Epilepsy Treatment
The OHSU Comprehensive Epilepsy Center offers the most advanced care for people with epilepsy. Our specialists provide options and expertise you won’t find anywhere else in Oregon. We offer:
- Oregon’s only Level 4 epilepsy center for the highest level of care.
- A focus on controlling seizures early, starting with medication but quickly shifting to other options if needed.
- A robotic, MRI and laser system for complex epilepsy that makes minimally invasive surgery an option for more patients.
- The most experience in Oregon with using implantable devices to treat epilepsy.
- Expert neurologists, neurosurgeons and other specialists with advanced training in epilepsy care.
Treatment overview
Our goal is for you to live seizure-free with the fewest side effects possible. We will work with you to find the approach that works for you.
Team-based care
A nurse navigator will coordinate your care and answer your questions. Your care team will also include specialists who work together, including meeting twice a month to review cases.
Our approach
- Medication: We begin treatment with medication to control seizures. This successfully treats about 70% of patients.
- Next steps: If needed, we shift to additional options quickly so we can control seizures and protect your health. Options include the latest epilepsy surgeries and minimally invasive techniques.
- Diet: We can also provide counseling on special diets to help avoid epilepsy triggers.
Epilepsy medication
For most patients, medications can prevent or stop seizures. The effectiveness of each medication varies from person to person. It also varies by the type of seizure or epilepsy syndrome.
You may find relief with the first medication you try, or you may need to try another or a combination. Your care team will check in with you often to make sure you have the right medication(s) and dose. You will also have regular follow-up appointments.
For the most effective seizure control, we recommend that you:
- Take your medication exactly as prescribed.
- Talk with your doctor before taking other prescriptions or over-the-counter medications.
- Not stop taking your medication without consulting your doctor.
The Epilepsy Foundation keeps a detailed, updated list of seizure medications.
At regular follow-up visits, we usually do one or more tests to check how well your medications are working. Tests may include:
- Blood tests: We measure the amount of anti-seizure medication in your blood. Your team can adjust the dose as needed.
- EEG (electroencephalogram): We may do an EEG to see how well your medication is controlling your brain’s electrical activity. We use sensors attached with adhesive to record your brain’s electrical activity.
Diets to manage epilepsy
Special diets can help reduce seizures in some children and adults with epilepsy. Diet recommendations are usually in addition to medication. Following are the diet plans we recommend most often.
Doctors may recommend this high-fat, low-carbohydrate diet for children whose seizures remain uncontrolled after trying several medications. Research shows it is effective for adults, too, though it can be challenging to follow.
The ketogenic diet:
- Severely restricts carbohydrates
- Requires 3 to 4 grams of fat for every 1 gram of carbohydrate and protein
- Recommends consuming butter, heavy cream, mayonnaise and oils such as olive oil
- May require a fast of 18 to 24 hours before starting
The modified Atkins diet (MAD) also restricts carbohydrates but less so than the ketogenic diet. Doctors may recommend this diet after trying multiple medications.
The modified Atkins diet:
- Does not restrict proteins
- Encourages but does not require high-fat foods
- Does not restrict calories
- Requires no fast before starting
OHSU’s three-part system for diagnosis and surgery
OHSU provides the most advanced, minimally invasive system in Oregon for diagnosing and treating some types of epilepsy. It may be an option for severe epilepsy or epilepsy that hasn’t responded to other treatments. The three parts are:
- ROSA (robotic stereotactic assistance): The ROSA robot enables neurosurgeons to place as many as 20 fine electrode wires in any part of the brain. We use GPS-like imaging for pinpoint accuracy. We can precisely map the seizure focus, the place where seizures start.
- iMRI (intraoperative MRI): Our iMRI suite makes to-the-millimeter imaging part of surgery. The iMRI glides to the operating table so surgeons can see in real time the exact location and dimensions of the tissue to be removed.
- Laser therapy: Our minimally invasive laser probe, guided by the iMRI, allows us to remove the seizure focus through small incisions. Read more about laser therapy in the surgery section below.
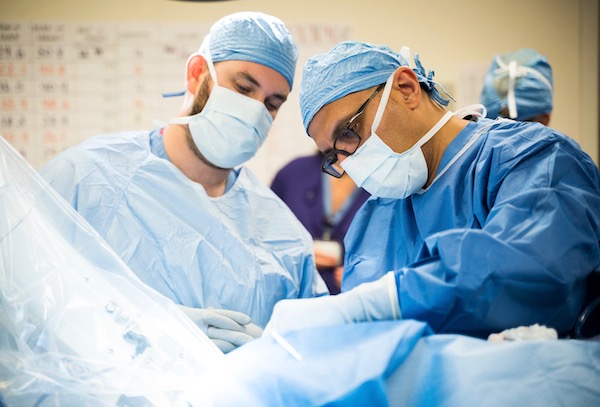
OHSU neurosurgeons are the first in Oregon to use this system for both children and adults. Advantages include:
- Minimally invasive: Patients who once needed two open brain surgeries can now have one minimally invasive procedure.
