Arthroscopy Boot Camp
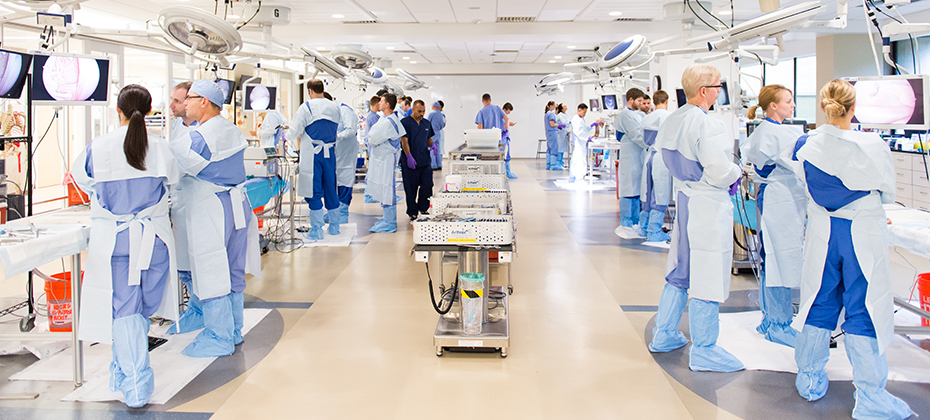
About the Arthroscopy Boot Camp

Arthroscopy is considered an advanced-level orthopaedic skill when it comes to resident education: with little room for variability in portal placement and skill with performing procedures, advance practice is imperative for residents to get a quality clinical experience. In addition, arthroscopy is one of the recommended topics for the ABOS simulation program required by interns. In order to provide this important training to its residents, OHSU has developed an Arthroscopy Boot Camp. Dr. Jacqueline Brady, assistant professor of Orthopaedics and Rehabilitation and the John and Susan Hayhurst Distinguished Scholar in Orthopaedic Research and Innovation, is the lead instructor of all orthopaedic surgical skills labs in VirtuOHSU and program director of the Arthroscopy Boot Camp.
2015 was the first year of OHSU’s boot camp. That year Steelhead Surgical in NW Portland hosted it at their 4-station lab. The PGY-3 and PGY-4 OHSU residents spent each day working through arthroscopic procedures under the guidance of local arthroscopists. Residents and faculty alike gave the experience rave reviews: the residents enjoyed the opportunity to learn from faculty they may not yet have met, and the faculty enjoyed the exchange of ideas and the opportunity to network with possible future partners in their practices.
In 2016, after gathering equipment and exploring options for fluid management, VirtuOHSU was ready to host an arthroscopy lab. The larger space offered the opportunity to spread out to two residents per station, instead of the two to three from the previous year, improving the quality of the experience for each learner. The additional stations also allowed OHSU to invite the Samaritan orthopaedic residents, who rotate with OHSU for oncology and trauma, to join in for the week. Once again, local arthroscopists joined the OHSU effort to enrich the experience and add to the exchange of ideas. This experience is a remarkable way to keep in touch with OHSU’s excellent alumni. Patrick Denard, Kevin Ko, and Ron Wobig were alumni faculty in 2016, and provided excellent perspective on resident education in arthroscopy.

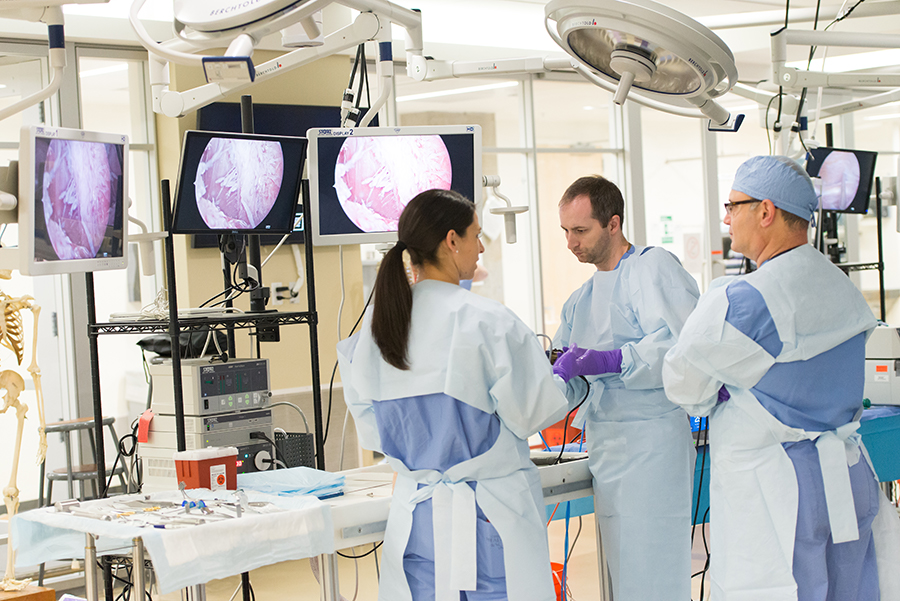
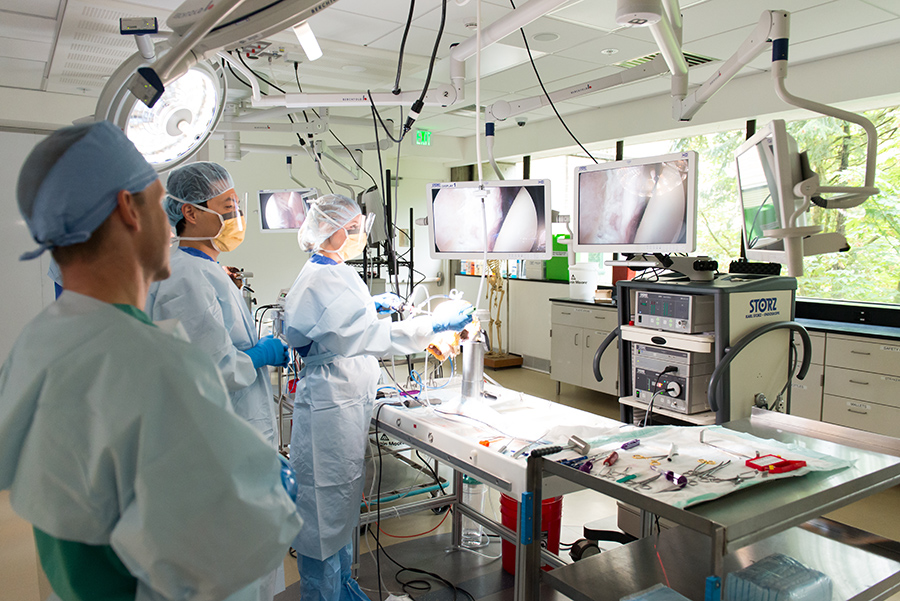
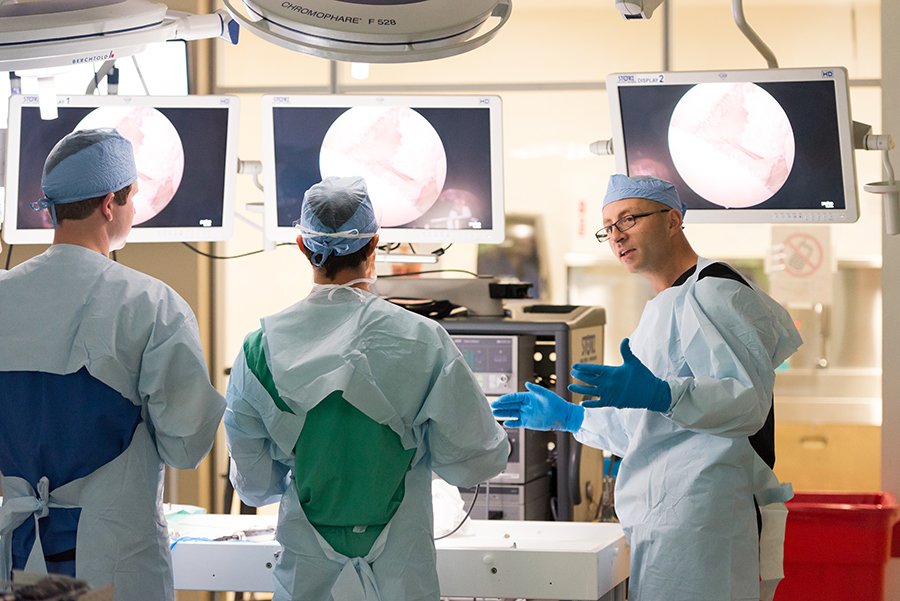
The procedures covered in our Arthroscopy Boot Camp can vary slightly from year to year. In 2016 residents spent the first three days of the boot camp working on shoulder arthroscopy, and the last two days working on knee arthroscopy. Each procedure was covered in detail the first time around, then repeated more expeditiously. Monday focused on glenohumeral procedures: diagnostic arthroscopy, anterior labral repair, superior