Understanding Pancreatic Cancer
Cancer of the pancreas, a large gland deep in the abdomen, is an especially complex illness. Things to know:
- Pancreatic cancer shows no or few signs at first, making it difficult to diagnose early.
- New-onset diabetes is an important risk factor.
- Patients do best at a major cancer center with extensive experience diagnosing and treating pancreatic cancer.
- Pancreatic cancer remains challenging to treat, but doctors are making progress.
This page is devoted to exocrine pancreatic cancer, which makes up about 95% of cases.
For pancreatic neuroendocrine tumors, or PNETS, see our page on neuroendocrine tumors.
Anatomy of the Pancreas
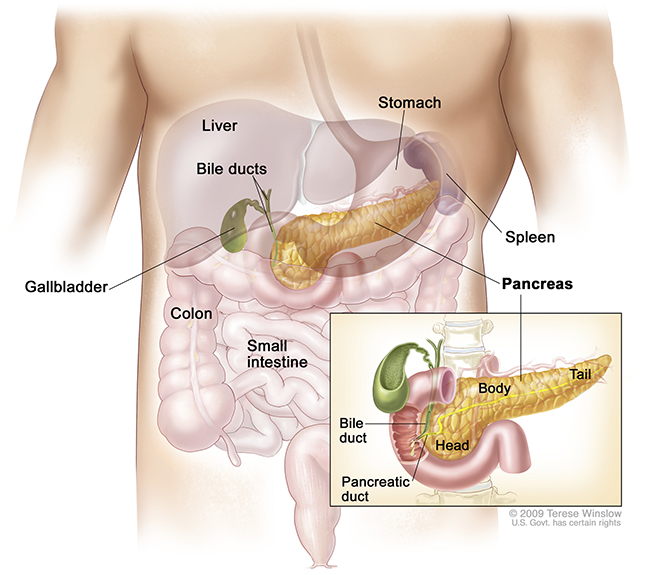
What is pancreatic cancer?
Pancreatic cancer occurs when abnormal cells in the pancreas grow out of control. The pancreas is a gland tucked between the stomach and spine. It’s shaped like a long, horizontal pear. It’s about 6 inches long and has three main parts: a head, body and tail.
The pancreas does two main things:
- It makes juices (enzymes) to digest food.
- It makes hormones (such as insulin) to control blood sugar.
Who gets pancreatic cancer?
About 66,000 new cases of pancreatic cancer are diagnosed in the U.S. every year, according to the National Cancer Institute. Roughly 101,000 Americans are living with it.
Risk factors
Scientists have identified several factors that put people at higher risk:
Gender: It’s slightly more common in men.
Age: Nearly 90% of patients are 55 or older when diagnosed. Two-thirds are 65 or older.
Race/ethnicity: Black people are at slightly higher risk than white people. White people are at slightly higher risk than Asian-Americans, Pacific Islanders, Latinos, Native Americans and Native Alaskans.
Smoking: Smokers are about twice as likely to get pancreatic cancer, according to the American Cancer Society. Smokeless tobacco also increases risk.
Obesity: Being very overweight increases risk about 20%, according to the American Cancer Society.
Family history: Those with a family history of pancreatic cancer or pancreatitis (inflammation of the pancreas) are at higher risk. Inherited syndromes such as multiple endocrine neoplasia and defects in the BRCA1 and BRCA2 genes also increase risk. At OHSU, we offer:
- A Pancreatic Cancer High Risk Clinic to provide monitoring, counseling on lifestyle changes, and other services to lower and manage risk.
- Expert medical geneticists who provide genetic counseling, risk assessment and testing.
Chronic pancreatitis: Repeated bouts of pancreatic inflammation are linked to an increased risk.
Diabetes: Most diabetes patients will not get pancreatic cancer. But diabetes is linked to an increased risk of pancreatic cancer. Research also suggests pancreatic cancer can cause diabetes, perhaps by disrupting how the pancreas produces insulin.
New-onset diabetes: This type of diabetes, in particular, has a strong link to pancreatic cancer. It may indicate a higher risk of pancreatic cancer, or it may be a sign that cancer is already present. It is of particular concern in a patient without risk factors for diabetes.
Pancreatic cancer survival rates
Pancreatic cancer is challenging to treat, in part because of:
- Few signs: Pancreatic cancer shows few symptoms early on. About 80% of patients are diagnosed after the cancer has spread to other parts of the body.
