Arrhythmia and Heart Rhythm Diagnosis and Treatment

At OHSU, we offer the widest array of arrhythmia treatments and services in Oregon. Our expert providers focus on your quality of life as well as your treatment success.
You’ll find:
- Electrophysiologists, physician associates, nurses and researchers who work as a team to offer you personalized care.
- Experts with deep experience treating complex and high-risk conditions.
- A safe-MRI program for people with pacemakers or defibrillators.
- Access to the latest devices and treatments through clinical trials.
- The most experienced lead extraction experts in Oregon.
- Access to OHSU experts in sleep apnea, genetics, heart failure and cardiac surgery.
Diagnosing arrhythmia
Physical exam: We will ask you about your medical history and symptoms, and listen to the speed and pattern of your heartbeat. We may check for signs of thyroid disease, heart failure or other conditions that can cause heart rhythm problems.
Electrocardiogram (EKG): This test measures your heart’s electrical activity, including how fast it is beating and whether the rhythm is steady.
Holter monitor: A wearable EKG device that records your heart’s electrical activity as you go about your activities.
Echocardiogram (echo): This test uses sound waves to make images of your heart’s size, structure, and movement. This gives us information on how well it is working.
Event monitor: This wearable EKG detects heart rhythm problems that don’t happen often. You will wear it for up to 30 days.
Stress test: Some arrhythmias are caused by exercise. We record your heart’s activity while you walk on a treadmill or pedal a stationary bike.
Electrophysiologic studies: We put a catheter (thin, soft tube) into a blood vessel and thread it to your heart. There, electrodes map and measure the electrical signals that make your heart beat and pump blood around your body. Sometimes we can treat the arrhythmia while doing the study.
Treatments and services
Arrhythmias are complex and you need a treatment tailored to your condition. Patients come to us from across Oregon because we offer:
- In-depth consultations with an electrophysiologist, a doctor trained to diagnose and treat heart rhythm problems.
- Caring doctors, physician associates and nurses to answer all your questions.
- In-person pacemaker and defibrillator checks paired with an exam for your convenience.
- Nurses to guide you through complex procedures like lead extraction.
-
We work with you and your primary care provider to help you:
- Lower your blood pressure and cholesterol
- Treat sleep apnea
- Quit smoking
- Cut down on alcohol
- Reach a healthier weight
- Manage stress that can affect your heart
-
We may suggest medicines to control your heart rate or rhythm. These will depend on your medical history and type of arrhythmia.
-
While you are sedated, your provider uses a machine outside your body to send your heart one or more controlled electric shocks. These shocks can restore a normal heart rhythm.
External Cardioversion
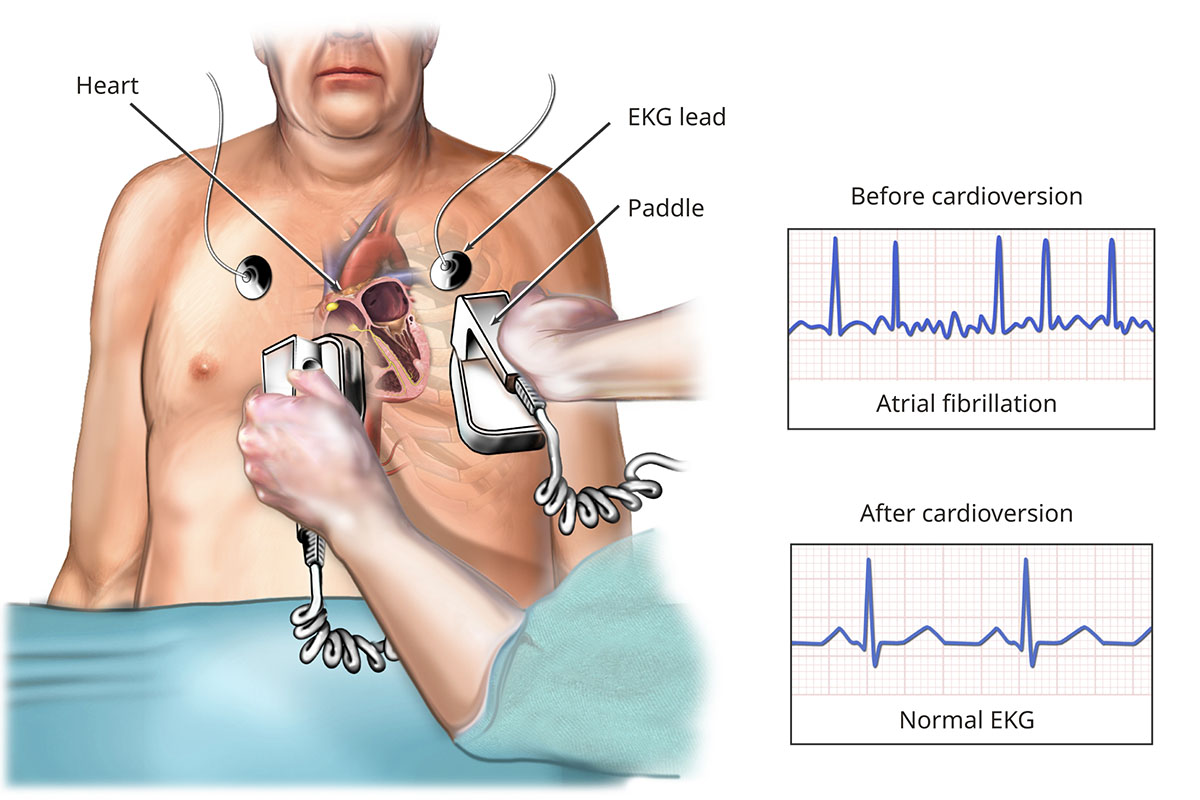
Cardioversion can return your heart to a normal rhythm. Medical Illustration Copyright © 2023 Nucleus Medical Media. All rights reserved. -
