ALS (Amyotrophic Lateral Sclerosis)

Your team of specialists at the ALS and Neuromuscular Disease Center will give you expert care at every stage of ALS. We offer you:
- A full team of doctors, therapists and other specialists in one place.
- Compassionate care tailored to your needs and quality of life.
- Regular consultation with ALS Association experts, where you meet with a team to discuss your symptoms and treatment.
- World-class research, with a commitment to help patients as quickly as possible.
Understanding ALS
ALS (amyotrophic lateral sclerosis) is also known as Lou Gehrig’s disease after the New York Yankees player who was diagnosed with it in 1939.
It is a group of conditions that affect muscle-controlling nerves in the brain and spinal cord. ALS has no cure, but treatments can ease symptoms and improve quality of life.
What is ALS?
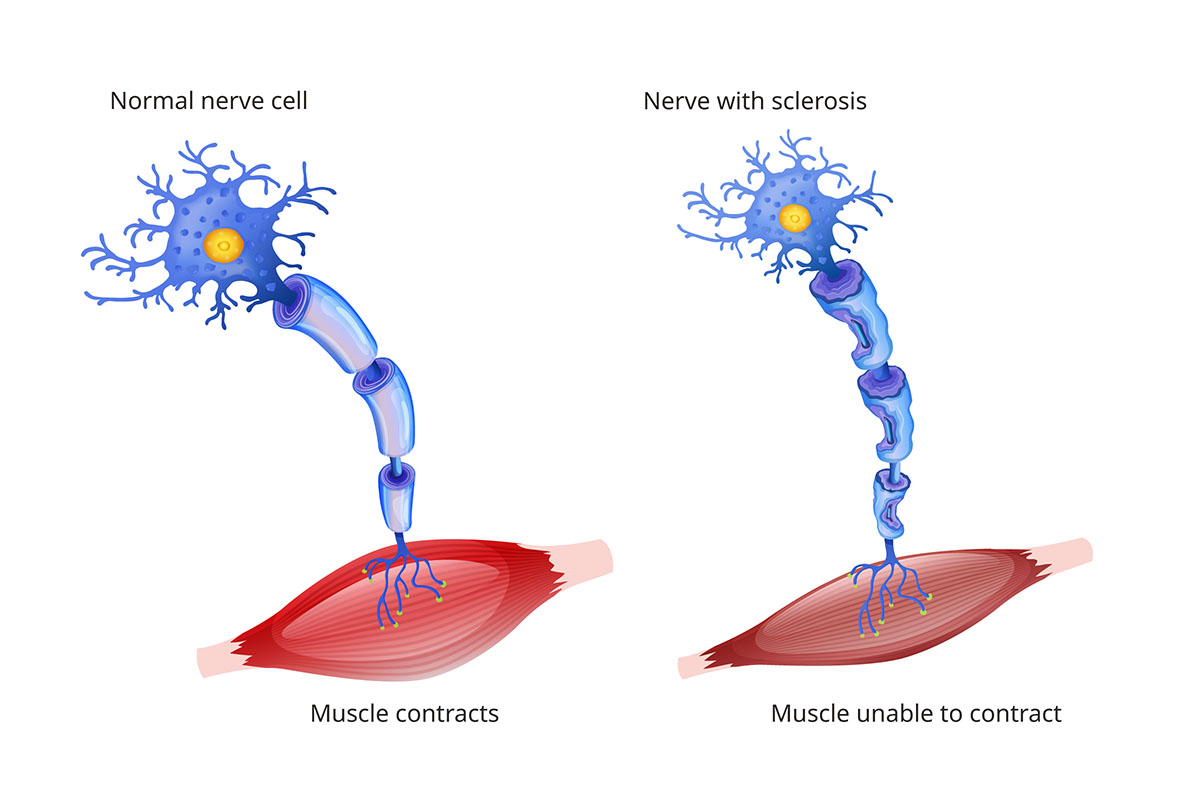
ALS affects nerve cells called motor neurons. These neurons carry messages from the brain and spinal cord to muscles that control voluntary movements. With ALS, the motor neurons gradually wither and die. ALS is a progressive disease, meaning it worsens over time. People with ALS lose the ability to speak, eat, walk and breathe on their own.
How slowly or quickly ALS progresses varies by patient. With the right care, many people living with ALS consider their quality of life to be high. At OHSU, we are committed to helping you manage your symptoms so you can stay mobile and independent as long as possible.
Amyotrophic Lateral Sclerosis
Who gets ALS?
About 16,000 Americans are living with ALS, according to estimates from the Centers for Disease Control and Prevention. It can affect anyone, though some people are at higher risk.
Risk factors include:
- Family history: About 5-10% of cases are passed down in families that have certain genetic mutations. Genes appear to play a role in some other cases as well.
- Age: People 40 to 70 years old are more often diagnosed with ALS.
- Gender: ALS is more common in middle-aged men than in middle-aged women. In later years, the disease is equally common in men and women.
- Race and ethnicity: ALS is more common in people who are white and non-Hispanic.
- Military service: Veterans are at higher risk of developing ALS, though scientists don’t know why.
What causes ALS?
Scientists don’t know exactly what causes ALS, but research is ongoing. OHSU is part of a national project to identify biomarkers, or indicators of ALS, in samples of blood and other bodily fluids. Biomarkers could be used to:
- Diagnose the condition sooner
- Monitor the progress of ALS
- Create new treatments
- Test new medicines in clinical trials
Types of ALS
The two main types are:
- Sporadic: This type can affect anyone. It accounts for 90-95% of U.S. cases.