- The location of the pancreas: The pancreas is deep in the abdomen, where it’s hard to see and reach. It’s also curved around large blood vessels, complicating surgical options. Blood vessels and many nearby lymph nodes (part of the immune system) can speed its spread.
- Complex tumors: Pancreatic tumors often have several cell types. This makes them more challenging to match with treatments.
- A related condition: Pancreatic cancer patients are especially likely to develop a wasting syndrome called cachexia (kuh-KECK-see-uh). These patients lose a lot of muscle and weight, leaving them less able to tolerate cancer treatments.
These factors result in discouraging long-term survival rates. At the same time, statistics are averages that can’t predict the outcome for any one patient. In addition, five-year relative survival rates, the most common measure, are by definition based on treatments that were available five or more years ago.
Signs of hope: Five-year survival rates have more than doubled over the past 20 years. The Knight Cancer Institute and other major cancer centers can offer surgery to more patients than ever.
Quality of life: Surgically removing all the cancer remains essential to a cure, but it’s not the only way to extend and improve life. The Knight Cancer Institute is devoted to giving every patient the best quality of life possible for as long as possible.
Signs and symptoms of pancreatic cancer
These symptoms also have other causes and don’t necessarily mean you have pancreatic cancer. Signs include:
- Jaundice: Cancer can block the bile duct, leading to a buildup of a dark yellow-brown substance called bilirubin. This can turn the skin and eyes yellow.
- Itchiness and dark urine: Bilirubin buildup can make the skin itch and turn urine dark.
- Stool changes: If cancer blocks bilirubin and pancreatic juices from breaking down fats in the digestive system, stools can be lighter colored and greasy.
- Weight loss for unknown reasons
- Appetite loss
- Fatigue
- Pain in the back or belly
- Diarrhea
- Vomiting
Types of pancreatic cancer
Exocrine pancreatic cancer: This type starts in the exocrine cells, which make enzymes to digest food. The most common type, ductal adenocarcinoma, starts in the pancreatic duct, where the enzymes are released. The pancreatic duct runs the length of the pancreas and connects with the small intestine.
Pancreatic neuroendocrine tumors (PNETs): These tumors arise in the endocrine cells, which make hormones. Learn more about pancreatic neuroendocrine tumors, or PNETs, on our page about neuroendocrine tumors.
Treatment and outcomes vary with where in the pancreas the cancer starts: the head/neck, body or tail.
Most start in the head. Because the head is next to the bile duct, cancer here is more likely to block the duct and cause jaundice and other symptoms. This can lead to earlier detection and better outcomes.
Resectable: The cancer can be surgically removed (resected).
Borderline resectable: The cancer has invaded major blood vessels but still might be removable with surgery if combined with additional treatment. Chemotherapy and/or radiation therapy can sometimes shrink the tumor before surgery. Expert surgeons can sometimes reconstruct affected blood vessels.
Unresectable: The cancer has spread too far for surgical removal.
Pancreatic cancer staging
Stage I: The tumor is confined to the pancreas.
- Stage IA: The tumor is no bigger than 2 centimeters at its widest point.
- Stage IB: The tumor is bigger than 2 centimeters but no bigger than 4 centimeters.
