Understanding Headaches and Migraines

Understanding headaches can be your first step toward easing your pain. The OHSU Headache Center is your resource for information and care.
Important things to know:
- Headaches affect nearly everyone at some point.
- Only a small portion of headaches are caused by a serious underlying medical issue.
- Headaches come in many types.
- Symptoms vary widely from patient to patient.
- Women, especially in childbearing years, are at higher risk.
- Headaches are a major public health issue and a leading reason for emergency room visits.
- Many treatments are available.
What are headaches?
The brain itself doesn’t feel pain. Though the brain has billions of neurons (cells that transmit sensory and other information), it has no pain receptors. The ache from a headache comes from other nerves — inside blood vessels in your head, for example — telling your brain something is wrong.
Who gets headaches?
Headaches are a major public health problem. They are one of the most common sources of pain and suffering. They are also a leading cause of disability, emergency-room visits, and work and school absences.
Globally, according to the World Health Organization:
- Nearly all people have a headache at some time in their lives.
- About half of adults have a headache at least once a year.
- Up to one in 20 adults have a headache every day or nearly every day.
- Migraines affect at least one in seven adults.
- Migraines affect about three times as many women as men.
In the U.S.:
- Headaches are among the top five reasons Americans go to an emergency room, according to a 2018 analysis of federal data*. For women under 64, it’s the third-leading cause.
- One in six adults (one in five women) reported a migraine or severe headache in the prior three months, according to 2017 national health statistics.
- Among those ages 18 to 64, one-third had a migraine or severe headache in the prior three months.
Headache categories
Headaches are categorized as either:
- Primary: The headache is the sole medical problem. This type makes up more than 90% of headaches.
- Secondary: The headache is a symptom of another medical issue, anything from a sinus infection to a stroke or tumor.
Headache types
The International Headache Society’s classification system lists more than 200 types and subtypes of headache, but about 90% are tension, migraine or cluster.
Tension
Tension headaches, the most common type, deliver a dull ache to both sides of the head. These headaches are usually treated with over-the-counter medication that contains ibuprofen (such as in Advil) or acetaminophen (Tylenol).
Tension headache symptoms
- Mild to moderate, non-throbbing pain on both sides of the head
- Tightening or pressing pain, like a band around the head
- Pain that lasts at least a half-hour
- Aching may affect the neck or back of the head
- Not worsened by physical activity
- May include a sensitivity to light or sound
Tension Headache Signs and Symptoms
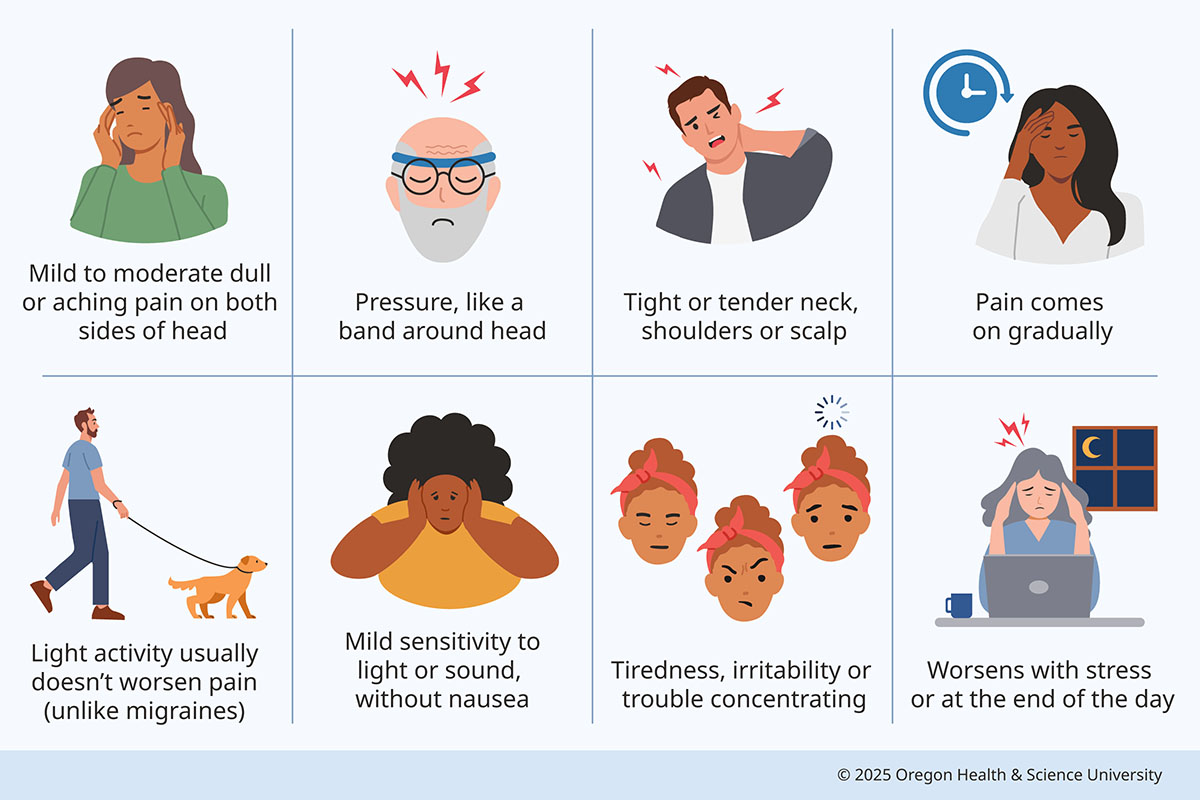
Migraine
Migraines affect an estimated 38 million Americans. Women, most often in their 30s, are three times more likely to get migraines. Migraines can be hereditary (passed down from a parent).
