About Our Program

Our vision is to develop exceptional and compassionate physicians from diverse backgrounds who serve their patients and communities by advancing science, promoting health equity, and delivering high-quality care. We emphasize academic excellence throughout residency while fostering a learning environment that supports both the personal and professional needs of our residents.
We provide broad foundational training that exposes residents to the full breadth and depth of medicine, ensuring they are well prepared for a wide range of future careers. Our program features innovative didactics, including curricula in Teaching Improvement Science, POCUS, and Advocacy, as well as unique clinical experiences such as the Social Medicine Block and a diverse array of rotations locally, nationally, and internationally.
Healthcare and resident education are evolving at a rapid pace. To ensure that we continue to train exceptional physicians who are fully prepared for their future careers, we are undergoing a multi-year strategic residency redesign process involving residents, faculty, leadership, and patients. We look forward to sharing more of where we are in the process and how you can become part of this exciting journey.
-
Our program uses a 3+1 schedule structure for all residents, allowing for a separation between inpatient and outpatient experiences such that residents can fully immerse themselves in patient care and education. Wards and ICU rotations are almost exclusively 3-weeks in duration, while other rotations in the X-block can vary in length. Residents always have the weekend off prior to starting their +1 week.
Averages for core PGY-1 and PGY-2/3 rotations are shown in the table below:
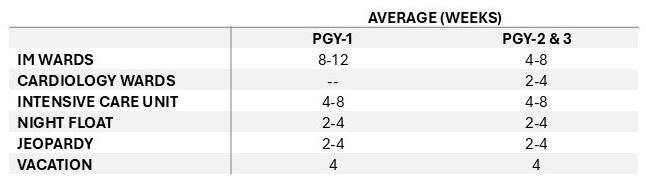
Sample Rotation Schedules
-
OHSU Wards
There are six general medicine teams on the Uni wards. Teams are comprised of one senior resident (PGY-2/3), one intern, and staffed by a hospitalist or general medicine faculty. Teams will often have medical students on their core or sub-internship rotations in addition to a physician assistant student. The admission cycle is a drip model with a team cap of 10 patients. A night float team is available six nights of the week, with the remaining night covered by a resident from one of the day teams (12h overnight shift).
PVAMC Wards
There are four general medicine teams on the VA wards. Teams are comprised of one senior resident (PGY-2/3), 2 interns, and staffed by a hospitalist. Teams will often have one medical student. The admission cycle is a drop model with a team cap of 14 patients. A night float team is available six nights of the week, with the remaining night covered by a resident from one of the day teams (~24h shift).
Cardiology Wards (11K)
All residents rotation on inpatient cardiology wards during PGY-2 and/or PGY-3. In Academic Year (AY) 2026-27, the team will be comprised of two residents during daytime hours only. Starting AY 2027-28, this will expand to a five-resident team and include nighttime coverage.
OHSU MICU
The MICU is a 16-bed closed unit with occasional off-unit boarders. There are four residents and four interns on service at any given time split between MICU A (primary rounding team), the Critical Care Activation Team (triage, codes, procedures), and nights. PCCM faculty and PCCM/CCM fellows are present in the hospital 24/7 for support.
PVAMC ICU
The VA ICU is a closed unit that services medical, cardiac, and surgical patients. There are four residents and three interns on service at any given time. Night coverage is provided by one resident and one intern, who rotate in blocks of 5-6 nights with a two-day transition back to the day schedule. A PCCM or CCM fellow is available until 10:00pm and will remain if needed, or can be called in overnight for urgent issues.
Work Hours
We are fully committed and adherent to the ACGME clinical and education work hour standards. We are continually seeking to improve, and residents have a strong voice in helping us design and implement necessary changes.
-
Ambulatory education is a foundational part of internal medicine training. We strive to foster an outpatient experience that is rich in learning and satisfying for the professional development of all our residents, regardless of their intended specialty.
Each year consists of thirteen +1 weeks. Residents are divided into four firms based on the timing of their +1 week. This supports residents developing close relationships with a subset of their peers. It also facilitates a team-based interprofessional practice model and allows patients to have consistent care from the same group of residents.
Each +1 week includes time in primary care continuity clinic, specialty clinics, and educational seminars, with protected administrative time for in-basket management. Senior residents also select a second longitudinal continuity clinic.

Primary Continuity Clinics
Residents can choose from one of three sites for their primary continuity clinic:Second Continuity Clinics
Starting during PGY-2, residents choose a second continuity clinic based on their career goals. Residents remain in this clinic for 12 months, then can select a new clinic in PGY-3, or repeat the same one. Select examples:- Subspecialty: Hepatology, Electrophysiology, Hematology, HIV, etc.
- Primary Care: Virginia Garcia, Multnomah County, etc.
