The Strategies to Innovate EmeRgENcy Care Clinical Trials Network (SIREN)
What is SIREN?
The goal of the SIREN Network is to improve the outcomes of patients with neurologic, cardiac, respiratory and hematologic emergencies by identifying effective treatments given in the earliest stages of care. SIREN is a cooperative and highly integrated clinical trials network that will build upon guiding design principles and organizational values essential for success. These include focus on:
- early treatment
- meaningful outcomes for patients
- efficiency
- collaboration
- transforming the clinical trials enterprise
SIREN at OHSU
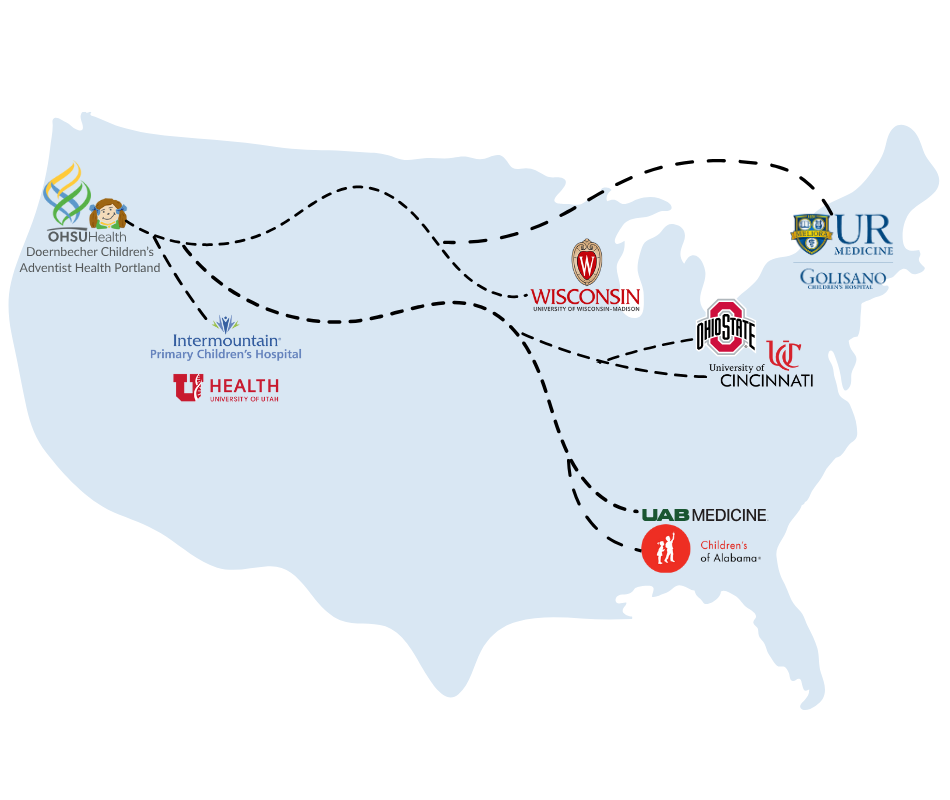
As a 'hub' site within the SIREN network, OHSU has created a network of partner institutions who will collaborate and participate with OHSU in SIREN trials. Our partner institutions are nationwide and represent a diverse group of patients, populations, and care teams.
Recent News & Events
Learn more about our new training program, HONE-IT and how eligible candidate can apply to join!
We have received the official Notice of Award from the NIH for years 6-10 of our OHSU SIREN Network. The new award started on February 1st, 2023, and will run for 5 years until 01/31/2028. The SIREN Award Hub network grew, adding four new hubs to the network this funding cycle. Yale, UC Davis, Duke, and Hopkins are new, and 8 hubs were renewed: University of Chicago, Pittsburgh, OHSU, Temple, University of Washington, VCU, University of Minnesota, Wayne State, and UCLA.
Our network now consists of:
- OHSU (award hub)
- OHSU-Adventist (spoke)
- OHSU-Doernbecher Children’s(spoke)
- The Ohio State University (Hub)
- OSU-East (spoke of OSU)
- University of Alabama – Birmingham (spoke)
- Children's Hospital of Alabama (UAB) (hub)
- University of Rochester Medical Center – Strong Memorial (spoke)
- Golisano Children's Hospital (URMC) (hub)
- University of Utah (hub)
- University of Wisconsin (spoke)
- University of Cincinnati (hub)
- Primary Children's of Utah (spoke)
Studies
Please read our newsletter (above) for the latest updates on trials such as network and site-specific enrollment totals.
BOOST-3 - Brain Oxygen Optimization in Severe TBI Phase-3
- Registered with ClinicalTrials.gov: NCT03754114
- NIH Project Number: 1U01NS099046-01A1
The study will determine the safety and efficacy of a strategy guided by treatment goals based on both intracranial pressure (ICP) and brain tissue oxygen (PbtO2) as compared to a strategy guided by treatment goals based on ICP monitoring alone. Both of these alternative strategies are used in standard care. It is unknown if one is more effective than the other.