- One location: The entire procedure can take place in our state-of-the-art neurosurgery suite.
- Time: It takes half the time of previous procedures.
- Patient safety and comfort: The system includes the ability to remove the electrode wires at bedside. The speed and smaller incisions also make it safer, with much shorter recovery times.
- New hope: This system can provide a diagnosis for patients with deep or more than one seizure focus. It also makes surgery to stop seizures available to more patients than ever.
- Precision: The high level of accuracy means surgeons can remove the seizure focus while protecting healthy brain tissue.
Surgery to treat epilepsy
For some people, medication and diet don’t control seizures. Epilepsy surgery offers another option.
Surgical planning and imaging

Before any surgery, our epilepsy team reviews your test results and other details. We talk with you about our recommendations and options.
For many epilepsy surgeries — for children and adults — we use the iMRI suite at OHSU Doernbecher Children’s Hospital. The intraoperative MRI enables our surgeons to see finely detailed brain maps during surgery. They can remove targeted tissue without harming nearby healthy tissue.
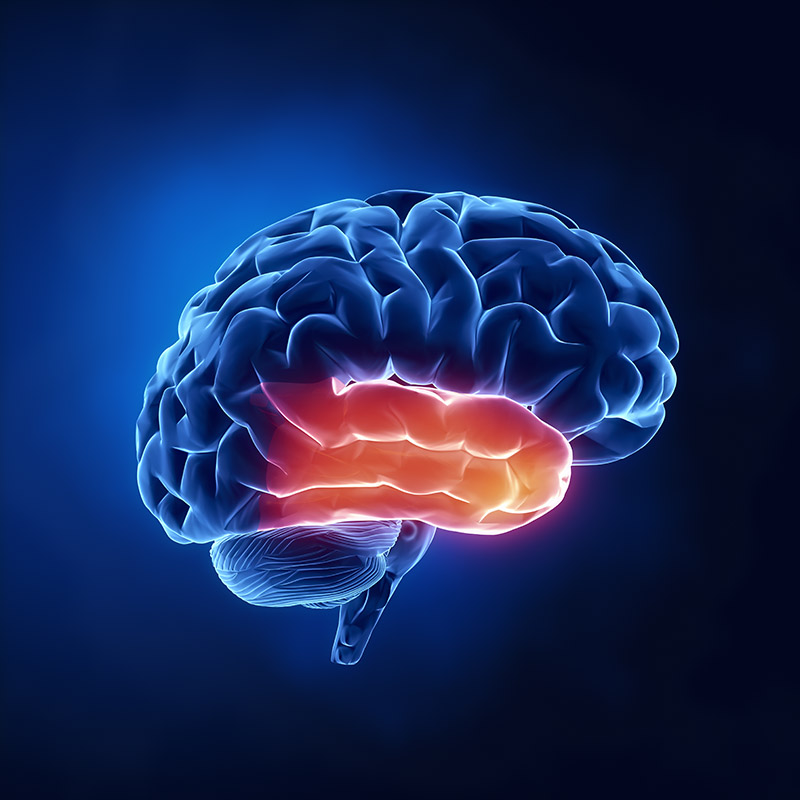
Temporal lobe surgery
In many people with epilepsy, seizures begin in one of the brain’s two temporal lobes. The temporal lobes sit on each side of the brain, behind each ear and temple.
A temporal lobectomy removes part of the lobe where seizures start. More than 85% of people who have a temporal lobectomy have improved seizure control.
When considering temporal lobectomy, you and your doctors will discuss the risks and benefits of each type:
Anterior temporal lobectomy: This is the most common surgery to control seizures that do not respond to medications. Your surgeon removes a small portion of the anterior, or front, of a temporal lobe. Risks include loss of some memory or vocabulary, partial vision loss, and mood problems. These effects may be temporary.
Selective amygdalohippocampectomy: In SAH, your surgeon removes small portions of the hippocampus and amygdala (within the affected temporal lobe) containing a seizure focus. Compared to anterior temporal lobectomy, SAH may have fewer effects on memory and other functions.
Laser ablation therapy
OHSU is one of only a few dozen centers in the country with laser interstitial thermal therapy. LITT is a type of ablation, which uses heat to remove unwanted cells. During this minimally invasive surgery:
- We use our iMRI to map the seizure focus in real time.
