Pediatric Leukemia
OHSU Doernbecher is a national leader in care for pediatric leukemia. We are the only children’s hospital in Oregon to offer CAR T-cell therapy, a groundbreaking treatment for childhood leukemia. Like you, we are committed to caring for your child or teen. Your family will find:
- World-class experts who focus on cancer care for children and teens
- A team-based approach to caring for each unique patient
- Social workers and child life specialists to support your family’s well-being
- Access to clinical trials to test promising treatments
Understanding pediatric leukemia
Pediatric leukemia begins in a child’s bone marrow, where blood cells are made before they enter the bloodstream. It’s important to know:
- Leukemia is the most common cancer in children.
- Doctors can now successfully treat and cure most children with leukemia.
- Scientists don’t know the cause of most childhood leukemias.
- Pediatric leukemia includes many subtypes. Some are more severe than others, and they may require different treatments. Learn more about treatment options for pediatric leukemia.
- CAR T-cell therapy is a breakthrough for some rare cases of childhood leukemia.
What is pediatric leukemia?
Leukemia is a cancer in which a child’s bone marrow makes abnormal blood cells, most often white blood cells.
Normal white blood cells help your child fight infection. Leukemia cells don’t fight infection.
With leukemia, the abnormal white blood cells crowd out other blood cells, including:
- Red blood cells, which carry oxygen through the body.
- Platelets that help blood clot.
This imbalance affects how your child’s organs work. It also keeps red blood cells and platelets from doing their jobs.
What Happens When You have Leukemia
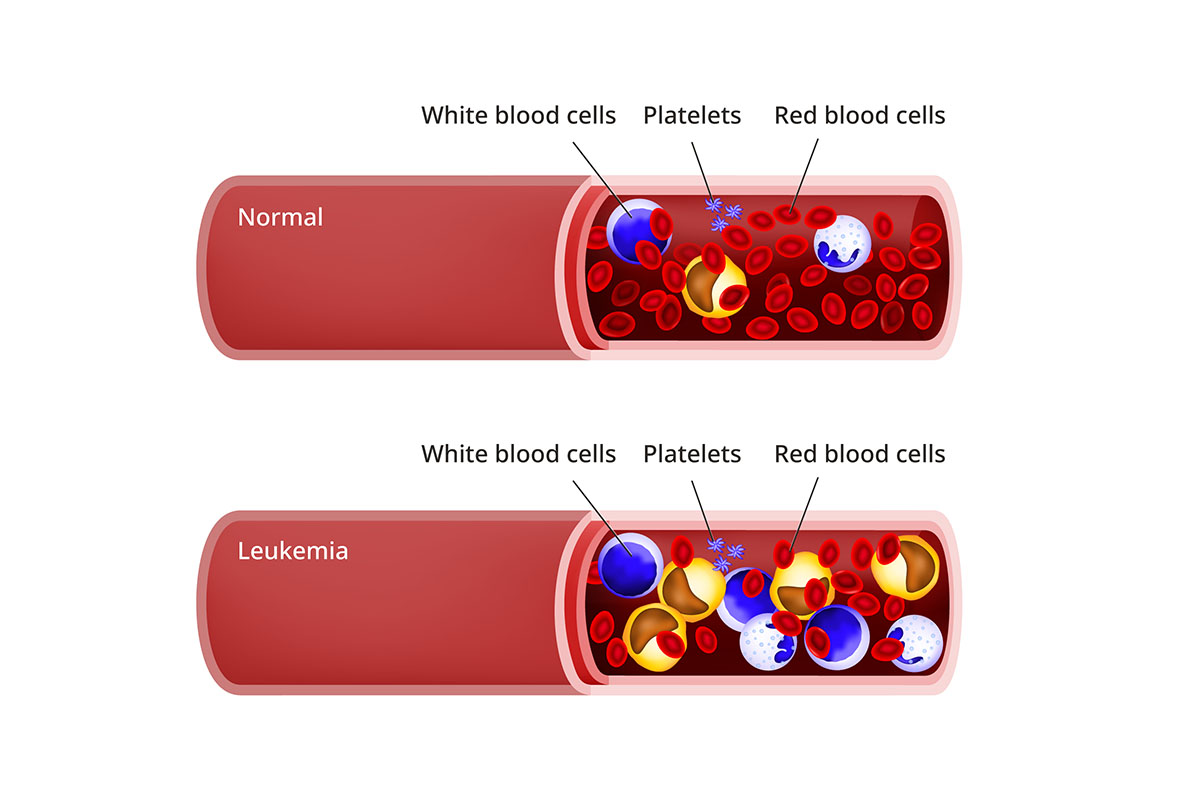
Who gets pediatric leukemia?
While leukemia is somewhat rare in adults, it is the most common form of cancer in children.