This study began enrolling in Sept 2019. OHSU Partner site University of Rochester Medical Center - Strong Memorial Hospital is currently enrolling subjects. OHSU began enrollment locally on March 16, 2020. Duke University Medical Center, Ohio State University Wexner Medical Center, and University of Utah, and University of Cincinnati also participate.
BioBOOST - The main goal of Bio-BOOST is to determine how the lack of oxygen to brain tissues affects the levels of blood tests for brain injury. OHSU is 1 of 10 sites that will be participating in the sub-study of BOOST3. This study is ending in 2026.
ICECAP - Influence of Cooling Duration on Efficacy in Cardiac Arrest Patients
- Registered with ClinicalTrials.gov: NCT04217551
- NIH Project Number: 1UG3HL145269-01A1
The Influence of Cooling duration on Efficacy in Cardiac Arrest Patients (ICECAP) study will enroll comatose adult survivors of out of hospital cardiac arrest that have already been rapidly cooled using a definitive temperature control method. Those with and without initial shockable rhythms will be studied as distinct populations (maximum of 1800 subjects over four years). ICECAP will determine if identifying an optimal duration of cooling can improve outcomes, and if development of a duration response curve can substantiate efficacy in a wider patient population.
This study concluded in 2025. The results will be forthcoming.
C3PO - Clinical Trial of COVID-19 Convalescent Plasma of Outpatients
The Clinical Trial of COVID-19 Convalescent Plasma in Outpatients (C3PO) is a multi-center randomized, single blind, two arm, placebo controlled phase III trial with blinded outcome assessment to establish the safety and efficacy of a single dose of convalescent plasma (CP) for preventing the progression from mild to severe COVID-19 illness.
COVID-19 is a respiratory illness caused by the Severe Acute Respiratory Syndrome Coronavirus 2 (SARS-CoV-2).
The overarching goal of this trial is to confirm or refute the role of passive immunization as a safe and efficacious therapy in preventing the progression from mild to severe/critical COVID-19 illness and to understand the immunologic kinetics of anti-SARS-CoV-2 antibodies after passive immunization.
This concluded in 2021. The results are were published in 2021
Korley FK, Durkalski-Mauldin V, Yeatts SD, Schulman K, Davenport RD, Dumont LJ, El Kassar N, Foster LD, Hah JM, Jaiswal S, Kaplan A, Lowell E, McDyer JF, Quinn J, Triulzi DJ, Van Huysen C, Stevenson VLW, Yadav K, Jones CW, Kea B, Burnett A, Reynolds JC, Greineder CF, Haas NL, Beiser DG, Silbergleit R, Barsan W, Callaway CW; SIREN-C3PO Investigators. Early Convalescent Plasma for High-Risk Outpatients with Covid-19. N Engl J Med. 2021 Nov 18;385(21):1951-1960. doi: 10.1056/NEJMoa2103784. Epub 2021 Aug 18. PMID: 34407339; PMCID: PMC8385553.
POST-ICECAP - Patterns of Survivors' Recovery Trajectories in the ICECAP Trial
- NIH Project Number: 1R01NS127959-01A1
This study will be among the first to focus on a new equitable science of OHCA survivorship itself, seeking empirically derived targets for preserving or restoring recovery. Our single-center pilot study has found that nearly one-third of the OHCA survivors had clinically important differences between long-term (12 months) and short-term (3 months) functional outcomes with large between- individual variability in recovery (i.e., improvement or worsening).
KESETT -Ketamine add-on therapy for Established Status Epilepticus Treatment Trial
- NIH Project Number: 1UG3NS131532-01A1
A multicenter, randomized, blinded study of treatment of patients with benzodiazepine-refractory status epilepticus in the emergency department, with either levetiracetam or levetiracetam combined with 1 mg/kg or 3 mg/kg dose ketamine to determine which treatment leads to more effective control of status epilepticus.
This trial begins in 2026. OHSU, Doernbecher, OSU, University of Utah, Primary Children's of Utah, University of Alabama-Birmingham, Children's of Alabama, University of Cincinnati
WINDSURFER - WIN ratio analysis to Determine a strategy of non-invasive SUpport for Respiratory Failure in the ER
- NIH Project Number: 1UG3HL175260-01A1
We propose the WINDSURFER trial to answer one of the signature questions of emergency care; “What is the best non-invasive respiratory support (NIRS) strategy for treating acute hypoxemic respiratory failure (AHRF) in the Emergency Department (ED)?” AHRF is the syndrome of impaired breathing resulting in low blood oxygen levels, most commonly from lung or other infections, acute decompensated heart failure (ADHF) and chronic obstructive pulmonary disease (COPD). AHRF is a major public health problem as evidenced by its seasonal and pandemic surges and the >100,000 associated deaths each year in the United States. Aggressive treatment of AHRF at its earliest stages in the Emergency Department (ED) is essential to prevent progression to death. Non-Invasive Respiratory Support (NIRS) is an important and widely used rescue treatment for AHRF that provides effective high-level breathing support without the pitfalls and consequences of mechanical ventilation.
This study will start in 2026. OSU, OSU-East, and the University of Cincinnati will be participating.