
Jennifer M. Loftis, Ph.D., Principal Investigator
Psychoneuroimmunology is the study of interactions between the immune and central nervous systems, and particularly how these interactions contribute to psychiatric function and health. The Psychoneuroimmunology (PNI) Research Lab led by Dr. Loftis is a “real time” translational research program that integrates human, animal, and in vitro experiments to examine how neuroimmune factors contribute to the neuropsychiatric effects of medical, psychiatric, and substance use disorders.
Support PNI research
Help advance research in cognitive impairment in methamphetamine use disorder.

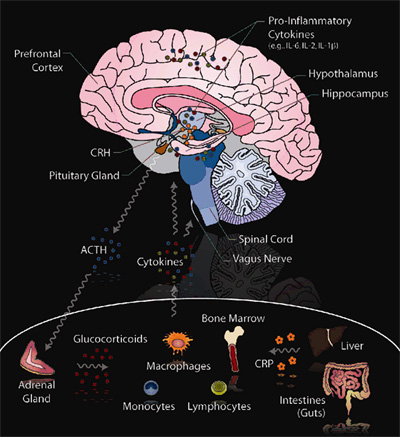
The Psychoneuroimmunology (PNI) Research Lab is led by Dr. Jennifer M. Loftis. Our long-term goal is an improved understanding of how the immune and central nervous systems interact to impact neuropsychiatric function. At high pathophysiological levels, immune factors such as cytokines, chemokines, and adhesion molecules regulate immune responses to pathogens and injury. However, immune factors are also required at low physiological levels for the regulation of synaptic plasticity, normal neuronal function, and therefore normal mood and cognition. Many conditions such as addiction and hepatitis C are associated with alterations in immune factor expression. The PNI Research Lab is interested in how these immune alterations then contribute to functional impairments—problems with cognition, depression, anxiety, and impulsivity. Within the delicate balance of these immune factors, there also exists significant potential for intervention. The PNI Research Lab, therefore, strives toward discovery, development, and testing of novel treatments for psychiatric and substance use disorders.