Glossary
The basics to understanding diabetes
Type 1 diabetes
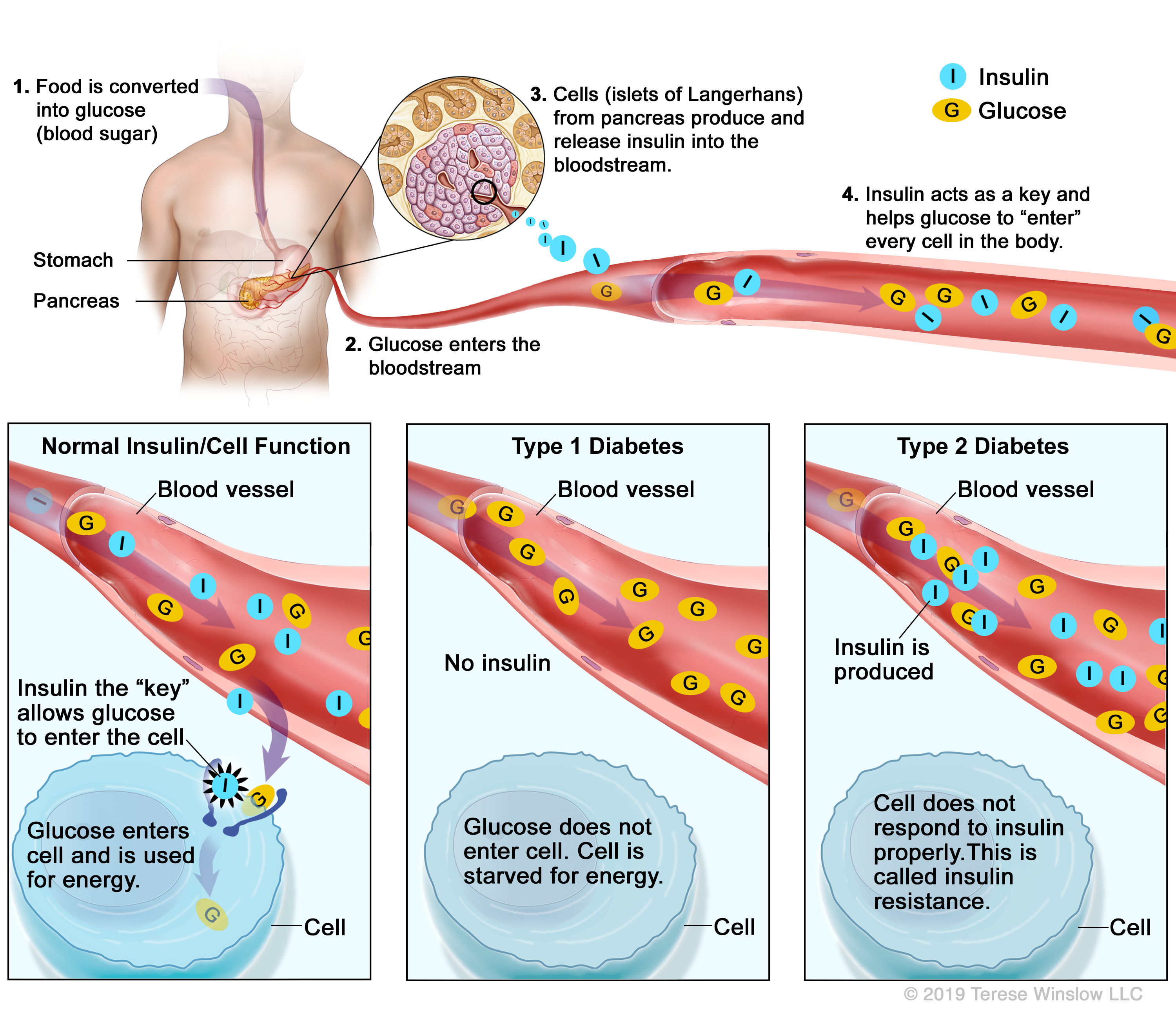
Type 1 diabetes occurs when the pancreas, the organ that produces the hormone called insulin, loses its ability to make insulin. Similar to a fuel pump in a car, insulin moves fuel from the food we eat into our cells for energy. The food is moved in the form of glucose, a type of sugar.
Doctors believe type 1 diabetes is caused by an immune system reaction that destroys insulin-producing cells in the pancreas. If you develop type 1 diabetes, glucose builds up in your blood because you do not have enough insulin to move it into your cells. If you do not get insulin from a source outside your body, like an injection, the glucose in your blood will cause a coma and possibly even death. This is why people with type 1 diabetes need to take insulin.
Around 5 to 10 percent of people with diabetes have type 1 diabetes. Half of people with type 1 diabetes are diagnosed with it before age 20. Type 1 diabetes used to be called juvenile diabetes or insulin dependent diabetes.
