Brain Tumor Treatment
At the OHSU Brain Institute, you’ll find an expert team and the latest approaches to brain tumor care. We offer:
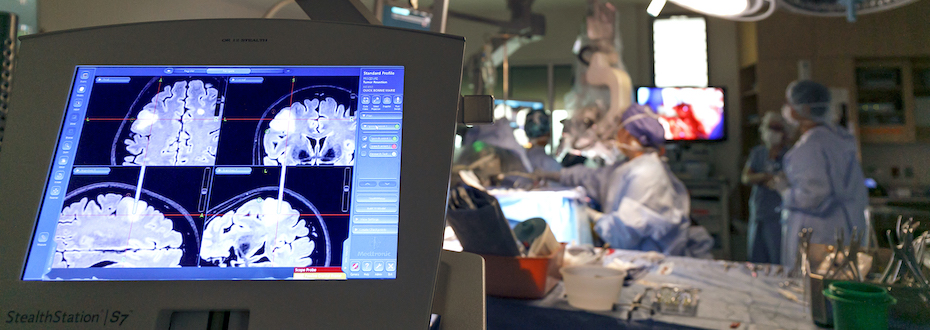
- Leading treatments, including less invasive options and real-time imaging to make surgery safer and more successful.
- Doctors with extensive training and experience who focus only on brain tumors.
- A weekly meeting where our brain tumor specialists work together for your care.
- Access to clinical trials that test promising new treatments, including a new method we developed to improve chemotherapy.
- Personalized treatment plans, based on your tumor’s size, location and genetic traits.
What to expect
Your plan will most likely include more than one treatment. You can also expect:
- Prompt care, typically meeting with our team within two weeks.
- Multiple specialists who see you during one visit, so you don’t have to come back more than necessary.
- Timely, precise diagnosis, even if you had your first evaluation with a doctor outside the Brain Institute. We provide test results within a day whenever possible.
- Custom treatment plan based on your test results.
- All your questions answered. We explain your options in detail and create your treatment plan with your help. We encourage you to ask questions, so you feel confident about your care.
- Doctors who are part of the OHSU Knight Cancer Institute, one of the nation’s top centers for cancer care and research.
Our expertise
As the only academic neuro-oncology program in Oregon, we care for hundreds of patients each year. We offer you specialists such as:
- Neuro-oncologists, who diagnose brain tumors and treat them with medications.
- Neurosurgeons, who use advanced surgical techniques to remove brain tumors.
- Neuroradiologists, who use imaging to help diagnose brain tumors.
- Neuropathologists, who examine tissue samples to help diagnose brain tumors.
- Radiation oncologists, who provide targeted radiation therapy to destroy tumors.
Surgery for brain tumors
Many people diagnosed with a brain tumor have surgery to remove as much of the tumor as possible. In some cases, this is the only treatment needed.
-
Our neurosurgeons are all fellowship-trained, with advanced knowledge of the skull base and the intricate blood vessels of the brain. Our highly skilled surgeons do hundreds of brain surgeries a year. Studies show better outcomes at centers that do many surgeries.
-
Our team uses advanced tools to:
- Make sure you receive the best treatment for you.
- Take out as much of the tumor as possible, with the smallest incision possible.
- Protect the parts of your brain that control speech, movement and your senses.
Tools include:
- MRI: We map areas of the brain controlling speech and other functions before and during surgery. We are the only center in Oregon with intraoperative MRI to scan the brain during surgery. We can target your tumor and make sure we remove as much as possible.
- Advanced contrast agents: Before an MRI, we inject special dyes to highlight the more aggressive parts of the tumor to make sure we remove and test them.
-
MRI-guided laser ablation: For some tumors, surgeons can make a small incision and use an image-guided laser to destroy the tumor (ablation).
Keyhole surgery: Endoscopic (keyhole) surgeries for certain brain tumors use a small incision for an easier recovery.
Awake craniotomy: We remove a small piece of the skull so we can reach the tumor. We ask you to answer questions or make small movements during surgery to help us remove as much tumor as possible without harming sensitive areas. We replace the piece of skull bone at the end of the surgery.
Cerebrovascular neurosurgery: These complex surgeries treat skull base tumors. These are tumors on the bottom of the brain and behind the eyes and nose.
Skull base neurosurgery: We often use endoscopic, minimally invasive procedures to remove skull base tumors through the nose or mouth, avoiding a skull incision.
Pituitary tumor surgery: Surgeons work closely with endocrinologists (doctors who are experts in hormone conditions) to find the best combination of medication and surgery.
Find out more about surgical technology at OHSU.
Radiation therapy for brain tumors
You may need high doses of radiation to shrink or destroy the tumor. Our team uses one of the most advanced radiation therapy systems available.
Our radiation oncologists work with your brain tumor team, including neurosurgeons, to plan precise radiation therapy. This therapy may be the only treatment we recommend, or we may recommend it after surgery to destroy any remaining cancer cells.
-
Radiation sessions are also called fractions. They usually happen daily, Monday through Friday, for several weeks. Each session lasts about 30 minutes.
Simulation: During this planning phase, your team determines the dose and precise angles for the radiation beams.
