step 1 and Step 2 CK results at the time of application. Given current circumstances, if unable to schedule Step 2 examinations prior to application that is understandable and will not preclude your consideration. Please attempt to schedule as soon as able, as it will be required to happen prior to our final ranking.
- Medical school transcripts
- Your personal statement (Please include a few sentences in your personal statement to let us know why you are interested in OHSU/Oregon.)
Please note that our review process lasts well into November. Per the AOA/CORD guidelines, we plan to send out interview invitations on Universal Offer Day, November 17, 2025. A 24-hour moratorium on accepting or scheduling invitations will follow. Each applicant will then have 48 hours to accept the offer or respond to the program.
If you have had postgraduate training, send letters of recommendation from the program director(s) of your first postgraduate year and any subsequent residency training.
OHSU accepts international medical graduates, but they must have an Educational Commission for Foreign Medical Graduates, also known as ECFMG, certificate before they will be appointed. All applicants must be legally able to work in the United States or eligible to obtain work authorization.
Interviewing: What to expect
Interview dates for the 2026 Match
- Monday, Dec. 1, 2025
- Friday, Dec. 12, 2025
- Thursday, Jan. 8, 2026
- Tuesday, Jan. 13, 2026
- Wednesday, Jan. 21, 2026
All interviews will be virtual using Thalamus
Questions
For more information, please contact Robin Sasaoka, Resident and Fellowship Program Coordinator, at 503 494-5842 or e-mail sasaokar@ohsu.edu. See the AMA's fellowship and residency electronic interactive database for more details (FREIDA). Upon acceptance and hiring, drug testing and criminal record checks will be done as part of the hiring process for OHSU.
-
Residency program details
Rotation
Intern year - PGY1
- Orthopaedic trauma (10 weeks)
- Orthopaedic spine (10 weeks)
- VA Orthopaedics (8 weeks)
- General surgery at Providence St. Vincent's (4 weeks)
- Physical medicine and rehabilitation (4 weeks)
- Surgical trauma ICU (4 weeks)
- General trauma surgery (4 weeks)
- Plastic surgery (4 weeks)
- Vascular surgery (4 weeks)
PGY2
- Trauma at OHSU (level 1 trauma center) - 2 rotations (10 weeks each)
- Night float (5 weeks)
- Day resident (5 weeks)
- Pediatrics at Shriner’s Hospital for Children (10 weeks)
- VA Medical Center (10 weeks)
- Pediatrics at Doernbecher Children’s Hospital (10 weeks)
PGY3
- Oncology at OHSU (10 weeks)
- Foot and ankle at OHSU (10 weeks)
- Joints at OHSU (10 weeks)
- Sports at OHSU (10 weeks)
- Upper extremity at OHSU (10 weeks)
PGY4
- Spine at OHSU (10 weeks)
- Trauma at OHSU (level 1 trauma center) (10 weeks)
- General orthopaedics at Providence St. Vincent's (10 weeks)
- Pediatrics at OHSU (10 weeks)
- Research (10 weeks)
PGY5
- Sports at OHSU (10 weeks)
- Hand and upper extremity at OHSU (10 weeks)
- VA Medical Center (10 weeks)
- Joints at OHSU (10 weeks)
- Trauma at OHSU (level 1 trauma center) (10 weeks)
On-call details
For the purposes of assigning the call schedule, residents are divided into a junior call pool and a senior call pool. The junior call pool consists of the 2nd and 3rd year residents rotating at OHSU. The senior call pool consists of the 4th and 5th year residents rotating at OHSU. Junior residents have in-house call responsibilities and field all patient calls, nurse calls and consults. Senior residents are on home-call and are available to back up junior residents and cover any cases that go to the operating room.
We have adopted a night float system for the junior in-house call that significantly decreases the call burden on the other junior non-night-float residents. It also ensures that the non-night-float junior residents do not have to leave post-call during their rotations, which would interrupt valuable surgical and clinical training.
The non-night-float residents are on call approximately every 14 days. The senior residents are on call approximately every six days and one in every six weekends. At the Shriner’s Hospital, the call is covered by the resident on that rotation as well as international pediatric orthopaedic fellows. The call schedule at the Shriner’s Hospital is approximately every five to six days. The VA Medical Center is covered by the OHSU call team at night.
National conferences
The Department of Orthopaedics and Rehabilitation provides funding for each class of residents to attend one conference per year as follows:
PGY2 year:
The annual AO Trauma Basic Techniques Conference provides extensive hands-on teaching of trauma principles with multiple sawbones labs. It includes lectures by national leaders in trauma surgery.PGY5 year:
Residents attend the AAOS Board Review Course to prepare for the written orthopaedic board exams.Residents in their final year are supported to attend the AAOS Annual Meeting. This is to provide time for professional development, practice management and Board preparations.
OHSU Orthopaedic Surgery Residency Research Travel Awards:
Residents will be provided time off from clinical responsibilities and will be financially supported for attendance at meetings at which they are delivering a podium presentation of a scientific paper. These meetings must be regional or national scientific meetings of recognized orthopaedic societies, Financial support in this manner will be limited to a maximum of two meetings during a resident’s tenure in the training program.
