Cervical Cancer

The OHSU Knight Cancer Institute has Oregon’s first team dedicated to treating gynecologic cancers. We provide sensitive, expert care for women dealing with cervical cancer. You'll find:
- Team-based care, with specialists from different medical fields who work together with you to plan the best course of treatment.
- The latest treatments for cervical cancer, including precision radiation therapy, targeted therapy and minimally invasive robotic surgery.
- Comprehensive screening and treatment for precancerous changes in the cervix.
- A full menu of support services including complementary medicine and fertility services.
Links
- Visit our Gynecologic Cancers page to:
- Learn more about our care
- Find anatomy illustrations
- Meet our team
- Learn about our sensitive care for your sexual health
Understanding cervical cancer
What is cervical cancer?
Cervical cancer develops in a woman’s cervix — the lower, narrow part of the uterus that leads to the vagina. It starts when cells lining the cervix develop abnormally.
If these cells are not found during routine screening, they may develop into cancer. Screening is especially important for cervical cancer because it’s effective at finding precancerous cells and cancer in early stages, when treatment works best.
What causes cervical cancer?
Practically all cervical cancer is caused by the human papillomavirus, or HPV.
More about HPV
Human papillomavirus is the most common sexually transmitted infection in the United States. It infects skin cells and cells that line body cavities.
Most people in the U.S. become infected at some point, according to the Centers for Disease Control and Prevention. Most women’s bodies clear the infection on their own, but in some people, the infection persists and can lead to cancer.
HPV has more than 200 types, classified by number. More than 40 are sexually transmitted. The strains that cause genital warts, or papillomas, are not the same as the 15 high-risk types that can cause cancers in the anus and genitals.
According to the World Health Organization, HPV-16 and HPV-18 cause 70% of precancerous cervical cell changes and cervical cancers worldwide.
Three vaccines prevent infection with HPV-16, HPV-18 and some other high-risk strains. These vaccines are recommended for males and females ages 9 to 26. They are effective against new infections but cannot treat established infections or related cancers.
Who gets cervical cancer?
About 14,000 new cases of cervical cancer are diagnosed in the U.S. every year, according to the National Cancer Institute. Anyone with a cervix, regardless of gender identity, is at risk. Roughly 296,000 people in the U.S. are living with the condition.
Risk factors include:
- Persistent HPV infection: Nearly all cases start with HPV infection.
- Age: Most cases are diagnosed in women ages 20-55.
- Lack of screening: Women without access to regular screening, such as a Pap test, are especially vulnerable.
- Exposure to diethylstilbestrol, or DES: Rarely, women who were exposed to the medication DES before birth develop cervical cancer. DES, a synthetic form of the hormone estrogen, was prescribed to pregnant women in the United States until 1971 to prevent miscarriage.
- Other: Giving birth to many children, being sexually active at a young age, having many sexual partners, long-term use of oral contraceptives.
Survival rates for cervical cancer
A key concept in understanding survival is five-year relative survival rate. This is the percentage of people who are still alive five years after they were first diagnosed, compared to the general population. (It doesn’t count death from other causes.)
The five-year relative survival rate for cervical cancer is 67%, according to the National Cancer Institute. This rises to 91% if it's is caught in the earliest stage.
It's important to remember that these figures are averages and can't predict the outcome for any one patient. It's also important to remember that these figures are based on the treatments that were available more than five years ago. Patients who are diagnosed now may have a better outlook. Treatments are getting better all the time.
Symptoms of cervical cancer
Early cervical cancer usually has no noticeable symptoms. In later stages, possible symptoms include:
- Bleeding between periods, after sex or at any time after menopause
- Pain during sexual intercourse
- Pelvic pain
- Unusual vaginal discharge that may smell unpleasant
All of these symptoms can be caused by other conditions, however, and don’t necessarily mean you have cancer.

Cervical cancer screening
Screening tests can detect precancers and early stages of cervical cancer before you have symptoms. If you have symptoms, your care team may also do an overall physical exam and ask about your medical history.