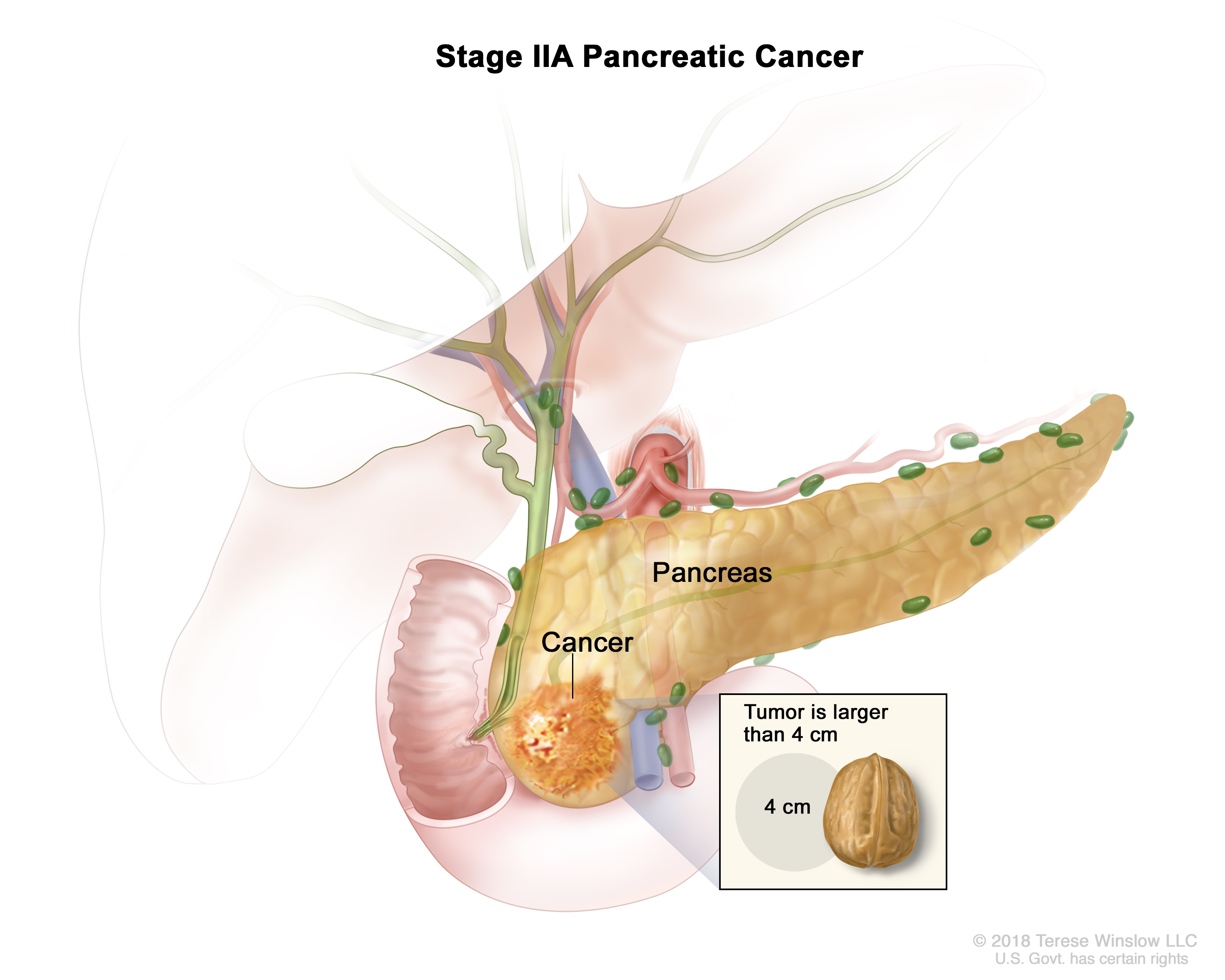
Stage II:
- Stage IIA: The tumor is confined to the pancreas and bigger than 4 centimeters.
- Stage IIB: The tumor ranges from smaller than 2 centimeters to larger than 4 centimeters. Cancer has spread to one to three nearby lymph nodes.
Stage III: One of the following:
- The tumor ranges from smaller than 2 centimeters to larger than 4 centimeters. Cancer has spread to four or more nearby lymph nodes.
- The tumor involves nearby major blood vessels and any number of lymph nodes.
Stage IV: Cancer has spread to distant parts of the body such as the liver or lungs.
Learn more
- OHSU Brenden-Colson Center for Pancreatic Care, a research institute devoted to early detection, advanced therapy and improving patient quality of life
- Pancreatic Cancer, National Cancer Institute
- Pancreatic Cancer, American Cancer Society
- Pancreatic Cancer Action Network, an advocacy, educational and support organization
- Lustgarten Foundation, an organization devoted to advancing research to prevent, diagnose, treat and cure pancreatic cancer
- National Pancreas Foundation, an advocacy, educational and support organization
- Pancreatica, Confronting Pancreatic Cancer, an advocacy and educational organization
- Pancreatic Neuroendocrine Tumors (Islet Cell Tumors), National Cancer Institute
For patients
Call 503-494-7999 to:
- Make an appointment
- Seek a second opinion
- Ask questions
Location
Knight Cancer Institute, South Waterfront
Center for Health & Healing, Building 2
3485 S. Bond Ave.
Portland, OR 97239
Free parking for patients and visitors
Refer a patient
- Refer your patient to OHSU.
- Call 503-494-4567 to seek provider-to-provider advice.
Cancer clinical trials
Clinical trials allow patients to try a new test or treatment.
Read more
Learn more about OHSU Knight Cancer Institute treatments: