Current Projects
Our lab specializes in a range of techniques, utilizing the strengths of both in vivo mouse models and in vitro cell culture experiments to discover more about a few very important proteins found in the human kidney.
K+ and blood pressure
How potassium prevents hypertension
Hypertension is the most common and morbid disease in the world, with an incidence projected to rise substantially in the next generation. While there has been a great deal of focus on the role that dietary salt (NaCl) plays in this rise, dietary potassium intake has received much less attention, at least until recently. The Ellison laboratory is a site in a new LeDucq Foundation Translatlantic Network of Excellence. Together with 5 sites in Switzerland, Denmark and the USA, we are using novel mouse models to explore what we have termed a ‘potassium switch’ in the kidney. This switch appears to act by ‘sensing’ the blood potassium concentration and translating this signal to both activate transport proteins and also to cause kidney remodeling. We use highly specific antibodies, developed in our own laboratory, coupled with tissue clearing approaches, such as Clarity®, to determine how dietary interventions alter the structure of kidney tubules, and how those changes, lead to high or low blood pressure.
Supported by a 5-year grant from Foundation LeDucq. Of note, this grant provides support for trainees to spend time in any of the participating labs in Baltimore, Nashville, Lausanne, Aarhus, or Brisbane to learn techniques.
How kidneys sense K+
How the kidney senses potassium
This is a related project designed to determine the mechanism by which kidney distal tubules ‘sense’ the blood potassium concentration. Working with Wen-Hui Wang at Medical College of New York, we have determined that potassium is sensed by the action of potassium channels (Kir4.1) in the basolateral membrane of the distal tubule. Naturally occurring mutations of these channels cause the human disease, EAST syndrome. We have postulated that these channels determine the membrane voltage, which in turn, affects the cell chloride concentration. It is known that chloride affects the activity of a unique class of serine/threonine kinases, called WNK kinases. When cell chloride concentration is low, the kinases are activated, thereby switching NaCl transporters from the off state to the on state. We are currently focusing efforts on measuring the chloride concentration inside of living distal tubule cells.
Supported by a Multiple PI grant (Wang and Ellison) from NIDDK, R01DK054983.
Genetic hypertension
How gene mutations cause hypertension
The cause of most hypertension (also known as high blood pressure) is unknown. Yet there are some cases caused by mutations in single genes. One of the most interesting is called familial hyperkalemic hypertension or Gordon syndrome. Mutations in four genes have been shown to cause this disease, and they all do so by activating salt transporters in the kidney tubules. The identification of these genes has unraveled a kinase network that was previously unknown, and in addition to affecting blood pressure, has effects on nerve transmission and on cell stability. These genes are called WNK kinases, and they act by phosphorylating and activating other kinases. Interestingly, other genes that cause the same disease phenotype are members of the cullin ring ligase family, which is involved in degrading WNK kinases. We are studying how mutations in these genes lead to hypertension, by developing novel mouse knock-in and knock-out models, and by studying cell culture model systems. The hope is that unraveling this new pathway will lead to new and more effective drugs to treat hypertension in people.
Supported by a Multiple PI grant (Ellison & Yang, with Gamba and Hadchouel) from NIDDK, R01DK051496.
Aldosterone control
How aldosterone damages the heart and kidney
Aldosterone is a potent salt retaining hormone, which plays key roles in the pathogenesis of hypertension, as well as heart failure and liver cirrhosis. Blocking the actions of aldosterone with drugs prolongs life in patients with heart failure. We recently discovered that the effects of aldosterone to promote salt retention in the kidney are different from what was long believed. Many groups, including our own, had believed that aldosterone activated both sodium channels and sodium chloride transporters in the kidney. We developed a novel mouse model and showed, instead, that aldosterone’s direct effects were only on sodium channels. Surprisingly, the effects on sodium chloride transport resulted from changes in blood potassium; they were not direct. We are now investigating how aldosterone stimulates sodium channels. While this has been a ‘holy grail’ for many years, the advent of new technology, such as RNAseq, is permitting us to explore the transcripts induced by aldosterone in more detail. Additionally, it seems that the effects of depleting aldosterone, which acts by binding to mineralocorticoid receptors, are not the same as those of depleting mineralocorticoid receptors. We postulated that this is because another steroid hormone, cortisol, stimulates mineralocorticoid receptors in vivo. We are using other unique mouse models to test this hypothesis.
Supported by a grant (Ellison) from Department of Veterans Affairs, I0BX002228.
Posters
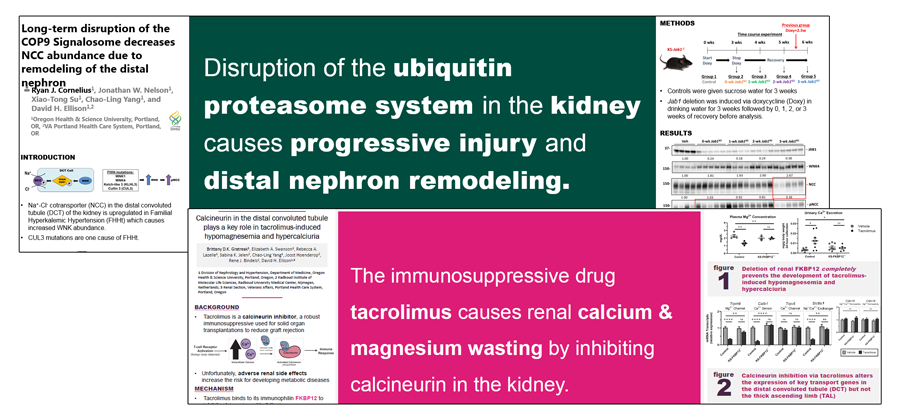
As part of our commitment to ensuring reproducibility of our research, posters made by our lab members are on display on the open-access research output repository, zenodo.org, after they have been presented at conferences. This allows us to keep the dialogue open for our current research. Please visit our community page on zenodo.org to browse our most recent posters.