Migraine and depression: People who get migraines are about four times more likely to have depression and anxiety. It’s a two-way street, with each increasing the risk for the other.
Migraine with aura: Roughly one-quarter of people with migraines have aura symptoms — sensory changes that signal a migraine is coming. Symptoms may include seeing flashes of light, having a tingling sensation or having trouble speaking.
Dr. Juliette Preston discusses the myths and truths about women and migraines.
Migraine symptoms
- Moderate to severe pulsating pain around one eye or on one side of the head
- Pain that lasts four hours to three days
- Sensitivity to light and/or sound
- Nausea and/or vomiting
- Worsened by physical activities
- Decreased ability to function in everyday situations
- Aura symptoms
- Depression, drowsiness, food cravings or irritability one or two days before the attack (called the prodrome phase)
Migraine Signs and Symptoms

Cluster
This type can be extremely painful, with stabbing pain near one eye or on one side of the head. Attacks usually occur in groups (clusters), with as many as eight in one day. Pain-free periods can last weeks, months or years. Cluster headaches are four times more common in men.
Cluster headache symptoms
- Severe stabbing or throbbing pain around one eye or on one side of the head
- Pain that strikes in the evening and that typically lasts 15 minutes to three hours
- Swollen, inflamed or drooping eyelid
- Runny or congested nose
- Sweating on the forehead or face
- Shrinking of one pupil
- Inability to stay still, agitation
Cluster Headache Signs and Symptoms
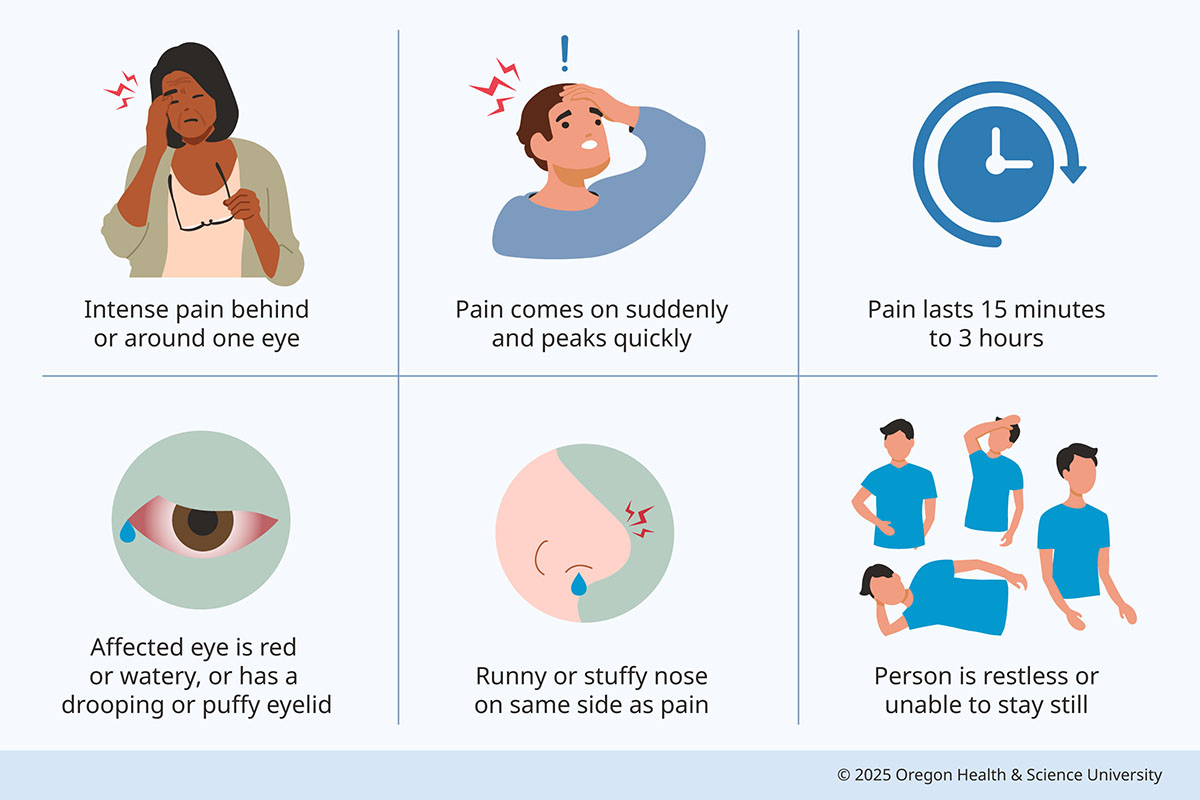
Other types
-
Sinus
A sinus infection can cause a headache, but most often, patients actually have a migraine. True sinus headaches come with pain on one side and improve as the infection is treated.
-
Cervicogenic headache
This is a secondary headache caused by a source of pain in the neck. Causes include tumors, bone breaks, infection or rheumatoid arthritis in the upper (cervical) spine.
-
Hormone-related
Though not a type defined by the International Headache Society, the doctors at the OHSU Headache Center Clinic pay attention to the influence of hormones. Women’s fluctuating hormones are why they are much more likely to get migraines. It’s also why many women with migraines see relief after menopause.
-
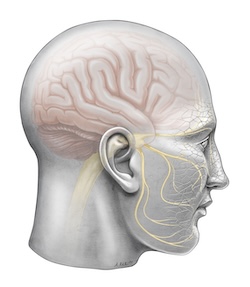