Type 2 diabetes
In type 2 diabetes, your body still makes insulin, but the cells that need glucose from the blood do not pick up the insulin as well as they used to. At first, the body tries to make up for this by producing extra insulin. After a while, your pancreas cannot make enough extra insulin to keep your blood sugar at a normal level, and you end up with too much sugar circulating in your blood.
Doctors think type 2 diabetes is caused by a combination of genetics (runs in families) and/or an unhealthy lifestyle. If you have family members with diabetes, and you are overweight and do not get much exercise, you have more risk of type 2 diabetes.
The treatment for type 2 diabetes is healthy eating, regular exercise and often diabetes pills. Type 2 diabetes is progressive over time. Some people with type 2 diabetes may need treatment with diabetes pills and/or insulin.
Ninety to 95 percent of people with diabetes have type 2. Type 2 diabetes used to be called adult onset diabetes or non-insulin dependent diabetes.
Prediabetes
Prediabetes is the condition of having blood sugar that is higher than normal. If you have pre-diabetes, your blood sugar (blood glucose) level is not high enough for diabetes, but not low enough to be normal.
Treatment for prediabetes includes:
- Moderate weight loss if you are overweight (weight loss of about 7 percent of your current weight)
- Eating a healthy, low-fat diet that includes lots of vegetables
- Getting at least 30 minutes of moderate exercise, like brisk walking, five days a week.
Gestational diabetes
Gestational diabetes is high blood sugar in pregnancy. This is caused by some of the hormones in the body during pregnancy. If it is not diagnosed or treated, it can cause birth defects.
The treatment for gestational diabetes is a healthy diet and physical activity. If diet and exercise do not work to control your blood sugar, your doctor may have you take diabetes pills or insulin. A woman who has gestational diabetes has more risk for type 2 diabetes later in life.
Preventing type 2 diabetes
A research study called the Diabetes Prevention Program was published in 2002. In this study, about 3000 overweight people with prediabetes were put in three groups.
The three groups had three different treatments:
- A placebo medication (no treatment)
- A diabetes medication called metformin
- A healthy, low-fat diet and 30 minutes of exercise, five days a week to achieve a weight loss of about 7% of current body weight
People in the placebo group had no change in their risk of getting diabetes. People who took metformin had a 31% lower risk of diabetes. The people who ate a healthy diet and exercised lowered their risk of diabetes the most, by 58%. Researchers stopped the study early because the people in the diet and exercise group did so much better.
This tells us that you can lower your risk of type 2 diabetes by losing about 7 percent of your body weight if you are overweight, eating a lower-calorie, low-fat diet and getting 30 minutes of exercise, five days a week.
Blood glucose testing and blood sugar goals
Keeping track of your blood sugar or glucose at home is done by placing a small drop of blood on a test strip in a blood glucose meter. The meter will show your blood glucose (blood sugar) level. Testing your blood sugar regularly will give you important information about your blood sugar control.
Other reasons to test your blood sugar include:
-
To learn how certain foods, activities, stress and other situations affect your blood sugar. Knowing this will help you find ways to control glucose levels and adjust your diet, medication and exercise if you need to.
-
To learn whether your blood sugar is too low (hypoglycemia) or too high (hyperglycemia). You might need additional treatment if this happens. To see how changes in your diet, medication or exercise routine affect your blood glucose.
-
Research shows that people who monitor their blood glucose levels regularly have lower blood sugar most of the time. This can lower your risk of having complications (problems) with diabetes.
Some people with diabetes test their blood sugar (blood glucose) up to seven times a day. Other people only test their blood sugar two or three times a week. Your doctor or diabetes educator will tell you how often to test your blood sugar.
American Diabetes Association goals for blood glucose*
- Fasting or before meals blood glucose range: 80 - 130 mg/dL
- 2 hours after start of meal: less than 180 mg/dL
*Your doctor may want you to follow blood glucose (blood sugar) goals that are different from the American Diabetes Association goals due to a number of factors. Be sure to discuss related questions to your goals with your doctor.
A1C blood test
The A1C blood test shows your blood glucose (blood sugar) level over three months. As red blood cells circulate in your body, glucose molecules stick to them. Since red blood cells circulate for about three months, the A1C test can tell how much glucose has been in your blood during that time. The A1C test is also called the hemoglobin A1C, HbA1c, glycated hemoglobin, or glycohemoglobin test.
Research shows that people with an A1C level of 7.0 percent or lower have less risk of having complications (problems) caused by diabetes.