- Niche: Sports Medicine, Pre-op, Dermatology, Pain, etc.
-
Social Medicine
The Social Medicine block is a core three-week rotation during intern year that blends clinical and non-clinical experiences focused on the care of vulnerable populations. The rotation is designed to expand residents' sociocultural awareness and understanding of how social and structural determinants of health shape health outcomes, and to recognize their capacity to make a meaningful impact. It also offers an opportunity to step "off the hill" and engage directly with the Portland community.
During the rotation, interns spend time at Central City Concern, Hooper Detox Center, and the student-run Bridges Clinic, and participate in home-based primary care visits through the VA, as well as community-based volunteer experiences. The rotation includes mentored time to develop a community-based advocacy project, along with asynchronous learning modules covering addiction management and buprenorphine training, implicit bias and systemic racism, and reflective practice on the health impacts of poverty.
Kaiser Permanente

Residents spend two months at Kaiser during their second year and often additional time during third year. The rotation is an opportunity to experience both primary care and ambulatory specialty care in a large non-government integrated HMO setting. Residents are given increasing levels of autonomy in management of outpatient cases and enjoy continuity with a small group of preceptors. Residents can express a preferences in their subspecialty experiences, and a week in the urgent care clinic provides further opportunity for procedures like suturing and injections as well as management of acute injuries. Third-year residents are also given an option for a two-week hospitalist rotation. The rotation includes a health science curriculum as well as didactics covering core ambulatory topics.
Subspecialty Consults
Between OHSU and Portland VAMC, we offer consult rotations in all of the IM subspecialties. Over the course of 3 years, residents will rotate on almost all of them, with assignments based on resident preferences. Consult rotations take place during the X-block, so residents do not have concurrent continuity clinic. Rotations are one to three weeks in duration. When scheduled for two or more weeks, you may be asked to work one weekend.
Neurology
A two-week inpatient rotation at OHSU during PGY-1. Typically consists of one-week on the stroke service and one-week on the consult service working alongside neurology residents and with supervision by neurology faculty.
Geriatrics
In addition to geriatrics clinics in the +1 week during PGY-1, interns also have a two-week geriatrics rotation at OHSU, which includes time spent at one of two local skilled nursing/long-term care facilities. Interns learn principles of geriatric medicine and common geriatric syndromes, models of geriatric care including rehabilitation and nursing home structures, transitions of care, and interprofessional team care.
Miscellaneous Rotations
- VA Addiction Medicine (PGY-1)
- VA Pre-Anesthesia Testing clinic (PGY-1)
- VA Ambulatory Subspecialty clinics (PGY-2 and/or PGY-3)
Electives
Residents receive a total of eight weeks of electives throughout training, including a two-week block and a three-week block during PGY-2, and a three-week block during PGY-3. We offer a diverse array of clinical and non-clinical options. We offer a variety of global health rotations locally, regionally, and internationally (see Tracks & Pathways). Many residents choose to use some of their elective time to pursue research activities.
-
Our comprehensive curriculum is designed not only to prepare graduates for independent practice, but also to confidently pass the American Board of Internal Medicine (ABIM) Certifying Examination. Graduates of our program have been highly successful at passing boards on their first attempt. Our most recent three-year rolling pass rate is 94%. We attribute this success in large part to the quality of our residents, who are exceptionally bright and intellectually curious, but also credit the strength of their training experience. Our curriculum is intentionally designed using a purposeful, data-driven approach to deliver high-quality instruction and comprehensively target all content areas tested on the ABIM examination. All residents receive individualized feedback based on annual In-Training Exam results. Curricular oversight is provided by a Residency Curriculum Committee (RCC), which continually modifies the curriculum in response to ITE performance and other metrics.
