Pituitary Disorders: Diagnosis and Treatment

The specialists at the OHSU Pituitary Center will give you a precise diagnosis and a treatment plan for your exact needs.
You’ll find:
- An experienced team that cares for hundreds of patients a year, making sure each one gets the right treatment.
- A program led by Dr. Maria Fleseriu, an internationally recognized pituitary expert.
- Highly skilled neurosurgeons who offer the latest minimally invasive techniques.
- Precise radiation therapy that targets pituitary tumors while sparing healthy tissue.
- Expert second opinions, with most evaluations completed in one day.
- The latest diagnostic testing in our dedicated facility.
- Clinical trials that test new approaches to care. Our work in past trials helped lead to FDA approval of new medications for acromegaly and Cushing disease.
Complete care
Expert team: Our team members are highly trained in endocrinology, a branch of medicine that deals with hormones. We have a special focus on neuroendocrinology, or how the nervous system and endocrine system interact.
Team-based care: Your care plan may bring together specialists from across OHSU, such as:
- Neurosurgeons
- Ear, nose and throat (ENT) surgeons
- Neuro-ophthalmologists (experts in the vision and the nervous system)
- Neuropathologists (doctors who help diagnose disorders of the nervous system)
- Nurse practitioners who focus on caring for patients with pituitary disorders
- Physician assistants who specialize in neurosurgery
Fast evaluation: We work to get answers quickly. We provide all the services you need in one place. Our team typically completes your evaluation in one day, including:
- Seeing a neuroendocrinologist
- Meeting with a neurosurgeon
- Having tests, including to measure hormone levels and take brain images
- Consultations with other specialists as needed
Diagnosing pituitary disorders
Many pituitary disorders have symptoms that are slow to develop or that can be confused with those of other illnesses. At the OHSU Pituitary Center, our experts are highly experienced in pinpointing pituitary disorders. You can count on getting answers so you can be matched with an effective treatment plan.
Hormone tests
Accurately measuring your pituitary hormone levels helps us confirm a diagnosis. Tests may include:
Baseline hormone evaluation: We measure hormone levels in your body before treatment to provide a baseline. Tests may involve taking samples of blood, saliva and urine over the course of a day.
- Blood test: We test your blood to measure your hormone levels.
- Urine test: We take urine samples over 24 hours to measure levels of cortisol, a hormone produced by the adrenal gland.
- Saliva test: A late-night saliva test also measures the level of cortisol.
Dynamic tests: These tests either increase or suppress production of specific hormones to judge the body’s response. We typically measure your hormone levels, then give you medication or another solution by mouth or IV. Then we recheck the levels over a period of time.
Dynamic tests include:
- Glucose suppression test: You drink a glucose solution to suppress growth hormone production. If levels don’t fall, that indicates your body makes too much.
- Growth hormone stimulation tests: We give you a solution in a shot or drink to increase growth hormone production. If levels don’t rise to expected levels, that could indicate growth hormone deficiency.
- Dexamethasone suppression tests: We give you a medication or medications by mouth and/or shot to lower your cortisol production, then check cortisol levels in your blood. If levels stay high, results can help us diagnosis Cushing disease/syndrome.
Imaging
We use scans to diagnose pituitary tumors and to see how tumors affect the surrounding area. If you need surgery, these images help us plan a successful procedure.
Advanced MRI technology enables us to see pituitary changes in greater detail:
- Rapid dynamic gadolinium-enhanced pituitary imaging uses gadolinium, a material we inject to highlight areas of concern so we can detect tumors. This approach is effective in finding pituitary tumors in patients with Cushing disease.
- Our intraoperative MRI (iMRI) provides high-resolution images during surgery. Your surgeon may recommend this approach for an especially large or complex tumor. If so, real-time scans show us a tumor’s exact location.
- Our open MRI machines provide high-resolution images without requiring you to be in a traditional closed-in scanner. Our sophisticated scanner provides sharper images than those of most open MRI scanners.
Neuropathology
Pathology is the study of tissues to diagnose disease. Our highly trained neuropathologists specialize in diagnosing brain and nervous system conditions. We offer:
- High volume: Our neuropathologists analyze more than 1,000 tissue samples a year, giving them extensive expertise.
- Dedicated lab: Expert technicians process tissue for fast and precise results.
Neuropathology tests include:
- Molecular pathology, to look at cell structures within tissues.
- Cytogenetics, to look for changes in chromosomes (strands of DNA) that might indicate disease.
- Ultrastructural analysis, to look at cells in greater detail than with a regular microscope.

Pituitary disorder treatments
Medication
Pituitary disorders, including pituitary tumors, can throw your hormones out of balance. Medication can:
- Decrease hormone production and reduce symptoms.