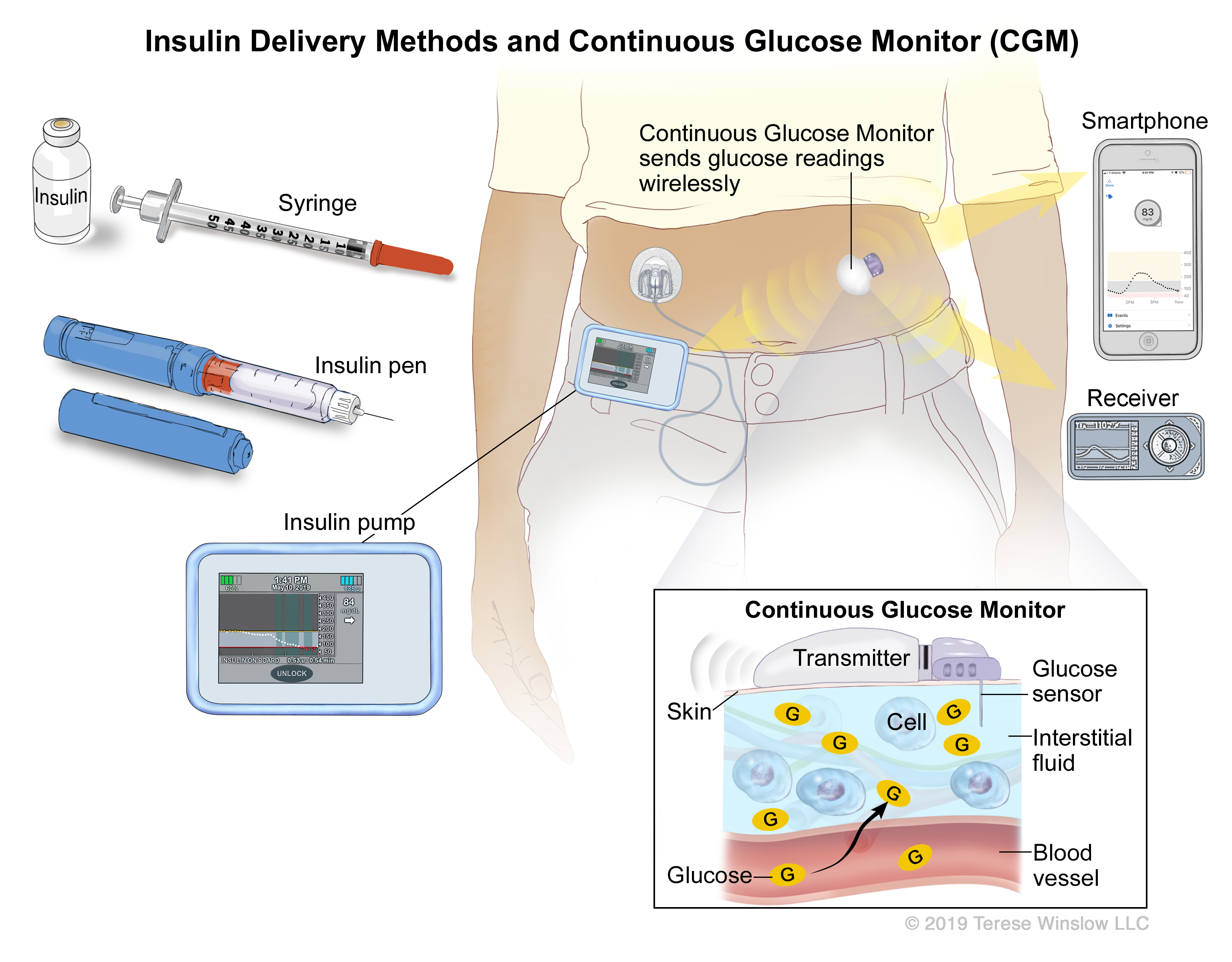
Insulin pumps and other insulin delivery options
An insulin pump is one of several insulin delivery options available to children and adults living with diabetes. Many people may switch between the following insulin delivery options over time:
- Injections
- Smart pen
- Insulin pump
- Inhalable insulin
The insulin delivery option you use depends on a number of factors such as activity levels, cost, preference, health insurance and several other reasons. Your diabetes care team can discuss the pros and cons of each option with you. It’s also important to note that any of these options can be combined with a CGM (continuous glucose monitoring) that can further assist you in reaching your blood sugar target or time-in-range goal.
An insulin pump user typically administers an insulin bolus during a mealtime or snack. The pump itself works to regularly deliver a basal or continuous delivery of insulin that is programmed by the pump user or caregiver. Both bolus and basal insulin is delivered via a cannula (see illustration).
Pumps require special training to ensure that a patient living with diabetes can use them safely and effectively because of this, your diabetes doctor or endocrinologist must authorize its use.
An insulin pump does not automatically give you insulin or control your blood sugar levels (a common misconception or misunderstanding about a pump acting as a pancreas). It is important to know that insulin pumps give you insulin, based on how you program them. A true artificial pancreas or closed-loop system does not exist at this time, researchers are working to develop fully automated artificial pancreas systems.