Pediatric Heart Care: Diagnostic Tests

OHSU Doernbecher Children’s Hospital offers Oregon’s most complete and accurate evaluation of children’s heart conditions.
Our offerings include:
- Imaging and testing rooms designed for your child’s comfort and safety.
- Same-day availability for many tests, including echocardiography and ECG.
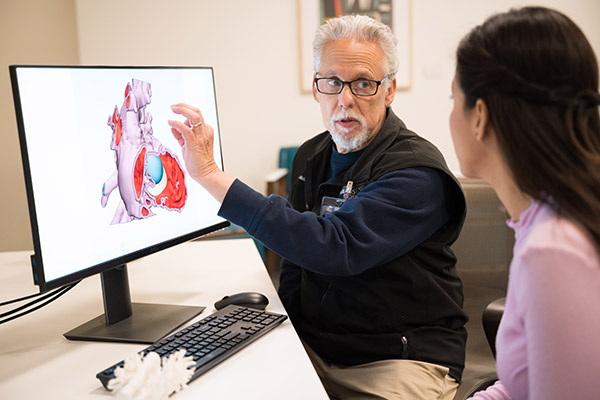
- High-definition 3D images of moving hearts.
- 3D printed heart models for complex conditions.
- Advanced 3D technology for mapping heart rhythm problems (arrhythmias).
- Oregon and southwest Washington’s first and largest accredited pediatric echocardiography lab.
- Genetic testing with certified counselors to help families weigh options and understand results.
- A full range of portable heart rhythm monitors, including the state’s only implantable option.
- The state’s largest and most experienced heart care team, with specialists working together to assess even the most rare or complex heart disorders.
What to expect
Heart problems in children can be difficult to diagnose. Our goal is to find and treat them as quickly and accurately as possible so your child can resume an active life.
At Doernbecher, your child’s care team will guide you through testing options and help you understand results. If needed, we’ll work with you to create a care plan tailored to your child’s needs.
We will:
- Schedule all your child’s tests and doctor visits on the same day whenever we can.
- Talk with you about the results as soon as they are available, often right after the test.
- Follow up with you on test results, either in person or on the phone.
- Do our best to put your child at ease with child-friendly labs and imaging rooms.
- Consult with your child’s pediatrician about the test results and care options in your community.
What makes our program different
Pediatricians across Oregon turn to our heart team to discuss cases, and to read and interpret test results. Each year, we perform more than 10,000 tests to detect fetal and pediatric heart conditions.
We are the only children’s hospital in the state with:
- An echocardiography laboratory certified in pediatric transthoracic, fetal and transesophageal imaging.
- 3D mapping to find and treat heart rhythm problems quickly, safely and accurately.
- 3D models — virtual and printed — to see heart structures and plan complex treatments.
- Imaging and catheterization labs that specialize in children’s heart conditions.
- Small wearable and implantable monitors for long-term, wireless recording of the heart’s electrical activity.
- Specialists trained in cardiovascular MRI, CT and other advanced imaging techniques.

Our tests
-
Echocardiogram (echo)
An echocardiogram is an ultrasound of the heart. This test uses sound waves to create moving images of the heart. It shows the heart’s structures and blood flow as the heart pumps. It’s the tool we use first and most often to find and monitor children’s heart conditions.
Our pediatric echocardiography lab was the first in the region accredited by the Intersocietal Accreditation Commission, meaning we meet the highest standards. We are also the only hospital in Oregon with an echocardiography lab certified to do all three types of prenatal and children’s echocardiograms:
- Transthoracic
- Transesophageal
- Fetal
Our heart doctors and ultrasound technicians all have specific training and many years of experience doing these scans, so they can get the best images.
How it’s done: The test is usually done in one of five scanning rooms in our children’s echo lab. It is safe, painless and takes about 30 minutes. Your child can watch a video during the test, and you can stay in the room. No radiation is used. We sometimes recommend sedation for a complete echocardiogram.
An imaging specialist rubs warm gel on your child’s chest. The specialist lightly presses a wand (transducer) against your child’s chest. Sound waves bounce off of blood vessels, valves, muscles and tissue and back to the transducer to create a moving image on a screen.