Resident pay and benefits
Pay scale: 2025-2026 academic year
PGY1: $73,681.52
PGY2: $77,202.91
PGY3: $80,850.27
PGY4: $84,873.09
PGY5: $89,399.22Medical, dental, life and disability insurance, OHSU provides a stipend that helps cover insurance.
Surgical loupes
The Department of Orthopaedics has a fund supported by alumni donations that provides loupes for all residents at the beginning of the intern year.
Meals: OHSU provides approximately $200 per month that residents can use to purchase meals during OHSU rotations. Residents are given meal cards to cover their expenses on rotations at the VA Medical Center. On-call meals at the Shriner’s Hospital are free.
OHSU advantages
- Excellent clinical education
- Early operating room experience
- Great one-on-one learning environment
- Great camaraderie among residents and family support network
- Very good fellowship placement
- Good research opportunities in both clinical trials and basic science
- Fun, active lifestyle outside of the residency
- Portland is a great place to live.
Where we work
OHSU Hospital
- 562 beds, Level 1 trauma center
- The Department of Orthopaedics has 26 faculty members including 23 orthopaedic surgeons and three physical medicine and rehabilitation specialists.
- Orthopaedic surgeons on the faculty cover all specialty areas. There are two foot and ankle surgeons, three hand and upper extremity surgeons, four spine surgeons, three trauma specialists, three sports medicine specialists, three joint replacement specialists, four orthopaedic oncologists and one pediatric orthopaedic surgeon.
- The department has more than $2 million in current research grant funding and more than 40 current research projects.
- The department has its own biomechanics and basic science labs.
Doernbecher Children’s Hospital
- 151 beds
- One pediatric orthopaedist
Portland VA Medical Center
- 245 beds
- Six part-time faculty
Shriner’s Hospital for Children
- 40 beds
- Shriner’s Hospital has eight faculty. Full-time faculty members include two spine surgeons, two lower extremity surgeons and one general pediatric orthopaedist. Part-time faculty includes two hand and upper extremity surgeons and one general pediatric orthopaedist.
- This facility has a gait analysis lab and an on-site prosthetics and orthotics lab.
Please note: All of the hospitals listed above are located on the OHSU campus and are connected by sky bridges.
Living in Oregon
Oregon offers majestic landscapes, a vibrant yet easygoing vibe, and some of the best food, beer and coffee in the world. Learn about the sights, sounds and people in the state we love to call home.
Monthly conferences
-
Intern year
The first year as an intern gives residents the opportunity to learn orthopaedics from the start. Half the year is dedicated to orthopaedic surgery and related specialties, including physical medicine and rehabilitation. The other half is focused on subspecialties of general surgery relevant to orthopaedics, such as vascular surgery, trauma ICU, trauma surgery, plastic surgery, and pediatric surgery.
Orthopaedic interns are encouraged to attend orthopaedic Grand Rounds, teaching conferences and journal clubs. Interns also have sufficient time outside the hospital to explore everything that Portland and the beautiful surrounding areas have to offer.
PGY-2 to PGY-5
These years are dedicated to the study of orthopaedics. This part of the program is set up as a mentorship program, with each resident working with 1-3 attendings on each rotation. This helps individualize training and helps residents develop surgical skills. Residents also have early exposure to the operating room to learn these skills.
As an example of the number of procedures residents might do, one OHSU orthopaedics resident had 682 CPT codes recorded by the end of the R2 year. Most of these came from operating room cases; however, this number also included some fracture reductions and other minor procedures in the emergency department. Furthermore, the only surgical fellowship that the Department of Orthopaedics offers is in spine surgery, which leaves a wider range of educational experiences open to residents only.
The rotation cycle is designed to expose residents to all orthopaedic subspecialties by the end of their third year. This training is useful when residents decide whether to pursue fellowship training, and in what specialty. Finally, the orthopaedics residency includes a dedicated research rotation. Residents have protected time to focus on this important component of our resident education program.
-
- Intern year
- Joints
- Emanuel
- Foot and Ankle
- Pediatrics PGY1
- Pediatrics PGY4
- Physical Medicine and Rehabilitation
- Research
- Shriners
- Sports Medicine
- St. Vincent
- Trauma
- Tumor
- Upper Extremity
- Veterans Administration
-
VirtuOHSU Simulation and Surgical Training Center
This highly versatile space supports open, arthroscopic, laparoscopic, endoscopic, and microscopic technical skills training. The 7,500 square-foot simulation and surgical training center includes:
- Lab A: 2 surgical scrub sinks and a 16 table anatomy dissection lab or 8 station simulated OR (able to flex between 8 or 10 with Lab B).
- Lab B: 2 station simulated OR (able to flex to become part of 10).
- Lab C: Microsurgery suite with 8 Ziess microscopes.
- 70 seat amphitheater with full AV and conferencing capabilities;
- 18-24 seat classroom with SMART board
- MIS Training Suite with 10 laparoscopy stations, 1 laparoscopic VR simulator, 1 endoscopic/bronchoscopic VR simulator, and 1 da Vinci Robot VR simulator.
