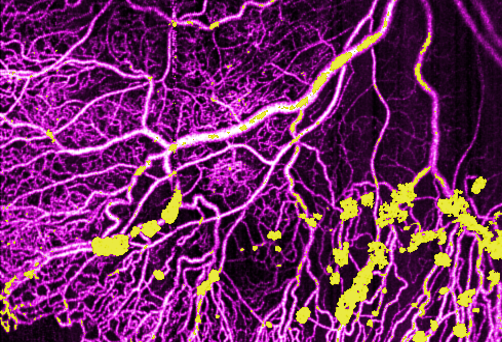
Groundbreaking work in ultrawide-field represents next evolution of optical coherence tomography
OHSU Casey Eye Institute is a leader in noninvasive imaging technology to detect vascular changes in the eye, an underlying pathology of several eye diseases that can lead to blindness. A world-recognized leader in optical coherence tomography (OCT) structural and angiographic imaging, David Huang, M.D., Ph.D., runs the Center for Ophthalmic Optics and Lasers, or COOL Lab, at OHSU
Casey Eye Institute. With his team, Huang is currently pioneering new applications of this extraordinary technology.
“In our original prototype, we were getting 40 axial scans, or image lines, per second,” said Huang, who co-invented the technology in 1991. “Current OCT systems get hundreds of thousands of axial scans per second, making it feasible to image wide areas of the retina with ultrawidefield OCT systems. Several of our faculty are working on different applications. It’s exciting because a lot of pathologies happen in the periphery of the eyes. This area of research represents an open canvas for designing innovative technology to improve clinical practices and standards.”
Developing AI in diabetic retinopathy
Yali Jia, Ph.D., transformed OCT angiography (OCTA) by developing split-spectrum amplitude decorrelation angiography (SSADA), a highly efficient algorithm that made clinical OCTA feasible. Jia remains at the forefront of OCTA imaging research in retinal diseases. She’s now developing an algorithm to provide fast, automatic and reliable biomarkers for diabetic retinopathy progression using ultrawide-field OCTA, a noninvasive method to detect capillary dropout and neovascularization.
“Dr. Jia’s work is the most important recent advance for the evaluation of diabetic retinopathy, one of the top three blinding diseases,” Huang said.
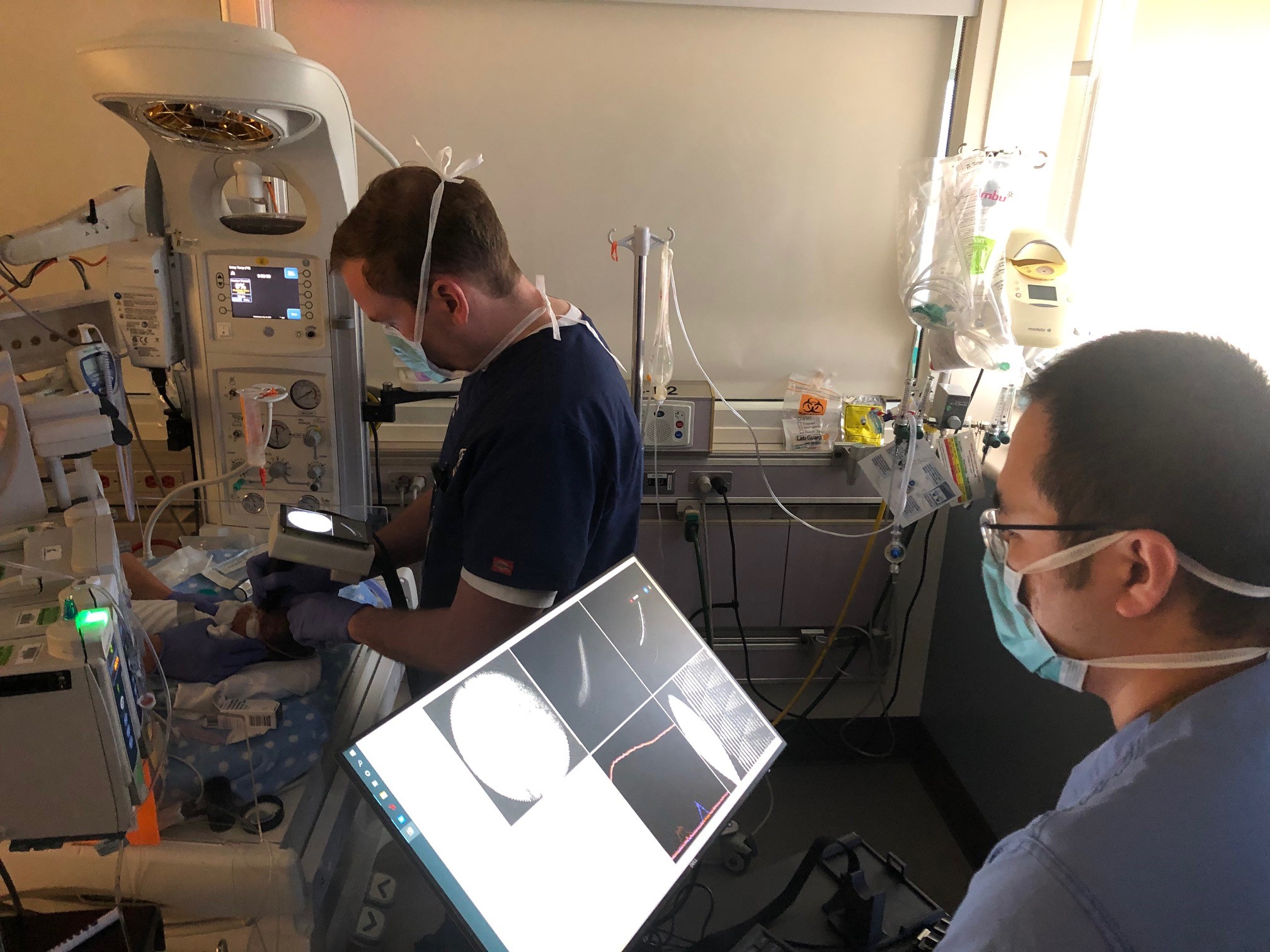
Inventing a handheld device for retinopathy of prematurity and retinoblastoma