Inpatient Conferences
Residents on inpatient rotations attend the following didactics:
- All wards: Noon report, Intern report, Noon conference
- OHSU wards: Radiology rounds, SPARK (QI) rounds, POCUS rounds
- VA wards: ECG rounds, Mock codes
- MICU: ICU wellness rounds
Noon Report / Intern Report
Noon report is a resident-presented, chief-facilitated conference held on Mondays and Fridays for one hour, with an emphasis on clinical reasoning, problem solving, and evidence-based medicine. Generalist and subspecialty faculty regularly participate. On Fridays, we also have a separate Intern Report, where PGY-1s can work on developing core competencies and clinical reasoning skills in a low-stakes environment.Noon Conferences
Noon conferences serve as the primary forum for our core internal medicine curriculum, which follows an 18-month repeating cycle. Conferences are held on Tuesdays, Wednesdays, and Thursdays. Key core concepts are reinforced during the first two months of each academic year. Additional content areas include fellowship advising sessions and Fireside Chats with program leadership.Educational Seminars
During the +1 week, all residents attend half-day educational seminars on Tuesday mornings and Friday afternoons. Interns have an additional half-day seminar on Wednesday mornings. Didactics consist of the following:
- Ambulatory Report
- Department of Medicine Grand Rounds
- Evidence-Based Medicine
- Practice Based Learning & Improvement
- Primary Care Ambulatory Topics
- Advocacy (interns only)
- Teaching Improvement Science (interns only)
Primary Care Ambulatory Topics (PCAT)
A three-year curriculum on high-yield outpatient general internal medicine topics taught through innovative and engaging methods.Practice Based Learning & Improvement (PBLI)
Designed to help residents develop mastery in the management of a portfolio of important chronic illnesses in primary care. Faculty facilitators provide up-to-date guideline recommendations and review relevant clinic resources.Ambulatory Report
An informational conference where residents share cases that have piqued their curiosity, taught them new clinical skills, led to exciting outcomes, or remain puzzling.Ambulatory Editorial Board - Resident Steering Committee
Residents participate as active members in ambulatory curricular development and continuous process improvement.Advocacy Curriculum
We believe that to truly promote health in our communities, we must address the root causes of illness. Many of our residents are drawn to medicine because of their commitments to human welfare and social justice. The consequences of social determinants like systemic racism, housing insecurity, hunger, and poor access to healthcare are all around us. Advocacy can offer solutions where clinical medicine falls short. To read more about our novel advocacy curriculum, click here.Teaching Improvement Science (TIS) Curriculum
The TIS curriculum provides innovative instruction in Health Systems Science for our residents. Developed at OHSU, this curriculum is now sponsored by the American Medical Association and disseminated nationally as a model for comprehensive and forward-thinking education in Health Systems Science. TIS covers the full spectrum of Health Systems Science, grounded in the principle that improving our systems promotes well-being. Interns develop a deeper understanding of how health systems affect both patient care and the professional experience of clinicians, fostering the development of engaged, fulfilled physicians who are equipped to serve as agents of change in creating a safer, more equitable health care system. To read more about our TIS curriculum, click here.Point-of-Care Ultrasound (POCUS) Curriculum
"Tell me, I forgot; show me, I remember; involve me, I understand."
Point-of-Care Ultrasound (POCUS) is a patient-centered, powerful tool to aid diagnostic evaluation, sharpen clinical decision-making, monitor therapies, guide procedures, and reinforce patient understanding. OHSU IM faculty and residents have been at the forefront of advancing POCUS through research, innovation, and national leadership in education. OHSU is one of the few institutions offering a dedicated fellowship in general medicine POCUS after residency, giving our residents exceptional access to diverse learning and mentorship opportunities. Our cutting-edge clinical POCUS workflow allows residents to save images, receive feedback from an attending, and add documentation and images to the patient chart. This supports residents in creating a portfolio of images throughout residents, which is valuable for both career development and patient care. The following represents the core POCUS curriculum that all residents receive during training:- POCUS Workshop: All interns participate in two half-day workshops during intern intensive covering basic cardiopulmonary and abdominal ultrasound. These sessions combine didactics with hands-on scanning of standardized patients in a low-stakes, interactive environment. Faculty-led case-based discussions illustrate how POCUS can guide the care of common problems, such as acute kidney injury and hypotension - building a strong foundation for clinical application.
- Friday POCUS Rounds: Residents on OHSU Wards rotations gather every Friday morning with a POCUS expert to review images they acquired on their own patients. These sessions focus on image optimization, interpretation, clinical integration, and evidence review. This innovative format fosters longitudinal learning and spaced repetition in a real-world clinical environment.
POCUS Elective
Residents seeking more extensive training may also choose to do a one-,two-, or three-week individualized POCUS elective. This includes practice on a state-of-the-art cardiopulmonary simulator, bedside practice with faculty and IM ultrasound fellows, and participation in weekly conferences, with options for specialized experiences such as ICU scanning, shadowing echocardiographers, or sessions in a musculoskeletal clinic. -

We are deeply committed to fostering research and scholarship in all its forms. Engagement in scholarly activity during training offers substantial benefits, including professional development, skill acquisition, mentorship, and preparation for fellowship applications and future careers. For these reasons, we believe that exposure to scholarship is an essential component of every resident's training.
