Pediatric Heart Catheterization Program
The heart catheterization program at OHSU Doernbecher Children’s Hospital enables us to diagnose and treat complex heart problems without surgery.
You’ll find:
- Highly trained specialists who do hundreds of catheter procedures a year.
- Anesthesiologists who specialize in caring for children with heart disease and who will make sure your child is safe.
- Minimally invasive techniques for less pain and a quicker recovery compared with surgery.
- The lightest possible sedation for each child, avoiding breathing tubes in many cases.
- Access to clinical trials and the latest research advances.
Understanding cardiac (heart) catheterization
What is heart catheterization?
Heart catheterization uses thin, flexible tubes called catheters to diagnose and repair heart conditions. Catheters provide a path for your child’s doctor to see, test and sometimes treat the heart’s structures, pumping, rhythm, blood flow and blood pressure.
Why catheterization is done
Cardiac catheterization is done to diagnose a heart condition before surgery, or as a treatment in the heart or blood vessels to avoid or delay heart surgery. Catheter procedures are shorter and less painful than heart surgery, and with a faster recovery.
Heart Catheterization in Infants
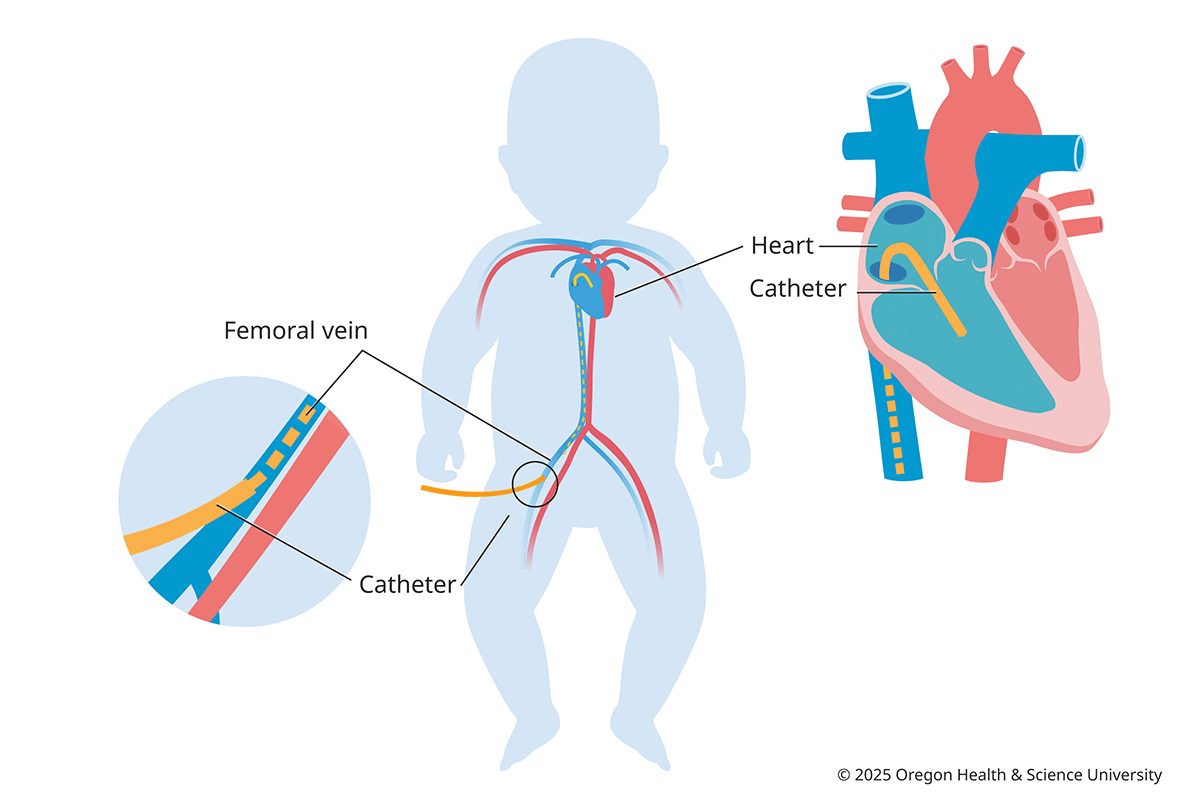
How catheterization is done
Children are sedated for the procedure. An anesthesiologist with special training in children’s heart disease will make sure your child’s breathing, pulse and blood pressure are as they should be.