- Replace hormones when your body doesn’t make enough.
We will work with you to find the best medication and dose to reduce your symptoms. Medication can improve how you feel, helping you go about daily activities. Some patients take medication after surgery or instead of surgery.
We have uncommon expertise with pituitary medications:
- Range of choices: Our team is familiar with all types of pituitary medications, from older drugs to the newest options. We will discuss how we expect the medication to work and how long you need to take it. Certain medications control symptoms and shrink tumors. Some patients can eventually stop taking them.
- Clinical trials: Our experience with clinical trials means we test many medications before they become widely available. When these new medications are approved, we are already familiar with them, so we can prescribe appropriately. OHSU was involved in clinical trials that led to approval for:
- Mifepristone for hyperglycemia (high blood sugar) associated with Cushing syndrome
- Pasireotide for acromegaly and Cushing disease
- Off-label medications: We have the expertise to prescribe off-label medications for pituitary tumors. Off-label means we use an FDA-approved medication for a reason other than its specified use. For example, we often prescribe an off-label combination treatment for acromegaly and Cushing disease. We base this practice on our own experience and on studies showing the benefits to patients.
Eye care
A pituitary disorder can cause vision problems or vision loss, especially if a pituitary tumor presses on an optic nerve. If the tumor develops slowly, you may not notice vision problems for some time.
At the OHSU Pituitary Center, you will receive excellent eye and vision care:
- We work with specialists from the OHSU Casey Eye Institute to diagnose and treat pituitary conditions that affect the eyes.
- Skilled eye doctors such as neuro-ophthalmologists do a full exam. These doctors specialize in vision problems caused by the nervous system rather than problems in the eyes themselves.
- Our team includes eye doctors, endocrinologists and neurosurgeons to offer you complete care.
During a neuro-ophthalmology exam, you can expect:
- A full eye exam to test:
- Acuity, or sharpness and clarity
- Color perception and color blindness
- Field of vision
- Pupil responsiveness to light and dark
- Eye movement
- Dilated eye exam to check the back of your eye and examine:
- Retina: A layer of tissue in the back of the eye.
- Optic nerves: Nerves that send signals from the retina to the brain.
Surgery
The OHSU Pituitary Center is a surgical leader. We perform more than 100 tumor surgeries, a high number, in and around the pituitary gland every year. Studies show that experienced surgeons provide higher cure rates, with a lower chance the tumor will come back. Their surgeries also have fewer complications.
We use minimally invasive techniques to remove tumors, including surgery through the nose. These methods leave little scarring and offer an easier recovery.
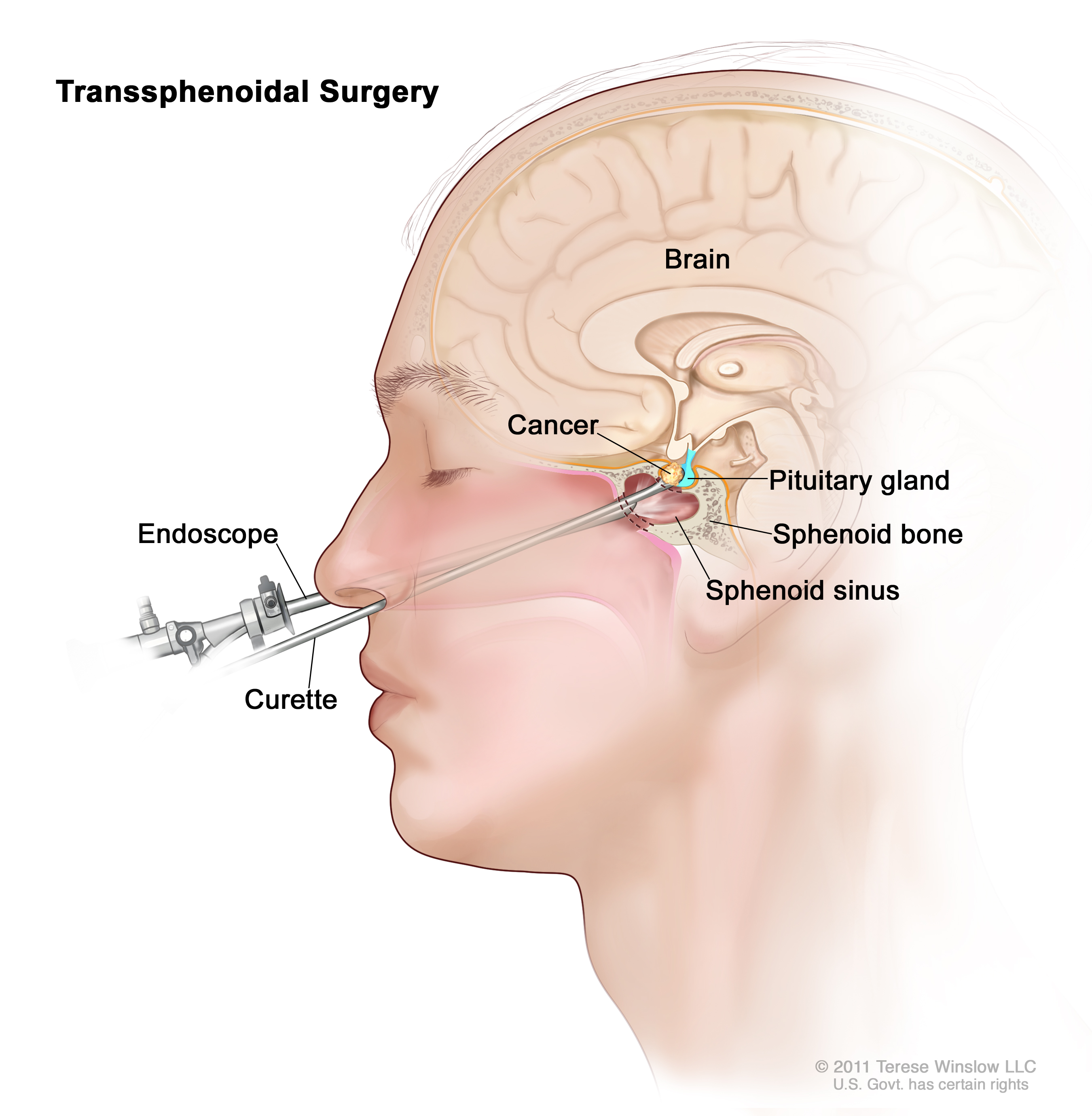
