Preclinical Research
Preclinical research projects
Dr. Neuwelt’s research interests have centered around the blood-brain barrier (BBB) and brain tumor therapy. In his initial VA Merit Review grant in 1978, Dr. Neuwelt predicted that manipulation of the BBB with transient osmotic shrinkage had the potential for a therapeutic role in brain tumor therapy. This hypothesis has been verified (Kraemer 2001), and the BBB disruption technique is now central to the preclinical and clinical research studies in the Neuwelt laboratory. Overall, Dr. Neuwelt’s research interests have centered around improving brain tumor therapy, reducing chemotherapy side effects, and improving brain tumor imaging. Dr. Neuwelt currently has a VA Merit review grant, three NIH research grants, an R13 NIH meeting grant, and is a member of a DOD breast cancer Center of Excellence.
Cancers in the brain are difficult to treat because of neurotoxicity, tumor resistance, and minimal delivery of potential therapies across the blood-brain barrier. We do basic science and preclinical studies of new approaches to delivery, treatment, and imaging in primary and metastatic brain tumor models.
Improving Brain Tumor Therapy
Chemotherapy has been relatively ineffective for the treatment of brain tumors in part because the blood-brain barrier (BBB) and blood-tumor barrier (BTB) limit agent delivery and therefore dose intensity at the tumor. We hypothesize that increased dose intensity may be achieved by increasing drug activity using chemo-enhancers, decreasing non-specific drug cytotoxicity using chemoprotective agents that do not cross the BBB, and increasing chemotherapy delivery to brain tumor with osmotic BBB disruption (BBBD). Preclinical brain tumor models include: CNS lymphoma (human MC116 B-lymphoma cells); lung cancer brain metastases (LX-1 human SCLC cells); breast cancer brain metastases (MDA-MB-231BR breast carcinoma cells that express high or low levels of the HER2 oncogene); medulloblastoma, both intracerebral and leptomeningeal (human DAOY medulloblastoma cells); and glioma (U87MG cells, UW28 cells, U251 cells).
Preclinical studies of osmotic BBBD
Intra-arterial drug administration into the carotid or vertebral arteries can improve drug delivery to rat brain tumors by ten-fold. Osmotic BBBD can increase delivery by ten-fold, and the combination IA/BBBD results in up to a 100-fold increase in tumor concentrations of chemotherapeutic agents (Barnett 1995; Neuwelt 1998). Vascular permeability to small chemotherapeutics is increased maximally by 15 minutes after infusion of mannitol, after which permeability decreases rapidly and returns to pre-infusion levels within two hours in animal models. Current studies with BBBD include enhanced chemotherapy delivery in glioma models, and radioimmunotherapy in the CNS lymphoma model.
Preclinical studies with Avastin
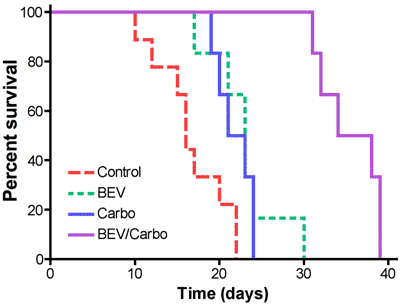
Avastin (bevacizumab) is a monoclonal antibody (mAb) which binds to VEGF (vascular endothelial growth factor). It blocks the formation of new blood vessels in tumors, but also affects existing vasculature. Avastin reduces brain tumor edema, “normalizes” tumor blood vessels, and improves chemotherapy antitumor efficacy, but its effects on drug delivery and the mechanisms of its anti-tumor effect remain unclear.
We recently evaluated the efficacy of IV Avastin and/or carboplatin in a human glioma animal model. Carboplatin plus Avastin was effective and superior over bevacizumab or carboplatin monotherapy (Figure 1). Median overall survival was: 1) controls, 16 days; 2) Avastin, 23 days; 3) carboplatin, 22 days; 4) Avastin plus carboplatin, 36 days. Survival with the combination therapy was significantly longer than untreated control (p = 0.0011), Avastin alone (p = 0.0014) and carboplatin alone (p = 0.0015).
Current therapy studies with Avastin include combination with chemotherapy +/- BBBD in glioma, and combination therapy approaches in other brain tumor models.
Chemo-enhancement
Further dose intensification may be achieved by enhancing the activity of chemotherapeutics or increasing the susceptibility of the tumor cells to chemotherapy toxicity. The endogenous thiol glutathione detoxifies toxic agents, including chemotherapy, so we have investigated mechanisms to deplete glutathione concentrations as a mechanism to increase chemotherapy activity. We are investigating the use of buthionine sulfoximine (BSO), a glutathione synthesis inhibitor, and acetaminophen (Tylenol), which depletes glutathione in some cells including tumor cells. We are currently evaluating these agents for chemo-enhancement in several brain tumor models.
Antibody-based therapies
The BBB has very low permeability to large biomolecules such as antibodies. One approach to improve mAb efficacy is the use of chemotherapy immunoconjugates or radioimmunoconjugates directed to tumor antigens. We have shown that BBBD delivery improves the efficacy of a tumor specific mAb bound to doxorubicin chemotherapy (BR96-DOX, Neuwelt 2003; Remsen 2000), and this targeted cytotoxicity can be enhanced with radiotherapy (Remsen 2001). Current mAb studies are evaluating a Herceptin-auristatin immunoconjugate from Genentech, testing an yttrium-90 radioimmunoconjugate in the CNS lymphoma model, and assessing the importance of route of delivery of antibody-based therapeutics.
