Mpox: Frequently Asked Questions
What you need to know about symptoms, exposure, vaccines and protecting your health
Mpox is part of a family of viruses called poxviruses that cause a painful rash with blisters. OHSU experts say mpox is a rare virus that doesn’t spread as easily as COVID-19 or respiratory viruses.
OHSU has the Jynneos vaccine for mpox. Make a pharmacy appointment.
Jump to:
Mpox basics
-
What is mpox?
The virus is part of a family of viruses called poxviruses. They include smallpox. Poxviruses cause a painful rash that can look like pimples or blisters. A poxvirus infection can also cause health problems and, rarely, death.
Mpox was first reported in 1958 after it sickened monkeys in a research center in Denmark. It became known as monkeypox even though the monkeys were not the source. Scientists believe rodents carry the virus.
The first human case was reported in 1970. In 2003, the United States had an outbreak of 47 cases in six states linked to pet prairie dogs.
-
Is mpox a sexually transmitted disease?
No. While people can get the virus during sex, it is not considered a sexually transmitted disease because it can spread in other ways.
-
Are there different kinds of mpox?
Health officials say two strains of the virus have been reported since the most recent outbreak started in 2022.
Mpox symptoms and spread
-
What are signs and symptoms of mpox?
Symptoms usually start within three weeks of being exposed to the mpox virus.
Most people develop rashes, which can lead to sores that look like pimples or blisters. These can burst, leading to painful or itchy open sores that contain live virus.
Other symptoms include:
- Fever
- Intense headache
- Muscle aches
- Swollen lymph nodes
- Chills
- Lack of energy
- Sore throat, stuffy nose and coughing
Mpox rash examples
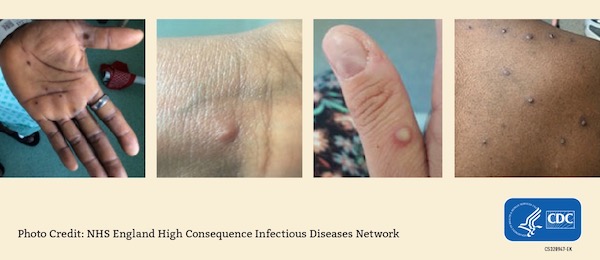
-
How does mpox spread?
The virus spreads mostly through lengthy, skin-to-skin contact with an infected person. It can spread through personal items such as clothing, bedding or towels.
OHSU experts say that casual contact, such as a handshake, is highly unlikely to spread the virus.
If you are pregnant and become infected with the virus, you can pass it:
- To your fetus through the placenta.
- To your newborn during close contact after birth.
-
How long is mpox contagious?
Infected people should be considered contagious from the time their symptoms start until the scabs from their rash fall off and a new layer of skin forms. This usually takes two to four weeks.
OHSU experts say that once people have recovered from the virus, they can no longer spread it.
-
What is the incubation period for mpox?
An incubation period is the time between getting infected and showing symptoms. OHSU experts say the incubation period for the virus is usually seven to 14 days but can range from five to 21 days.
-
Can you get mpox more than once?
Infectious-disease experts say that, based on what we know about closely related viruses, people who get infected or vaccinated should have long-term immunity.
Immunity can weaken for several reasons, including:
- Medications and medical treatments that suppress the immune system
- Untreated or unknown HIV infection
Information is limited on how long the vaccine remains effective.
-
What are the effects of mpox besides symptoms?
The virus can cause a range of complications such as:
- Scarring
- Secondary infections, including tonsillitis
- Pneumonia
- Vision loss
- Pregnancy complications including pregnancy loss
-
Can mpox cause death?
The WHO says the case fatality ratio (the portion of diagnosed cases that lead to death) has been 3% to 6% in recent years. Because not all cases are diagnosed or reported, the fatality rate among all cases is lower.
Mpox prevention
-
How can I protect myself from mpox?
If you are in a high-risk group, talk with your doctor about getting vaccinated against mpox.
OHSU experts recommend that you avoid:
- Having unprotected contact with an infected person’s skin lesions, body fluids or personal items.
- Having lengthy face-to-face contact (within 6 feet) with an infected person without masks.