Medical training simulator
OHSU uses the VirtaMed ArthroS™ medical training simulator to train orthopaedic residents on diagnostic and therapeutic knee shoulder, hip and ankle arthroscopy. Benefits of the simulator include:
- Residents practice procedures and build surgical skills in a risk-free, hands-on environment.
- Residents and trainers can see progress and focus training efforts.
- Skills can be objectively assessed to measure against benchmarks and targets.
-
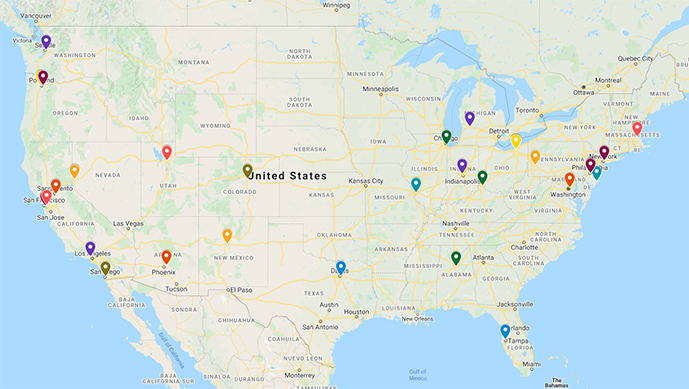
Fellowships over the past 10 years. Click on map for additional detail. 2023 Fellowships
- Orthopaedic Trauma - Harborview Medical Center, Seattle, WA
- Hand and Upper Extremity and Microvascular Fellowship, UC Davis
- Sports Medicine and Shoulder Surgery - UCSF
- Adult Reconstruction - Rush University, Chicago, IL
- Hand and Upper Extremity - OHSU
2022 Fellowships
- Hand Fellowship - University of New Mexico
- Hand and Upper Extremity - Brown Department of Orthopaedic Surgery
- Sports Medicine and Shoulder - UCSF Orthopaedic Institute
- Adult Reconstruction - Rothman Orthopaedics
- Pediatric Orthopaedics - Children’s Hospital Los Angeles
2021 Fellowships
- Sports Medicine - Southern California Orthopedic Institute
- Adult Reconstruction - Rothman Orthopaedics
- Hand and Upper Extremity - University of Utah Health
- Arthroplasty - Tahoe/Reno Orthopedic Center
- Adult Reconstruction – Houston Methodist
2020 Fellowships
- Spine - New York University
- Adult Reconstruction - Florida Orthopaedic Institute
- Adult Reconstruction - Scripps, San Diego
- Musculoskeletal Oncology - Massachusetts General Hospital/Harvard Medical School
- Foot and Ankle - Baylor, Dallas
2019 Fellowships
- Adult Reconstruction - Rothman Institute, New Jersey
- Adult Reconstruction - Washington University, St. Louis, MO
- Sports Medicine - Jefferson University, Philadelphia, PA
- Spine - New York University
- General Orthopaedics
2018 Fellowships
- Hand and Upper Extremity – University of Chicago
- Hand and Upper Extremity – University of Alabama, Birmingham
- Hand and Upper Extremity – Cleveland Clinic
- Hand and Upper Extremity – University of Cincinnati
- Adult Reconstruction – Tahoe/Reno Arthroplasty
2017 Fellowships
- Adult Reconstruction – Scripps Health, San Diego, CA
- Adult Reconstruction – University of Utah, Salt Lake City, UT
- Adult Reconstruction – Melbourne Orthopaedic Group, Melbourne, Australia
- Sports Medicine – Steadman Hawkins Clinic, Denver, CO
2016 Fellowships
- Adult Reconstruction – Mayo Clinic, Scottsdale, AZ
- Adult Reconstruction – Indiana University, Bloomington, IN
- Trauma & Adult Reconstruction – Dr. Paul Duwelius, Orthopaedic + Fracture Specialists, Portland, OR and Sydney Arthroplasty and Trauma, Sydney, Australia
- Shoulder & Elbow Surgery – Cleveland Clinic, Cleveland, OH
- Spine Surgery – Cleveland Clinic, Cleveland, OH
2015 Fellowships
- Adult Reconstruction – Tahoe Reno Arthroplasty, Reno, NV
- Adult Reconstruction – University of California-Davis, Davis, CA
- Hand & Upper Extremity – University of New Mexico, Albuquerque, NM
- Pediatric Orthopaedics – Children’s Hospital of Pittsburgh, Pittsburgh, PA
- Foot & Ankle – Melbourne Orthopaedic Group, Melbourne, Australia and Summit Orthopaedics, Portland, OR
2014 Fellowships
- Sports Medicine – University of Pennsylvania, Philadelphia, PA
- Foot and Ankle – University of California-Davis, Davis, CA
- Spine – Spine Institute of Arizona, Scottsdale, AZ
- Orthopaedic Traumatology – R Adams Cowley Shock Trauma Center/University of Maryland
- Shoulder and Elbow – Rothman Institute, Thomas Jefferson University, Philadelphia, PA
Additional information
For additional information about the residency program please contact:
Robin Sasaoka
Residency and fellowship education manager
Phone: 503 494-5842
sasaokar@ohsu.edu