Understanding Alzheimer’s Disease
Alzheimer’s disease is a type of dementia. Dementia, a group of brain disorders, causes memory loss and other problems with thinking. It usually occurs in older people.
Important things to know:
- Alzheimer’s disease does not have a cure, but treatment can slow symptoms and improve quality of life.
- Many people become forgetful with age. Forgetfulness does not necessarily mean you have Alzheimer’s.
- Research shows that healthy habits, such as exercising and spending time with loved ones, can lower your risk of Alzheimer’s.
- Scientists, including at the Layton Aging & Alzheimer's Disease Center, are striving to develop better treatments.
What is Alzheimer’s disease?
Alzheimer’s disease is the most common form of dementia. About 60-80% of people with dementia are diagnosed with Alzheimer's disease, according to the Alzheimer’s Association.
With Alzheimer’s, brain cells gradually die. Their connections vanish, preventing sections of the brain from communicating. This causes:
- Changes in emotion and behavior that can include depression, anger and restlessness
- Loss of memory, reasoning and thinking
Living with Alzheimer’s disease
Alzheimer’s gets worse over time. Treatment can't stop the disease, but it can slow symptoms.
Early stages cause mild loss of memory and other functions. Gradually, people lose the ability to live on their own and need help with all activities.
How quickly it gets worse varies by person and type of Alzheimer’s (early or late onset). Some people live with Alzheimer’s up to 20 years after diagnosis. Most live with it for four to eight years.
Who gets Alzheimer’s disease?
About 6.9 million people in the U.S. are living with Alzheimer’s disease, according to the Alzheimer’s Association. About 1 in 9 people age 65 and older have it, as do 1 in 3 age 85 and older.
Alzheimer’s disease risk factors
Having a risk factor doesn’t mean you will get Alzheimer’s. Not having one doesn’t mean you won’t.
- Age: Alzheimer’s isn't a normal part of aging, but it's most common among those 65 and older.
- Family history: People with a parent or sibling who has or had Alzheimer’s are at higher risk. Risk increases if you have more than one relative with Alzheimer’s.
- Gender: Women are at higher risk.
- Race and ethnicity: Black people have about twice the risk compared with white people. Latinos have about 1½ times the risk that white people do.
- Genetics: Scientists have identified genetic changes that increase risk. They don't fully understand how the changes can lead to Alzheimer’s, though.
- Down syndrome: People with Down syndrome are more likely to develop Alzheimer’s. They also tend to develop it about 10 to 20 years earlier than others.
- Head trauma, or mild memory and thinking issues: People who have had a traumatic brain injury or who have memory or other thinking problems are at higher risk.
Lowering risk of Alzheimer’s disease
Lifestyle changes can lower risk. Alzheimer’s disease is linked to heart and blood vessel health, for example.
To lower risk, you can:
- Quit smoking.
- Get regular exercise.
- Get enough sleep.
- Eat a healthy diet with plenty of fruits and vegetables.
- Get treatment to manage health conditions. Be especially alert to depression, type 2 diabetes, high blood pressure and high cholesterol.
- Keep a healthy weight.
- Keep your mind active through lifelong learning.
- Spend time with family and friends.