Yifan Jian, Ph.D., has developed a portable ultrawide-field OCT/OCTA prototype that J. Peter Campbell, M.D., M.P.H., is using in the neonatal intensive care unit to examine infants for retinopathy of prematurity (ROP). The handheld device can obtain a 105° OCT or a 55° OCTA in just 1.5 seconds. This is ideal for detecting retinal neovascularization in the periphery. This noninvasive method provides rapid real-time data for disease screening in a population at risk for blindness. Alison Skalet, M.D., an ocular oncologist at Casey Eye Institute, is using this ultrawide-field OCT system to evaluate the extent of ocular tumors and their response to treatment. The portable system is particularly useful in retinoblastoma, an eye cancer of childhood that can be fatal if not treated in time. Though developing this technology for pediatric patients, it may also translate to adults.
Pioneering new methods for scleral lens fitting
With more than 20 years of research together using OCT for the anterior of the eye, Huang and research assistant professor Yan Li, Ph.D., are now using an ultrahigh-speed/ultrawide-field OCT for corneoscleral topography. The prototype can scan 22 mm wide and 10 mm deep, covering the whole anterior eye. Their purpose is to improve scleral lens fittings
for people with irregular ocular surfaces. “We want to be able to map an individual’s eye shape and provide a custom design for each eye, like a tailored suit that fits precisely for comfort and quality of vision.” Huang said.
“Current OCT systems get hundreds of thousands of axial scans per second, making it feasible to image wide areas of the retina with ultrawide-field OCT systems. Several of our faculty are working on different applications. It’s exciting because a lot of pathologies happen in the periphery of the eyes. This area of research represents an open canvas for designing innovative technology to improve clinical practices and standards.”
David Huang, M.D., Ph.D.