Types:
- Transthoracic: This is the most common type of echocardiogram. It’s done on the outside of the chest.
- Fetal: We scan through mom’s belly to look at a developing baby’s heart.
- Transesophageal: This type is usually done during surgery or catheterization. We insert the transducer into the food pipe (esophagus) to see the heart from behind.
- 3D echo: This advanced technique combines multiple images into a 3D image your doctor can turn and examine. It shows the heart in greater detail. Transthoracic, fetal and transesophageal echocardiograms can all be done in 3D.
Why it’s done: An echo can find — or rule out — a range of heart conditions, including:
- Conditions that can cause murmurs
- Valve problems
- Holes in the heart
- Pulmonary hypertension
- Abnormal heart connections
- Any other structural, pumping or blood-flow issue
-
Electrocardiogram (ECG or EKG)
This test measures and records the heart’s electrical activity. It is a quick, painless and safe way to check for rhythm problems and signs of other heart conditions. We also use electrocardiograms to monitor heart conditions through childhood.
How it’s done: Small adhesive patches with electrical sensors (electrodes) are placed on the child’s chest, arms and legs. The sensors are connected to a machine that records the heart’s rhythm as a series of lines, waves and spikes. The child is asked to lie still for a few minutes during the test.
Why it’s done: It’s often the first step in diagnosing a heart condition. More tests may be needed to confirm a diagnosis. ECG can help find:
- Fast, slow or irregular rhythms (arrhythmias)
- Heart thickening or enlargement
- Structural defects in the heart
- Blood flow and valve problems
-
Exercise stress testing

This test measures how well your child’s heart and lungs adjust to exercise.
How it’s done: The child uses a stationary bike or treadmill while attached to heart and lung monitors. The child wears an arm cuff, adhesive electrodes (electrical sensors) on the chest, and a mouthpiece to measure blood pressure, heart rhythm, oxygen intake and carbon dioxide output.
As the child exercises for about 10 to 12 minutes, the resistance or speed slowly increases until the child is working as hard as possible. A doctor supervises the test to make sure it’s safe.
Why it’s done: Exercise testing can help determine:
- If your child’s heart has trouble coping with exercise.
- A safe level of physical activity for your child.
- The effects of a treatment or surgery.
- If it’s safe to start heart rehabilitation.
-
Cardiac MRI (magnetic resonance imaging)
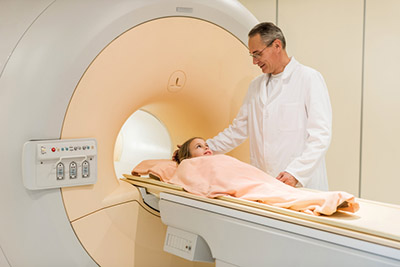
This test uses radio waves and a strong magnet to show detailed images of your child’s moving heart. MRI allows us to measure blood flow and to see if the heart muscle is healthy. Our imaging specialists have extra training for doing this test and interpreting the results.
How it’s done: MRI is done in a large, tube-shaped machine. The test takes about one or two hours. Young children are often sedated. Our doctors have also pioneered a method to scan infants without sedation.
Why it’s done: An MRI can:
- Provide a better view than an echocardiogram of some cardiovascular structures, such as the aorta.
- Allow us to see the details of complex heart conditions.
- Show the heart in motion, including how blood flows through veins and valves.
- Reveal any inflammation, scarring or stiffness in the muscle and tissues that might affect future heart function.
-
CT (computed tomography) scan
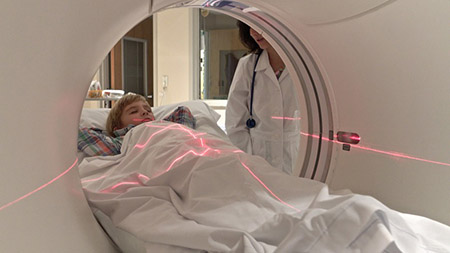
A CT scan is a quick way to see the small structures and blood vessels in your child’s heart. It makes high-resolution pictures using X-rays and a computer.