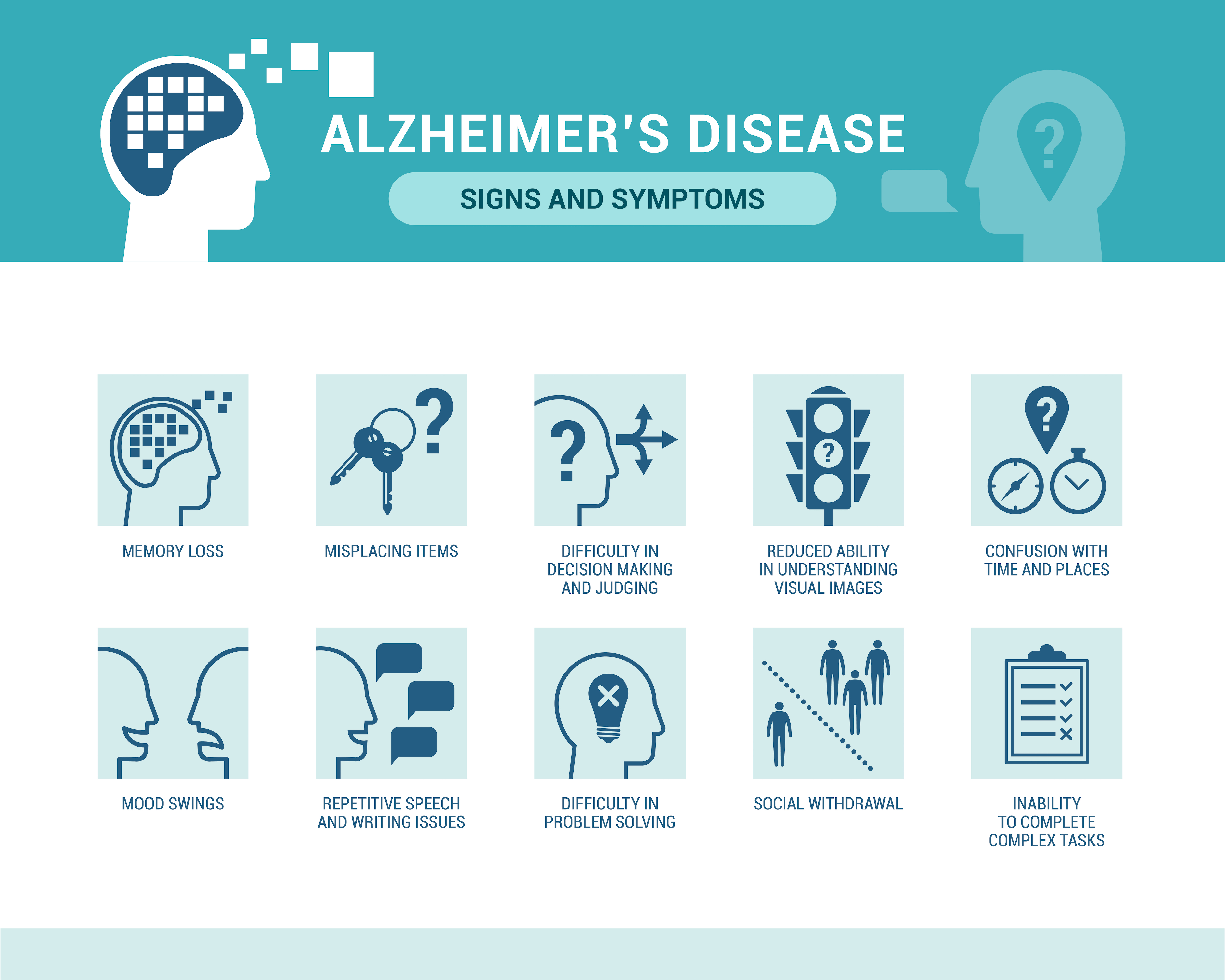
Stages and symptoms of Alzheimer’s disease
Early-stage Alzheimer's disease
In early-stage Alzheimer’s disease, people begin to notice they are forgetful or confused. Symptoms may look like normal aging or those of other conditions. People can usually do most daily tasks.
Early-stage signs and symptoms:
- Short-term memory loss, such as forgetting appointments or repeating questions
- Trouble with tasks that used to be easy
- Taking much longer with routines
- Putting things in unusual places and getting upset or suspicious when they aren't found
- Trouble with common words or with tracking conversations
- Confusion with times, dates or familiar places, such as getting lost on the way home
- Loss of interest in favorite activities or social events
- Less judgment with money, safety or health
- Mood or behavior changes, or being more impulsive
Moderate-stage Alzheimer's disease
With moderate-stage Alzheimer's, signs and symptoms may interfere with self-care and other daily tasks. People may need more supervision. This stage can last many years.
Moderate-stage signs and symptoms:
- Trouble with daily tasks such as dressing, driving, reading or writing
- Forgets current or life events
- Lacks judgment or sense of danger
- Mixes up or mispronounces words
- Believes things that aren’t true (delusions) or sees things that don’t exist (hallucinations)
- Mood changes such as depression, agitation or aggression
- Avoids social contact
Late-stage Alzheimer's disease
People with late-stage Alzheimer’s need constant help with daily tasks. They can't have a conversation or respond to what’s happening around them.
They may have trouble swallowing. Food or drink can enter the lungs, causing aspiration pneumonia. For most people with Alzheimer's, this pneumonia is the direct cause of death.
Late-stage signs and symptoms
- Doesn't recognize family members
- Can’t eat, dress or bathe
- Can’t communicate
- Lacks bladder or bowel control
When to get checked for Alzheimer’s disease
Everyone forgets things from time to time, especially as we age. But age-related memory problems are quite different from those that come with Alzheimer’s.