We thread catheters (small, soft tubes) through blood vessels to the heart. Electrodes on the catheters find the source of electrical signals that are disrupting your heartbeat. We burn or freeze tiny parts of this tissue to make small scars. These scars block the bad electrical signals, restoring a normal heartbeat.
-
When abnormal electrical signals start on the outside of the heart, we can’t treat them with standard ablation. Instead, we insert a needle and catheter into the space around your heart. We then create tiny scars on the outside of the heart to block the bad electrical signals. We are one of the few centers in Oregon to offer this procedure.
-
A permanent pacemaker (PPM) is a small device that is implanted under the skin, just below the collarbone. If your heart beats abnormally or stops, the pacemaker sends out electrical signals to restore a normal heartbeat.
A biventricular pacemaker placement (cardiac resynchronization therapy) is used to treat heart failure if the heart’s two lower chambers aren’t pumping together. This pacemaker keeps the right and left ventricles in rhythm.
A leadless (wireless) pacemaker is much smaller than a PPM. We thread a catheter through blood vessels to your heart and place the pacemaker right in a lower chamber. At OHSU, we place more of these than any other center in the Northwest.
-
We place this small device in your chest or abdomen to constantly check for abnormal heart rhythms. If it picks up a dangerous rhythm, it sends out electrical shocks to restore a normal rhythm.
-
This device is also called an implantable loop recorder. It detects dangerous heart rhythms before they become deadly. We place it just under the skin in a minor surgery. It allows us to monitor your heart rhythms for up to three years. Your provider may recommend an implantable loop recorder if you have unexplained fainting spells, arrhythmias or stroke.
-
If we need to remove or replace your pacemaker or defibrillator, we also need to take out the leads (wires) that deliver energy from the device to your heart. Your body forms scar tissue around the leads, making them hard to remove.
Our electrophysiologists are lead removal experts. In complex cases, they use a special laser and other tools to help break up scar tissue, making removal safer and easier.
You may need to have leads removed if:
- The wire is damaged.
- There is an infection near the lead or the device.
- Scar tissue interferes with the functioning of the device.
- A vein is blocked with a clot or scar tissue.
Safe MRI for people with pacemakers or defibrillators
Until recently, people with an old pacemaker or defibrillator couldn’t get an MRI, even if they needed one for other health problems.
At OHSU, people with older devices can safely get an MRI. We pioneered this process in Oregon and do more device-safe MRIs than any other center in the state.
We check your device before the MRI to be sure it is safe to do the scan. During the MRI, we monitor your heart rhythms. We check your device again after the MRI to make sure it is working correctly.
Other OHSU services
At OHSU, you have access to other programs that offer support and treatment for issues that can be linked to arrhythmia. These include:
Learn more
- Arrhythmia treatments, Heart Rhythm Society
Location
Center for Health & Healing, Building 1
3303 S. Bond Ave.
Portland, OR 97239
Free parking for patients and visitors
Refer a patient
- Refer your patient to OHSU.
- Call 503-494-4567 to seek provider-to-provider advice.