Urinary Incontinence and Overactive Bladder

If you leak urine when you laugh or cough, or feel a sudden urge to, you’re not alone. Urinary incontinence is common, especially as we age. The OHSU Center for Women’s Health provides expert care for women's bladder health.
You’ll find:
- Team-based care from top specialists in stopping leaks and urges.
- Specialized tests and technology to fully evaluate and treat your condition.
- Effective non-surgical care options tailored to your needs and preferences.
- Minimally invasive surgical techniques for faster relief and easier recovery.
Understanding urinary incontinence
What is urinary incontinence?
Urinary incontinence is a loss of bladder control. It causes urine leaks, frequent urination, or strong, sudden urges to urinate. Without the right care, it can disrupt your activities. Incontinence can affect your sleep, your ability to stay active and your confidence.
Urinary System
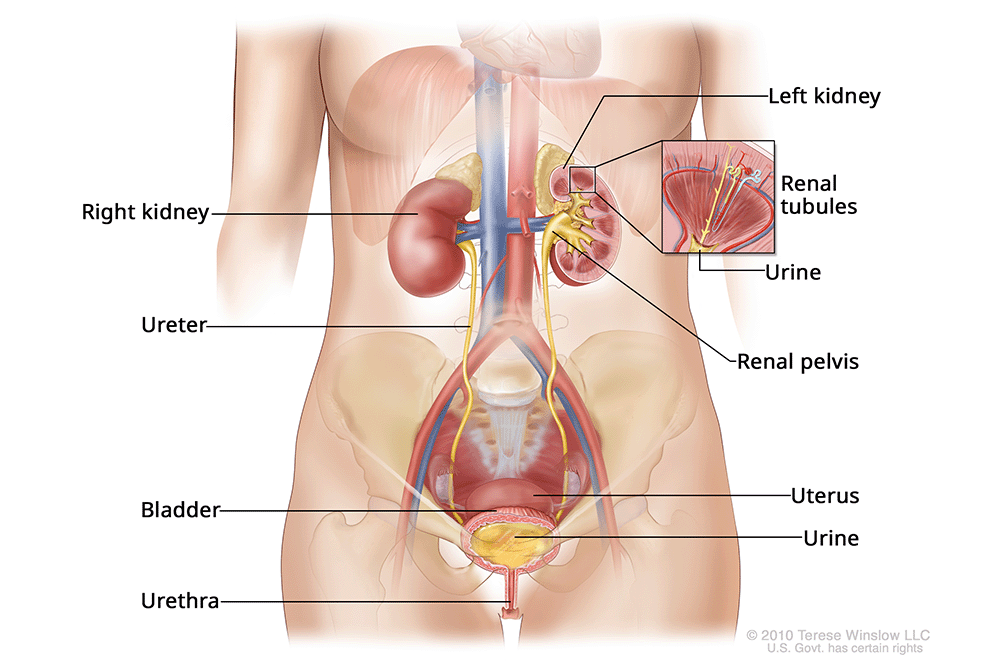
Types of urinary incontinence
Knowing what type of urinary incontinence you have will help you choose the best treatment. Your care team will help identify the cause of your symptoms.
Stress urinary incontinence
- What it is: Urine leakage when you cough, sneeze, exercise or laugh, which puts pressure on your bladder. Leaks can feel like a squirt and be small or big.
- What causes it: Weak muscles and tissues in your bladder and urethra (the tube that takes urine out of your body). The bladder acts like a balloon filled with liquid. The rise in pressure forces the tube open, and urine comes out.
Urgency incontinence (overactive bladder)
- What it is: Frequent, strong, or sudden urges to urinate. You may not make it to the restroom in time, and you may leak. Urges can wake you up at night.
- What causes it: A muscle spasm or increased sensitivity of your bladder. Everyday activities — such as hearing running water — can trigger the urge.
Who gets urinary incontinence?
Urinary incontinence is common in women. About 30% to 50% of women have it. The rates increase with age and peak around menopause.