The catheterization specialist (also called an interventional cardiologist) enters a vein or artery, usually in the groin, with a needle. The doctor then guides the catheter through blood vessels to your child’s heart. Once the catheter is inside, the doctor uses moving X-rays (fluoroscopy) to take pictures, and measures pressure and oxygen levels in the heart.
Next, the doctor may perform a procedure such as:
- Closing an atrial septal defect
- Closing a patent ductus arteriosus
- Placing a new pulmonary valve
- Placing a stent to expand a blood vessel that’s too small
- Using a balloon to expand a narrowed aortic valve
Heart Catheterization in Children
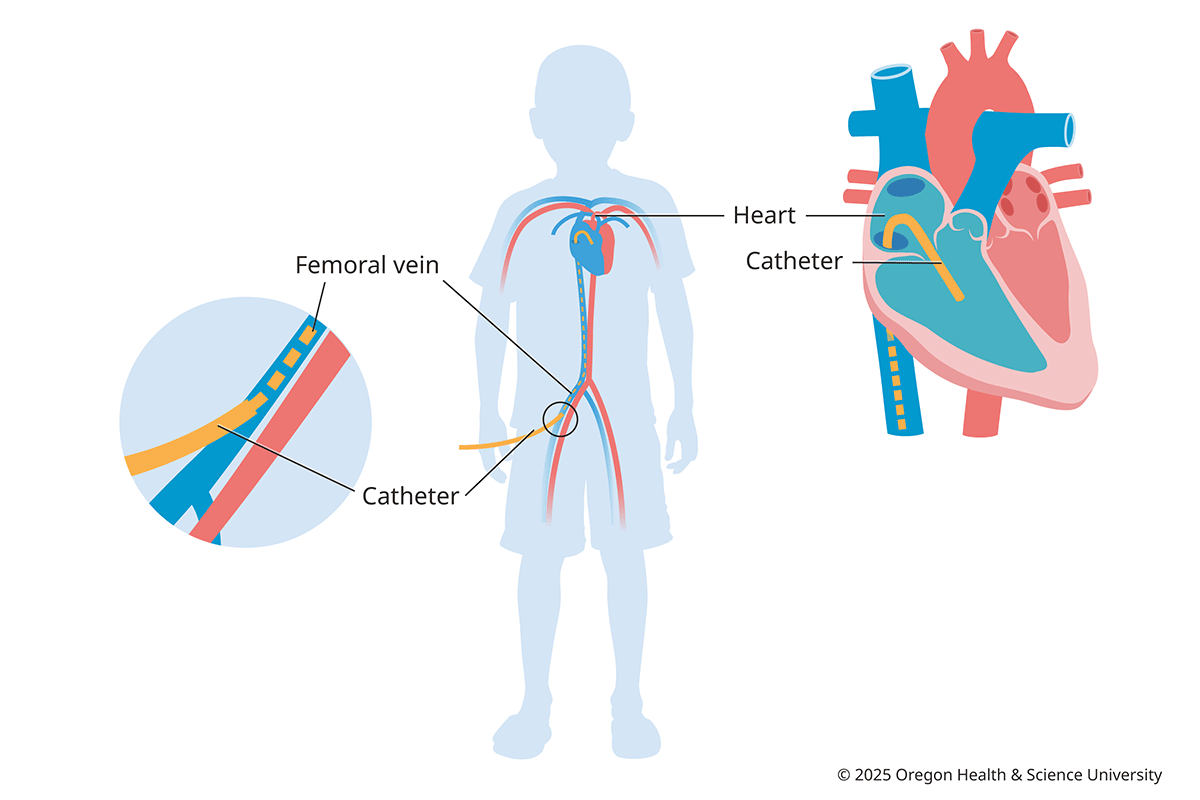
What makes our program different
Experienced providers
Doernbecher is the only children’s hospital between Seattle and San Francisco with two children’s heart specialists who have advanced training and expertise in catheter procedures. That means one is available at all times.