- Familial: This type is inherited through genetic changes passed down in families. If a parent has familial ALS, each child has a 50% chance of developing it, too. If you have this type of ALS, your care team may suggest genetic counseling.
ALS is also described by how it starts:
- Rapid-onset ALS has symptoms that appear quickly.
- Limb-onset ALS starts with symptoms in arms or legs.
- Bulbar-onset ALS starts with trouble swallowing or speaking.
Symptoms of ALS
The first symptoms develop gradually and can vary from person to person. They include:
- Difficulty walking
- Weakness in hands, legs or feet
- Slurred speech or change in pitch
- Swallowing difficulties
- Uncontrollable crying or laughing
- Difficulty holding head up or maintaining posture
- In some cases, cognitive (thinking) and/or behavior impairment
Diagnosing ALS
Our ALS team includes experts at diagnosing this challenging condition. If you are referred to OHSU for an ALS diagnosis, you’ll meet with multiple specialists during one visit. Your team may include:
- A neuromuscular expert
- Physical, occupational, speech and respiratory therapists
- A dietitian
- A social worker
All your specialists will work together to confirm a diagnosis and help you plan for treatment.
What to expect during diagnosis
Review of tests and physical exam: We will do a complete physical and neurological exam, looking for signs of muscle weakness. We will also look over any previous tests.
EMG: You can expect to take an electromyography test, which takes about 30 minutes. An EMG shows doctors if there’s a problem with messages between your nerves and muscles.
Pulmonary function tests: These tests help determine how well your lungs are working. They measure the size of your lungs, the airflow and how well oxygen reaches your blood.
Blood and urine tests: We use these tests to look for high levels of certain proteins and hormones that may be signs of ALS.
Imaging tests: You may have an MRI (magnetic resonance imaging) or X-ray. These give us detailed pictures of the structures in your body. They can help rule out other conditions that may be causing your symptoms.
Treatments for ALS
The goal of treatment is to manage your symptoms as ALS progresses. A social worker can help you with financial issues, finding resources and other issues around care.
Treatment often includes:
Medications: Your care team may prescribe medications to:
- Reduce damage to motor neurons, possibly prolonging survival.
- Slow the decline in daily functioning.
- Relieve symptoms such as muscle cramps, stiffness, excess saliva and constipation.
- Help with pain, depression, unwanted displays of emotion and sleep difficulties.
Two medications are approved in the United States to slow the disease’s progression:
- Riluzole (brand name Rilutek), taken as a pill, may prolong life for several months.
- Edaravone (Radicava), taken as a pill or given as an IV, is a newer medication that shows promise for some patients with rapid-onset ALS.
Physical therapy: We offer one-on-one physical therapy sessions using the latest equipment. Our neurologic rehabilitation specialists will customize a plan for you that may include:
- Low-impact aerobic exercises to strengthen muscles, improve heart health, and combat fatigue and depression.
- Stretching exercises to help prevent muscle stiffening.
Mobility devices: We will help you decide if ramps, wheelchairs, walkers or braces are the right tools to help you stay mobile as ALS progresses.
Palliative care: Our palliative care specialists are here for you at any stage of ALS. You do not have to stop other treatments. These specialists can:
- Help you and your family make decisions.
- Support communication with your family and care team.
- Provide emotional and spiritual support.
- Offer treatments to relieve pain and stress.
Other support services:
- Speech therapy to help you speak louder and more clearly.
- Nutritional support, including menu plans to help you avoid losing weight. If eating becomes impossible, we’ll guide your transition to a feeding tube.
- Breathing support, such as a ventilation mask, as respiratory muscles weaken.
- ALS Northwest meetings twice a month. People with ALS typically come to a session once every three months to meet with providers and discuss next steps. You may meet with:
- A neuromuscular expert
- A dietitian
- Physical, speech and occupational therapists
- A respiratory therapist
Research and clinical trials
The OHSU Brain Institute is a leading recipient of research funding from the National Institutes of Health, with studies on improving ALS treatment. They include work by internationally recognized scientist Melanie Fried-Oken, Ph.D., on a communication system for patients with ALS and other conditions. It uses a computer interface to read brain signals, restoring a voice to patients with paralysis.

Learn more
- What is ALS?, ALS Association
- ALS: Amyotrophic Lateral Sclerosis (ALS), The Muscular Dystrophy Association
- Amyotrophic Lateral Sclerosis (ALS) Fact Sheet, National Institute of Neurological Disorders and Stroke
- Amyotrophic Lateral Sclerosis, U.S. National Library of Medicine
- For People with ALS and Caregivers, ALS Association
- ALS Northwest
For patients
- Referral: To become a patient, please ask your doctor for a referral.
- Nerve Center referrals: You may also be referred to us by the OHSU Nerve Center, where specialists direct patients to the team best able to treat them.
- Questions: For questions or follow-up appointments, call 503-494-5236.
Location
Parking is free for patients and their visitors.
OHSU ALS and Neuromuscular Disease Center
Center for Health & Healing Building 1, eighth floor
3303 S. Bond Ave.
Portland, OR 97239
Refer a patient
- Refer your patient to OHSU.
- Call 503-494-4567 to seek provider-to-provider advice.
Clinical trials
- Look for an OHSU Brain Institute clinical trial.
-
Learn more about current clinical trials for patients with ALS or other neuromuscular disorders by contacting:
Diana Dimitrova, Ph.D.
503-494-7269Research assistants:
Katie Lewis lewiskat@ohsu.edu
Katie Norris norriska@ohsu.edu
Difficult diagnosis ends a mystery
Why was a Eugene novelist’s voice faltering? For 14 months, with a series of doctors, she searched for answers. Then she saw OHSU neurologist Nizar Chahin. Read the story from The Washington Post.