People with Alzheimer’s disease may not realize they have a problem, even as family or friends notice changes. If you recognize signs in yourself or a loved one, see a doctor for a full exam.
Your doctor can use tests to trace the cause of your symptoms and to rule out other possible causes. Learn about diagnosis and treatment at the Layton Aging & Alzheimer’s Disease Center.
How Alzheimer’s Affects Brain Cells
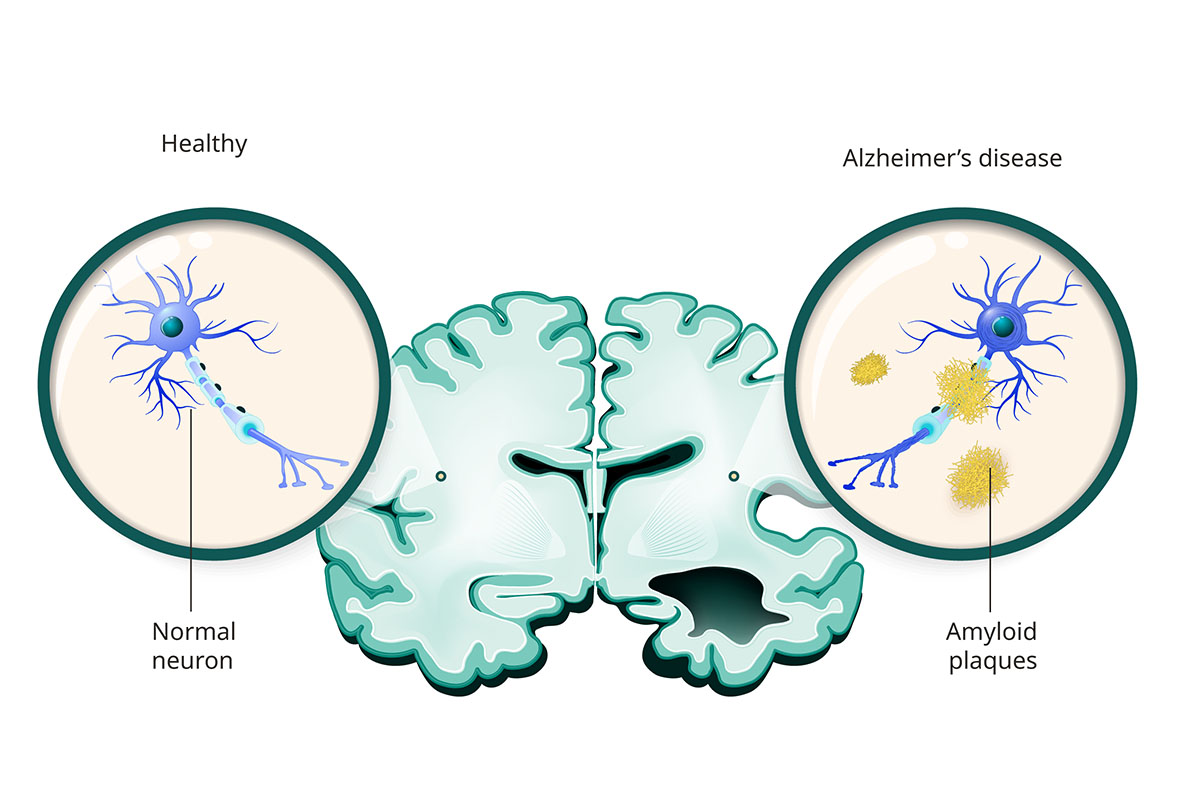
What causes Alzheimer’s disease?
Doctors don’t understand the exact causes. Alzheimer’s may result from a combination of genetic, environmental and lifestyle factors.
Alzheimer’s disease affects a type of brain cell called a neuron. Neurons send messages between parts of the brain, and between the brain and the rest of the body.
Changes to neurons and the brain from Alzheimer’s include:
- Shrinkage: The brain shrinks as networks of neurons break down. This is also known as brain atrophy.
- Amyloid plaques: A naturally occurring protein called amyloid-beta can build up in the brain for reasons doctors don't fully understand. It can form clumps, known as plaques, between neurons that keep them from communicating.
- Neurofibrillary tangles: Tau, another naturally occurring protein, builds up inside neurons. Tau forms threads known as tangles. The tangles keep neurons from communicating and transporting nutrients. Without nutrients, neurons die.
Types of Alzheimer’s disease
Early onset: Symptoms start in the person's 40s or 50s. The disease tends to worsen quickly. This type is much less common than late-onset Alzheimer’s, making up less than 5% of cases.