Interventional cardiologists Grant Burch and Laurie Armsby have more than 40 years of combined experience. They do more than 300 catheterization procedures a year on newborns, children and adults with congenital heart disease. This gives our doctors unmatched experience in the region.
They often work together, sharing expertise to give your child the best care possible. Jennifer Mustard, a physician associate, works closely with both doctors and with families before, during and after procedures.
Doernbecher specialists
Your child will also benefit from the combined expertise of specialists throughout Doernbecher. They have the resources of a top children’s hospital behind them, including:
- Fetal heart care to plan catheterization treatment as soon as your baby is born.
- Coordinated care with OHSU’s adult congenital heart disease program as your child grows older. It is the only program of its kind in Oregon.
- Anesthesiologists, imaging specialists (radiologists), nurses and technicians who focus on children’s heart procedures.

“We’re going to take care of their child for the rest of their life.”
What to expect
Before the procedure: You will have a chance to talk with the cardiologist. The doctor will describe the procedure in detail, explain how it can help, and go over any potential risks.
When you arrive: The doctor will talk with you again to answer questions and make sure you understand what will happen.
Minimal sedation: Our anesthesia team will help your child go to sleep before the procedure. We use the lightest possible sedation and avoid using breathing tubes for most children older than 2.
During the procedure: Your child will be taken to the catheterization lab. The lab team usually includes the doctor, an anesthesiologist, technicians and two nurses. Specialists will constantly monitor your child’s heart rate, blood pressure, heart rhythm, oxygen levels and breathing. Most procedures take about two to four hours.
Recovery: Your child will be brought to a recovery room for observation. Most children go home the same day or spend a night in the hospital. Sometimes children need to stay longer or, rarely, go to the Pediatric Intensive Care Unit.
Follow-up care: Your child’s catheterization team will come to the recovery area to talk with you as soon as possible after the procedure. The doctor will show you pictures of what they found. They will explain what they did and what it means for your child’s care.
the heart in better shape as the child gets older,” Dr. Burch says.
Catheterization treatments
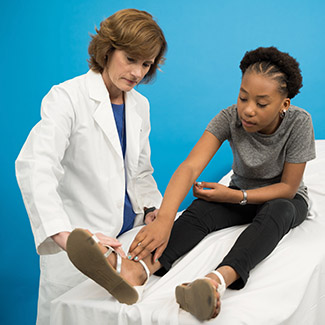
Advances in cardiac catheterization are helping more children delay or avoid heart surgery.
Treatments (also called interventions) include:
Atrial septal defect closure: We use catheters instead of surgery to plug most ASDs (holes between the heart’s two upper chambers). Dr. Burch was the first to offer this option in Oregon. Most children can go home after one day and return to regular activities after a few days.
Patent ductus arteriosus closure: Normally, the ductus arteriosus, a blood vessel in a developing heart, closes on its own after birth. If it stays open (patent), too much blood flows to the lungs, potentially causing heart failure and poor growth. We can close these blood vessels in even the youngest babies.
Ventricular septal defect closure: If your child is born with a hole between the two lower chambers of the heart, we may be able to close it with catheterization instead of surgery.
Balloons: We insert catheters with tiny balloons at their tips. The balloons are inflated to open a valve (valvuloplasty) or enlarge blood vessels (arterioplasty, venoplasty).
Pulmonary valve replacement: We were the first children’s hospital in Oregon to use catheters instead of surgery to replace pulmonary valves. The latest replacement valves are safer and longer-lasting than some other options. These advanced valves can improve heart function and reduce the need for surgery.
Stents: These thin mesh tubes enlarge and hold open narrowed blood vessels or keep open needed connections between heart chambers. They may be used, for example, for a patient with a narrowed (coarctation) of the aorta.
Clinical trials
Our catheterization team takes part in national studies of new technology and techniques. We will talk with you about any clinical trials that might be right for your child.
For families
Call 503-346-0640 to:
- Request an appointment.
- Seek a second opinion.
- Ask questions.
Locations
Parking is free for patients and their visitors.
Doernbecher Children’s Hospital
700 S.W. Campus Drive
Portland, OR 97239
Map and directions
Find other locations across Oregon and in southwest Washington.
Refer a patient
- Refer your patient to OHSU Doernbecher.
- Call 503-346-0644 to seek provider-to-provider advice.