Hypospadias

OHSU Doernbecher Children’s Hospital offers expert care for hypospadias, a birth defect involving the opening in the penis. You’ll find:
- Doctors with advanced surgical training who do hundreds of hypospadias surgeries a year.
- A high rate of success in treating the most common type of hypospadias.
- Experts in treating all types of hypospadias, including correcting failed surgeries.
Understanding hypospadias
What is hypospadias?
In hypospadias, the opening in the penis is on the underside, not at the tip. The opening (called the meatus) is for the urethra, the tube the carries urine and semen. It may be:
- Most commonly, near the tip of the penis (distal hypospadias)
- In the middle of the penis
- At the base of the penis
- Rarely, in or under the scrotum
Some boys with hypospadias may also have these conditions:
- The penis is curved downward (chordee).
- The foreskin is fully formed only on top of the penis.
- One testicle doesn’t fully drop into the scrotum.
If it’s untreated: Depending on the severity, untreated hypospadias can lead to embarrassment, needing to sit to urinate, or problems with intercourse.
Causes: The causes of hypospadias are unclear. Problems with the hormones that trigger the urethra and foreskin to develop may be one cause, according to the American Urological Association. OHSU researchers are working with Shriners Hospitals for Children to study the genetic causes of hypospadias.
Types of Hypospadias
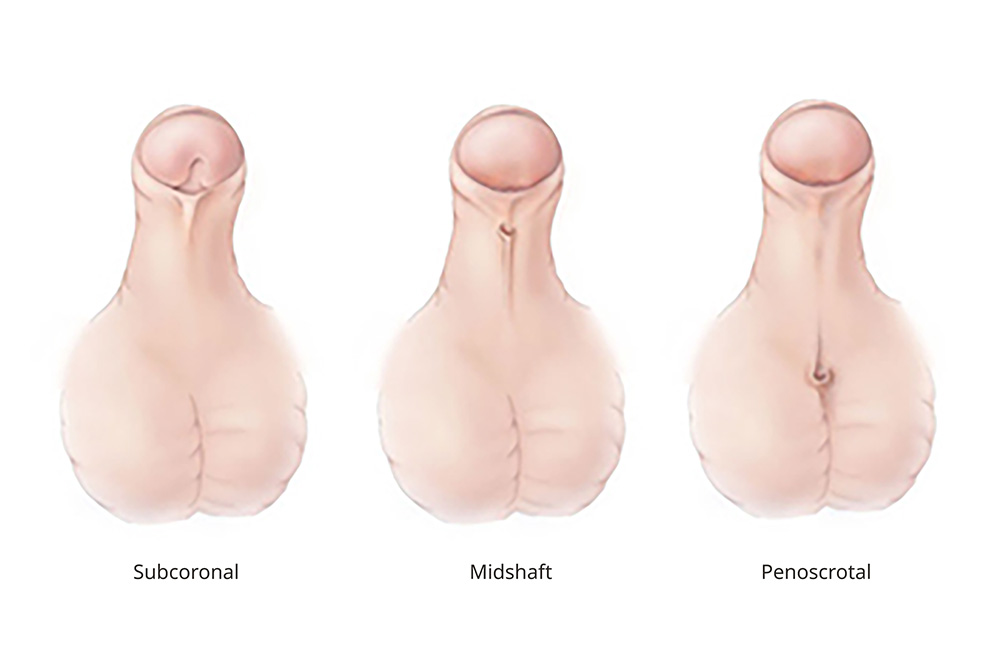
Who gets hypospadias?
Hypospadias is one of the most common birth defects in boys. It affects about 1 in 200 boys, according to the Centers for Disease Control and Prevention.
Signs and symptoms of hypospadias
Hypospadias is usually apparent but not always. Other than a misplaced opening, you may notice:
- Your child’s penis is curved downward.
- Your child’s penis appears hooded because the foreskin covers only the top part.
- Your child’s urine stream sprays or isn’t straight.
Risk factors for hypospadias
Recent research by the CDC and the National Institutes of Health shows these may increase risk of hypospadias:
- Family history: The risk is higher if the boy’s father had hypospadias.
- Baby’s weight: Risk increases for babies born underweight.
- Fertility treatments: Risk is higher for babies whose mothers used treatments such as fertility medications or in vitro fertilization.
- Hormones: Babies are at higher risk if their mother took certain hormones, such as progesterone, while pregnant or just before.
Diagnosing hypospadias
Hypospadias is typically diagnosed shortly after birth, usually during a physical exam in the hospital. Sometimes it’s noticed when a doctor prepares for a circumcision. A slight misplacement might not be diagnosed until later.
If hypospadias is found, we typically recommend that your son not be circumcised until a pediatric urologist can evaluate him. In mild cases, though, we can usually correct hypospadias on circumcised boys.
Treating hypospadias
-
Boys with mild hypospadias may not need surgery. Most often, though, surgery is recommended to:
- Move the opening to the tip of the penis.
- Create a normal urinary channel.
- Straighten the penis, if needed.
- Rebuild or remove the foreskin.
Your son can usually go home the same day. He may need a small catheter (a flexible tube) to drain urine for a week.
If your child needs surgery, our pediatric urologists offer:
- Successful repair of distal hypospadias in more than 90% of cases.
- Experience in correcting all types of hypospadias, including severe penis curvature.
- Expertise in using tissue grafts to create a new urethra when it hasn’t fully formed.
-
We typically do surgery when your son is 6 months to 18 months old.
-
Most boys have a normal-looking, fully functional penis in about six months. The urethra usually grows with the penis.
Fewer than 1 in 10 boys have complications from hypospadias surgery, the American Urological Association reports. Problems can include a hole forming elsewhere on the penis and scars that restrict urine. These usually show up within a few months and can be fixed with surgery.
Learn more
- FAQ for Parents, Hypospadias and Epispadias Association
- What Is Hypospadias? Urology Care Foundation
Locations
Parking is free for patients and their visitors.
Doernbecher Children’s Hospital
700 S.W. Campus Drive
Portland, OR 97239
Map and directions
We also offer locations in Eugene and Salem.
Refer a patient
- Refer your patient to Doernbecher.
- Call 503-346-0644 to seek provider-to-provider advice.