Pelvic exam: Your doctor will examine your pelvic organs, on the outside and through the vagina, to look for signs of abnormality.
Pap test: Your doctor will gently scrape or brush some cells from your cervix so they can be examined under a microscope for abnormalities.
HPV test: Cells are collected from your cervix to check for high-risk strains of the HPV virus that can cause cell abnormalities. For women 30 and older who may have more risk of long-lasting HPV infections, a Pap test combined with an HPV test is effective at finding early-stage cervical cancers.
Diagnosing cervical cancer
If abnormal cells are detected, your doctor will conduct tests that might include:
Colposcopy: Your doctor uses a lighted magnifying glass called a colposcope to look, from outside your body, for cell changes on your cervix. Your doctor might do a biopsy, removing a small sample of tissue so the cells can be analyzed for cancer or precancer.
Endocervical curettage: Your doctor uses a small spoonlike instrument called a curet to remove a small sample of tissue from inside your cervix.
Cone biopsy: This is a small operation to remove a cone-shaped section of tissue from your cervix. This can be a diagnostic test or, if all abnormal cells are removed, a treatment.
Imaging: Your care team will use imaging such as X-ray, MRI, CT or PET scan to precisely locate the cancer and see if it has spread.
Types of cervical cancer
- Squamous cell carcinoma: The lower part of the cervix that opens to the vagina is lined with squamous cells that are flat and skinlike . About 90% of cervical cancers arise in these cells.
- Adenocarcinoma: The upper part of the cervix near the uterus is lined with glandular cells that produce mucus and other fluids. Tumors that arise from these cells are called adenocarcinomas. They account for about 10% of cervical cancers. Evidence suggests that adenocarcinomas have become more common in recent decades.
- Adenosquamous or mixed carcinomas: Tumors in this relatively rare type of cervical cancer have both squamous and glandular cells.
- Small cell carcinoma of the cervix: This is a rare, fast-growing form that can be difficult to treat.
- Clear cell adenocarcinoma of the cervix: Women who have been exposed to DES in the womb are at risk of developing this rare type.
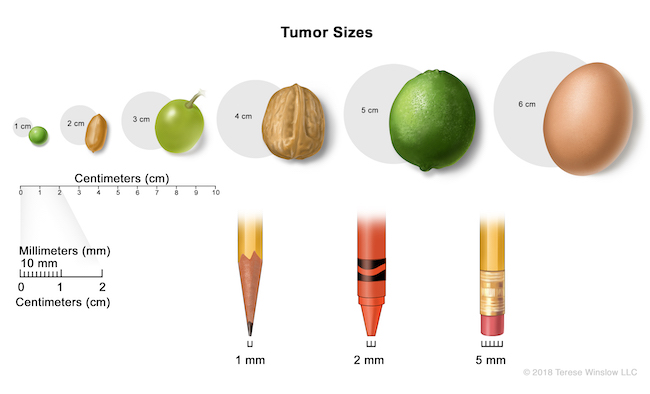
Cervical cancer staging
Your doctors assign a stage to your cancer, based on its size and spread. This helps them plan the most effective treatment.
Stage I: Cancer cells are located in the cervix but have not spread beyond.
- Stage IA: Cancer is microscopic, no deeper than 5 millimeters.
- Stage IB: The tumor is visible without a microscope, or it’s microscopic but bigger than in Stage 1A.
Stage II: The cancer has spread, but not to the pelvic wall or to the lower third of the vagina.
- Stage IIA: The tumor has not spread to the parametrium, tissue next to the cervix.
- Stage IIB: The tumor has spread to the parametrium.
Stage III: The cancer has spread to the lower third of the vagina and/or to the pelvic wall. It may also have blocked one or both ureters (the tubes that drain urine from the kidneys), causing kidney problems. It may also have spread to the lymph nodes (bean-shaped structures that are part of your immune system.)