The trigeminal nerve branches across each side of the face. (Illustration by Andy Rekito/OHSU) Facial pain
These headaches may trace back to a problem with your jaw. Disorders of the temporomandibular joint (jaw), for example, or with facial nerves can cause pain perceived as a headache. At OHSU, our headache experts work with dental and facial pain specialists to identify and treat your pain.
-
Trigeminal autonomic cephalgia
This group of headaches is marked by pain on one side of the face in the area of the trigeminal nerve. This nerve pair splits into three branches on each side of the face and is linked to intense pain. Subtypes in this headache group include:
- Paroxysmal hemicrania
- Hemicrania continua
- SUNCT and SUNA
At OHSU, we work with the OHSU Facial Pain Program to make sure patients see the specialists best able to treat their pain.
-
Atypical facial pain
This pain doesn’t follow the trigeminal nerve. (See “trigeminal autonomic cephalgia” above). It’s also not a type of facial pain called trigeminal neuralgia, usually caused by a blood vessel pressing on the trigeminal nerve. In atypical facial pain, pain may be on both sides of the face.
Headache causes
Headaches can have many causes, including injury or an underlying illness. But the vast majority are primary headaches, meaning the headache is the only medical issue. For these, the most common causes include:
- Medication overuse (taking more than 10 doses of headache medication a month has been found to cause headaches)
- Drinking alcohol
- Skipping meals
- Eating certain foods
- Dehydration
- Stress and anxiety
- Lack of sleep
Headache triggers: Some causes are referred to as triggers. Some patients track their triggers so they can avoid them and ward off headaches.
Find more information, including answers to frequent questions, on our Headache FAQ and Resources page.
For patients
- Referral: To become a patient, please ask your doctor for a referral.
- Questions: For questions or follow-up appointments, call 503-494-7772.
- Virtual visits: Online follow-up appointments are available through MyChart.
- Find forms for new patients.
- See our FAQ and resources for patients.
Location
Parking is free for patients and their visitors.
OHSU Headache Center
Center for Health & Healing Building 1, eighth floor
3303 S. Bond Ave.
Portland, OR 97239
Map and directions
Refer a patient
- Refer your patient to OHSU.
- Call 503-494-4567 to seek provider-to-provider advice.
- See our headache information for providers.