Risk factors include:
- Pregnancy and vaginal delivery
- Pelvic surgery
- Radiation treatment to the pelvis
- Pressure on the abdomen from obesity, chronic coughing, constipation or heavy lifting
- Conditions that affect your muscles and nerves, such as spinal cord injuries or multiple sclerosis
- An inherited weakness in the connective tissues of your pelvis
- Drinking a lot of caffeinated beverages
- Smoking
Symptoms of urinary incontinence
Talk with your care provider if you have:
- Bothersome urine leaks
- A need to urinate often during the day and more than twice at night
- Sudden, strong urges to urinate
- Difficulty making it to the restroom fast enough
- Bladder pain or discomfort
Diagnosing urinary incontinence
We offer complete pelvic floor testing to find your specific problem. Our lab provides quick, painless tests in a private, comfortable setting. Your care team will explain each test in detail. We may use one or more of these tests:
Urodynamics: These tests help figure out how well your bladder holds and empties urine. We use them to evaluate whether surgery could improve your condition.
Cystoscopy: This test uses a lighted flexible telescope to look inside your bladder. It allows us to see if your bladder is inflamed or has other problems that may be causing your leaks.
Ultrasound: We are leaders in evaluating pelvic floor disorders with 3D ultrasound. Ultrasound uses sound waves to create moving images of the organs and muscles in your pelvis. We place an ultrasound transducer on your abdomen or near your vagina and look at the images on a screen.
Urinary incontinence treatments
You may improve quickly with the right treatment, or you may try a few approaches before we learn what works best. We will help you choose the best treatment for you and adjust your care plan as needed.
-
Non-surgical treatments
We offer effective options to treat urinary incontinence without surgery. Your provider will talk with you about which options could help you.
Physical therapy: Pelvic floor exercises, such as Kegels, can reduce urinary leaks and urges. You can do them at home or with the help of our physical therapists. Kegel exercises help you build strength by squeezing your pelvic floor muscles.
Biofeedback: You can improve Kegel exercises by using a biofeedback device to target the right muscles and measure the strength of your squeeze. You can do this at home or in our office with special equipment.
Lifestyle changes: Certain foods and drinks can irritate your bladder. You may also have daily routines that make your condition worse. We review your habits to find any patterns you could change to improve your condition.
Pessary: This is a flexible device you can insert in your vagina. It lifts and supports the pelvic organs. It can help by removing pressure on your bladder.
Tibial Nerve Stimulation: We place an electrode on your inner ankle to send electrical signals to the nerves in your bladder. The nerve stimulation regulates your urges to urinate.
Medications: There is a wide range of medications that can reduce your urges by relaxing your bladder muscle. We also offer drugs to relieve bladder pain.
-
Surgical treatments
Our skilled surgeons specialize in treating women’s pelvic floor disorders.
They have the most experience in Oregon and Southwest Washington with minimally invasive surgeries.
Procedures for stress incontinence include:
- Mid-urethral sling: Your surgeon places surgical mesh under the urethra (the tube that empties urine from the body) to support it.
- Burch colposuspension: We lift your vaginal wall by stitching it to ligaments or other tissues in your pelvis, providing more support.
- Fascial sling: We take a small piece of strong connective tissue from your abdomen and place it under your urethra to support it.
- Urethral bulking: We inject a filler into the soft tissue of your urethra. The material tightens the opening from your bladder to the urethra, helping it close more easily.
Procedures for urgency incontinence and overactive bladder include:
- Botox injections: Botox, the chemical used to reduce wrinkles, can stop your frequent urges to urinate. Your doctor injects it into your bladder to quiet the nerves that signal your muscles to urinate. You can repeat the procedure every 6-12 months.
- Sacral neuromodulation: We place a nerve stimulator in your low back in a two-step procedure. The device regulates the nerves that control your bladder. You can set it to a level that works for you. You do not have to stay in the hospital to get these surgeries.
Resources about urinary incontinence
- Bladder control, Voices for PFD
- Overactive Bladder, National Association for Continence
- Stress Urinary Incontinence in Women, National Association for Continence
- Urinary Incontinence, Office on Women’s Health, U.S. Department of Health & Human Services
- Bladder Control Problems in Women, National Institute of Diabetes and Digestive and Kidney Diseases
- Urinary Incontinence, U.S. National Library of Medicine
For patients
Call 503-418-4500 to make an appointment.
Location
OHSU Center for Women’s Health, Marquam Hill
Kohler Pavilion, seventh floor
808 S.W. Campus Drive
Portland, OR 97239
Free parking for patients and visitors
Refer a patient
- Refer your patient to OHSU.
- Call 503-494-4567 to seek provider-to-provider advice.
FAQ and Resources
Find answers to common questions and links to national resources.