Pediatric Cancer Treatment Options

OHSU Doernbecher Children’s Hospital is a national leader in caring for children with cancer, including solid tumors, leukemia, lymphoma and brain tumors. We are on the front edge of research, helping pioneer next-generation therapies.
We seek parents’ input on everything, including treatment plans and side effects. We’ll listen to your concerns, answer your questions and help you prepare for treatment.
We’ll also get to know your child — what grade they’re in, what they like to do — and introduce you to a cancer social worker. Your family’s social worker is part of your care team, offering continual support.
Some important things to know:
- Our team will create a treatment plan tailored to your child. We strive to limit short-term side effects and to avoid long-lasting ones.
- Your child’s oncologist (cancer doctor) will talk with your family and lead overall treatment. They work with an experienced team, including specialists such as surgeons and radiation oncologists.
- Experts on our team meet at least once a week to discuss solid tumor cases. This gathering is called a tumor board. Your child benefits from our providers’ decades of combined experience to shape each treatment plan.
- Doernbecher was the first hospital in the Pacific Northwest to offer CAR T-cell therapy for a type of childhood leukemia. We are the only Oregon hospital to offer this treatment for children.
- Specialists in our Bridges and Child Life programs are an important part of your child’s team. They support your child’s and family’s physical, emotional, social and spiritual needs during treatment and beyond.
Understanding treatment options
Every family’s experience with cancer is different. Our team will meet with you and your child to understand your child’s overall health and to talk about options.
Learn about:
Pre-cancer treatments
Children who might have leukemia or lymphoma may also have other health concerns that need immediate care. These conditions may include severe bleeding, infections and circulatory issues.
We’ll check for:
- A shortage of normal white blood cells, which can lead to serious infections.
- Low levels of the substances that help blood clot normally.
- A lack of red blood cells, which can lower oxygen levels and strain the heart.
If your child has any of these conditions, we will treat them before beginning cancer treatment. We may give your child antibiotics, IV fluids and blood transfusions.
Chemotherapy
Chemotherapy drugs are powerful medications used to treat many childhood cancers by killing cancer cells. Different kinds of chemotherapy medicines are used for different types of cancer. They can be given as a pill, as a shot or through an IV.
Chemotherapy can also be given through a long, thin tube called a catheter that is placed in a large blood vessel in your child’s chest. Your child will be asleep under anesthesia when the catheter is placed.
Our cancer doctors treat only children and young adults. They are experts at knowing the best chemotherapy medications for your child’s specific cancer.
When chemotherapy is used to treat solid tumors, it can:
- Be used alone or with other treatments, like surgery or radiation.
- Stop a tumor’s growth.
- Shrink a tumor before surgery.
- Destroy cancer cells that might remain after surgery.
Chemotherapy is the main treatment for both leukemia and lymphoma.
We will tailor chemotherapy to your child’s leukemia or lymphoma type. For example, acute myeloid leukemia (AML) responds best to higher doses over a shorter period, often less than a year. Acute lymphoblastic leukemia (ALL) is usually treated with lower doses over several years.
Chemotherapy drugs attack fast-growing cancer cells, but they also can damage normal cells. This may cause side effects such as hair loss, nausea, loss of appetite, diarrhea, and increased risk of infection. At Doernbecher, we have deep expertise in reducing and treating these side effects.
Some side effects may take a while to show up. Our team works with experts in fertility, audiology (hearing) and other specialties to lower your child’s risk of long-term issues.
Radiation therapy
Radiation therapy aims high-energy beams, such as X-rays, directly at cancer cells to kill them. Most often these rays are aimed from outside the body (external beam radiation).
Unlike chemotherapy, radiation therapy damages cells only near the area where it is directed. Cells in other parts of the body are not affected.
Radiation might be combined with chemotherapy or used on its own. It is used more often in Hodgkin lymphoma.
Radiation therapy is sometimes used to shrink a tumor so it’s easier to remove during surgery. In other cases, we may use it to shrink or eliminate a tumor without surgery.
Our radiation oncologists (cancer doctors) are experts at treating children. We use the smallest amount of radiation therapy needed to be safe and effective.
Radiation can be difficult for kids because they cannot move during treatment. We use sedation for very young children. Our team is also skilled in helping children stay still.
Radiation treatment can cause fatigue, skin irritation and other side effects. Our team has the expertise needed to help your child reduce or avoid short- and long-term side effects.
Surgery
We often use surgery to remove a tumor. We may recommend having chemotherapy or radiation therapy first to shrink the tumor and make it easier to remove.
Our surgeons and other experts will review all the options to help you choose the one that’s most effective and least invasive.
For example, if your child has bone cancer, our team includes orthopedic surgeons who specialize in making sure their arm or leg still works well after removing the tumor.
Surgery is rarely used in leukemia or lymphoma treatment except for placing a port for chemotherapy. But your child’s doctor may use surgery for lymph node biopsies.
Surgery is sometimes used for an early stage of a non-Hodgkin lymphoma called Burkitt lymphoma. In this case, your child’s surgeon might remove a tumor before chemotherapy begins.