Reducing chemotherapy side effects
Increasing chemotherapy dose intensity can be a problem due to the toxic side effects of chemotherapy such as ototoxicity, mucositis, nephrotoxicity, and bone marrow toxicity. We are investigating the use of thiol chemoprotective agents to reduce these chemotherapy-induced side effects.
Preclinical chemoprotection studies
Delayed administration of sodium thiosulfate (STS) protects against carboplatin-induced ototoxicity and cochlear hair cell loss in guinea pigs (Neuwelt 1996) and blocks cisplatin-induced hearing loss in rats (Dickey 2005). The thiol N-acetylcysteine (NAC) reduced cisplatin-induced hearing loss, and also blocked nephrotoxicity and weight loss in normal rats (Dickey 2004). Route of administration was very important for NAC nephroprotection: oral NAC was not effective even at the highest dose (1200 mg/kg), while IV NAC was effective at 400 mg/kg and intra-arterial NAC was effective even at doses as low as 50 mg/kg (Dickey 2008). When NAC was administered via an “aortic infusion” technique to increase bone marrow perfusion in conjunction with chemotherapy in rats, the magnitude of chemotherapy-induced bone marrow toxicity was reduced, even with BSO chemo-enhancement (Neuwelt, 2001). Current studies are evaluating neuroprotection and protection against mucositis.
Effect of chemoprotection on efficacy
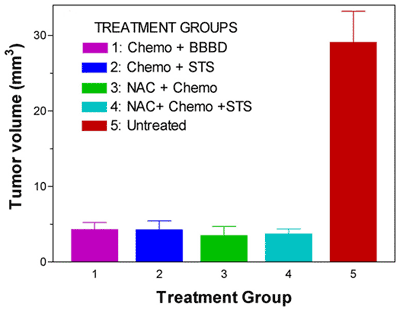
One impediment to clinical use of chemoprotective thiols is the potential to interfere with the anti-tumor activity of chemotherapy. We showed that an optimized chemoprotective regimen (pretreatment with NAC combined with delayed administration of STS) reduced hematological toxicity in the rat, but had no impact on BBBD-enhanced chemotherapy efficacy against rat intracerebral tumors (Neuwelt 2004; Figure 2). Negative interactions of thiols with anti-tumor efficacy were avoided by temporal and spatial separation of chemoprotectant and chemotherapy treatments by changing the route and timing of administration. Similar results were found in a subcutaneous neuroblastoma model (Harned 2008). Current studies are evaluating combination chemo-enhancement and chemoprotection strategies.
Improved brain tumor imaging
A major area of research in the Neuwelt preclinical labs involves new magnetic resonance (MR) imaging modalities to monitor brain tumor growth and anti-tumor efficacy, characterize tumor changes associated with gene activation, apoptosis, or necrosis, and evaluate delivery of therapeutic agents to brain and intracerebral tumors. The Advanced Imaging Research Center (AIRC), under the direction of Dr. Charlie Springer, has state-of-the-art imaging equipment, including one of the only 12 Tesla animal MRI scanners in the country.
Tumor imaging with iron oxide nanoparticles
Ultrasmall superparamagnetic iron oxide (USPIO) MR agents, such as Combidex (Ferumoxtran 10) and Ferumoxytol (Advanced Magnetics, Inc.) have a long plasma half-life coupled with uptake by phagocytic cells. We showed that the USPIO agents have no toxicity when injected in rat brain, and they can be detected for at least 3 months after injection into brain, but only 3-7 days after BBBD delivery (Muldoon 2005). The nanoparticles slowly leak across the BBB and blood-tumor barriers, and provide excellent brain tumor imaging from 2 h to 72 h after administration due to uptake by trapping in reactive cells in and around the tumor. Another nanoparticle agent, Feridex (ferumoxides) does not cross into the brain, but can be used to label cells in vitro and in vivo (Wu 2007). Iron-labeled cells act as a “cellular contrast agent” to allow imaging of inflammatory cell trafficking into the CNS.
Dynamic MRI
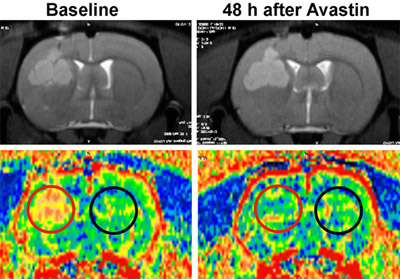
Use of the 12 T animal MRI scanner allows us to acquire serial rapid (2 second) scans of contrast agent traveling through CNS and tumor blood vessels. We evaluated the utility and reliability of dynamic susceptibility contrast (DSC) perfusion MRI and permeability, or dynamic contrast enhanced (DCE) measurements to assess tumor response to the antiangiogenic agent Avastin in comparison to glucocorticoid. We also investigated the potential of the USPIO ferumoxytol as a blood pool contrast agent for MR perfusion. Contrast extravasation was seen rapidly after gadolinium but not ferumoxytol administration. Significantly decreased BBB permeability to gadolinium was measured at all time points after Avastin and at 72h after high dose steroid. Avastin decreased the relative cerebral blood volume in tumor (Figure 3), and was more effective than steroid. Current studies involve perfusion, permeability, and angiography measurements in multiple tumor types treated with Avastin or other agents targeting the vasculature.
Disclosures
Dr. Muldoon, Oregon Health & Science University (OHSU), Portland Veterans Affairs Medical Center (PVAMC) and the Department of Veterans Affairs have a significant financial interest in Adherex, a company that may have a commercial interest in the results of this research and technology. This potential conflict of interest has been reviewed and managed by the OHSU Integrity Program Oversight Council and the PVAMC Conflict of Interest in Research Committee.