How it’s done: Your child will lie on a table as the scanner rotates around your child’s chest, taking images. The test takes about 30 seconds. Young children (up to about age 6) are sedated. Our imaging experts have reduced radiation levels to as low as possible. They also track the amount each child receives.
Why it’s done: This test enables us to take detailed measurements of small structures in your child’s heart. It can help your child’s care team better understand a complicated heart condition.
-
3D-printed heart models

If your child has a complicated heart defect, we can make a 3D model of the heart to better understand the problem and guide care. We are the only children’s hospital in Oregon with this technology.
How it’s done: We use computer software to combine MRIs, echocardiograms and CT scans to create a detailed 3D image. We use a 3D printer to make a life-size plastic model showing all the major arteries, valves and structures.
Why it’s done: A 3D model can help doctors and surgeons plan solutions that are tailored to your child. Your child’s care team can study the heart’s structures before a surgical or catheter procedure, improving results. The team will also show you the model to help you understand your child’s condition.
-
Diagnostic heart catheterization
This minimally invasive technique allows heart specialists to reach your child’s heart by using a long, thin, flexible tube (catheter). They can use the tube to see, test and monitor your child’s heart and lungs without surgery.
How it’s done: The doctor inserts the catheter in a vein or artery, usually in the groin, and guides it to your child’s heart. Once it’s in place, a small amount of dye is injected and tracked using X-ray imaging as the dye passes through blood vessels. Most children are sedated and breathe on their own during the procedure. We can often treat the problem during the same procedure.
Why it’s done: Catheterization can give us detailed information about complex heart conditions, including:
- Abnormal rhythms
- Structural defects
- High blood pressure in the lung arteries or the aorta
Heart Catheterization in Children
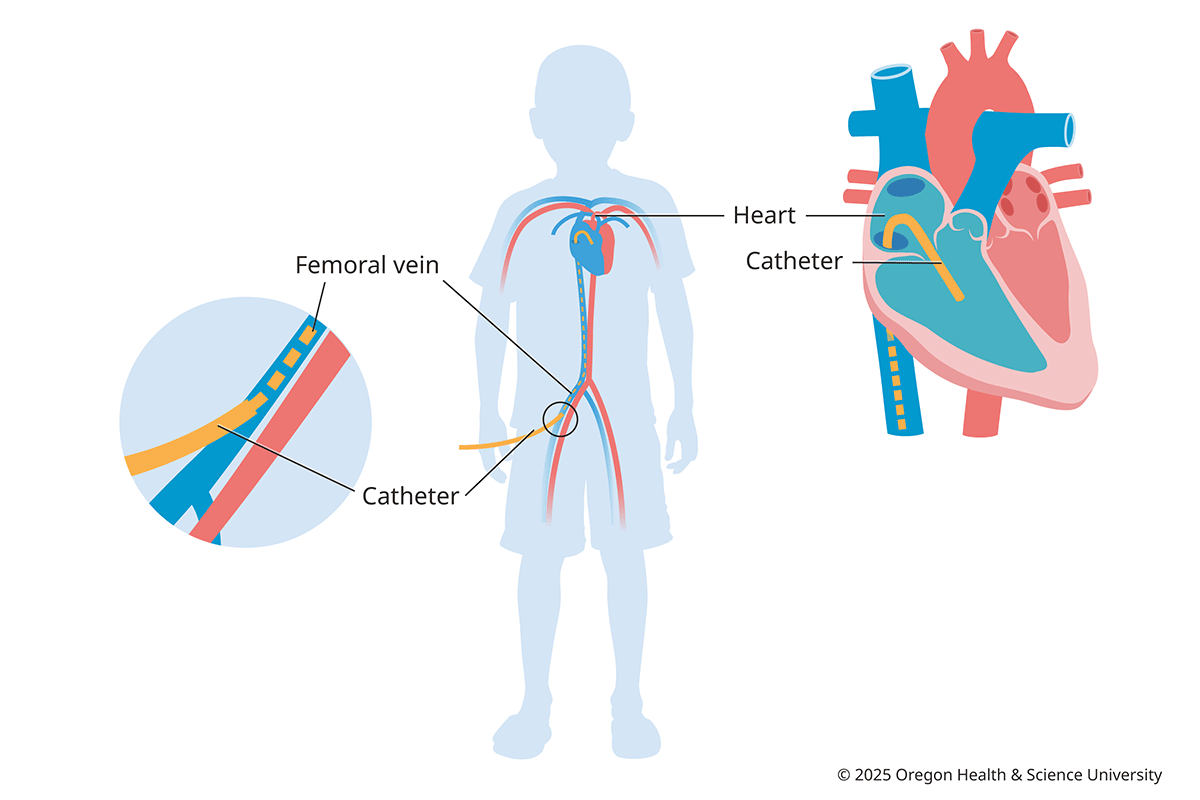
Heart catheterization allows your child's doctor to take pictures and measure pressure and oxygen levels in your child's heart. We use the lightest possible sedation and avoid using breathing tubes for most children older than 2.