What it is: Transsphenoidal surgery removes pituitary tumors through the nose’s air passages.
- Endoscopic surgery: The surgeon uses an endoscope (small, lighted tube with a high-resolution camera) and tiny instruments to remove the tumor.
- Microscopic surgery: The surgeon uses a surgical microscope to magnify the surgical area, and removes the tumor with tiny instruments through an incision inside the nose.
- Advanced imaging: We use computer-guided imaging for both surgery types to increase safety and accuracy.
How it works: You will receive general anesthesia.
- An ear, nose and throat (ENT) surgeon widens the nasal passages to make room for surgical instruments.
- The neurosurgeon removes a thin piece of bone covering the tumor.
- The team removes the tumor, gently separating it from the normal pituitary gland and other structures.
Advantages:
- You typically go home within a few days.
- Complication rates are low.
- The chances of preserving the pituitary gland and its functions are higher.
- We can remove even large tumors, up to 5 centimeters across (about the size of a lime).
What it is: Transcranial surgery enables the surgeon to reach a tumor through a small incision behind the hairline or in the eyebrow.
When it’s done: To remove a tumor when transsphenoidal surgery is not an option, often because of the tumor's size and location.
How it works: Your surgeon will:
- Make a small incision behind the hairline or in the eyebrow, where it’s hidden.
- Remove a small piece of bone to reach the tumor.
- Use a surgical microscope to magnify the area while carefully removing the tumor from surrounding nerves and arteries.
Advantages: This method may provide more effective results for certain patients compared with the transsphenoidal approach.
Radiation therapy
Radiation therapy can shrink a pituitary tumor or keep it from growing larger. We may recommend radiation after surgery or, in rare cases, instead of surgery. We offer traditional radiation therapy and stereotactic radiosurgery, which shapes the radiation beams to match the tumor, avoiding healthy tissue.
Our program offers:
- Experts in radiation therapy.
- The Novalis Tx radiosurgery system, the most advanced available, to destroy tumor cells while protecting surrounding healthy tissue.
After you finish radiation therapy, you will:
- See your doctor to make sure treatment was successful.
- Have detailed scans (CT scans or MRI) every three to six months for two years, then once a year after that.
- Have yearly pituitary gland, vision and blood tests.
For patients
- Referral: To become a patient, please ask your doctor for a referral.
- Questions: For questions or follow-up appointments, call 503-494-4314.
Location
Parking is free for patients and their visitors.
OHSU Pituitary Center
Center for Health & Healing Building 1
3303 S. Bond Ave.
Portland, OR 97239
Map and directions
Refer a patient
- Refer your patient to OHSU.
- Call 503-494-4567 to seek provider-to-provider advice.
- See more pituitary information for health care professionals.
- OHSU Provider’s Guide to Pituitary Disorders