If you share a household or health care setting with an infected person, you can use common household disinfectants to kill the virus on shared surfaces and personal items.
-
Who is at risk of getting mpox?
Anyone can get the virus. Most cases in the 2022 outbreak were in men, and mostly among men who have sex with men.
People who have not gotten a smallpox vaccine also may be more vulnerable to the virus, the CDC says. The United States stopped routine smallpox vaccinations in 1972.
For those who have had a smallpox vaccination, one childhood dose can offer up to 75 years of protection, OHSU researchers found.
See these related questions to learn more about those considered at high risk of getting mpox:
Mpox vaccines
-
Is there a vaccine for mpox?
The U.S. Food and Drug Administration has approved two vaccines for poxviruses, the family of viruses that includes mpox:
- Jynneos is for use in people ages 18 and older who are at high risk of infection with the virus. Jynneos can also be used for people under 18 under FDA “expanded access” rules.
- ACAM2000 is approved for use against smallpox in people who are considered at high risk of infection. The FDA has made it available for use against mpox under “expanded access” rules.
Neither vaccine contains smallpox or mpox. Both are made from a related virus that does not cause disease in humans. Both spur the immune system to make antibodies to fight infection.
Both vaccines may have side effects including pain, swelling, fever and rash.
-
Are the vaccines for mpox safe?
Both Jynneos and ACAM2000 have FDA approval for use against poxviruses. That means they were cleared for use after extensive testing in people.
Jynneos is linked to few possible complications. It can be given even to people with weakened immunity.
ACAM2000 is linked to a risk of myocarditis and pericarditis, potentially serious inflammation of the heart muscle and surrounding tissue. Risk is higher for those who have never had a smallpox vaccine, such as most people under age 60.
The CDC says ACAM2000 should not be given to people who:
- Have severely weakened immunity
- Are living with HIV
- Have skin conditions such as eczema or psoriasis
- Have heart disease
- Have eye disease treated with topical steroids
- Are pregnant
- Are less than 12 months old
-
How are the vaccines given?
Jynneos is given in two doses, typically 28 days apart. A dose is usually injected under the skin of the underside of the forearm. Jynneos may also be given in the upper back, under the skin just below the shoulder blade.
ACAM2000 is given in one dose with a two-pronged needle. The needle is dipped in vaccine and then used to quickly prick a small section of arm skin multiple times.
-
When should I get vaccinated for mpox?
After exposure: OHSU experts say getting a vaccine within four days of exposure can stop an infection. Getting a vaccine within 14 days of exposure can reduce the length and severity of an infection.
Before exposure: The Oregon Health Authority says some people at high risk of infection should get or be considered for vaccination. See "Who should get the Jynneos vaccine?"
OHSU has Jynneos. See "Who can get vaccinated at OHSU?" to learn who qualifies.
-
How can I get vaccinated for mpox?
Vaccines are available for people who have been exposed to mpox or who are considered at high risk of infection.
- OHSU has Jynneos. Make a vaccine appointment.
- Call your health care provider.
- Call your public health department:
-
Who can get vaccinated at OHSU?
The mpox vaccine (Jynneos) is available to anyone who is eligible. You do not need to share your personal risk.
You can get the mpox vaccine if you:
- Are 18 or older.
- Do not have symptoms that are or could be from mpox (rash, fever, swollen lymph nodes, muscle aches, backache or headache).
- Have no history of mpox infection.
- Have not had a severe reaction to the mpox vaccine.
- Have been exposed to the virus in the last 14 days.
If you’ve been exposed to mpox, you should get vaccinated right away, ideally within four days of exposure.
To schedule an appointment:
- Call OHSU Physicians Pavilion Pharmacy, Marquam Hill, at 503-494-7570. Pharmacy hours are 8 a.m.-9 p.m. weekdays, 9 a.m.-5:30 p.m. weekends.
- Use our vaccine scheduling tool.
You can also:
- Contact your provider or schedule an in-person or virtual Immediate Care visit.
- Contact your public health department:
-
Who should get the Jynneos vaccine?
Under Oregon Health Authority guidelines, people should get or be considered for a Jynneos vaccination if they:
- Have been in contact with people who have a presumed or confirmed case of mpox.
- Are at higher risk of mpox infection.
