OHSU Northwest Clinic for Pediatric Voice-Diagnostics
We offer advanced imaging technology for vocal cord imaging and analysis of vocal quality. Our focus includes not only obtaining the best possible images of the larynx, but also on completing the examination in a manner that allows the child to be engaged in the process and as comfortable as possible. Our diagnostic services include:
- Perceptual and acoustic voice evaluation, including voice recordings and instrumental analysis
- Indirect laryngoscopy –visualization of the larynx using a standard halogen light for evaluation of laryngeal structure and motion
- Videostroboscopy –visualization of the larynx using a stroboscopic light for evaluation of vocal fold vibration, allowing for detailed evaluation of the vocal fold mucosa or tissue.
Problems/Disorders:
The following information discuss the symptoms, causes, and treatment for some of the more common pediatric voice disorders. Note: The information contained in these pages is for educational purposes only. It should not be construed as individualized diagnostic and treatment advice.
Hoarseness:
Hoarseness, also known as dysphonia, is a general term for difficulty voicing. Most people will experience hoarseness at some time, usually related to a cold or after a period of heavy voice use, such as yelling at a football game. This rough, scratchy voice will usually last for a few days and then the voice quickly returns to normal. Any change in voice that lasts for more than two weeks may indicate a more serious problem and should be checked by a doctor. Ongoing (chronic) hoarseness can be caused by many different voice reasons. Common voice complaints include, but are not limited to: hoarseness, poor vocal quality, fluctuating voice, vocal tiredness, effortful voicing, pitch changes, poor vocal control, weak voice, and pain or discomfort with voicing. Hoarseness in children has been shown to negatively affect a child's communication, social participation and academic performance and is not a natural occurrence that children will "outgrow." As such, chronic hoarseness should be evaluated by a physician so that an appropriate treatment plan can be established, minimizing the impact of hoarseness on a child's development.
Nodules and Cysts
Vocal fold nodules and cysts are benign (non-cancerous) growths which can affect people of all ages and are the most common cause of hoarseness in children. Nodules are most often found on both sides of the folds, and are found at the junction of the front and middle third of the free edge of the vocal folds. Cysts are usually only found on one side and can occur anywhere on the fold. When the cyst is at the free edge, it is common for a reactive nodule to form at the same location on the other fold.
Nodules typically occur as a result of voice misuse or overuse, which causes irritation and inflammation of the vocal fold mucosa. With continued voice use, the tissue becomes hardened. Cysts, on the other hand, are usually the result of a blocked mucous gland within the fold. As mucous fills up the area behind the blockage, the tissue grows and swells, and a cyst is produced. Some cysts occur at the time of birth and may show up with symptoms years later.
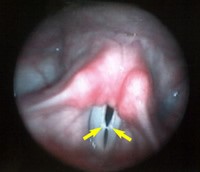
Vocal Cord Dysfunction (VCD):
Vocal cord dysfunction, also known as paradoxical vocal fold motion impairment, is a condition which leads to shortness of breath or stridor (high pitched or gasping sounds coming from the throat). VCD occurs most commonly in adolescent and teenage athletes. It is often mistaken for asthma because of its occurrence in exercise, but it does not typically respond to asthma medications. Often the person with VCD feels as if their airway is closing or partially closing with difficulty getting air in. In some cases the throat feels squeezed tight on both breathing in and out. During normal breathing, the vocal cords, which sit at the top of the airway, open to allow air to flow freely in and out of the lungs. During a VCD attack, the airway becomes temporarily narrowed due to the vocal cords partially blocking the airway. The shortness of breath is caused by movement of the vocal cords toward each other during the breathing cycle. Though the sensation of not being able to breathe is very frightening, VCD is typically a functional disorder and may successfully respond to treatment.
The primary symptom of VCD is shortness of breath, often accompanied by a sensation of tightness in the throat and/or upper chest. There is often more difficulty breathing in than breathing out. VCD can occur with asthma (in as many as 40% of the cases) making the diagnosis more complicated. Because the vocal cords are drawn together during a VCD attack, coughing, stridor (noisy breathing) and difficulty talking may occur. VCD symptoms usually come on fairly suddenly, often during exercise or after exposure to an irritant, and then subside anywhere from 2-30 minutes after the exercise or exposure has been stopped. Between attacks, individuals typically breathe normally and do not feel short of breath.
Any breathing difficulty should first be evaluated by a physician. A pulmonologist or asthma allergy specialist can diagnose whether asthma is present. The best way to confirm VCD is by doing laryngoscopy to look at the vocal cords, during an attack if possible. Laryngoscopy is an examination which is conducted in the ENT clinic and allows the doctor to see the larynx or voice-box with a special camera. Laryngoscopy can rule out any physical problem with the larynx as well as identify abnormal vocal cord motion during breathing. Some asthma and allergy specialists are able to do this, as are otolaryngologists (ENT doctors) and some speech pathologists. In specialty clinics such as ours at OHSU, we will often try to trigger an attack so that we can view what happens to the airway when this occurs. The examination is recorded so that the individual with VCD can be taught about the vocal cords and how it works. VCD often responds very well to therapy and is treated by the voice therapists in the ENT clinic.
Vocal Fold Motion Impairment (Vocal Cord Paralysis):
The vocal folds, because of the position in the airway, play a vital role in speech, swallowing, and breathing. In order to perform these functions normally, the laryngeal muscles must be able to abduct (open) and adduct (close) the folds.
Vocal fold motion impairment is of two major types: unilateral (more common) and bilateral. These types differ in their seriousness, symptoms, and treatment.
Symptoms: Patients with unilateral paralysis may have a weak and "breathy" voice, and speaking may require considerable effort. The sound associated with crying may also be affected. Because the vocal folds are unable to close completely during swallowing, patients may also experience coughing and choking while eating or drinking.
Causes: The most common cause of vocal fold motion impairment is injury to the recurrent laryngeal nerve, the nerve responsible for controlling the main muscles of the larynx. This may be due to injury, surgery, viral infection, a tumor pressing on the recurrent laryngeal nerve, or other causes. Occasionally, injury or diseases of the brain result in impaired motion.
Recurrent Respiratory Papillomatosis:
Rarely the virus that causes warts can infect the larynx. The warts (papillomas) can grow on the vocal cords causing hoarseness. Or they can grow to block the airway and cause breathing difficulties. To improve the child's voice and prevent life-threatening obstruction the papillomas must be removed surgically. Papillomas can occur at any age, though in children they typically develop during infancy or the pre-school years.
Symptoms: Children with papillomas are typically hoarse. The hoarseness can be present soon after the child starts to talk. And if the papillomas are bulky, noisy or loud breathing—like a wheeze but heard when breathing in—is heard.
Causes: It is thought that the virus (HPV or Human Papilloma Virus) is transmitted during birth, though this is controversial. However once infected the virus stays with the patient. The rate of growth of the warts, thus the frequency of needing removal, is highly variable between different patients.