Precise targeting: We mold and target the beams directly to the tumor. This lets us use a high dose while protecting healthy tissue.
Side effects: The treatment is not painful, but you may experience side effects. You may feel tired, nauseous, or have a headache. You may lose hair in the targeted area.
-
Radiation therapy for brain tumors is external. This means you lay on a table while we direct the radiation beams at the tumor.
Stereotactic radiosurgery delivers a precise dose of radiation to the tumor in just one session or a few sessions. We use SRS for brain tumors that we can’t remove surgically. This is also an option if you aren’t a good candidate for surgery due to other health conditions.
3-D conformal radiation therapy (3D-CRT) uses several high-dose radiation beams from different directions that are shaped to match the tumor.
Intensity-modulated radiation therapy (IMRT) is a type of 3D-CRT. We use a machine that changes your position during treatment. We can adjust beam strength while protecting healthy brain tissue.
Whole brain radiation therapy is an option for patients with metastatic brain tumors. It treats tumors throughout the brain, including tumors that are too small to see on scans.
Chemotherapy for brain tumors
Chemotherapy uses medication to destroy cancer cells that we cannot remove surgically. You may get chemotherapy after surgery, possibly along with radiation therapy. Chemotherapy can also slow the growth of brain tumors and help relieve symptoms.
Brain tumors can be hard to treat with chemotherapy because the body’s blood-brain barrier keeps many medications from reaching the brain. We are studying ways to make chemotherapy treatment more effective while causing fewer side effects.
We use chemotherapy for:
- Metastatic cancer, when the cancer has spread to the brain from another part of your body.
- Recurrent cancer, when the cancer returns after treatment.
Other brain tumor medications
The targeted therapy drug bevacizumab (Avastin®) may be an option for glioblastomas that return after treatment. Targeted therapy focuses on specific tumor traits while mostly leaving healthy cells alone. Bevacizumab targets the blood vessels that tumors need to grow.
Clinical trials for brain tumors
You may be eligible to participate in a clinical trial. At the Brain Institute and the Knight Cancer Institute, we have hundreds of clinical trials to test promising new treatment methods. We’ll talk with you early in your care about any trials that might be right for you.
Chemotherapy clinical trials
Blood-brain barrier disruption chemotherapy: BBBD was developed at the Brain Institute to slip chemotherapy past the brain’s natural barrier. Our technique infuses a drug that shrinks the cells lining blood vessels, creating temporary openings for medication to reach the tumor. OHSU and its partners in the study have done more than 7,300 of these procedures in more than 700 patients. We are one of the most active BBBD centers in the world.
Chemotherapy via catheter: We are studying a method to deliver chemotherapy directly to a tumor using a catheter, or thin tube. This method may work better and lead to fewer side effects.
Chemoprotection: Researchers at the Brain Institute are pioneers in the study of chemoprotectants. These medications protect people from some side effects of chemotherapy. We developed a medication that protects hearing after chemotherapy for certain tumors.
Other clinical trials
Our researchers are also studying:
Targeted therapy: The Brain Institute is part of the NCI-MATCH trial to find medications that target specific genetic traits in tumors.
Gene therapy: We can block a specific protein to allow chemotherapy to work better. This means we can use a lower dose.
Immunotherapy: This harnesses the body’s immune system to fight cancer. We are studying:
- Combining immunotherapy with radiation therapy to treat cancer that has spread to the brain from other parts of the body.
- Injecting medication directly into the tumor to activate the immune system, so only the tumor is destroyed.
Additional services
Palliative care: Our expert palliative care specialists can help you and your family manage stress, pain and difficult decisions. This care is available to any OHSU patient with a complex illness. You do not have to end treatment or be terminally ill.
Moving to outpatient care: Our case managers and physician associates can help you manage the transition from inpatient to outpatient care. For example, we’ll help you coordinate with a rehabilitation facility and set up transportation for radiation therapy.
Hospice care: We’ll make sure you are comfortable if therapy is no longer working. We honor your wishes and help your loved ones process emotions and concerns.
Knight Cancer Institute services include:
- Our Adolescent and Young Adult Oncology Program is the only one in Oregon to address the needs of patients diagnosed with cancer from ages 15 to 39.
- Cancer registries offer patients a chance to help advance research.
- Survivorship services, including a program specifically for patients who receive radiation therapy, to help you transition to follow-up care.
Learn more
- Adult Central Nervous System Tumors Treatment, National Cancer Institute
- Stereotactic Radiosurgery (SRS) and Stereotactic Body Radiotherapy (SBRT), RadiologyInfo.org
- Brain Tumor Treatment, RadiologyInfo.org
For patients
- Referral: To become a patient, please ask your doctor for a referral.
- Questions: For questions or follow-up appointments, call 503-494-5626.
Location
Parking is free for patients and their visitors.
OHSU Neuro-Oncology Clinic, Marquam Hill
3270 SW Pavilion Loop, 2nd floor
Portland, OR 97239
Map and directions
Refer a patient
- Refer your patient to OHSU.
- Call 503-494-4567 to seek provider-to-provider advice.