- Through a small opening in the skull, the surgeon guides the laser, using the mapping to reach the target area.
- The surgeon removes or destroys the seizure focus. Nearby healthy brain tissue is unharmed.
Because the procedure requires only a small incision, you will probably recover more quickly and go home sooner. LITT also may have fewer effects on thinking.
Lesionectomy
A lesionectomy is open surgery to remove a seizure focus caused by a lesion — damaged or diseased brain tissue. Brain lesions can result from:
- Tumors
- Hematomas, swollen areas filled with blood that can develop after head trauma
- Scar tissue from a head injury or infection
- Abnormal blood vessel formation, known as arteriovenous malformation, or AVM
Responsive neurostimulation
OHSU is the only center in Oregon offering responsive neurostimulation, or RNS. Our epilepsy specialists were involved in developing the implanted RNS system and doing the research that led to FDA approval in 2013.
Who gets RNS: RNS can provide an option for people whose seizures have not responded to multiple medications and who cannot have surgery because of seizures that:
- Start in more than one area in the brain
- Are difficult to locate
- Happen in brain regions that cannot be operated on without affecting critical brain function
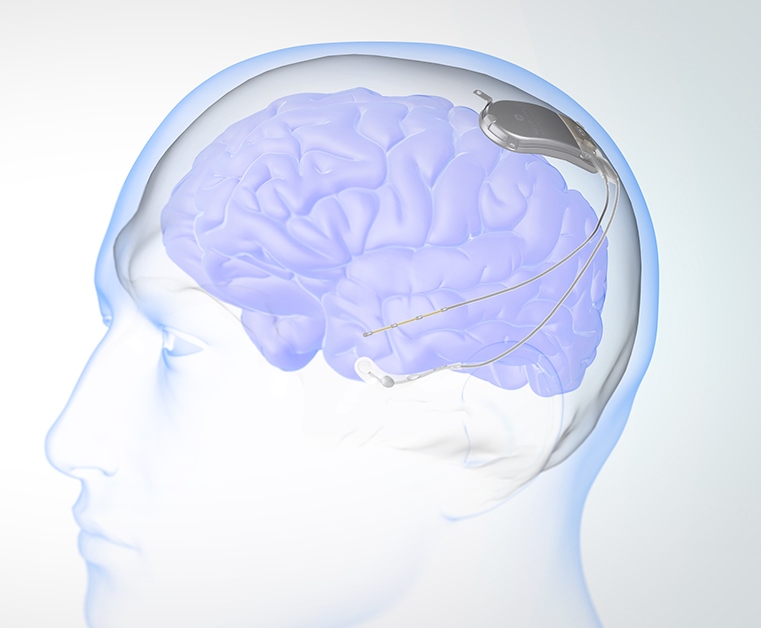
How RNS works: The RNS system consists of a small device called a neurostimulator and one or two electrodes connected to tiny wires. During the procedure:
- The surgeon implants the neurostimulator on the brain through a small opening in the skull.
- The surgeon connects the electrode(s) to the device and places them in or on the brain at the seizure focus.
- Your doctor programs the RNS system to continuously monitor your brain’s unique electrical activity to detect seizures or seizure-like responses.
When the system spots unusual activity, it delivers a small electrical signal to disrupt or prevent seizures. Your care team monitors your brain’s electrical activity over time. Doctors can adjust the device’s settings to customize the system to your needs.
This therapy is also reversible. The device can be removed if it proves ineffective.
Vagus nerve stimulation
Vagus nerve stimulation (VNS) consists of a device and wires that are implanted during a minimally invasive procedure.
Who gets VNS: Like RNS, VNS offers an option for people whose seizures have not responded to multiple medications and who cannot have surgery.
How VNS works: For VNS, the surgeon implants the device under the skin of your chest, like a pacemaker. The surgeon connects the wires to the vagus nerve in your neck.
The stimulator does not detect or monitor seizure activity. Instead, your doctor programs it to deliver electrical impulses in specific cycles. You receive a handheld magnet to turn the stimulator on when you sense a seizure is coming.
For patients
- Referral: To become a patient, please ask your doctor for a referral.
- Questions: For questions or follow-up appointments, please call 503-494-7772.
- Epilepsy FAQ and resources
- OHSU care for children and teens with epilepsy
Location
Parking is free for patients and their visitors.
Mark O. Hatfield Research Center, 13th Floor
3250 S.W. Sam Jackson Park Road
Portland, OR 97239
Map and directions
Refer a patient
- Refer your patient to OHSU.
- Call 503-494-4567 to seek provider-to-provider advice.