Stage IV: The cancer has spread to the bladder or rectum and possibly beyond the pelvis to organs such as the liver or lungs.
Cervical cancer treatment
Treatment depends on the stage of your cancer, your age, general health and whether you want to have children. Your care team will develop recommendations tailored to your needs.
For early-stage cancer, you may only need surgery. For cancer that has spread outside the cervix, your care team may recommend radiation therapy combined with chemotherapy instead.
Surgery
Early cancers can be treated with a cone biopsy, a small operation to remove affected tissue. For women with Stage I cancer who want to have children, it may be possible to remove only the cervix, leaving the uterus and ovaries. For later-stage cancers, it may be necessary to remove the uterus and sometimes the ovaries, fallopian tubes and surrounding tissue.
At OHSU, we offer the latest minimally invasive and robotic surgical techniques, which allow for smaller incisions, less pain and quicker recovery.
Radiation therapy
Radiation therapy uses beams of energy to target cancer cells.
External beam radiation therapy: This type uses a machine outside the body to precisely target cancer cells
Brachytherapy: This is a form of internal radiation therapy, with implants placed in or near the tumor.
- Our doctors use special devices to implant radioactive seeds often no bigger than a grain of rice. The treatment can be temporary, with the seeds in place only a few minutes. Or it can be permanent, with the material staying in place. This is safe because the implants produce less radiation over time.
- We were the first center in the U.S. to use a Geneva applicator, which combines two types of brachytherapy: intracavity (a device placed in a body cavity) and interstitial (in the tumor). The applicator offers precise treatment for cervical cancers.
Radiation during surgery: If your cervical cancer has come back, your care team may recommend intraoperative radiation therapy. Our Mobetron device delivers high-energy beams directly to the tumor area. OHSU is the only hospital in Oregon and southwest Washington with this therapy.
Chemotherapy
Chemotherapy medications can kill cancer cells or stop them from growing nearly anywhere in your body. They are usually circulated through your bloodstream using an IV drip called an infusion. Chemotherapy can be used to:
- Shrink a tumor before surgery.
- Kill cancer cells circulating in your body after surgery.
- Slow growth and control symptoms of advanced cancer.
Targeted therapy
These drugs home in on receptors on cancer cells and shut them down. minimizing damage to healthy cells. Some medications are given as pills. Others are by injection. The Knight Cancer Institute is a leader in targeted therapy.
Immunotherapy
These drugs harness the power of your immune system to knock out cancer cells. They prime immune cells to seek out and target cancer cells. Learn more about immunotherapy.
Support for you and your family
- Look for an OHSU clinical trial for cervical cancer.
- Learn about options to protect your fertility.
- We offer the area’s only program to support the sexual health of women affected by cancer.
Learn more
- Cervical Cancer, National Cancer Institute
- Cervical Cancer, American Cancer Society
- HPV and Cancer, National Cancer Institute
- National Cervical Cancer Coalition
Survival rates for cervical cancer
A key concept in understanding survival is five-year relative survival rate. This is the percentage of people who are still alive five years after they were first diagnosed, compared to the general population. (It doesn’t count death from other causes.)
The five-year relative survival rate for cervical cancer is 67%. The rate rises to 91% if cancer is caught early.
It's important to remember that these figures are averages and can't predict the outcome for any one patient. It's also important to remember that these figures are based on the treatments that were available more than five years ago. Patients who are diagnosed now may have a better outlook. Treatments are getting better all the time.
For patients
Call 503-494-7999 to:
- Request an appointment
- Seek a second opinion
- Ask questions
Location
Knight Cancer Institute, South Waterfront
Center for Health & Healing, Building 2
3485 S. Bond Ave.
Portland, OR 97239
Free parking for patients and visitors
Refer a patient
- Refer your patient to OHSU.
- Call 503-494-4567 to seek provider-to-provider advice.
Cancer clinical trials
Clinical trials allow patients to try a new test or treatment.