Learn more about pediatric heart catheterization.
-
Electrophysiology study (EPS)
This test precisely maps the heart’s electrical activity (electroanatomic mapping). It uses catheterization (see section above).
How it’s done: Children are sedated and asleep during this test but usually breathing on their own. A doctor inserts one or more thin flexible tubes (catheters) into blood vessels leading to the heart. The catheters deliver electric pulses to gently stimulate the heart and gather data. The data lets us precisely trace the heart’s electrical activity and pinpoint where it’s not working properly.
Why it’s done: If your child has an abnormal heart rhythm (arrhythmia), an electrophysiology study can help us find the exact location of the disorder. We can often repair the problem during the same procedure.
Learn more on our Electrophysiology and Heart Rhythm Program page.
-
Portable monitor
A portable heart monitor can record your child’s heartbeats during regular activities at home and school. It provides the same information as an electrocardiogram, but over a longer time.
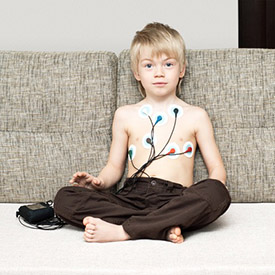
A boy wears a Holter monitor. How it’s done: We use several types of monitors, including:
- Holter: We attach adhesive electrodes to the child’s chest. They connect to a small monitor that can be worn around the neck for one or two days.
- Patch monitor: A small adhesive chest patch records electrical activity for up to two weeks.
- Cardiac event recorder: This device, similar to a Holter monitor, is used for a month or more. You can turn it on when your child has symptoms.
- Small implantable monitor: If we suspect that your child might have a serious issue not found by an external monitor, we can implant a tiny monitor under the skin. These devices can wirelessly record your child’s heart rate for up to three years. We are the first and only hospital in Oregon to offer these monitors.
Why it’s done: A portable monitor allows your child’s care team to measure the heart’s electrical activity for 24 hours or longer. It can help us diagnose complex heart rhythm problems, heart disease and congenital heart defects.
-
Genetic testing
Some heart defects are linked to genetic conditions. Genetic tests can identify the changes in your child’s DNA that caused the heart condition, and this can help guide treatment.
How tests are done: Genetic tests can be done before or after birth. An experienced and certified genetic counselor will talk with you about your family’s history, testing options, and what results mean.
- Babies and children: We take a saliva or blood sample and send it to a lab.
- Before birth: Our prenatal screening and diagnostic tests include ultrasounds, maternal blood tests, chorionic villus sampling and amniocentesis.
Why it’s done: Genetic testing can help you and us understand your family’s risks so you can make care decisions for your child. If your child has a genetic condition, other relatives may benefit from testing and treatment.
For families
Call 503-346-0640 to:
- Request an appointment.
- Seek a second opinion.
- Ask questions.
Locations
Parking is free for patients and their visitors.
Doernbecher Children’s Hospital
700 S.W. Campus Drive
Portland, OR 97239
Map and directions
Find other locations across Oregon and in southwest Washington.
Refer a patient
- Refer your patient to OHSU Doernbecher.
- Call 503-346-0644 to seek provider-to-provider advice.
Tiny heart monitors

OHSU was the first hospital in Oregon to implant tiny wireless heart monitors that are smaller than a AAA battery.