- About 28% of all childhood cancers are leukemia.
- About five in 100,000 children in the U.S. will be diagnosed with leukemia this year.
What causes pediatric leukemia?
Scientists don’t know yet. There is nothing anyone could have done to prevent it.
Types of pediatric leukemia
Most childhood leukemia is one of these three types.
-
Acute lymphoblastic leukemia (ALL)
This is by far the most common childhood leukemia, making up about three in four cases. It occurs when your child’s bone marrow produces too much of a type of white blood cell called a lymphoblast. The “acute” in ALL means it usually spreads quickly if not treated.
-
Acute myeloid leukemia (AML)
AML is the second most common childhood leukemia. It occurs in about one in five cases. It starts in myeloid cells, which normally develop into cells that fight infection. Instead, your child’s body makes a large number of abnormal blood cells. Like ALL, it usually spreads quickly if not treated.
-
Chronic myelocytic leukemia (CML)
This type is rare in children. It happens when your child’s bone marrow makes an abnormal number of myeloid cells. Unlike AML, CML tends to spread slowly. Some subtypes can be more challenging to treat. The best treatment for CML was developed by researchers at OHSU’s Knight Cancer Institute and is used worldwide.
Pediatric leukemia survival rates
Leukemia treatment has come a long way over the past 40 years. It’s now successfully treated in most children.
On average, nearly 85% of children with pediatric leukemia survive five years or more after their diagnosis. The five-year survival rate is a standard way of measuring cancer outcomes.
Children with ALL or AML who are cancer-free after five years are likely cured. It is extremely rare for acute leukemias to come back after this long.
- For ALL: Nearly 92% of children who are younger than 15 years old when diagnosed are free of leukemia five years later.
- For AML: Survival rates vary depending on the subtype. About 69% of children younger than 15 are free of leukemia five years later.
- For CML: Nearly 70% of children younger than 15 are free of leukemia five years later.
It’s important to remember that all of these rates are averages. They can’t predict the outcome for your child’s individual circumstances.
Symptoms of pediatric leukemia
Symptoms of leukemia are similar to many other conditions. Your child’s oncologist (cancer doctor) will look at the full picture of your child’s symptoms to diagnose pediatric leukemia.
Low numbers of normal blood cells can cause a variety of symptoms:
- Low red blood cells (anemia)
- Paleness
- Lightheadedness and tiring easily
- Headache
- Low white blood cells
- Repeated, frequent infections
- Low platelets
- Easy bleeding and bruising
If leukemia spreads from the bone marrow to other organs, it can cause:
- Swollen lymph nodes (small glands that help your child’s body filter toxins) or lumps in the underarm, groin, neck or other parts of the body.
- Swollen liver or spleen.
Other symptoms include:
- Pain from pressure in the bone marrow, which can cause irritability and refusal to walk in young children.
- Frequent or long-lasting fevers, as your child’s immune system fights leukemia.
Pediatric leukemia classification
Treatment for childhood leukemia varies based on its type and subtype. ALL and AML are fast spreading (acute). CML is slow spreading (chronic). ALL and AML have subtypes.
-
ALL subtypes
Subtypes of ALL are mainly based on the type of cell where your child’s leukemia starts.
- B-cell ALL starts in B lymphocytes — also called B cells — which protect your child’s body from germs by making antibodies. B-cell ALL has several subtypes.
- T-cell ALL starts in T cells, which normally recognize and destroy cells with viruses.
-
AML subtypes
AML has many subtypes. Your child’s doctor will classify it based on factors such as:
- The type of bone marrow cell where the leukemia started.
- Whether the leukemia cells have specific changes in genes or chromosomes.
- Whether the leukemia is related to chemotherapy or radiation used to treat a previous cancer.
- Whether your child also has Down syndrome.
-
CML phases
Doctors categorize CML based on how many immature white blood cells, or blasts, are found in your child’s blood or bone marrow.
- The chronic phase is an early stage with mild symptoms.
- The accelerated phase has more noticeable symptoms such as fever, night sweats and weight loss.
- The blast phase is more aggressive, as leukemia cells spread to tissues and organs throughout the body.
Learn more about leukemia from the National Cancer Institute.
For families
- Request an appointment.
- Seek a second opinion.
- Ask questions.
Knight Cancer Institute
We offer advanced treatments and expert care as part of the OHSU Knight Cancer Institute.
Locations
Doernbecher Children’s Hospital, tenth floor
700 S.W. Campus Drive
Portland, OR 97239
Find other locations across Oregon and in southwest Washington.
Free parking for patients and visitors
Refer a patient
- Refer your patient to OHSU Doernbecher.
- Call 503-346-0644 to seek provider-to-provider advice.
Cancer clinical trials
Clinical trials allow patients to try a new test or treatment.