Your child’s surgeon might also take a biopsy or place a small device called a port in your child’s chest. It’s connected to a large blood vessel and lets us give medications or do blood work without needing a needle or IV at each visit.
Bone marrow/stem cell transplant
Your child’s doctor might recommend a bone marrow/stem cell transplant. In this therapy, stem cells are given to your child in an IV. The cells collect in bone marrow, where they begin making healthy blood cells.
Doernbecher’s pediatric bone marrow transplant program is ranked among the nation’s best. Learn more about bone marrow/stem cell transplants.
Targeted therapies
Our providers at Doernbecher and the Knight Cancer Institute are pioneers in targeted therapies.
Targeted therapies are medications designed to attach to and block a specific type of leukemia or lymphoma cell or solid tumor without attaching to normal cells. These medications don’t kill healthy cells like chemotherapy does, so there are fewer side effects.
For example, we treat the childhood cancer neuroblastoma with targeted therapy. Neuroblastomas begin in certain nerve cells, often near the spine or in the adrenal gland.
Neuroblastoma Locations
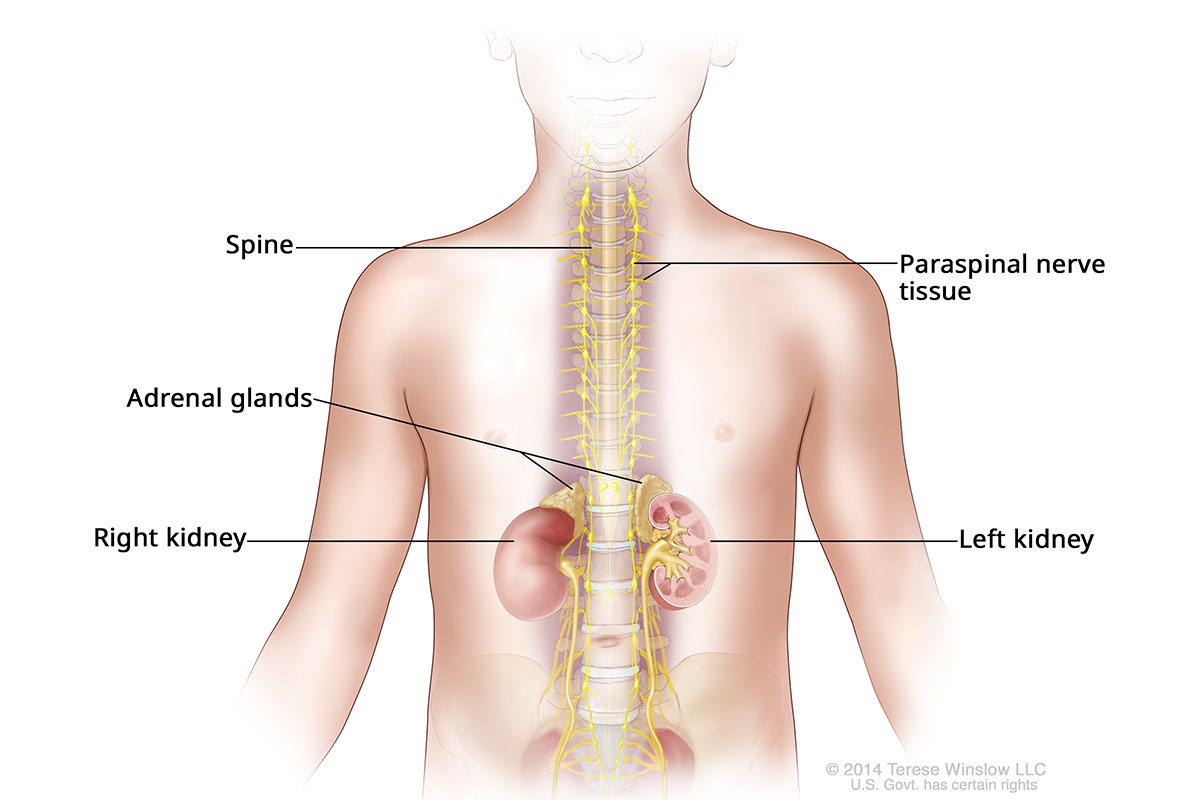
Immunotherapy or Cell therapy
Immunotherapy treatments help your child’s immune system recognize and kill cancer cells.
Some types may treat neuroblastomas. A type called CAR T-cell therapy offers a powerful new option for a hard-to-treat leukemia. Doernbecher is the only hospital in Oregon able to provide this complex therapy for children.
For families
- Request an appointment.
- Seek a second opinion.
- Ask questions.
Knight Cancer Institute
We offer advanced treatments and expert care as part of the OHSU Knight Cancer Institute.
Locations
Doernbecher Children’s Hospital, tenth floor
700 S.W. Campus Drive
Portland, OR 97239
Find other locations across Oregon and in southwest Washington.
Free parking for patients and visitors
Refer a patient
- Refer your patient to OHSU Doernbecher.
- Call 503-346-0644 to seek provider-to-provider advice.
Cancer clinical trials
Clinical trials allow patients to try a new test or treatment.