Scholarship Requirements
Prior to graduation, residents must complete a minimum of two qualifying scholarly activities: either one from Column A and one from Column B, or two from Column A: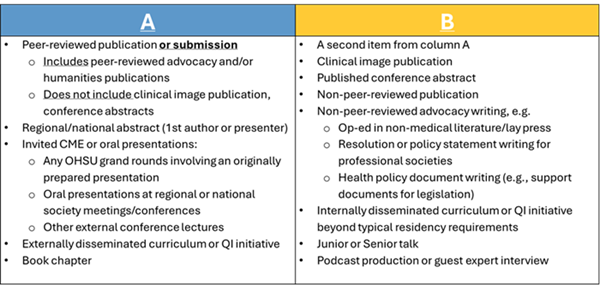
-
Overview
Our program offers both formal and informal mentorship, advising, and coaching. Each residents meets twice yearly with their linked Associate Program Director to review performance and receive guidance on professional development and career planning. With support from our Associate Program Director for Research and Assistant Program Director for Subspecialty Medicine, we are intentional and proactive about connecting residents with subspecialty research and career mentors early in training. Residents also frequently identify mentors independently, as OHSU faculty are warm, approachable, and deeply invested in resident success.
CLEAR Coaching
All residents participate in Coaching for Life-Long Learning (CLEAR), which provides a confidential, non-evaluative space to reflect on their experiences alongside a dedicated faculty coach. CLEAR is modeled after a program developed at MGH that has been shown to reduce resident burnout and has been adopted by residency programs nationwide. Each incoming resident is paired with a faculty coach who remains with them throughout all three years of training, meeting four times per academic year. Using a positive-psychology coaching approach, faculty coaches help residents to reflect on achievements and challenges, identify opportunities for growth, and develop actionable, individualized goals.
Big Sib/Lil Sib
We offer a Big Sib/Lil Sib program that pairs incoming interns with second-year residents based on shared interests, including career goals, family life, and hobbies. This initiative was developed by our residents to reduce isolation, normalize feelings of burnout and self-doubt, and promote wellness. Big Sib/Lil Sib pairs meet during orientation, with protected time for quarterly meet-ups built directly into the noon conference curriculum.
-
Overview

Wellness is a core priority of our program. Our philosophy is that self-care is essential to being your best self. We offer a number of resources to support resident wellbeing:
- Rotations are scheduled a full year in advance to facilitate time-off planning
- Schedules are created with an emphasis on residents' personal and professional needs
- A minimum five full days off per month
- Four health-maintenance half-days per year to address personal healthcare needs
- An IM Residency Council that leads initiatives to improve wellbeing, community, and sense of belonging
- Continuous efforts to improve the system in which residents work to optimize wellbeing, continuity of care, and overall educational experience
Resident and Faculty Wellness Program
The OHSU Resident and Faculty Wellness Program (RFWP) was established in 2024 to promote clinician wellness, reduce burnout and distress, and support personal and professional thriving. The RFWP offers free, completely confidential counseling, coaching, and psychiatric services. Visits are not documented in the electronic health record to ensure privacy. Appointments are conducted virtually for ease of scheduling, and our program is highly supportive of residents stepping away from rotations to attend. We normalize seeking help, and our residents and faculty regularly make use of these services.
-
We are deeply committed to diversity, equity, inclusion, and belonging. We acknowledge the longstanding and pervasive harm cause by bias and systemic racism to marginalized and minoritized communities. We will continue to work as a program, department, and institution to dismantle inequalities and to promote justice and anti-racism.
Institution-wide Programs and Initiatives
- Diversity, equity, inclusion, and belonging are foundational to the mission of our institution and essential to the success of all that we do.
- A variety of Employee Resource Groups are available for faculty and staff from underrepresented backgrouds
- The OHSU Health Equity Organization works to advance how we deliver health care effectively and equitably
- The School of Medicine (SOM) Diversity, Equity, Inclusion, and Belonging Action Plan charts how the SOM contributes to institutional aims
- We proudly support gender-diverse and gender-nonconforming communities, and OHSU is a leader in transgender health and gender-affirming care
- Oregon is the state most protective of abortion rights in the country, and OHSU is committed to safeguarding reproductive health care for all
- The Northwest Native American Center for Excellence (NNACoE) at OHSU works to sustainably address the health care needs of all people by increasing the number of American Indians and Alaska Natives (AI/ANs) in the health professions workforce
- The Office of Civil Rights Investigations and Compliance (OCIC) oversees policies related to protected characteristics; reviews and investigates reports of violations; and provides education, training, and other resources, as well as confidential advocacy for employees regarding bias, discrimination, harassment, retaliation, and interpersonal violence.
Department of Medicine Initiatives
- The Department of Medicine Justice, Equity, and Belonging (JEB) Collaborative, led by our Vice Chair for JEB, strives to cultivate an environment where belonging is integral to our work.
Residency Program Initiatives
- Aim to integrate principles of equity and social/structural determinants of health into all that we do
- Created a novel Associate Program Director role that focuses specifically on advancing Health Equity and Community Engagement in our program
- Utilize a holistic approach to recruiting a diverse group of residents
- Participate in University and GME led efforts to end racism at OHSU
- Support community organizations who work to dismantle racism, including longstanding partnership with the NxNE Community Health Center