Late onset: This is the most common type, typically affecting people age 65 and older. Symptoms usually worsen more slowly than in early-onset Alzheimer’s.
Familial Alzheimer’s disease: This rare type results from genetic changes passed down from parent to child. Familial Alzheimer’s makes up less than 1% of cases overall but about 60% of early-onset cases.
-
Other types of dementia
Frontotemporal dementia: FTD results from neuron loss in the brain’s frontal lobes (behind the forehead) or temporal lobes (behind the ears). FTD usually begins in a person’s 40s or 50s. It generally causes more problems with behavior and speech than Alzheimer’s does.
Lewy body dementia: Lewy body dementia results from unusual buildup in the brain of a protein called alpha-synuclein. It usually begins in people age 50 and older.
Parkinson’s disease dementia: Parkinson’s disease first affects areas of the brain that control movement. Changes can spread to areas involved with memory and thinking.
Vascular dementia: Reduced blood flow to the brain can cause memory loss and other thinking problems. Vascular dementia is the most common dementia after Alzheimer’s.
Mixed dementia: Some people have a combination of dementias. Because doctors can't diagnose most types of dementia for certain until after a person dies, most people are treated for only one type.
-
Other brain disorders with dementia
These are some of the brain disorders that can lead to dementia or cause dementia-like symptoms:
Creutzfeldt-Jakob disease: This rare brain disorder occurs when a protein known as a prion develops an unusual shape. CJD, a fatal illness, causes dementia that worsens quickly. Learn about prion diseases.
Huntington’s disease: A damaged gene causes this inherited brain disorder. It causes neuron loss, especially in parts of the brain that control voluntary movement. Symptoms usually start between ages 30 and 50. Huntington's gets worse over time. Learn about Huntington’s disease.
Korsakoff syndrome: This memory disorder results from a severe lack of vitamin B1 (thiamine), usually due to heavy alcohol use.
Normal pressure hydrocephalus: NPH occurs when fluid builds up in the brain’s ventricles, or cavities. It causes include bleeding, inflammation or infection in the brain.
Posterior cortical atrophy: This condition occurs in the outer layer of the brain at the back of the head. It may be related to Alzheimer’s disease. It typically begins between ages 50 and 65. Patients are less able to process visual information. They can have trouble reading, for example, or moving through space.
Genetic testing and Alzheimer’s disease
Testing can show whether you have a version (variant) of a gene that increases your risk of Alzheimer’s. Testing can also uncover the rare cases when an inherited genetic change, or mutation, causes Alzheimer’s.
At OHSU, we generally do not recommend routine genetic testing for Alzheimer’s because:
- Many factors can lead to the disease.
- Most people who develop Alzheimer’s do not have a related genetic variant.
- Most people who have a variant do not develop the disease.
Talk with your primary care doctor or to a medical geneticist to learn more or to better understand risk if you’ve taken a test on your own.
-
Testing for familial Alzheimer’s disease
Genetic testing can show whether you carry an inherited genetic mutation that causes early-onset Alzheimer’s. We may recommend testing to confirm a diagnosis in someone with symptoms.
Some family members, after careful discussion with a genetic counselor, may want testing to see if they carry the mutation.
-
Testing for late-onset Alzheimer’s disease
At-home DNA tests can detect variants that increase risk of late-onset Alzheimer's, but without guidance from a genetic counselor. It’s important to know:
- These tests don't diagnose any health conditions.
- The tests don’t check for all variations linked to late-onset Alzheimer's disease.
- They don't check for mutations linked to early-onset Alzheimer's disease.
Learn more about the genetics of Alzheimer’s disease from the National Institute on Aging.
Learn more
- Alzheimer’s Disease, National Institute of Neurological Disorders and Stroke
- Alzheimer’s Disease, U.S. National Library of Medicine
- Alzheimer’s Association
For patients
- Referral: To become a patient, please ask your doctor for a referral.
- Questions: For referrals or follow-up appointments, call 503-494-7772.
- Nurse line: To talk with a nurse, call 503-494-7615.
Location
Center for Health & Healing Building 1, eighth floor
3303 S. Bond Ave.
Portland, OR 97239
Free parking for patients and their visitors
Refer a patient
- Refer your patient to OHSU.
- Call 503-494-4567 to seek provider-to-provider advice.
Resources
- Resources for patients and families
- Learn about research opportunities: 503-494-7647 or adresearch@ohsu.edu
- Look for a clinical trial