labral repair, and posterior labral repair. Tuesday shifted gears to the subacromial spaces (after practicing diagnostic arthroscopy again): subacromial decompression, distal clavicle excision, rotator cuff repair, and biceps tenodesis. Wednesday addressed glenohumeral procedures in the morning, and subacromial procedures in the afternoon. On Thursday, residents shifted to the knee: diagnostic arthroscopy, meniscus repair, and meniscectomy in the morning; and ACL reconstruction in the afternoon. On Friday, participants repeated that order, with shifts in technique for portal placement and switching graft choice for ACL reconstruction to make sure the residents got a broad education. Those residents who finished in time moved on to more advanced procedures such as PCL reconstruction, posterolateral corner repair with augmentation, and MCL repair and reconstruction. At the end of every day of the week, time was set aside to dissect the specimens and review the relevant anatomy: nerves and blood vessels that are in peril with various procedures, accuracy of anchor/tunnel placement, and any additional approaches the residents sought to cover.
VirtuOHSU Simulation and Surgical Training Center
The core mission for VirtuOHSU is to provide outstanding leadership in education and training opportunities in surgical skills and simulation. VirtuOHSU serves the entire continuum of health professionals, trainees, students, and researchers at OHSU. This highly versatile space supports open, laparoscopic, endoscopic, and microscopic technical skills training using task trainers, virtual reality, synthetic, animal, and cadaveric tissues. The primary goal of VirtuOHSU is to provide a controlled setting for simulation of technical skills and invasive procedures. Learners include medical students, residents, physicians in practice, physicians seeking re-entry into the work force or needing remediation, nursing and other healthcare providers. VirtuOHSU is also the home of all gross anatomy coursework at OHSU for the School of Medicine, School of Dentistry, and School of Nursing.
The 7,500 square-foot VirtuOHSU Simulation and Surgical Training Center includes 3 labs. Lab A has 2 surgical scrub sinks and a 16 table anatomy dissection lab or 8 station simulated OR (able to flex between 8 or 10 with Lab B). Lab B is a 2 station simulated OR (able to flex to become part of 10). Lab C is a microsurgery suite with 8 Ziess microscopes. The center also includes a 70 seat amphitheater with full AV and conferencing capabilities; an 18-24 seat classroom with SMART board; and a MIS Training Suite with 10 laparoscopy stations, 1 laparoscopic VR simulator, 1 endoscopic/bronchoscopic VR simulator, and 1 da Vinci Robot VR simulator.
More Arthroscopy Boot Camp photos