- Are lab workers who do mpox tests.
- Are health care workers who have been exposed to mpox without personal protective equipment.
-
Should children be vaccinated against mpox?
The virus can cause more severe disease in children, according to OHSU experts.
The CDC says children may be eligible for vaccination if they have had close personal contact with someone who has or may have mpox.
-
Should people 60 and older automatically be vaccinated against mpox?
No. OHSU experts say most Americans age 60 and older have had the smallpox vaccine, which also protects against mpox. OHSU researchers found that the smallpox vaccine provides immunity for up to 75 years after a single childhood dose.
Mpox exposure, testing and treatment
-
I may have been exposed to mpox. What should I do?
If you think you have been exposed to mpox, OHSU experts encourage you to:
- Check yourself for symptoms for 21 days after your most recent exposure. This includes taking your temperature twice a day to check for fever.
- Stay away from group events.
- Avoid public transportation.
- Avoid donating blood, tissue, breast milk, sperm or organs.
If you develop symptoms, you are encouraged to:
- Stay away from people and pets (isolate).
- Seek testing and medical care.
- Cover your lesions if possible.
- Wear a mask.
- Keep your used clothing and bedding in a separate bag or container that can be disinfected, and wash your clothing and bedding separately from other laundry.
-
Can I get tested for mpox?
Yes. Ask your health care provider about getting a test. If you do not have a health care provider, call your local public health department:
- Oregon health departments
- Washington health departments
- Clackamas County Health, Housing and Human Services
- Multnomah County Health Department
- Washington County Health & Human Services
-
Is there a treatment for mpox?
Most people who get mpox recover without treatment within two to four weeks.
For more serious cases, the CDC and FDA allow the use of tecovirimat, or TPOXX, an antiviral drug approved for smallpox. Ask your doctor about tecovirimat.
-
How can I take care of myself if I have mpox?
Most people who get mpox can care for themselves at home. The most common concerns are rashes (lesions), pain and itching.
How to care for rashes:
- Keep them clean and dry.
- Cover them with gauze, long sleeves, pants or gloves.
- Avoid scratching a rash, popping a lesion or picking a scab.
- Avoid shaving the skin around rashes or lesions.
- Apply povidone-iodine ointment (Betadine) to reduce the risk of spreading the virus and to speed healing.
- If a lesion is producing fluid, dispose of any soaked gauze where others can’t come into contact with it. Place clothing or bedding that has come into contact with the fluid in a separate bag or container that can be washed or disinfected afterward.
If you touch a rash:
- Wash your hands with soap and water or a hand sanitizer with alcohol in it.
- Avoid touching sensitive body parts such as the eyes, nose, mouth, genitals or anus. A rash that gets in the eyes can cause vision loss.
If you have a rash on your hands:
Wear gloves when touching shared surfaces or objects. Reusable gloves should be washed with soap and water after each use.If you have a rash in your mouth:
Rinse with saltwater several times a day. If the rash is painful, talk to a health care provider about a prescription mouthwash or a local anesthetic.How to manage pain or itching:
- Pain: Take ibuprofen (Advil, Motrin) or acetaminophen (Tylenol).
- Itching: Take an oral antihistamine (Benadryl). Apply a numbing gel (lidocaine), steroid cream, calamine lotion or ointment (Aquaphor, Vaseline).
In general:
- Stay home and rest as much as possible.
- Wear a mask around others if you have a rash in your mouth or throat.
- Drink lots of fluids.
When to seek medical care:
- Pain: If you have pain that can't be managed with over-the-counter medications.
- Rashes: If a rash spreads toward an eye or another area that may be especially sensitive, including broken skin; and if rashes spread over more than 5% or 10% of your body surface. (The arm is about 9% of your body surface).
- Infection: If you think you have signs of a secondary infection, including fever (100.4 or higher), chills or sweats, swollen lymph nodes or a new rash.
Find an mpox test or vaccine
OHSU has the Jynneos vaccine. Contact your provider or schedule a pharmacy appointment.
You can also contact your public health department:
More information about mpox
- Oregon Health Authority information
- Mpox, The New York Times
- Stat information
Tracking mpox
- In Oregon, Oregon Health Authority
- Around the world, World Health Organization